
For families in our service areas
For families in our service areas, this guide explains caregiver support and how non-medical in-home caregiving can support care planning in East Idaho, Treasure Valley & Magic Valley, Northern Wasatch, North Central West Virginia, and Northeast Ohio.
Why PAD Risk Factors Every Family Caregiver Matters
Understanding Peripheral Artery Disease (PAD) is essential for family caregivers who are crucial in managing the health of older adults. The problem is that age, smoking, diabetes, and other factors significantly increase the risk of PAD. This places caregivers in a challenging position, as they must recognize and mitigate these risks effectively.
As the prevalence of PAD continues to rise, caregivers face the daunting task of identifying subtle signs and implementing proactive measures. The implications of neglecting these signs can lead to serious health consequences for their loved ones. So, how can caregivers navigate this complex landscape to protect their family members from the dangers of PAD?
To address this issue, caregivers should focus on education and awareness. Here are some actionable strategies:
- Stay Informed: Regularly update your knowledge about PAD and its risk factors.
- Recognize Symptoms: Be vigilant for signs such as leg pain, cramping, or wounds that don’t heal.
- Encourage Healthy Habits: Promote a lifestyle that includes regular exercise, a balanced diet, and smoking cessation.
By equipping themselves with the right information and strategies, caregivers can significantly improve health outcomes for older adults at risk of PAD.
Age as a Primary Risk Factor for PAD
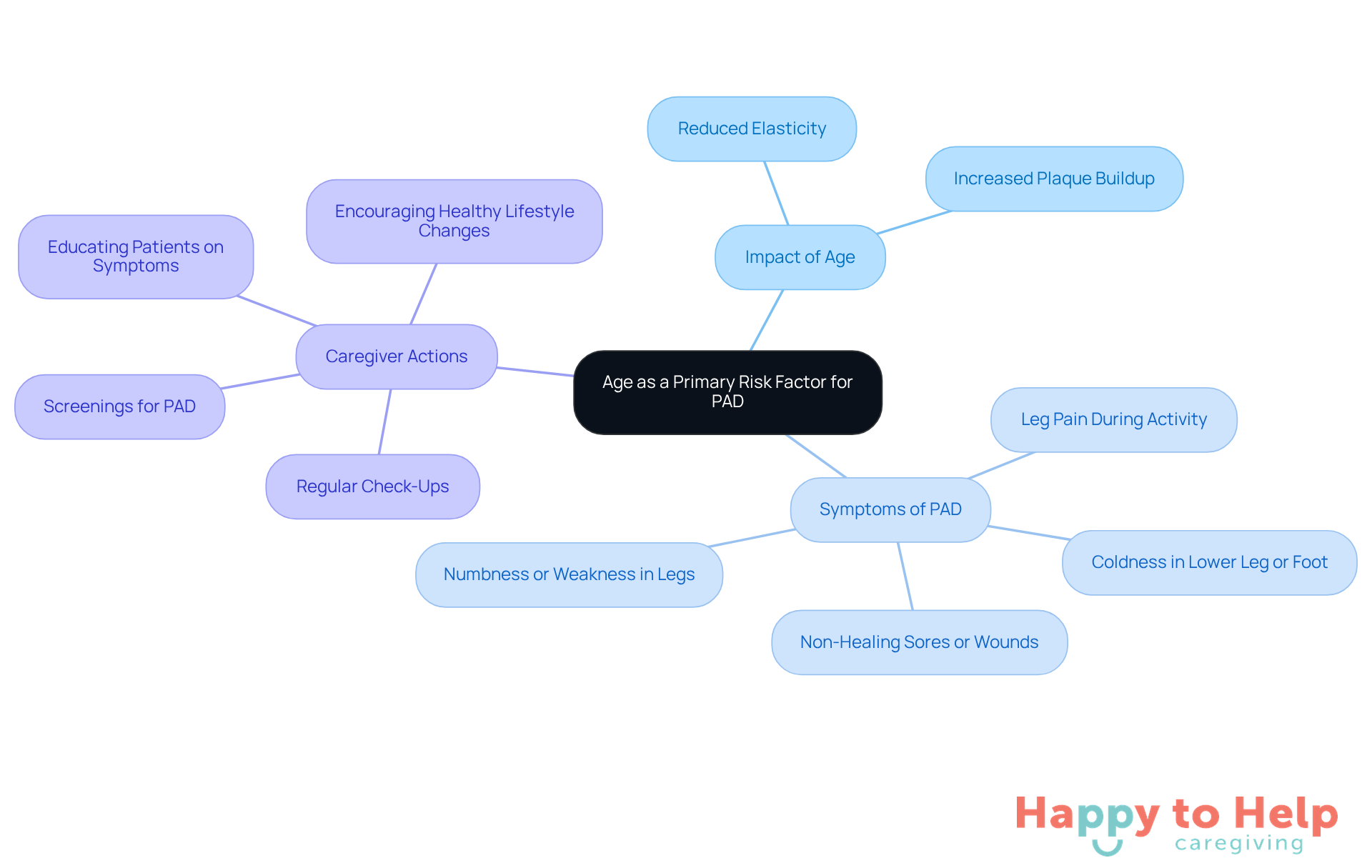
Peripheral Artery Disease (PAD) is a significant concern for older adults, particularly those over 65. The problem escalates with age due to natural changes in blood vessels, such as reduced elasticity and increased plaque buildup. Caregivers must recognize the symptoms of PAD in older individuals, as early detection can lead to improved management and outcomes.
To address this issue, caregivers should prioritize regular check-ups and screenings for PAD. These proactive measures are essential for this demographic, ensuring that any potential complications are caught early. By staying informed and vigilant, caregivers can play a crucial role in enhancing the health and well-being of older adults at risk for PAD risk factors.
Impact of Smoking on PAD Risk
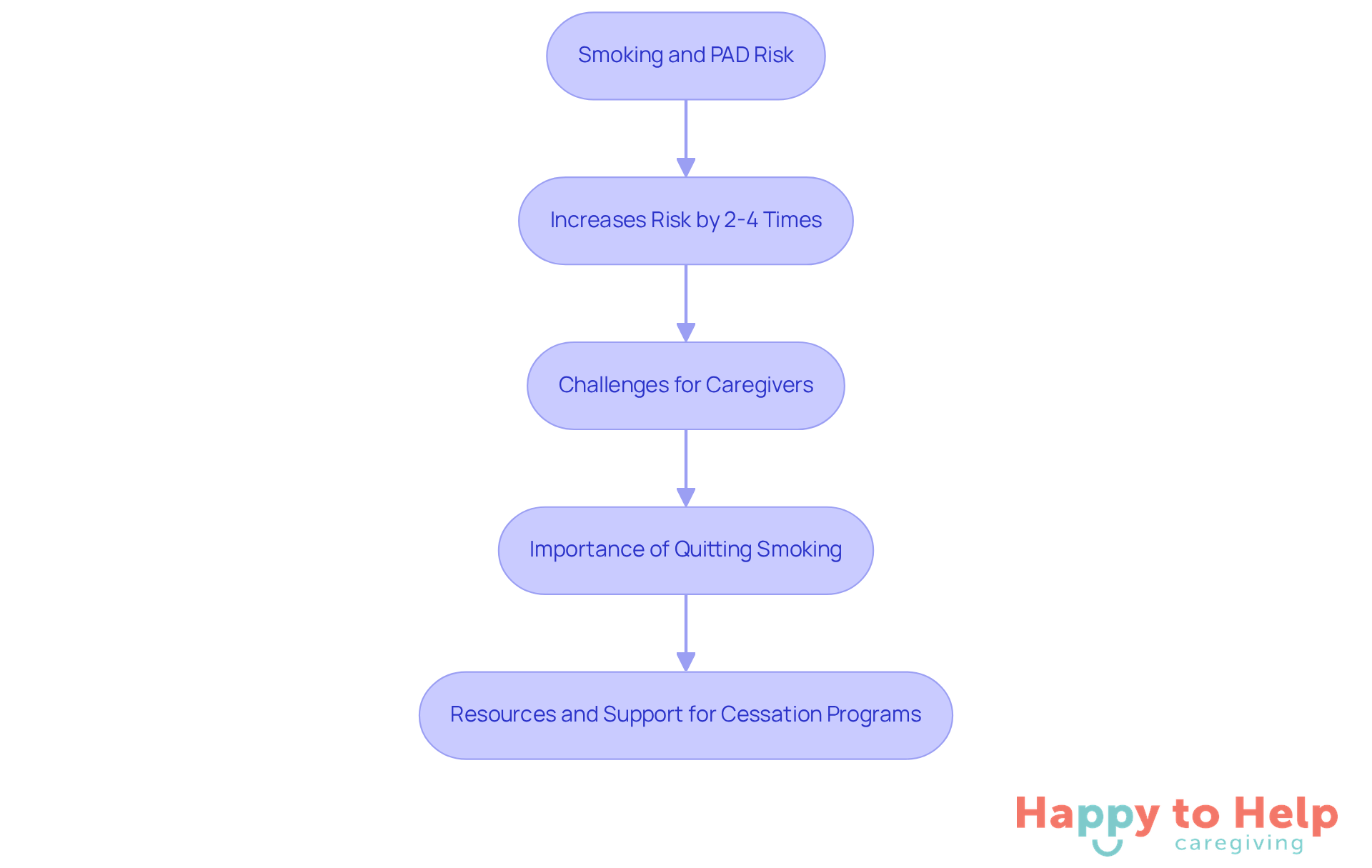
Smoking is a significant problem that contributes to Peripheral Artery Disease (PAD) and is one of the PAD risk factors, increasing the risk of developing the condition by two to four times. The harmful chemicals in tobacco damage blood vessels, leading to atherosclerosis, which can severely impact vascular health.
Caregivers face the challenge of helping individuals understand the importance of quitting smoking. This issue not only affects their health but also complicates their overall well-being. Therefore, it’s crucial for caregivers to motivate individuals to stop smoking.
To address this, caregivers can offer resources and assistance for cessation programs. Providing support and guidance can significantly enhance an individual's vascular well-being, making a real difference in their health journey.
Diabetes and Its Connection to PAD
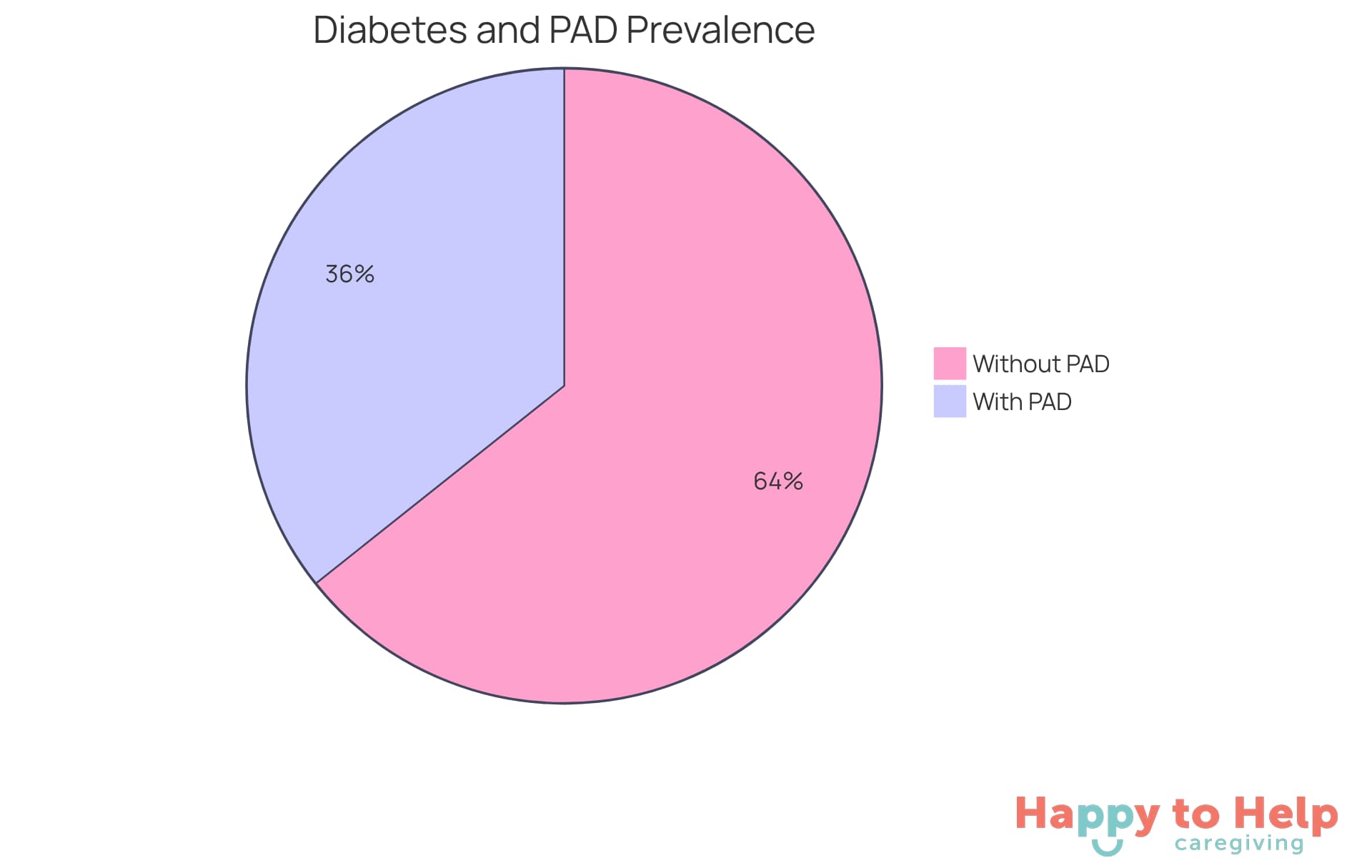
Diabetes significantly increases the pad risk factors associated with developing peripheral artery disease (PAD). Individuals diagnosed with diabetes are more than twice as likely to face this condition. High blood sugar levels lead to vascular damage, which promotes atherosclerosis, a major contributor to the risk factors associated with PAD.
Recent studies reveal that approximately 35.7% of patients with type 2 diabetes mellitus (T2DM) in sub-Saharan Africa have PAD. This statistic underscores the urgent need for effective blood sugar management. Caregivers must prioritize strategies that include:
- Balanced nutrition
- Regular physical activity, such as home-based walking exercises for at least 30 minutes, three days a week
- Strict adherence to prescribed medications
Expert Marc Bonaca points out that many individuals with PAD remain undiagnosed, highlighting the importance of awareness and proactive management. Maintaining ideal blood glucose levels not only reduces pad risk factors but also enhances overall vascular health. Therefore, it's crucial for caregivers to support those they assist in achieving these health goals.
High Blood Pressure as a Contributing Factor to PAD
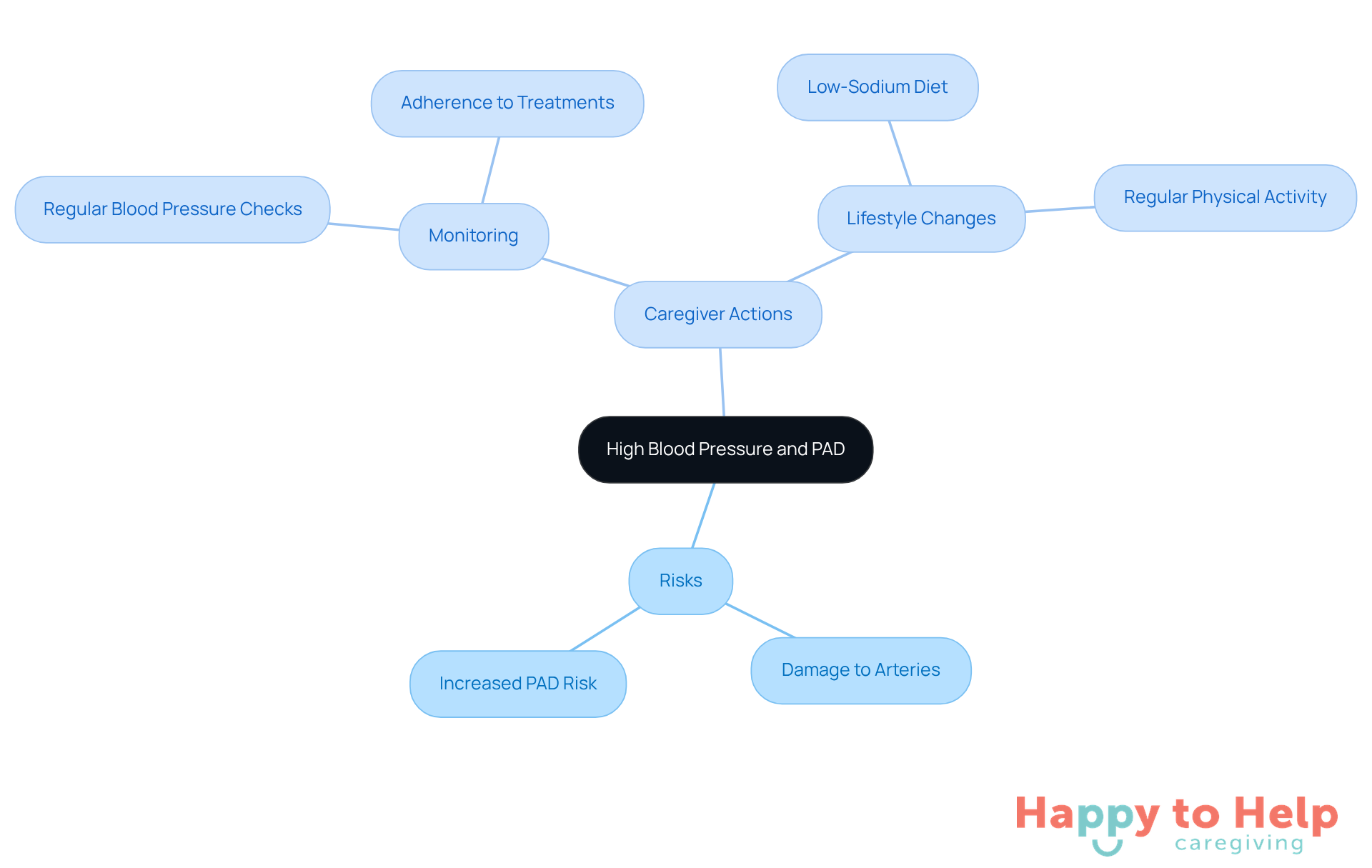
Elevated blood pressure poses a serious problem for individuals who have PAD risk factors for Peripheral Artery Disease (PAD). Over time, high blood pressure can damage arteries, which increases the likelihood of developing PAD risk factors. This situation calls for caregivers to take action.
Caregivers should actively encourage individuals to:
- Monitor their blood pressure regularly
- Adhere to prescribed treatments
By doing so, they can help mitigate the risks associated with hypertension. Additionally, implementing lifestyle changes can significantly aid in managing blood pressure.
Consider adopting:
- A low-sodium diet
- Engaging in regular physical activity
These practical solutions not only help lower blood pressure but also reduce the likelihood of developing PAD risk factors. By focusing on these strategies, caregivers can play a crucial role in promoting better health outcomes.
High Cholesterol Levels and PAD Risk
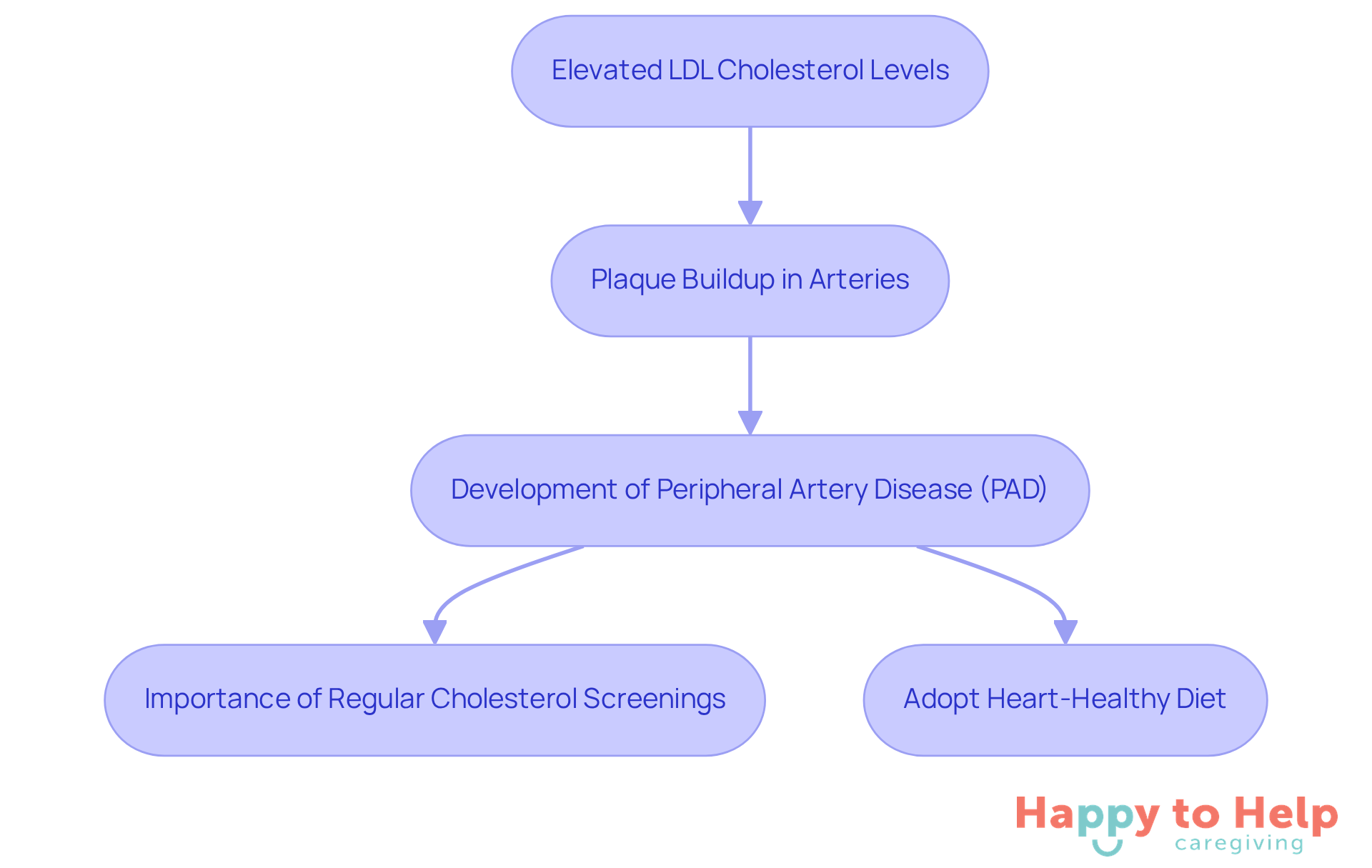
Elevated cholesterol levels, especially low-density lipoprotein (LDL), pose a significant problem as they contribute to the development of peripheral artery disease (PAD) by promoting plaque buildup in the arteries. This issue affects approximately 200 million individuals worldwide, with prevalence increasing with age. Therefore, regular cholesterol screenings are crucial for seniors.
Caregivers play a vital role in addressing this challenge. They should encourage individuals to:
- Undergo cholesterol screenings
- Adopt heart-healthy diets rich in fruits, vegetables, and whole grains while limiting saturated fats
Recent studies indicate that cumulative exposure to elevated LDL cholesterol is an independent contributor among the PAD risk factors in the development of PAD. Notably, the highest quartile of LDL-C burden is significantly linked to new occurrences of PAD, with an odds ratio (OR) of 1.75.
To combat this issue, caregivers can promote understanding of these dietary selections and advocate for regular health examinations. By doing so, they can help decrease the likelihood of PAD risk factors and enhance their patients' overall cardiovascular health.
Obesity as a Risk Factor for PAD
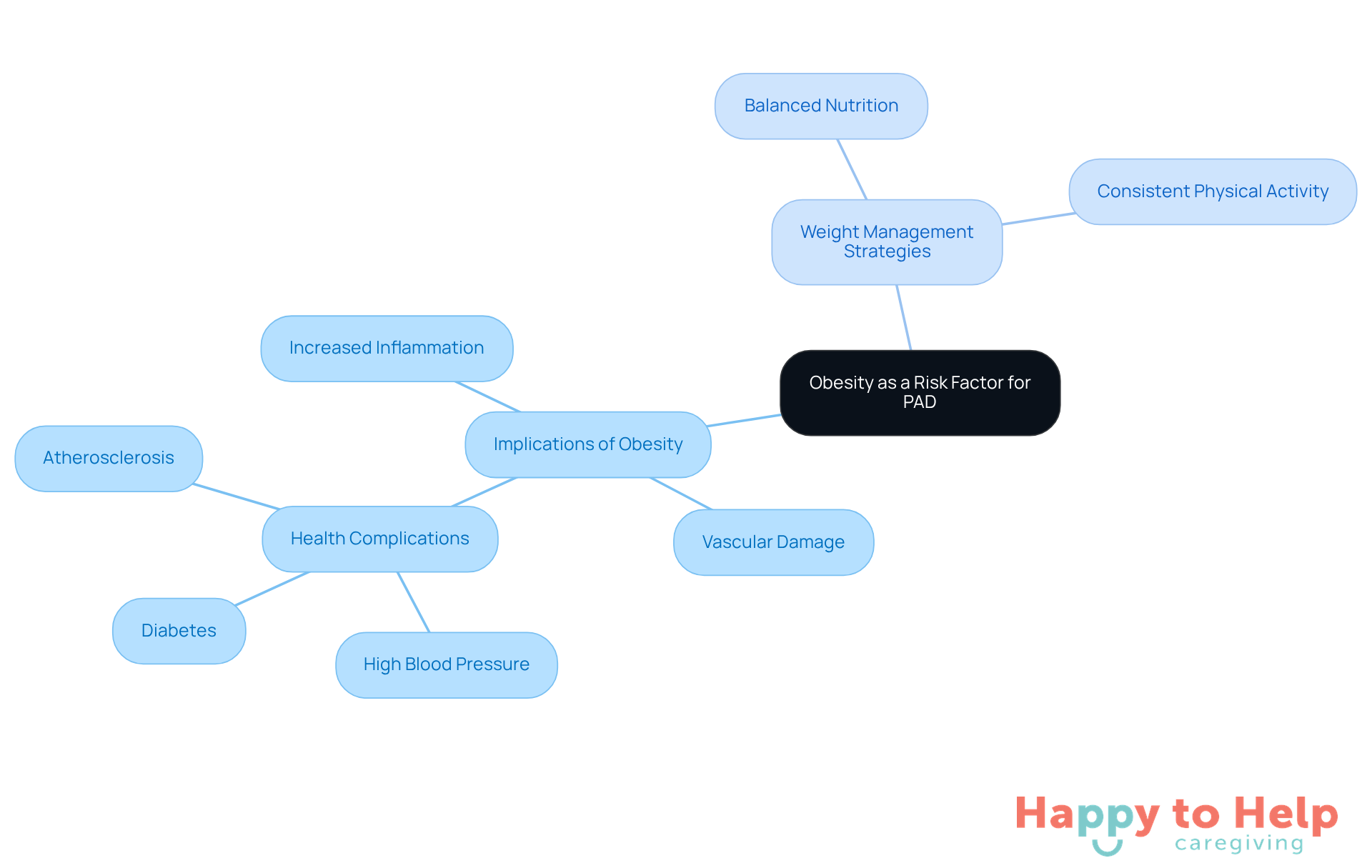
Obesity presents a significant problem, as it is associated with an increased likelihood of PAD risk factors. Excess weight can lead to inflammation and vascular damage, increasing the risk of serious health complications.
For caregivers, this connection underscores the importance of addressing weight management with their clients. The implications of obesity extend beyond just physical appearance; they can severely impact overall health and quality of life.
To combat this issue, caregivers should collaborate with clients to develop individualized weight management strategies. These strategies should focus on:
- Balanced nutrition
- Consistent physical activity
By implementing these solutions, caregivers can greatly lower the likelihood of PAD risk factors and enhance their clients' health outcomes.
Sedentary Lifestyle and Its Effect on PAD Risk
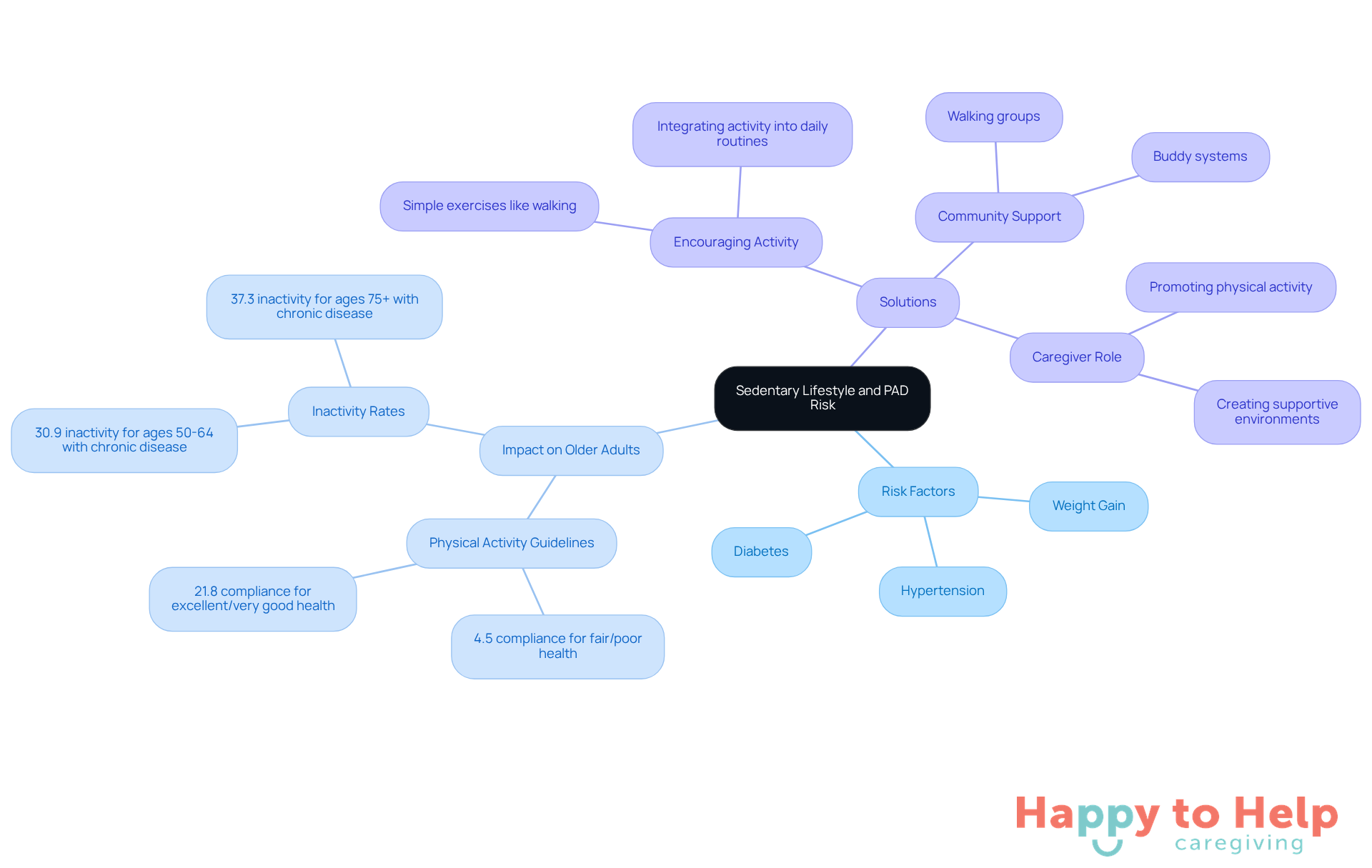
A sedentary lifestyle is one of the significant PAD risk factors that contribute to the development of Peripheral Artery Disease (PAD). This lifestyle can lead to weight gain, hypertension, and diabetes, which are key PAD risk factors for this condition. Studies indicate that older individuals who engage in regular physical activity are less likely to face these medical issues. For instance, only 4.5% of older adults who rated their well-being as fair or poor met the federal physical activity guidelines, compared to 21.8% of those who reported excellent or very good well-being. This stark contrast underscores the essential role of physical activity in maintaining vascular health.
Caregivers face the challenge of encouraging clients to incorporate regular physical activity into their daily routines. Simple activities like walking or gentle exercises can significantly improve circulation and overall well-being. Evidence shows that older adults with at least one chronic disease are less active, with inactivity rates soaring to 30.9% for those aged 50-64. Therefore, creating an environment that promotes movement is crucial.
Community support systems, such as walking groups and buddy systems, can enhance motivation and adherence to physical activity. By fostering social interactions, these initiatives not only improve physical health but also contribute to better mental well-being. Caregivers can play a pivotal role in promoting these activities, helping to mitigate the challenges associated with a sedentary lifestyle and supporting the overall health of seniors, particularly in addressing PAD risk factors.
Genetic Factors Influencing PAD Risk
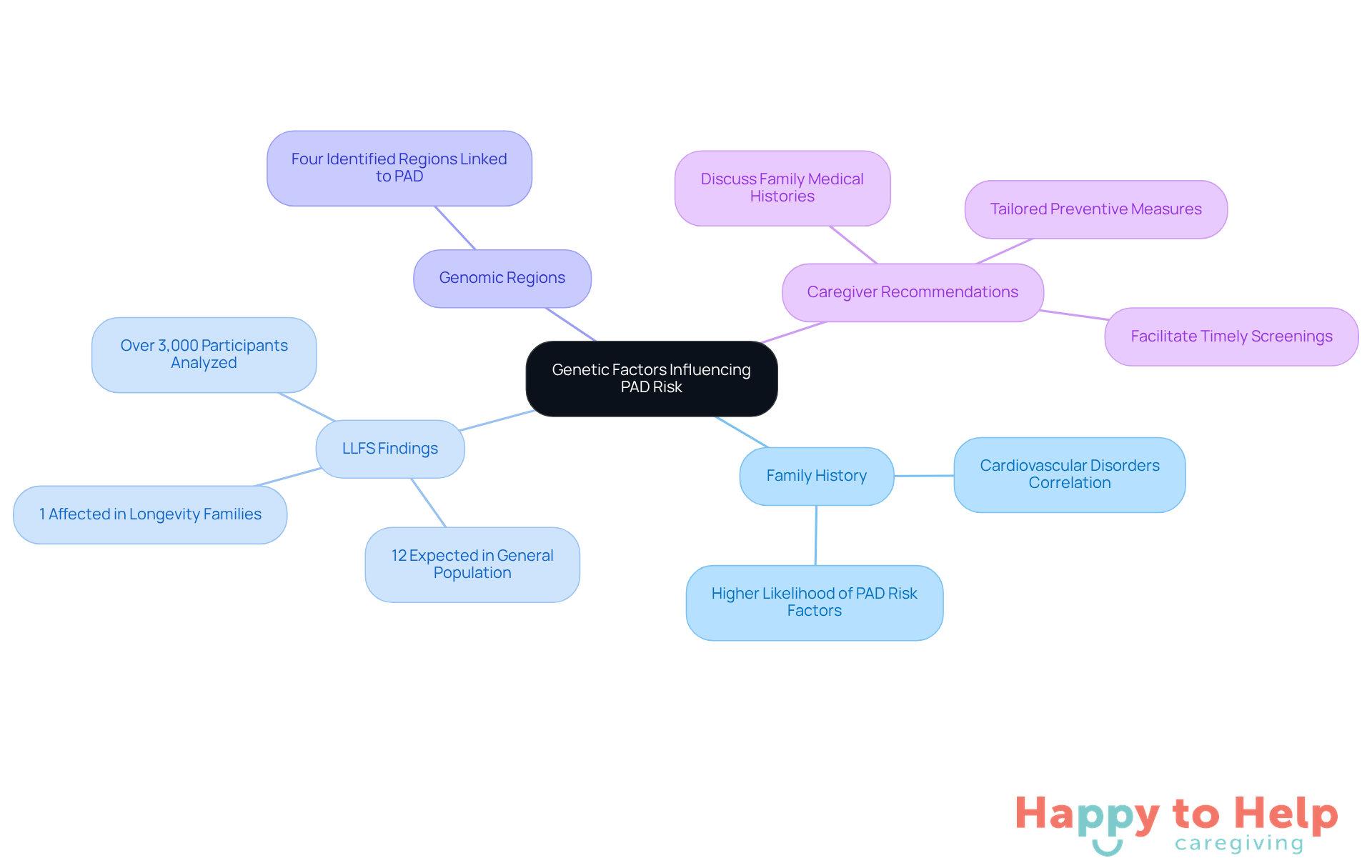
Genetic predisposition significantly affects the PAD risk factors for developing Peripheral Artery Disease (PAD). A family history of cardiovascular disorders often correlates with a higher likelihood of PAD risk factors, which can restrict blood flow to the legs and increase the risk of heart disease, stroke, and mobility issues. This situation underscores the necessity for caregivers to collect comprehensive medical histories from their clients.
Recent findings from the Long Life Family Study (LLFS) reveal that individuals from families with a history of longevity show markedly lower rates of PAD - only 1% of their children are affected, compared to the expected 12% in the general population. This suggests that inherited genetic traits, combined with healthier lifestyle choices, may help in reducing PAD risk factors. Additionally, the study identified four genomic regions linked to PAD risk factors, providing valuable insights for potential prevention strategies.
To address this issue, caregivers should encourage clients to discuss their family medical histories with healthcare professionals. This proactive approach can facilitate timely screenings and tailored preventive measures based on individual health profiles. Understanding the role of family background in PAD risk factors is essential for effective assessment and management in older adults.
Inflammatory Diseases and Their Link to PAD
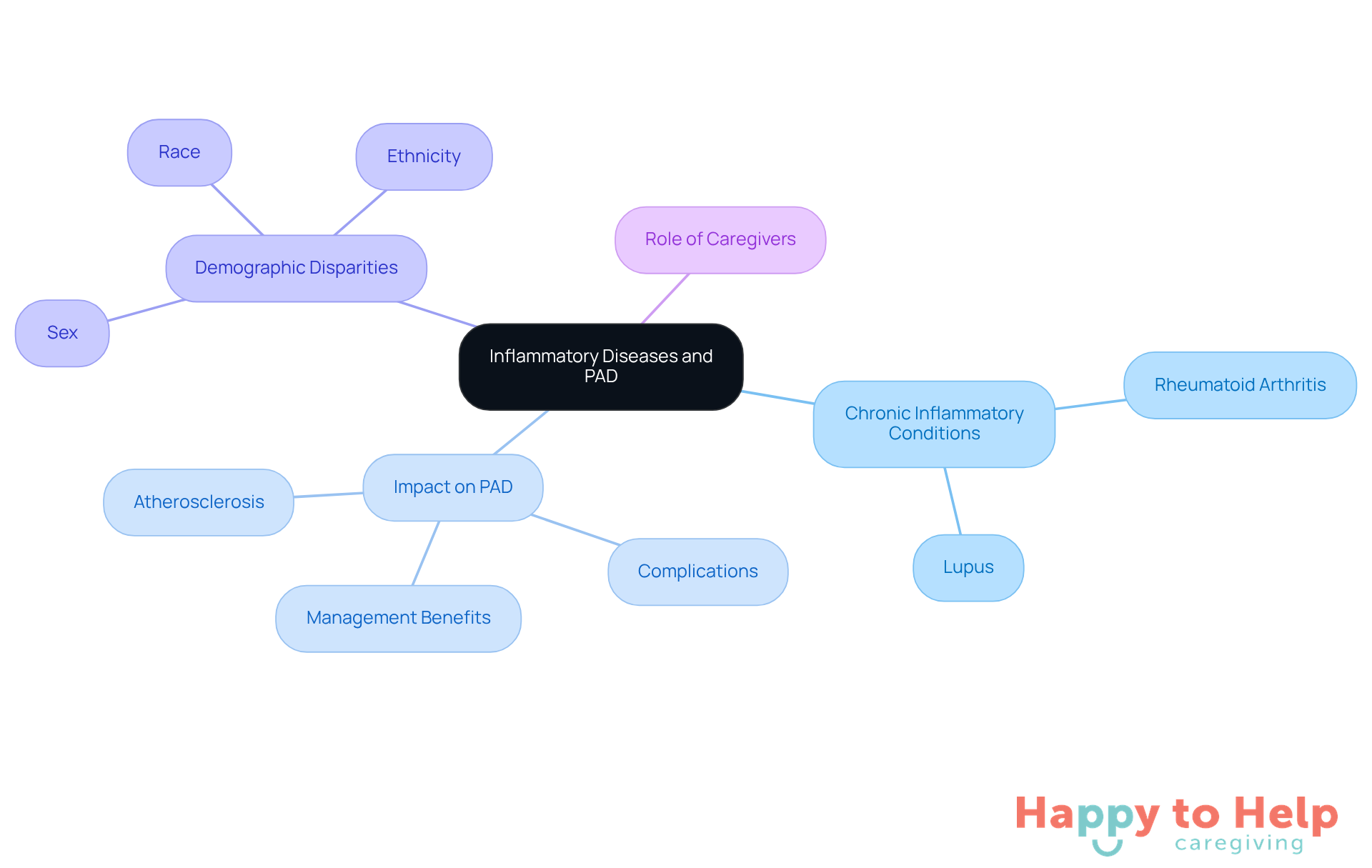
Chronic inflammatory conditions, like rheumatoid arthritis and lupus, pose a significant problem by increasing the likelihood of peripheral artery disease (PAD). These conditions can damage blood vessels, leading to atherosclerosis and other cardiovascular complications. Caregivers must be vigilant about any inflammatory conditions their patients may have, as these can worsen the PAD risk factors.
The implications of unmanaged chronic inflammation are serious. Recent studies show that effectively managing these conditions can improve PAD outcomes. For example, patients with well-controlled inflammatory diseases experience a lower incidence of PAD-related complications. Understanding the link between chronic inflammation and PAD is crucial, especially for older patients who may already be vulnerable due to age-related vascular changes.
Moreover, it's important to note that 50% of patients with PAD also have coronary artery disease or cerebrovascular disease. This statistic underscores the need for comprehensive care strategies. Additionally, the prevalence of PAD varies across sex, race, and ethnicity, with Black American patients being disproportionately affected.
To combat these challenges, caregivers can play a vital role in reducing the PAD risk factors by ensuring that clients receive thorough care for their inflammatory conditions. The American Heart Association emphasizes that social determinants of health significantly impact PAD outcomes, highlighting the necessity for tailored care strategies. By focusing on these areas, caregivers can improve overall well-being and enhance patient outcomes.
Cumulative Risk Factors for Developing PAD
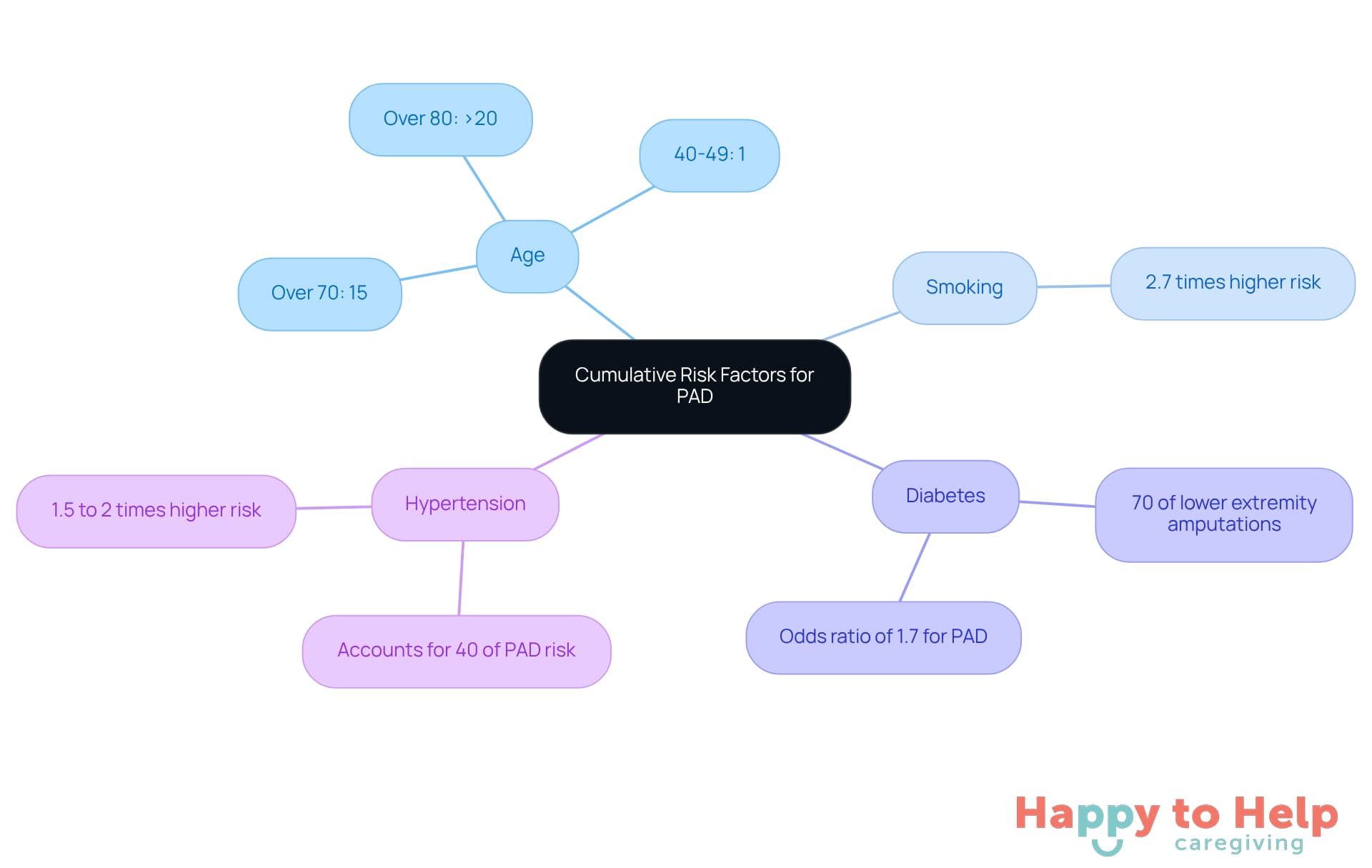
The risk of developing Peripheral Artery Disease (PAD) is a growing concern, particularly due to the PAD risk factors that come into play. The condition is significantly influenced by PAD risk factors such as age, smoking, diabetes, and high blood pressure. For example:
- Individuals over 70 years old have a prevalence of about 15% for PAD.
- Those aged 40 to 49 see rates as low as 1%.
- After age 60, the prevalence rises sharply, exceeding 20% in people over 80.
Smoking can nearly double the PAD risk factors, increasing the likelihood by 2.7 times compared to non-smokers. Additionally, diabetes plays a crucial role, accounting for approximately 70% of lower extremity amputations in the U.S., with an odds ratio of 1.7 related to PAD risk factors. Caregivers face the challenge of addressing these risk factors effectively.
To combat this issue, implementing a comprehensive care strategy is essential. This should include lifestyle modifications such as:
- Promoting regular exercise
- Healthy eating
- Routine health screenings
Collaborating with healthcare providers is vital to ensure that all potential contributing factors, especially the PAD risk factors related to hypertension, are considered, particularly since hypertension contributes to roughly 40% of PAD vulnerability.
The American Heart Association/American College of Cardiology (AHA/ACC) guidelines stress the importance of measuring the ankle-brachial index (ABI) in individuals at increased risk of PAD, even in the absence of symptoms. This holistic approach not only aids in preventing PAD but also enhances the overall well-being of seniors, fostering a healthier and more active lifestyle.
Key Takeaways for Caregivers
Understanding the key risk factors associated with Peripheral Artery Disease (PAD) is crucial for family caregivers. These caregivers play a pivotal role in supporting the health and well-being of older adults. Recognizing the multifaceted nature of PAD allows caregivers to take proactive steps to mitigate risks, ultimately enhancing the quality of life for those they assist.
Several critical risk factors contribute to the likelihood of developing PAD:
- Age
- Smoking
- Diabetes
- High blood pressure
- High cholesterol levels
- Obesity
- Sedentary lifestyle
- Genetic predisposition
- Chronic inflammatory diseases
Each of these factors significantly increases the risk of PAD, highlighting the need for caregivers to be vigilant and informed. By promoting regular health screenings, encouraging lifestyle changes, and maintaining open communication with healthcare providers, caregivers can effectively address these risks and foster a healthier environment for their clients.
The implications of this knowledge extend beyond individual health; they encompass broader public health considerations. As the prevalence of PAD continues to rise, particularly among older adults, it becomes increasingly important for caregivers to advocate for preventive measures and comprehensive care strategies. By prioritizing education, support, and lifestyle modifications, caregivers can reduce the risk of PAD and empower their clients to lead healthier, more active lives.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5M2Y1MDk0NGM3OGNhYjkzOThjNmZhYiIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What is Peripheral Artery Disease (PAD) and who is primarily affected by it?
Peripheral Artery Disease (PAD) is a significant concern for older adults, particularly those over 65, as the risk escalates with age due to natural changes in blood vessels.
How does age impact the risk of developing PAD?
As individuals age, blood vessels lose elasticity and experience increased plaque buildup, which heightens the risk of developing PAD.
What role do caregivers play in managing PAD in older adults?
Caregivers should prioritize regular check-ups and screenings for PAD in older individuals to ensure early detection and improved management of the condition.
How does smoking affect the risk of PAD?
Smoking significantly increases the risk of developing PAD by two to four times due to the harmful chemicals in tobacco that damage blood vessels and promote atherosclerosis.
What can caregivers do to help individuals quit smoking?
Caregivers can provide resources and assistance for smoking cessation programs and offer support and guidance to motivate individuals to stop smoking.
What is the connection between diabetes and PAD?
Diabetes more than doubles the likelihood of developing PAD, as high blood sugar levels lead to vascular damage and atherosclerosis.
What statistics highlight the prevalence of PAD among individuals with diabetes?
Approximately 35.7% of patients with type 2 diabetes mellitus (T2DM) in sub-Saharan Africa have PAD, indicating a critical need for effective blood sugar management.
What strategies should caregivers prioritize for individuals with diabetes to reduce PAD risk?
Caregivers should promote balanced nutrition, regular physical activity (such as home-based walking exercises for at least 30 minutes, three days a week), and strict adherence to prescribed medications.
Why is awareness and proactive management of PAD important?
Many individuals with PAD remain undiagnosed, making awareness and proactive management essential for reducing risk factors and enhancing overall vascular health.
List of Sources
- Age as a Primary Risk Factor for PAD
- Global, regional, and national trends in peripheral arterial disease among older adults: findings from the global burden of disease study 2021 - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC12075273)
- New Treatments for PAD (2025) (https://cacvi.org/new-treatments-for-pad)
- Long-Lived Families Show Lower Risk for Peripheral Artery Disease | Aging (https://aging-us.com/news-room/long-lived-families-show-lower-risk-for-peripheral-artery-disease)
- Epidemiology, classification, and modifiable risk factors of peripheral arterial disease - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC1994028)
- The Current U.S. Prevalence of Peripheral Arterial Disease (https://hmpgloballearningnetwork.com/site/vdm/current-us-prevalence-peripheral-arterial-disease)
- Impact of Smoking on PAD Risk
- Smoking and Peripheral Artery Disease: A Dangerous Combo | Washington Vascular (https://washingtonvascular.com/smoking-and-peripheral-artery-disease-a-dangerous-combo)
- A modern day perspective on smoking in peripheral artery disease - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10175606)
- Smoking Cessation in Peripheral Artery Disease - American College of Cardiology (https://acc.org/Latest-in-Cardiology/Articles/2020/03/05/07/53/Smoking-Cessation-in-Peripheral-Artery-Disease)
- Smoking cessation for peripheral arterial disease: systematic review protocol - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10508677)
- Diabetes and Its Connection to PAD
- Making Strides: Global Research Finds Semaglutide Helps Patients with Peripheral Artery Disease and Type 2 Diabetes (https://news.cuanschutz.edu/department-of-medicine/research-semaglutide-patients-peripheral-artery-disease-diabetes)
- Frontiers | Exploring the prevalence and risk factors of peripheral artery disease in patients with type 2 diabetes in sub-Saharan Africa: a systematic review and meta-analysis (https://frontiersin.org/journals/clinical-diabetes-and-healthcare/articles/10.3389/fcdhc.2025.1563984/full)
- Epidemiology and Burden of Peripheral Artery Disease in People With Type 2 Diabetes: A Systematic Literature Review - Diabetes Therapy (https://link.springer.com/article/10.1007/s13300-024-01606-6)
- Diabetes and peripheral artery disease: A review - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC8192257)
- Impact of diabetes on mortality in peripheral artery disease: a meta‐analysis - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC6490626)
- High Blood Pressure as a Contributing Factor to PAD
- Products - Data Briefs - Number 289 - October 2017 (https://cdc.gov/nchs/products/databriefs/db289.htm)
- Hypertension in Patients With Peripheral Artery Disease: An Updated Literature Review (https://cureus.com/articles/243834-hypertension-in-patients-with-peripheral-artery-disease-an-updated-literature-review)
- Products - Data Briefs - Number 511 -October 2024 (https://cdc.gov/nchs/products/databriefs/db511.htm)
- Risk factors and prevalence of hypertension in older adults from south-eastern Poland: an observational study - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10792009)
- Long-Lived Families Show Lower Risk for Peripheral Artery Disease | Aging (https://aging-us.com/news-room/long-lived-families-show-lower-risk-for-peripheral-artery-disease)
- High Cholesterol Levels and PAD Risk
- Frontiers | Association Between Cumulative Exposure to Increased Low-Density Lipoprotein Cholesterol and the New Occurrence of Peripheral Artery Disease (https://frontiersin.org/journals/neurology/articles/10.3389/fneur.2021.696695/full)
- 'Bad' cholesterol can be deadly in otherwise healthy people (https://heart.org/en/news/2018/08/20/bad-cholesterol-can-be-deadly-in-otherwise-healthy-people)
- Elevated Remnant and LDL Cholesterol and the Risk of Peripheral Artery Disease: A Mendelian Randomization Study (https://sciencedirect.com/science/article/abs/pii/S0735109725003195?via%3Dihub)
- Elevated Remnant and LDL Cholesterol and the Risk of Peripheral Artery Disease: A Mendelian Randomization Study (https://jacc.org/doi/abs/10.1016/j.jacc.2024.12.033)
- Obesity as a Risk Factor for PAD
- Abstract 14944: Comorbid Obesity in Symptomatic Peripheral Artery Disease: A Modifiable Factor Associated With Health Status | Circulation (https://ahajournals.org/doi/10.1161/circ.146.suppl\_1.14944)
- The Link Between Weight and PAD (https://usavascularcenters.com/blog/the-link-between-weight-and-pad)
- Health Disparities in Peripheral Artery Disease: Key Points - American College of Cardiology (https://acc.org/Latest-in-Cardiology/ten-points-to-remember/2023/07/28/14/44/health-disparities-in-pad)
- Sedentary Lifestyle and Its Effect on PAD Risk
- Characteristics of Older Adults Who Met Federal Physical Activity Guidelines for Americans: United States, 2022 - National Health Statistics Reports - NCBI Bookshelf (https://ncbi.nlm.nih.gov/books/NBK610676)
- High-intensity walking exercise benefits people with peripheral artery disease (https://news-medical.net/news/20210406/High-intensity-walking-exercise-benefits-people-with-peripheral-artery-disease.aspx)
- Report: Adults 50 and Older Need More Physical Activity (https://cdc.gov/physical-activity/php/reports/adults-50-and-older.html)
- Genetic Factors Influencing PAD Risk
- Long-Lived Families Show Lower Risk for Peripheral Artery Disease | Aging (https://aging-us.com/news-room/long-lived-families-show-lower-risk-for-peripheral-artery-disease)
- Inflammatory Diseases and Their Link to PAD
- Health Disparities in Peripheral Artery Disease: A Scientific Statement From the American Heart Association | Circulation (https://ahajournals.org/doi/10.1161/CIR.0000000000001153)
- Autoinflammatory Disease Quotes (https://pinterest.com/ideas/autoinflammatory-disease-quotes/895643803682)
- Chronic Pain Quotes | MoreGoodDays Pain-management Program (https://moregooddays.com/post/chronic-pain-quotes)
- Prediction of Peripheral Artery Disease Prognosis Using Clinical and Inflammatory Biomarker Data - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC11278072)
- Cumulative Risk Factors for Developing PAD
- Epidemiology of Peripheral Artery Disease and Polyvascular Disease | Circulation Research (https://ahajournals.org/doi/10.1161/CIRCRESAHA.121.318535)
- Peripheral Arterial Disease Incidence and Associated Risk Factors in a Mediterranean Population-based Cohort. The REGICOR Study (https://sciencedirect.com/science/article/pii/S1078588415009235)
- Peripheral Artery Disease: 5 major causes, and ways to prevent it (https://timesofindia.indiatimes.com/life-style/health-fitness/health-news/peripheral-artery-disease-5-major-causes-and-ways-to-prevent-it/photostory/125468224.cms)
- Long-Lived Families Show Lower Risk for Peripheral Artery Disease | Aging (https://aging-us.com/news-room/long-lived-families-show-lower-risk-for-peripheral-artery-disease)