
Why Dementia Questions to Ask for Better Matters
Caring for individuals with dementia presents a significant challenge, often marked by uncertainty and emotional strain. Families face the complexities of diagnosis and treatment options, grappling with essential questions as their loved ones navigate this difficult condition. This article addresses ten critical questions caregivers should consider, offering valuable insights and actionable strategies to improve the quality of care.
How can caregivers effectively bridge the gap between medical advice and the emotional needs of those they support? It’s crucial to ensure that every interaction fosters understanding and compassion. By focusing on these aspects, caregivers can enhance their approach and provide the support that individuals with dementia truly need.
Happy to Help Caregiving: Essential Support for Dementia Care
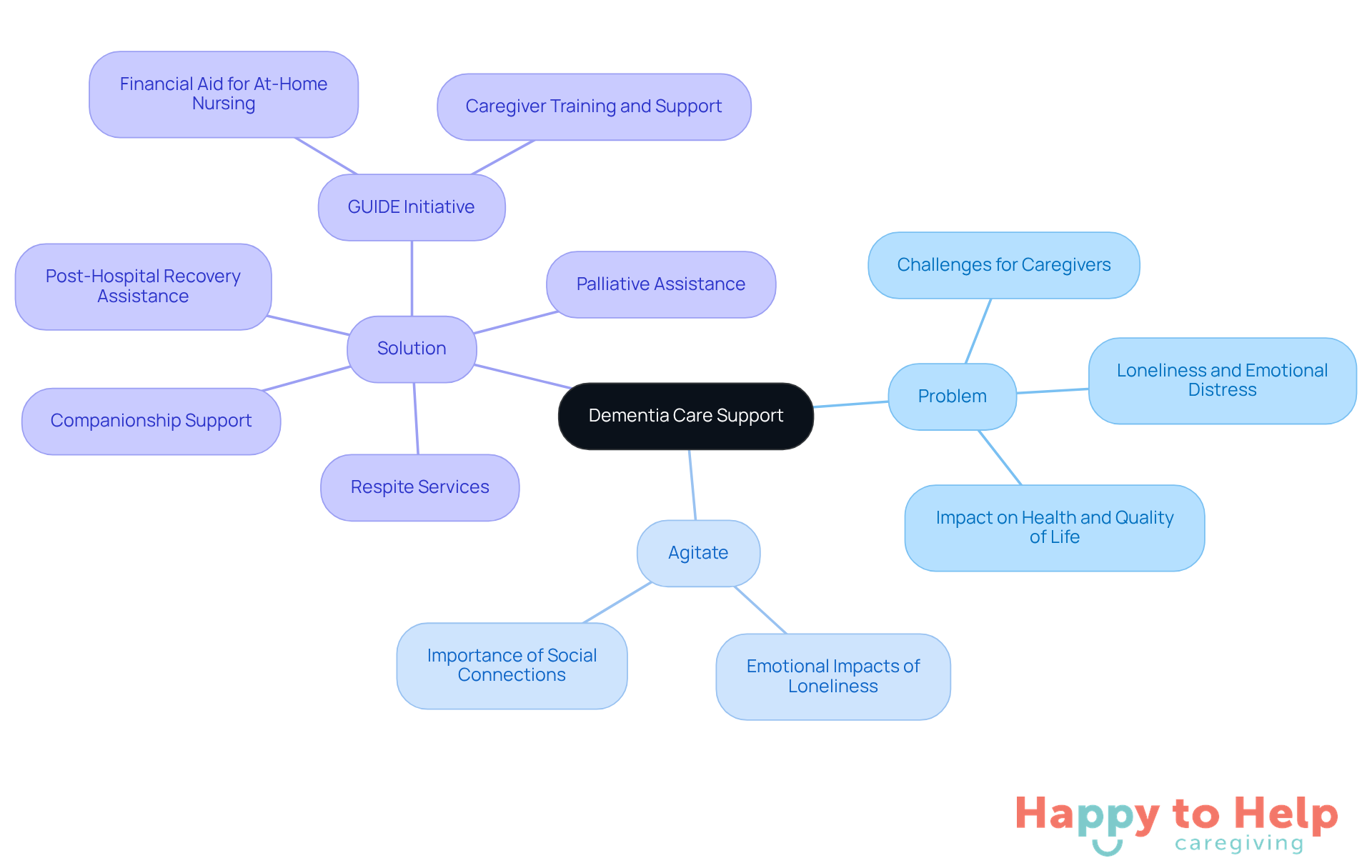
Problem: Caring for individuals with cognitive impairments presents significant challenges for families and caregivers. These individuals often experience feelings of loneliness and emotional distress, which can negatively impact their overall health and quality of life.
Agitate: The lack of companionship and meaningful engagement can exacerbate these feelings, leading to a decline in emotional well-being. Research indicates that social connections are crucial for individuals with cognitive impairments, as they can enhance mood and cognitive function. Caregivers frequently note the importance of building relationships with their clients, as these connections can lead to improved outcomes.
Solution: Happy to Help Caregiving addresses these challenges through customized in-home support services. Their offerings include:
- Companionship support
- Post-hospital recovery assistance
- Respite services
- Palliative assistance
All designed to enhance clients' quality of life. By providing empathetic support in familiar environments, caregivers foster a sense of safety and comfort.
Additionally, recent advancements in tailored caregiving emphasize the importance of addressing personal needs. Programs like the GUIDE initiative offer financial aid for at-home nursing services, allowing families to keep their loved ones in a comfortable setting while receiving essential support. Such initiatives underscore the growing recognition of individualized care in managing cognitive decline, ensuring that patients receive the attention and companionship they need to thrive.
What is the Official Diagnosis of Dementia?
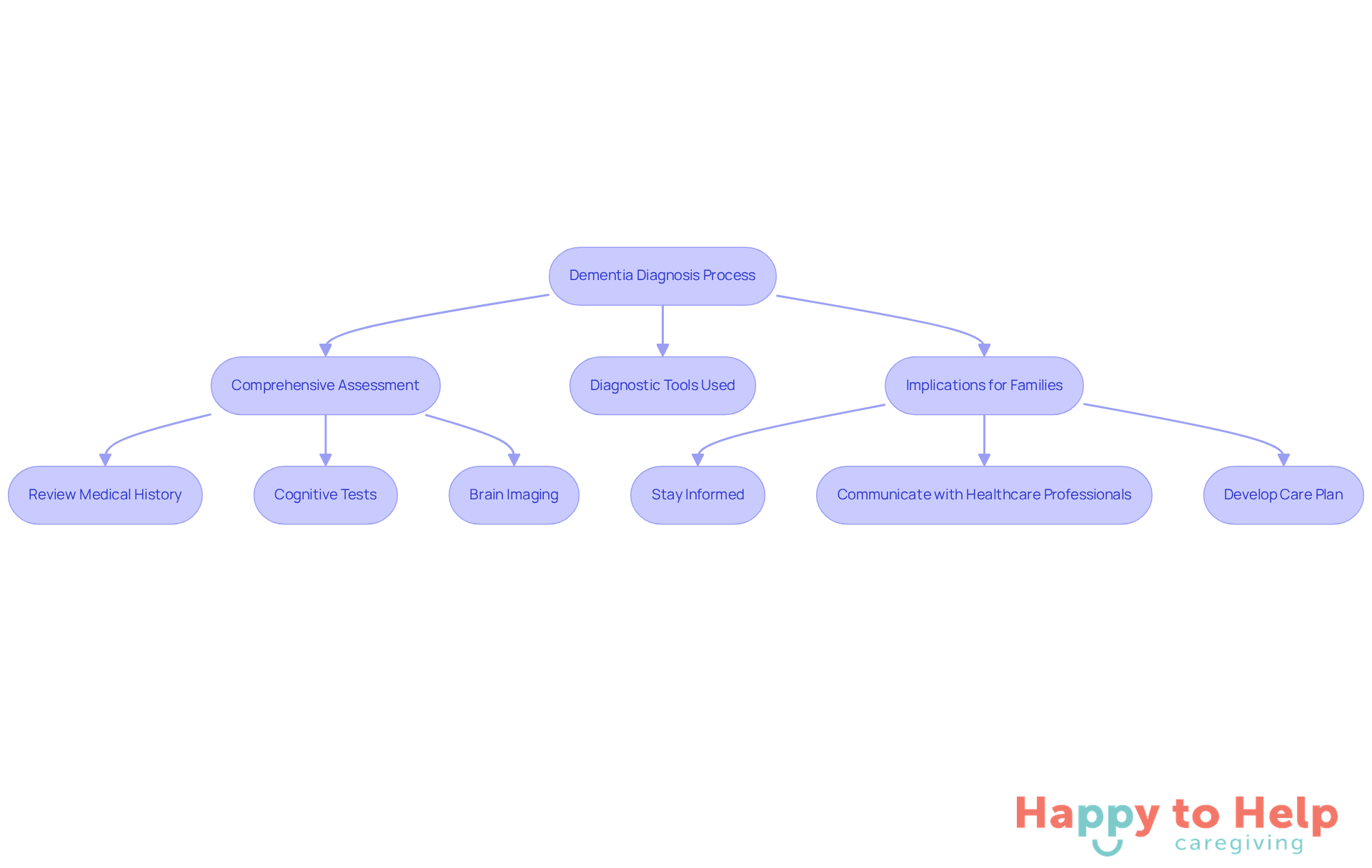
Cognitive decline poses significant challenges for families, particularly when it comes to understanding the diagnosis and addressing dementia questions to ask. The formal diagnosis typically involves a comprehensive assessment by a healthcare professional, which includes a review of medical history, cognitive tests, and possibly brain imaging. Common diagnostic tools, such as the Mini-Mental State Examination (MMSE) and the Montreal Cognitive Assessment (MoCA), are used to evaluate cognitive function.
Recognizing the implications of a cognitive decline diagnosis is crucial for families. It helps them prepare for the challenges ahead and facilitates appropriate care planning. Caregivers can take proactive steps by familiarizing themselves with these diagnostic tools and knowing the dementia questions to ask to understand their significance. This knowledge empowers them to engage more effectively with healthcare providers and advocate for the best care options.
To support caregivers, here are some actionable tips:
- Stay informed about cognitive assessments and their outcomes.
- Communicate openly with healthcare professionals to clarify any uncertainties.
- Develop a care plan that addresses the specific needs of the individual diagnosed.
By understanding the diagnosis and its implications, families can navigate the complexities of cognitive decline with greater confidence and clarity.
What Treatment Options Are Available for Dementia?
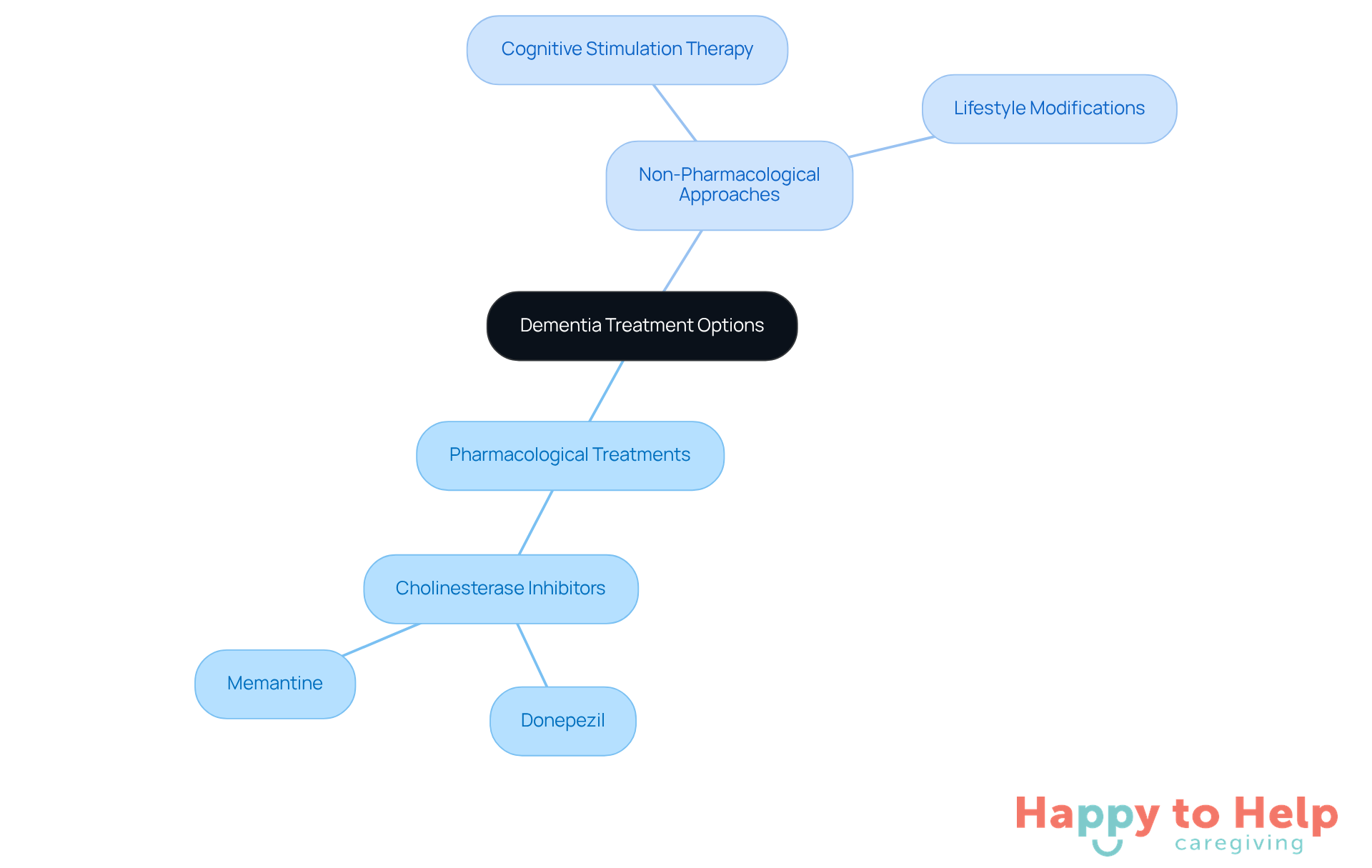
Treatment options for dementia can be a significant challenge for caregivers, as they vary widely based on the type and stage of the disease. This variability can lead to confusion and frustration when trying to find the most effective care for loved ones.
To address this issue, it's essential to understand the common medications available. Cholinesterase inhibitors, such as Donepezil and Memantine, are often prescribed to help manage symptoms. However, relying solely on medication may not be enough.
In addition to pharmacological treatments, non-pharmacological approaches can play a crucial role. Cognitive stimulation therapy and lifestyle modifications have been shown to be beneficial in enhancing the quality of life for individuals with dementia. Families should actively engage with healthcare providers to develop a comprehensive treatment plan that includes important dementia questions to ask, tailored to their loved one's specific needs.
By combining medication with supportive therapies, caregivers can create a more effective and holistic approach to dementia care.
How Will Dementia Progress Over Time?
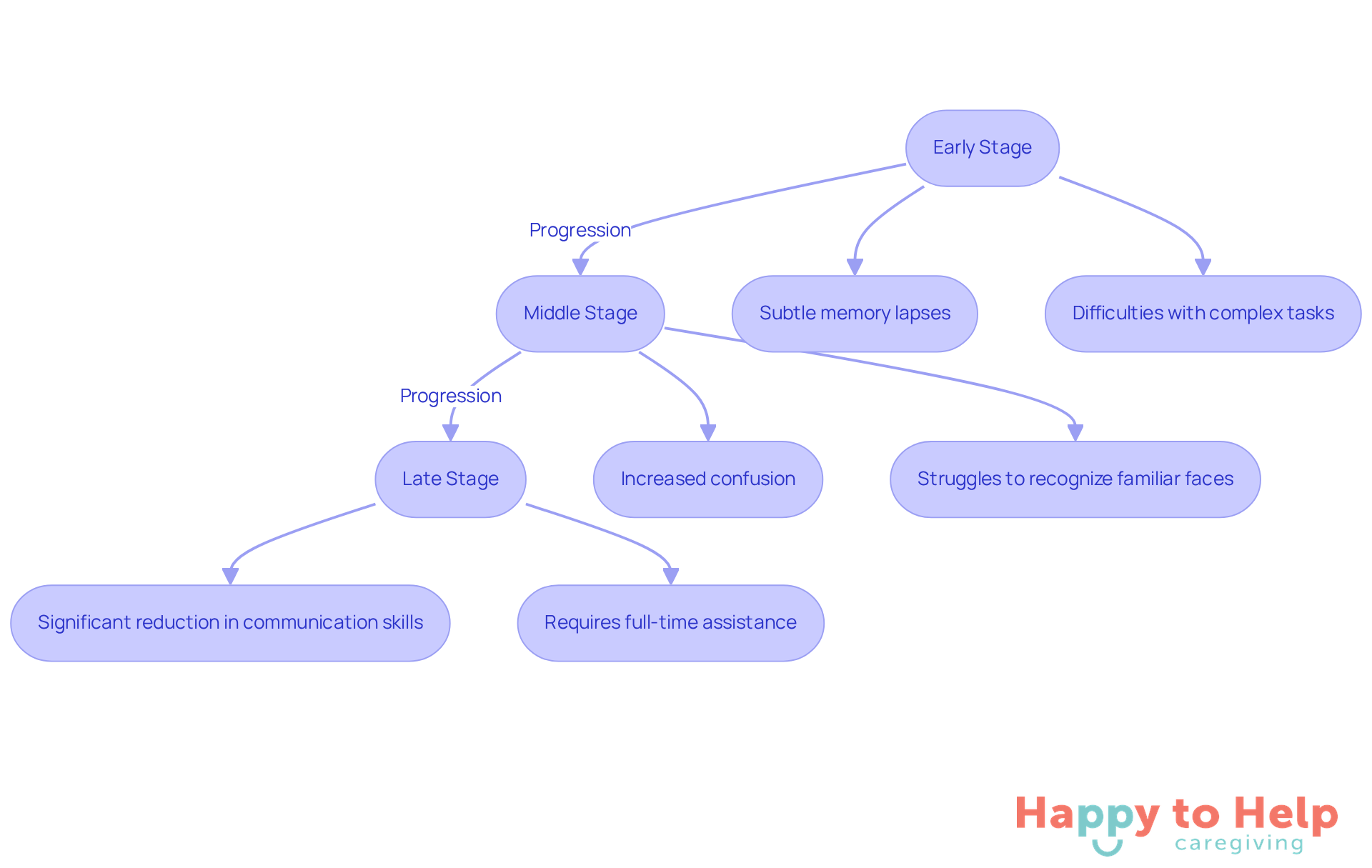
Dementia presents a significant challenge as it typically progresses through three distinct stages: early, middle, and late. In the early phase, lasting about two years, individuals may experience subtle memory lapses and difficulties with complex tasks. As the disease advances into the middle stage, which lasts approximately two to four years, symptoms become more pronounced, leading to increased confusion and noticeable changes in daily independence. During this phase, individuals may struggle to recognize familiar faces and require assistance with daily activities.
The final phase, which may last one to two years, is characterized by a significant reduction in communication skills and mobility, necessitating full-time assistance. Understanding this progression is crucial for families, as it allows them to effectively plan for necessary support and interventions, including considering dementia questions to ask.
Families face the problem of navigating these stages without adequate preparation, including knowing the dementia questions to ask. The implications of this lack of planning can lead to increased stress and inadequate care for their loved ones. To address these challenges, personalized support plans can be developed to meet the unique needs of individuals at every stage, ensuring they receive appropriate assistance while preserving their dignity.
For instance, memory support communities that offer organized routines and round-the-clock supervision illustrate how customized assistance can enhance the quality of life for those living with cognitive impairments. By recognizing the signs of progression early, families can seek professional guidance and explore supportive care options, ultimately fostering a smoother transition through the stages of cognitive decline.
What Safety Measures Should Be Implemented at Home?
Problem: Establishing safety protocols at home is crucial for people with cognitive impairment. Without proper measures, individuals may face increased risks of accidents and confusion in their environment.
Agitate: This can lead to serious injuries and a decline in their overall well-being, which can be distressing for both the individual and their caregivers. The challenges of navigating a home filled with tripping hazards or inadequate lighting can significantly impact daily life.
Solution: To enhance safety, consider implementing the following strategies:
- Remove tripping hazards: Clear pathways of clutter and secure loose rugs.
- Install grab bars: Place these in bathrooms to provide support and stability.
- Use bright lighting: Ensure all areas are well-lit to reduce confusion and enhance visibility.
- Label rooms: Use simple signs to help individuals navigate their environment more easily.
- Conduct routine safety evaluations: Regularly assess the living space to ensure it meets the changing needs of the individual with cognitive challenges.
By taking these steps, caregivers can create a safer and more supportive home environment.
What Communication Strategies Work Best with Dementia Patients?
Problem: Caregivers often face significant challenges when communicating with individuals who have cognitive impairment. These challenges can lead to misunderstandings and frustration for both parties.
Agitate: Overwhelming a person with too much information can exacerbate these difficulties. Caregivers may find that their attempts to communicate effectively are met with confusion or disengagement, which can hinder the caregiving process.
Solution: To improve communication, caregivers should use clear, simple language and maintain eye contact. Here are some actionable tips:
- Use short sentences to convey information clearly.
- Allow ample time for responses, ensuring the individual feels comfortable.
- Incorporate non-verbal cues, such as gestures and facial expressions, to aid understanding.
- Create a calm environment with minimal distractions to facilitate effective communication.
By implementing these strategies, caregivers can enhance their interactions and foster a more supportive atmosphere.
What Behavioral Changes Should We Expect in Dementia Patients?
Behavioral changes in dementia patients present significant challenges for caregivers. Increased agitation, mood swings, and withdrawal from social interactions can stem from confusion, frustration, or unmet needs. These behaviors not only affect the patients but also create stress for those caring for them.
To address these issues, caregivers should approach these behaviors with patience and understanding. Utilizing calming techniques and engaging in familiar activities can help ease distress. For instance, maintaining a consistent routine offers a sense of stability, which is crucial for individuals with dementia.
Here are some actionable tips for caregivers:
- Use calming techniques: Gentle touch or soothing music can help reduce agitation.
- Engage in familiar activities: Activities that the patient enjoys can provide comfort and reduce withdrawal.
- Establish a routine: A predictable schedule can help alleviate confusion and anxiety.
By implementing these strategies, caregivers can create a more supportive environment that addresses the needs of dementia patients while also reducing their own stress.
What Should We Consider When Planning for Future Care?
When preparing for future support, families face a significant challenge: understanding the individual's preferences, medical requirements, and financial resources. Failing to consider these factors can lead to misunderstandings and unmet needs as care progresses.
To address this issue, it's crucial for families to engage in open discussions about long-term care options. This includes weighing the benefits of in-home care against assisted living. Involving all family members in these conversations ensures that everyone is on the same page and that the individual's wishes are prioritized.
Additionally, legal and financial planning cannot be overlooked. Establishing advance directives and appointing a power of attorney are essential steps to ensure that the individual's preferences are respected as their condition evolves. By taking these proactive measures, families can create a supportive environment that honors the needs and desires of their loved ones.
How Can We Address the Emotional Impact of Dementia?
The emotional impact of cognitive decline is significant, affecting both individuals with the condition and their caregivers. Nearly 12 million Americans provide unpaid support for loved ones with dementia, leading to alarming rates of burnout among these caregivers. In fact, 59% report high levels of emotional stress, often exacerbated by the complexities of the healthcare system. Additionally, 66% struggle to find the necessary resources and support, underscoring the challenges they face in accessing assistance.
To address these issues, caregivers must prioritize self-care and actively seek support from community resources. Local support groups and counseling services can be invaluable. Engaging in open discussions about emotions and experiences can alleviate feelings of isolation, fostering a sense of community among caregivers.
Programs like Mason CARES demonstrate that effective support can lead to a 15% reduction in stress levels for caregivers, highlighting the importance of community resources. Moreover, participating in enjoyable activities with those receiving care can strengthen emotional connections and enhance the overall caregiving experience. For instance, caregivers who share music time with their loved ones often find it a powerful bonding method, as familiar tunes can evoke positive memories and improve communication.
By adopting these strategies, caregivers can enhance their emotional well-being while providing compassionate support.
How Often Should We Schedule Follow-Up Appointments?
When scheduling follow-up appointments for dementia patients, it's essential to consider key dementia questions to ask. Irregular appointments may lead to missed opportunities for monitoring cognitive changes and adjusting treatment plans. This can leave families feeling uncertain about the best course of action for their loved ones, including the dementia questions to ask.
To address this issue, it’s essential to schedule these appointments regularly - typically every six to twelve months, depending on the individual’s condition. These visits allow healthcare providers to closely monitor changes in cognitive function and address any emerging concerns. Families should also maintain open communication with healthcare providers to ensure that all aspects of the patient’s care are effectively managed. By prioritizing these appointments and fostering collaboration with healthcare professionals, caregivers can significantly enhance the quality of care for dementia patients.
Moving Forward with Dementia Questions to Ask for Better
Caring for individuals with dementia presents significant challenges for families and caregivers. The complexities of dementia can lead to feelings of frustration and helplessness, making it essential to approach care with a clear understanding and effective strategies.
One of the key issues is the emotional toll on caregivers, who often feel overwhelmed by the demands of providing support. This emotional strain can impact their ability to communicate effectively and maintain a nurturing environment. To address these challenges, caregivers should prioritize self-care and seek community support, which can alleviate some of the burdens they face.
To enhance the quality of care, families must engage in open discussions with healthcare providers and actively participate in care planning. This proactive approach ensures that loved ones receive personalized support tailored to their unique needs. Implementing safety measures at home is also crucial, as it helps create a secure environment that fosters independence while minimizing risks.
Effective communication strategies are vital in dementia care. Caregivers should focus on using clear, simple language and non-verbal cues to connect with their loved ones. Understanding the progression of dementia allows families to anticipate changes and adapt their care strategies accordingly.
Ultimately, while the journey of dementia care can be daunting, informed decision-making and strong communication can significantly improve the experience for both patients and caregivers. By embracing available resources and fostering a supportive network, families can create a nurturing environment that honors the dignity and preferences of their loved ones.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5MjRmMWI5ZWM0Y2FiOGU3NGVjMDA5YiIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What challenges do families and caregivers face when caring for individuals with cognitive impairments?
Families and caregivers face significant challenges such as feelings of loneliness and emotional distress in individuals with cognitive impairments, which can negatively impact their overall health and quality of life.
Why are social connections important for individuals with cognitive impairments?
Social connections are crucial as they can enhance mood and cognitive function, helping to improve emotional well-being and overall outcomes for individuals with cognitive impairments.
What services does Happy to Help Caregiving provide to support dementia care?
Happy to Help Caregiving offers customized in-home support services, including companionship support, post-hospital recovery assistance, respite services, and palliative assistance, all designed to enhance clients' quality of life.
How does Happy to Help Caregiving ensure a comfortable environment for clients?
By providing empathetic support in familiar environments, caregivers foster a sense of safety and comfort for clients.
What is the GUIDE initiative and how does it support families?
The GUIDE initiative offers financial aid for at-home nursing services, allowing families to keep their loved ones in a comfortable setting while receiving essential support, emphasizing the importance of individualized care in managing cognitive decline.
How is dementia formally diagnosed?
Dementia is formally diagnosed through a comprehensive assessment by a healthcare professional, which includes a review of medical history, cognitive tests, and possibly brain imaging.
What are common diagnostic tools used for assessing cognitive function?
Common diagnostic tools include the Mini-Mental State Examination (MMSE) and the Montreal Cognitive Assessment (MoCA).
What steps can caregivers take to prepare for the challenges of cognitive decline?
Caregivers can stay informed about cognitive assessments, communicate openly with healthcare professionals, and develop a care plan that addresses the specific needs of the individual diagnosed.
What treatment options are available for dementia?
Treatment options for dementia vary widely and may include medications such as cholinesterase inhibitors (e.g., Donepezil and Memantine) as well as non-pharmacological approaches like cognitive stimulation therapy and lifestyle modifications.
How can caregivers create an effective treatment plan for dementia?
Caregivers should actively engage with healthcare providers to develop a comprehensive treatment plan that combines medication with supportive therapies tailored to their loved one's specific needs.
List of Sources
- Happy to Help Caregiving: Essential Support for Dementia Care
- Medicare covers at-home nursing care for dementia patients for the first time this year (https://tampabay.com/news/health/2025/08/14/medicare-covers-at-home-nursing-care-dementia-patients-first-time-this-year)
- Alzheimer's Disease Facts and Figures (https://alz.org/alzheimers-dementia/facts-figures)
- New Medicare program offers much-needed relief for caregivers of dementia patients (https://finance.yahoo.com/news/new-medicare-program-offers-much-needed-relief-for-caregivers-of-dementia-patients-203450020.html)
- 2025 Home Care Statistics: Trends & Insights To Know (https://premierhcinc.com/blog/home-care-statistics)
- Pa., N.J. and Del.families can now enroll in a new Medicare dementia program (https://whyy.org/articles/medicare-dementia-guide-program-pennsylvania-new-jersey-delaware)
- What is the Official Diagnosis of Dementia?
- ADI - Dementia statistics (https://alzint.org/about/dementia-facts-figures/dementia-statistics)
- Mayo Clinic's AI tool identifies 9 dementia types, including Alzheimer's, with one scan - Mayo Clinic News Network (https://newsnetwork.mayoclinic.org/discussion/mayo-clinics-ai-tool-identifies-9-dementia-types-including-alzheimers-with-one-scan)
- 2025 NIH Alzheimer’s Disease and Related Dementias Research Progress Report: Advances and Achievements (https://nia.nih.gov/about/2025-nih-dementia-research-progress-report)
- Diagnosis of dementia - Dementia Statistics Hub (https://dementiastatistics.org/about-dementia/diagnosis)
- Risk and future burden of dementia in the United States (https://nih.gov/news-events/nih-research-matters/risk-future-burden-dementia-united-states)
- How Will Dementia Progress Over Time?
- Top List of Inspirational Dementia Quotes for Caregivers (https://rochesterlawcenter.com/dementia-resources/dementia-quotes)
- 2025 NIH Alzheimer’s Disease and Related Dementias Research Progress Report: Advances and Achievements (https://nia.nih.gov/about/2025-nih-dementia-research-progress-report)
- How Fast Do the Stages of Dementia Progress? (https://onelifeseniorliving.com/blog/how-fast-do-the-stages-of-dementia-progress)
- ADI - Dementia statistics (https://alzint.org/about/dementia-facts-figures/dementia-statistics)
- Alzheimer's Research Advances at AAIC 2025 | alz.org (https://aaic.alz.org/releases-2025/highlights-aaic-2025.asp)
- What Safety Measures Should Be Implemented at Home?
- Creating a dementia-friendly home environment | Healthcare Homes (https://healthcarehomes.co.uk/support-articles/creating-a-dementia-friendly-home-environment)
- (PDF) Creating homes for individuals living with dementia (https://researchgate.net/publication/382315105\_Creating\_homes\_for\_individuals\_living\_with\_dementia)
- Stay Safe in the Home With Dementia (https://psychologytoday.com/us/blog/managing-your-memory/202201/stay-safe-in-the-home-with-dementia)
- Care Tips to Keep Dementia Patients Safe at Home (https://aarp.org/caregiving/home-care/dementia-home-safety)
- Dementia Care: Keeping Loved Ones Safe and Happy at Home (https://hopkinsmedicine.org/health/wellness-and-prevention/safe-and-happy-at-home)
- What Communication Strategies Work Best with Dementia Patients?
- Communicating with a Person with Dementia | Strategy (https://allenbrook-fordingbridge.co.uk/news/effective-communication-strategies-with-dementia-patients)
- Study offers guidance for communicating with loved ones living with dementia (https://news-medical.net/news/20250827/Study-offers-guidance-for-communicating-with-loved-ones-living-with-dementia.aspx)
- Top List of Inspirational Dementia Quotes for Caregivers (https://rochesterlawcenter.com/dementia-resources/dementia-quotes)
- The facilitators of communication with people with dementia in a care setting: an interview study with healthcare workers (https://academic.oup.com/ageing/article/45/1/164/2195309)
- Improv training: A new approach to dementia care | Emory University | Atlanta GA (https://news.emory.edu/stories/2025/01/hs\_improving\_dementia\_care\_through\_improv\_15-01-2025/story.html)
- How Can We Address the Emotional Impact of Dementia?
- New Alzheimer’s Association Report Reveals Top Stressors for Caregivers and Lack of Care Navigation Support and Resources (https://alz.org/news/2024/new-alzheimers-association-report-reveals-top-stressors-caregivers)
- Dementia Statistics & Facts (https://mastermindbehavior.com/post/dementia-statistics-facts)
- Caregivers: the invisible backbone of dementia care (https://hap.gmu.edu/news/2025-11/caregivers-invisible-backbone-dementia-care)
- Alzheimer’s Association Honors the Nearly 12 Million Americans Who Serve as Dementia Caregivers and Shares New Resources to Help Them Thrive (https://alz.org/news/2025/november-national-family-caregivers-alzheimers-disease-awareness-month)
- How Often Should We Schedule Follow-Up Appointments?
- Improving the diagnosis of dementia in care homes with DeAR-GP - The Health Innovation Network (https://thehealthinnovationnetwork.co.uk/case\_studies/improving-the-diagnosis-of-dementia-in-care-homes-with-dear-gp)
- New Alzheimer’s Association Report Finds Patient-Physician Communication About Cognitive Concerns Needs Improvement as New Treatments Become Available (https://alz.org/news/2023/new-alzheimer-s-association-report-finds-patient-physician-communication-about-cognitive-concerns-ne)
- (PDF) Effects of Tracking Technology on Daily Life of Persons With Dementia: Three Experimental Single-Case Studies (https://researchgate.net/publication/261923008\_Effects\_of\_Tracking\_Technology\_on\_Daily\_Life\_of\_Persons\_With\_Dementia\_Three\_Experimental\_Single-Case\_Studies)
- Development and Implementation of an Anticipatory Care Calendar for people with learning disabilities or dementia - Quality in Care Awards Programme (https://qualityincare.org/case\_studies/development\_and\_implementation\_of\_an\_anticipatory\_care\_calendar\_for\_people\_with\_learning\_disabilities\_or\_dementia)

