
Understanding Palliative Care Services in
Navigating the complexities of serious illness can be overwhelming for families. Caregivers often struggle to ensure their loved ones receive the right care, which can lead to increased stress and uncertainty. This challenge is compounded by the emotional and social needs of patients, which are just as critical as their physical health.
Palliative care services in Philadelphia provide a vital lifeline. These services address not only the physical needs of patients but also their emotional and social well-being. By exploring the essential services available, families can discover how tailored support can significantly enhance quality of life during challenging times.
Yet, with so many options available, caregivers may wonder how to identify the most effective resources. Understanding the landscape of palliative care can empower families to make informed decisions that truly meet their loved ones' needs.
Happy to Help Caregiving: Palliative Support Care Services
Caregivers often face significant challenges when supporting clients with severe health conditions. These challenges can lead to feelings of helplessness and stress, impacting both the caregiver and the client.
Happy to Help Caregiving addresses these issues by providing a comprehensive range of supportive services aimed at enhancing the quality of life for clients. These services include:
- Symptom management
- Emotional support
- Assistance with daily activities
All delivered in the comforting environment of the client’s home. Caregivers are specially trained to offer compassionate support that meets both physical and emotional needs, fostering a sense of security and dignity during difficult times.
Recent advancements in comfort treatment underscore the importance of tailored approaches. Innovative practices, such as nature-based therapeutic interventions, have been shown to alleviate distress for seriously ill patients and their families, as evidenced by recent case studies. Statistics reveal that in-home supportive treatment significantly improves quality of life, with many clients reporting reduced symptoms and increased satisfaction with their care. According to the U.S. Centers for Medicare & Medicaid Services, there has been a 2.5% increase in Medicare payments for supportive services, reflecting a growing recognition of their value.
By focusing on the holistic needs of clients, Happy to Help Caregiving ensures that individuals receive not only medical support but also emotional and social engagement, which are vital for overall health and happiness. Family caregivers are encouraged to actively participate in the support process, advocating for their loved ones’ needs and preferences to maximize the benefits of these essential services.
Quality of Life: The Core Goal of Palliative Care
The main challenge in caregiving is ensuring quality end-of-life support through palliative care Philadelphia for individuals and their families. Many caregivers struggle with the emotional, social, and spiritual dimensions of well-being, which can be overlooked in traditional medical approaches. This lack of comprehensive support can lead to diminished quality of life for patients, even as they face serious illness.
Supportive treatment addresses these challenges by focusing on the individual’s overall health. It promotes dignity and comfort, allowing patients to engage in meaningful activities and maintain vital relationships. Research indicates that early incorporation of supportive treatment significantly enhances health-related quality of life, with an effect size of 0.33. This approach not only decreases unnecessary hospital admissions but also improves symptom management.
For instance, 25.7 million individuals require end-of-life support, and those receiving this assistance report improved emotional well-being and the achievement of personal objectives-key elements of their quality of life. Healthcare experts emphasize that a comprehensive approach to palliative care in Philadelphia meets medical needs while honoring the personal values and choices of patients.
Dr. Lori Wiener notes, 'The aim of palliative care Philadelphia is to reduce symptoms and improve quality of life,' while Dr. Matthew DeCamp adds that 'palliative care Philadelphia is a comprehensive approach to medicine and caregiving.' This thorough emphasis ultimately results in a more compassionate and effective support experience.
Conditions Requiring Palliative Care: Understanding the Need
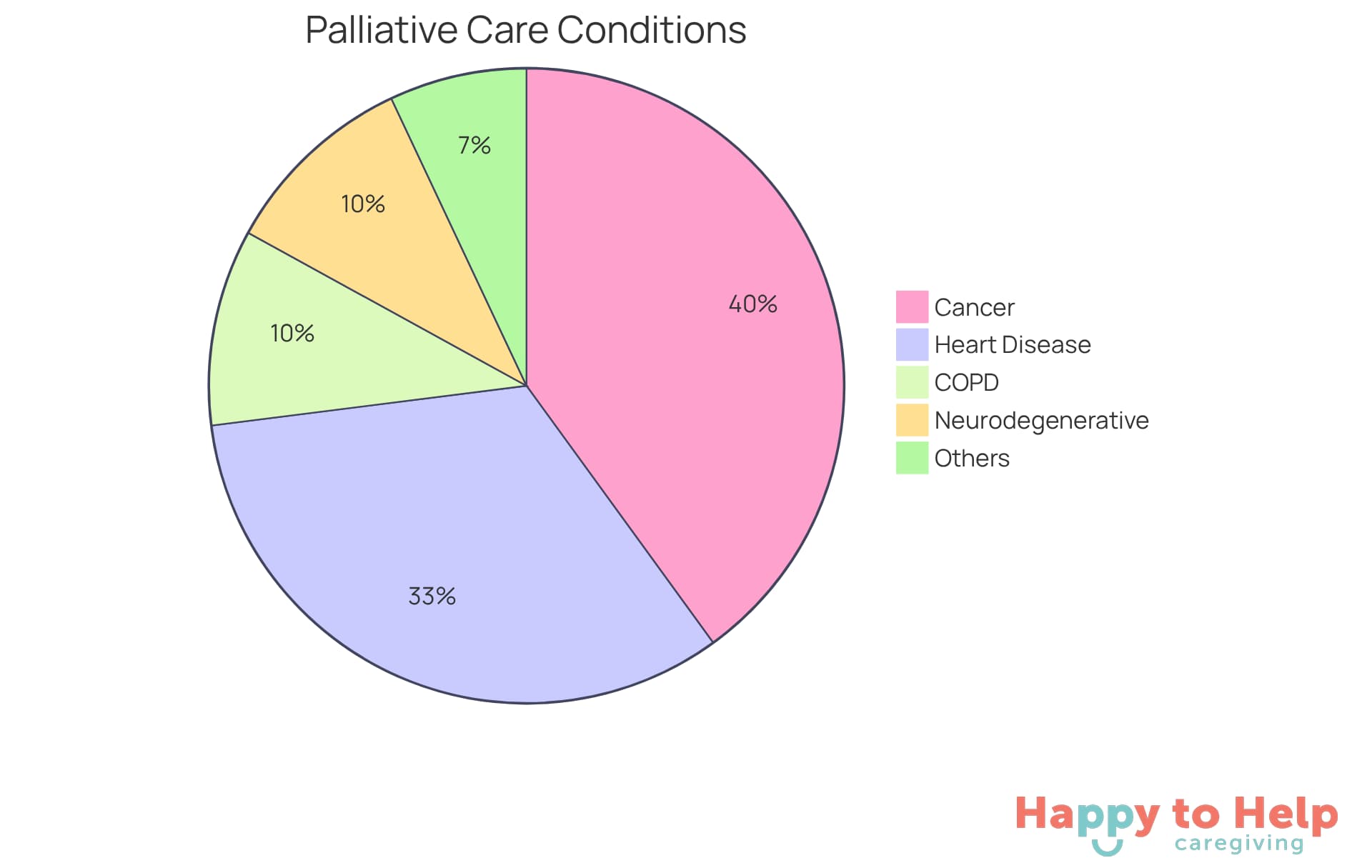
Palliative care Philadelphia is crucial for individuals grappling with serious illnesses like cancer, heart disease, COPD, and neurodegenerative disorders such as Alzheimer's and Parkinson's disease. However, many caregivers face challenges in recognizing the need for supportive treatment, which can significantly enhance quality of life and effectively manage symptoms at any stage of illness.
Statistics reveal that approximately 12 million adults in the U.S. suffer from severe conditions that could benefit from palliative care, a number projected to double by 2050. Among these, cancer and heart disease are prevalent; nearly 40% of those requiring comfort measures are diagnosed with cancer, while one-third are affected by heart disease. This highlights a pressing issue: the need for caregivers to proactively address these supportive care requirements.
To tackle this challenge, caregivers should engage in open discussions with healthcare providers in Philadelphia about palliative care Philadelphia treatment options early in the process. Case studies demonstrate that integrating comfort services early not only alleviates symptoms but also enhances overall well-being, leading to fewer hospital admissions and increased patient satisfaction. As the demand for supportive services rises, especially among the elderly, it’s essential for caregivers to recognize and address these needs effectively.
Interdisciplinary Team: Collaborative Care in Palliative Services
Palliative support often faces the challenge of fragmented care, where individuals may receive treatment from various providers without a cohesive strategy. This can lead to gaps in addressing not only medical needs but also emotional and spiritual support, leaving caregivers feeling overwhelmed and unsure of how to proceed.
To tackle this issue, a collaborative team approach is essential. This team may include:
- doctors
- nurses
- social workers
- chaplains
All working together to ensure that every aspect of an individual's care is considered. By developing a unified treatment plan that aligns with the individual's goals and preferences, caregivers can enhance the overall experience for those they support.
Implementing this cooperative method not only improves communication among team members but also fosters a more holistic approach to care. Caregivers can feel more confident knowing that they are part of a system that prioritizes the well-being of the individual, ultimately leading to better outcomes.
Emotional Support: A Pillar of Palliative Care
Emotional distress is a significant challenge faced by individuals and their loved ones during end-of-life treatment. The difficulties of severe illness can lead to feelings of anxiety and isolation, making it essential for caregivers to step in. Without proper emotional support, both patients and caregivers may struggle to cope with the situation, which can hinder their overall well-being.
To address this issue, caregivers can provide vital emotional support through a few key actions:
- Offering a listening ear
- Providing companionship
- Giving reassurance
By implementing these actions, caregivers can help alleviate feelings of anxiety and isolation. This support not only fosters resilience but also encourages a more positive outlook during these challenging times.
Incorporating these practices can make a significant difference. Caregivers should prioritize open communication, actively listen to concerns, and create a comforting environment. These steps can enhance the emotional well-being of both the caregiver and the individual receiving care.
Personalized Care Plans: Tailoring Palliative Support
Problem: End-of-life support often lacks personalization, which can lead to dissatisfaction among patients and their families. Many caregivers struggle to meet the unique needs of individuals during this critical time.
Agitate: When treatment plans do not cater to individual preferences, it can result in a diminished quality of life. Patients may feel overlooked, and their specific desires for comfort and dignity can go unmet. This not only affects their well-being but also places additional stress on caregivers who want to provide the best support possible.
Solution: Customized treatment plans are essential in end-of-life support. These plans are developed through collaboration among the individual, family, and support team, ensuring that every aspect of treatment aligns with the individual's preferences. This tailored approach boosts the effectiveness of palliative care Philadelphia provides and significantly enhances the quality of life for individuals.
Research shows that individuals receiving personalized treatment strategies report higher satisfaction levels. Many express appreciation for the focus on their unique situations. For instance, a notable case involved a patient who managed symptoms effectively while maintaining dignity and comfort in their final days through a personalized plan.
Palliative care Philadelphia specialists emphasize that understanding and adapting to personal needs is crucial for creating a supportive atmosphere. This approach leads to improved outcomes and a more compassionate experience for everyone involved.
Local Resources: Accessing Palliative Care in Philadelphia
In Philadelphia, caregivers face the challenge of navigating a complex healthcare landscape, especially when it comes to palliative care Philadelphia. Many families struggle to find adequate support for their loved ones, which can lead to increased stress and uncertainty during difficult times.
Statistics reveal that a significant portion of hospital admissions could be managed through outpatient support. Research indicates that 51% of admissions in regional healthcare systems might have been prevented with better outpatient management strategies. This underscores the importance of utilizing local resources to effectively address these challenges.
Fortunately, Philadelphia offers a diverse array of supportive resources, including palliative care Philadelphia, hospitals, home health agencies, and specialized providers. Institutions like Temple Health, Penn Medicine, and Redeemer Health provide extensive services tailored to meet the unique needs of individuals and their families. For instance, Redeemer Health's comfort support team collaborates closely with patients to manage symptoms and enhance their quality of life by providing palliative care in Philadelphia and in various settings, such as at home and in hospice facilities.
By leveraging these outpatient supportive services, families can ensure their loved ones receive compassionate care that aligns with their specific requirements. Moreover, studies show that incorporating these services is linked to better survival rates and reduced unnecessary healthcare resource usage, highlighting their critical role in improving patient outcomes.
In summary, caregivers in Philadelphia can benefit from the expertise of local providers in palliative care Philadelphia, ensuring that their loved ones receive the customized assistance they need during challenging times. Utilizing available resources not only alleviates the burden on families but also enhances the overall quality of care.
Technology Integration: Enhancing Palliative Care Delivery
The challenge of delivering effective palliative care Philadelphia support is significant. Caregivers often struggle with communication barriers, which can hinder timely interventions and access to treatment. This lack of effective communication can lead to increased stress for both caregivers and patients, ultimately affecting the quality of palliative care in Philadelphia.
Fortunately, technology offers practical solutions to these challenges. Tools like telemedicine, electronic health records, and mobile health applications enhance communication among individuals, families, and healthcare teams. By facilitating prompt interventions and improving access to treatment, these technologies enable more effective management of symptoms. As a result, caregivers can achieve better outcomes for those they support.
Caregiver Training: Ensuring Quality in Palliative Care
Caregivers in palliative assistance face a significant challenge: the lack of adequate training. Without proper education, they may struggle to provide the high-quality support that patients and their families need during difficult times. This gap in training can lead to misunderstandings, ineffective communication, and ultimately, a lower quality of care.
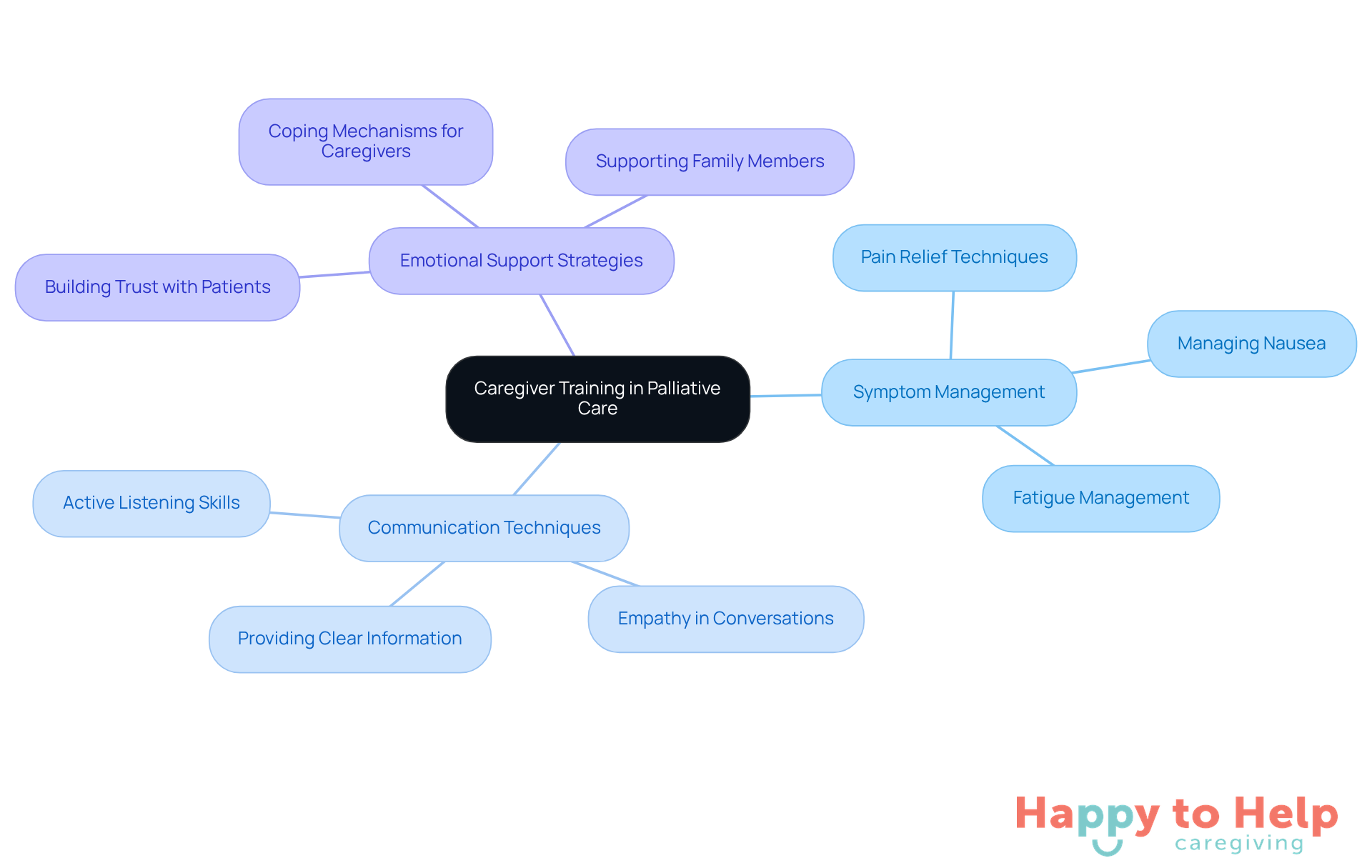
To address this issue, organizations must prioritize support provider training. Training programs should cover essential topics such as:
- Symptom management
- Communication techniques
- Emotional support strategies
By investing in these educational initiatives, organizations can empower caregivers with the skills and knowledge necessary to enhance the overall quality of support offered to individuals and their relatives.
In summary, effective caregiver training is not just beneficial; it is essential for improving palliative care in Philadelphia. By equipping caregivers with the right tools, we can ensure that they are prepared to meet the complex needs of those they serve.
Family Impact: The Benefits of Palliative Care Services
Caregivers often face significant challenges, including high levels of stress and emotional strain. The lack of adequate support can lead to feelings of helplessness and confusion during difficult times. This is where palliative care Philadelphia services come into play, providing a solution that addresses these pressing issues.
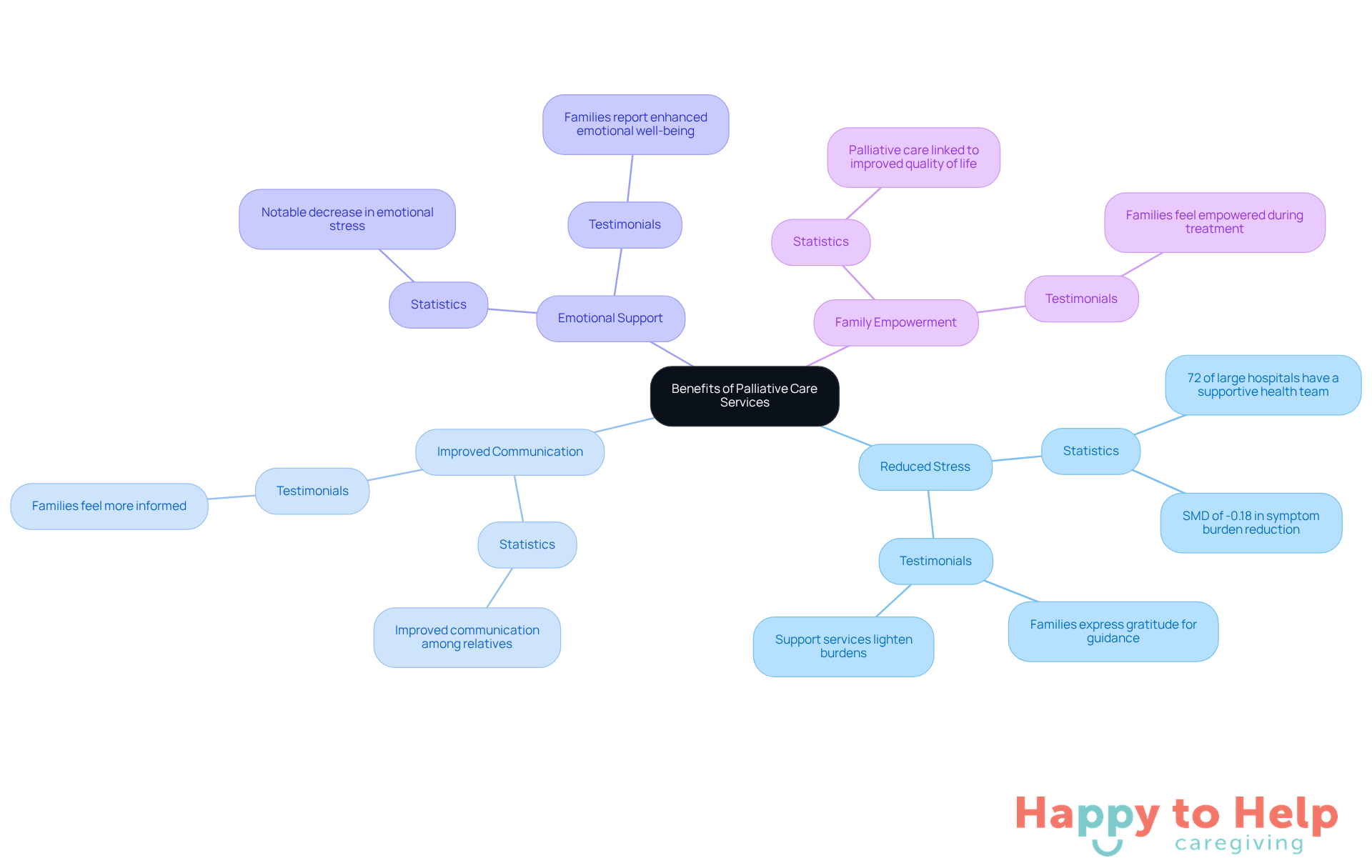
Palliative support services provide numerous advantages for families. They help reduce stress, improve communication, and enhance emotional support. By catering to the needs of both patients and their loved ones, these services foster a nurturing environment that strengthens connections among family members. Families frequently report feeling more empowered and informed about their loved one's treatment, which leads to a more positive experience during challenging periods.
Statistics underscore the importance of these services:
- As of 2019, 72% of large hospitals reported having a supportive health team, which significantly improves communication among relatives and access to essential services.
- Supportive treatment has been linked to a notable decrease in symptom burden at 4- to 6-month follow-ups, with a standardized mean difference (SMD) of -0.18.
This reduction helps alleviate anxiety and emotional stress for families.
Testimonials from families highlight the transformative impact of supportive services. Many express gratitude for the guidance and assistance provided, which lightened their burdens and allowed them to focus on quality moments with their loved ones. This holistic approach not only enhances the quality of life for patients but also significantly improves family dynamics, making palliative care Philadelphia an invaluable resource for those navigating serious health challenges.
Key Takeaways for Caregivers
Palliative care presents a significant challenge for families dealing with serious health conditions. The emotional, social, and spiritual complexities can be overwhelming, often leaving caregivers feeling isolated and unsure of how to provide the best support. This is where palliative care steps in as a vital resource, addressing not just the physical needs of patients but also their emotional and spiritual well-being.
By integrating services like symptom management and personalized care plans, palliative care providers in Philadelphia offer a holistic support system that enhances the overall quality of life for both patients and their families. Early intervention is crucial; studies show that families who engage with palliative care sooner experience less stress and better outcomes. Additionally, interdisciplinary teams play a key role in delivering comprehensive care, ensuring that all aspects of a patient's needs are met.
As the demand for palliative care rises, it’s essential for caregivers to actively seek these services. Doing so can alleviate the burdens associated with serious illness, fostering an environment of compassion and dignity. Embracing palliative care not only benefits individuals facing health challenges but also strengthens family bonds, leading to a more fulfilling experience during difficult times.
In summary, palliative care is not just about managing symptoms; it’s about enhancing the quality of life. By recognizing the importance of emotional support and utilizing local resources, families can navigate these challenges more effectively. Remember, seeking help is a sign of strength, and palliative care can provide the necessary support when it matters most.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5MjI2NTE0YWNkMDUyNjc3Yjk4NWRiMCIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What challenges do caregivers face when supporting clients with severe health conditions?
Caregivers often experience feelings of helplessness and stress, which can negatively impact both themselves and their clients.
What services does Happy to Help Caregiving provide?
Happy to Help Caregiving offers a range of supportive services including symptom management, emotional support, and assistance with daily activities, all delivered in the comfort of the client’s home.
How does Happy to Help Caregiving ensure compassionate support?
Caregivers are specially trained to provide compassionate support that meets both physical and emotional needs, promoting a sense of security and dignity for clients during difficult times.
What recent advancements have been made in palliative care?
Recent advancements include tailored approaches such as nature-based therapeutic interventions, which have been shown to alleviate distress for seriously ill patients and their families.
What impact does in-home supportive treatment have on clients?
In-home supportive treatment significantly improves quality of life, with many clients reporting reduced symptoms and increased satisfaction with their care.
How does palliative care address the emotional, social, and spiritual dimensions of well-being?
Palliative care focuses on the individual’s overall health, promoting dignity and comfort, and allowing patients to engage in meaningful activities and maintain vital relationships.
What statistics highlight the need for palliative care?
Approximately 12 million adults in the U.S. suffer from severe conditions that could benefit from palliative care, a number projected to double by 2050.
What types of serious illnesses require palliative care?
Palliative care is crucial for individuals with serious illnesses such as cancer, heart disease, COPD, and neurodegenerative disorders like Alzheimer's and Parkinson's disease.
How can caregivers recognize the need for palliative care?
Caregivers should engage in open discussions with healthcare providers about palliative care treatment options early in the illness process to better recognize and address supportive care needs.
What are the benefits of integrating comfort services early in the treatment process?
Early integration of comfort services can alleviate symptoms, enhance overall well-being, lead to fewer hospital admissions, and increase patient satisfaction.
List of Sources
- Happy to Help Caregiving: Palliative Support Care Services
- Palliative Care News Archives (https://hospicenews.com/category/palliative-care-news)
- Palliative Care Articles & News (https://capc.org/about/press-media/articles-news)
- Palliative Care Statistics (https://rosewood-nursing.com/post/palliative-care-statistics)
- Home-Based Care Providers Reap Benefits Of Palliative Care – But Broader Adoption Hinges On Reform (https://homehealthcarenews.com/2025/11/home-based-care-providers-reap-benefits-of-palliative-care-but-broader-adoption-hinges-on-reform)
- Quality of Life: The Core Goal of Palliative Care
- Support for Serious Illness (https://newsinhealth.nih.gov/2025/07/support-serious-illness)
- Palliative care (https://who.int/news-room/fact-sheets/detail/palliative-care)
- ‘A good death’: How compassionate care helps people navigate the end of life (https://news.yale.edu/2025/10/13/good-death-how-compassionate-care-helps-people-navigate-end-life)
- Quality of Life in Palliative Care - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC6405258)
- Palliative Care and Patient and Caregiver Outcomes (https://jamanetwork.com/journals/jama/fullarticle/2585979)
- Conditions Requiring Palliative Care: Understanding the Need
- Palliative Care Statistics (https://rosewood-nursing.com/post/palliative-care-statistics)
- Center to Advance Palliative Care Facts and Stats - Tuesday Health (https://tuesdayhealth.com/palliative-care-facts-and-stats)
- Palliative care (https://who.int/news-room/fact-sheets/detail/palliative-care)
- Demand for specialised medical care to ease suffering is surging (https://euronews.com/health/2025/02/27/demand-for-palliative-care-is-surging-worldwide-as-people-live-longer-but-unhealthier-live)
- Emotional Support: A Pillar of Palliative Care
- End Of Life Care Quotes (16 quotes) (https://goodreads.com/quotes/tag/end-of-life-care)
- Palliative Care Statistics (https://rosewood-nursing.com/post/palliative-care-statistics)
- The Importance of Emotional Support in Palliative Care (https://helpinghandshomecare.co.uk/care-advice/the-importance-of-emotional-support-in-palliative-care)
- Understanding the Role of Palliative Care in Advanced Illness Management (https://news.cuanschutz.edu/graduate-school/understanding-the-role-of-palliative-care-in-advanced-illness-management)
- Regence BlueShield Releases Findings on the Importance of a Holistic Approach to Palliative Care (https://news.regence.com/releases/regence-blueshield-releases-findings-on-the-importance-of-a-holistic-approach-to-palliative-care)
- Personalized Care Plans: Tailoring Palliative Support
- The Christie Enhanced Supportive Care Initiative; ’Supportive care makes excellent cancer care possible’ - Quality in Care Awards Programme (https://qualityincare.org/case\_studies/the\_christie\_enhanced\_supportive\_care\_initiative\_supportive\_care\_makes\_excellent\_cancer\_care\_possible)
- Here are 11 Inspiring Quotes to Help You Rethink End of Life Care (https://easylivingfl.com/assisted-living/11-inspiring-quotes-to-help-you-rethink-end-of-life-care)
- The Effectiveness of Palliative Care Interventions in Long-Term Care Facilities: A Systematic Review - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC11277722)
- Case Studies (https://savvyseniorshousing.com/Case\_Studies.html)
- The Midhurst Macmillan community specialist palliative care team - Quality in Care Awards Programme (https://qualityincare.org/case\_studies/the\_midhurst\_macmillan\_community\_specialist\_palliative\_care\_team)
- Local Resources: Accessing Palliative Care in Philadelphia
- Gale - Institution Finder (https://go.gale.com/ps/i.do?id=GALE%7CA98135737&sid=googleScholar&v=2.1&it=r&linkaccess=abs&issn=10715568&p=AONE&sw=w)
- Palliative Care | Redeemer Health (https://redeemerhealth.org/services/health-care/palliative-care)
- Utilization of palliative care resource remains low, consuming potentially avoidable hospital admissions in stage IV non-small cell lung cancer: a community-based retrospective review - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC9661463)
- CAPC Announces The Return of Its National Seminar - CAPC - Press Rease (https://capc.org/about/press-media/press-releases/2025-2-3/center-to-advance-palliative-care-announces-the-return-of-its-national-seminar)
- Technology Integration: Enhancing Palliative Care Delivery
- Identification of Digital Health Priorities for Palliative Care Research: Modified Delphi Study (https://aging.jmir.org/2022/1/e32075)
- Telehealth-facilitated palliative care enables more people to die at home: An analysis of clinical outcomes and service activity data - BMC Palliative Care (https://bmcpalliatcare.biomedcentral.com/articles/10.1186/s12904-024-01622-0)
- Telemedicine Utilization in the Ambulatory Palliative Care Setting: Are There Disparities? (https://sciencedirect.com/science/article/pii/S0885392421005649)
- CAPC’s Andrew Esch: Palliative Care Delivery ‘Maturing into Innovation’ (https://hospicenews.com/2025/11/19/capcs-andrew-esch-palliative-care-delivery-maturing-into-innovation)
- ‘Technology in end-of-life care is very important’: the view of nurses regarding technology and end-of-life care (https://springermedizin.de/technology-in-end-of-life-care-is-very-important-the-view-of-nur/50588762)
- Caregiver Training: Ensuring Quality in Palliative Care
- Family Caregiver Support, Education Needs Growing (https://hospicenews.com/2025/11/11/family-caregiver-support-education-needs-growing)
- (PDF) Effectiveness of symptom management training on caregiving preparedness and burden of family caregivers in-home palliative care: a quasiexperimental study (https://researchgate.net/publication/365453238\_Effectiveness\_of\_symptom\_management\_training\_on\_caregiving\_preparedness\_and\_burden\_of\_family\_caregivers\_in-home\_palliative\_care\_a\_quasiexperimental\_study)
- Caregiver training: Evidence of its effectiveness for cognitive and functional improvement in older adults - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10078788)
- 27 Inspirational Quotes for Caregivers (https://ultimatecareny.com/resources/27-quotes-for-caregivers)
- 20 Caregiver Quotes That Will Inspire You - MD Home Health (https://mdhomehealth.com/2018/06/10/20-caregiver-quotes-that-will-inspire-you)
- Family Impact: The Benefits of Palliative Care Services
- WHO EMRO - Palliative care: easing suffering, supporting families (https://emro.who.int/media/news/palliative-care-easing-suffering-supporting-families.html)
- Center to Advance Palliative Care Facts and Stats - Tuesday Health (https://tuesdayhealth.com/palliative-care-facts-and-stats)
- Palliative Care and Patient and Caregiver Outcomes (https://jamanetwork.com/journals/jama/fullarticle/2585979)
- End-Of-Life Care Statistics (https://rosewood-nursing.com/post/end-of-life-care-statistics)

