
For families in our service areas
For families in our service areas, this guide explains caregiving and how non-medical in-home caregiving can support care planning in East Idaho, Treasure Valley & Magic Valley, Northern Wasatch, North Central West Virginia, and Northeast Ohio.
What You Need to Know About 10 Most Common Causes of Falls in the
Falls among the elderly represent a significant public health issue, often resulting in serious injuries and even death. This alarming trend highlights the urgent need for understanding the various causes of these accidents. By identifying these factors, caregivers can develop effective prevention strategies that not only enhance safety but also help preserve the independence of older adults.
What can be done to combat this growing epidemic? Caregivers play a crucial role in implementing proactive measures. This article explores the ten most common causes of falls in seniors, providing insights and actionable tips for caregivers. By adopting tailored interventions, we can work together to ensure the well-being of our older loved ones.
Happy to Help Caregiving: Personalized In-Home Support to Prevent Falls
Problem: Accidents among seniors are a significant concern, often leading to serious injuries or fatalities. Falls are among the most common causes of falls in the elderly, serving as the leading cause of both fatal and non-fatal injuries in this demographic and underscoring the urgent need for effective preventive measures.
Agitate: The implications of these accidents extend beyond physical harm; they can severely impact a senior's independence and emotional well-being. With statistics indicating that high levels of informal care correlate with a 21% decrease in non-injurious incidents among seniors with multiple daily living limitations, it’s clear that tailored support is essential for safeguarding their health.
Solution: Happy to Help Caregiving offers customized in-home assistance designed to mitigate these risks. By assessing individual needs and creating personalized care plans, caregivers can help clients maintain their independence while ensuring a safe living environment. Caregivers are trained to recognize potential hazards and implement strategies that promote safety, such as:
- Assisting with mobility
- Encouraging safe practices at home
To further enhance safety, caregivers should regularly assess home environments for hazards and encourage clients to engage in physical activities that improve strength and balance. This holistic approach not only addresses physical needs but also fosters emotional wellness, which is crucial for overall health and can help mitigate the most common causes of falls in the elderly.
Muscle Weakness: A Major Contributor to Fall Risk in Seniors
Muscle weakness is among the most common causes of falls in the elderly, significantly increasing their risk. Research indicates that nearly 30% of older adults experience considerable muscle deterioration, particularly in the lower body. This decline can severely affect balance and stability, leading to falls, which are considered one of the most common causes of falls in the elderly and result in injury and hospitalization for individuals over 65 in Canada.
The implications of muscle weakness are serious. The most common causes of falls in the elderly can result in severe injuries, impacting seniors' independence and quality of life. Geriatric specialists emphasize the importance of addressing this issue through regular strength training. Effective exercises, such as:
- Resistance training
- Chair rises
- Balance-focused activities like Tai Chi
can enhance muscle mass and functional strength.
To combat muscle weakness, caregivers should encourage seniors to engage in strength training. Individuals who have experienced multiple falls or stability issues should undergo assessments to identify the most common causes of falls in the elderly. Caregivers play a crucial role in helping seniors establish a safe and effective exercise routine tailored to their needs, promoting greater independence and reducing the risk of accidents.
Additionally, fostering social interactions can help maintain activity levels and further decrease hazards. By prioritizing strength training and adhering to exercise routines, seniors can significantly improve their stability and overall quality of life.
Medication Side Effects: How Prescriptions Can Increase Fall Risk
Some medications are considered to be among the most common causes of falls in the elderly. Sedatives, antidepressants, and high blood pressure medications are considered some of the most common causes of falls in the elderly, often leading to dizziness, drowsiness, or confusion. A systematic review found that 65% to 93% of older adults who suffered injuries from falls were taking at least one medication, which is among the most common causes of falls in the elderly, that heightened their risk at the time of their injury. This underscores the critical need for effective medication management to prevent injuries.
Caregivers must regularly evaluate their clients' medications and consult healthcare professionals about potential side effects that could lead to accidents. Adjusting dosages or switching to alternative medications can help mitigate these risks. The American Geriatrics Society advises against prescribing benzodiazepines and many antidepressants to seniors due to their association with an increased likelihood of falls.
Moreover, the issue of polypharmacy, where older adults take multiple medications, is among the most common causes of falls in the elderly, exacerbating the danger. Approximately 43% of individuals over 65 are on several prescriptions, a factor that contributes to the most common causes of falls in the elderly due to compounded side effects that raise the risk of stumbling. Healthcare professionals stress the importance of discussing the risks and benefits of medications with primary care physicians to ensure that the advantages outweigh the potential hazards.
To promote safer medication management and reduce the chances of accidents, caregivers should maintain an updated list of medications and monitor side effects closely. In 2023, over 41,000 people aged 65 and older in the US died due to accidents, highlighting the urgent need to address this issue.
Environmental Hazards: Identifying Home Risks That Lead to Falls
Clutter, inadequate lighting, and uneven surfaces are among the most common causes of falls in the elderly, posing significant environmental dangers in the home. These hazards can lead to serious injuries, impacting the independence and well-being of older adults. Research shows that one in four individuals over age 65 experiences a fall each year, which highlights the most common causes of falls in the elderly and underscores the urgency of addressing these issues.
To mitigate these risks, caregivers should conduct regular assessments of the living environment. Simple modifications can make a big difference:
- Removing loose rugs
- Ensuring adequate lighting
- Installing grab bars in bathrooms
Additionally, keeping pathways clear and using nonskid mats or strips on wet surfaces can further enhance safety.
Experts recommend that families engage in environmental assessments, utilizing tools like the Falls Free CheckUp offered by the National Council on Aging. This tailored approach allows caregivers to implement changes that meet the specific needs of their loved ones. As Amanda Rudderman, Fall Prevention Coordinator for VCU Medical Center, states, "Most incidents are preventable with the right support, education, and small changes." By prioritizing these modifications, caregivers can help maintain the independence and safety of seniors in their care.
Vision Impairment: The Link Between Poor Sight and Increased Fall Risk
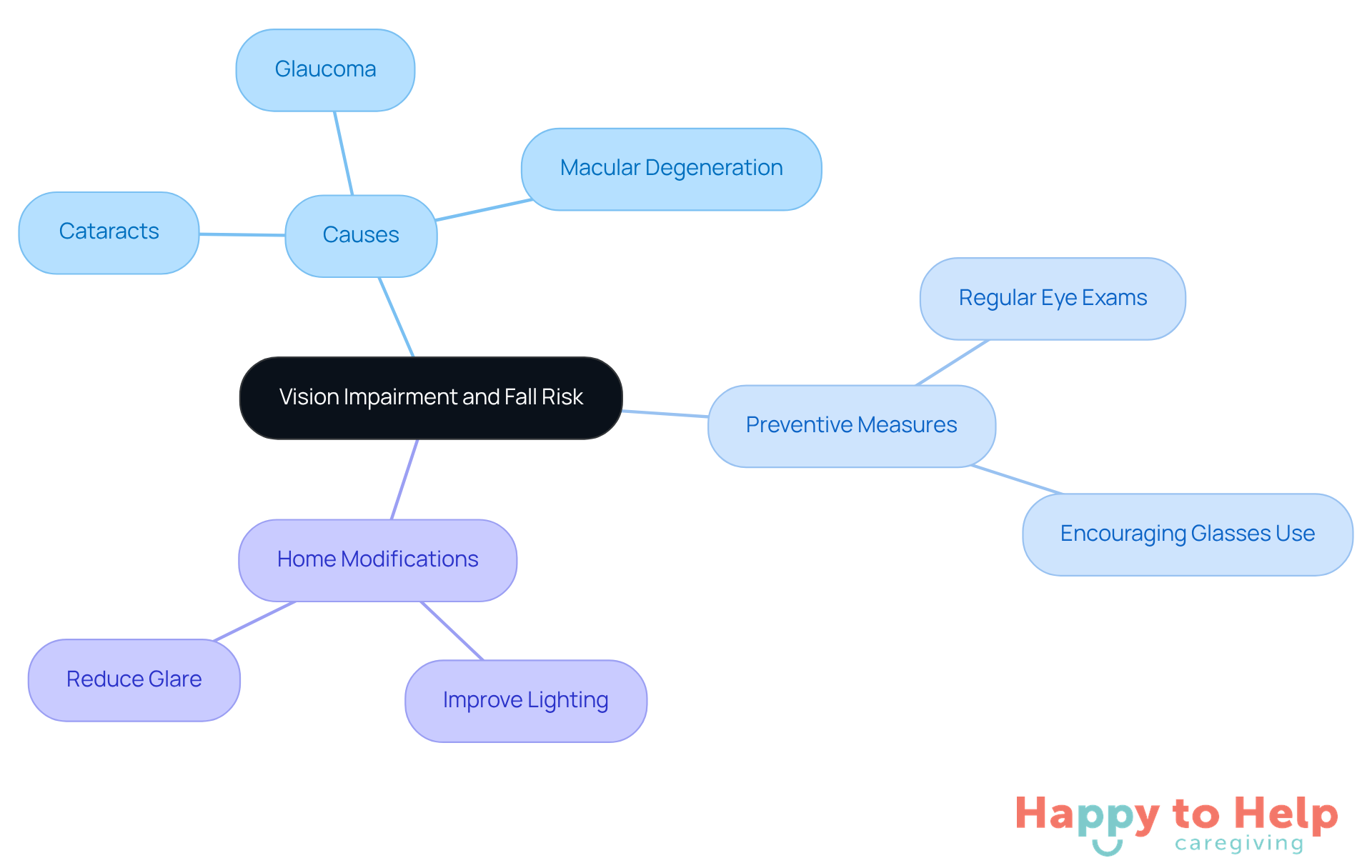
One of the most common causes of falls in the elderly is vision impairment, which significantly increases their risk. Conditions such as cataracts, glaucoma, and macular degeneration are considered to be some of the most common causes of falls in the elderly, as they can severely impact depth perception and overall visual acuity, leading to dangerous situations.
To address this issue, regular eye exams are essential for early detection and treatment of vision problems. Caregivers play a crucial role in this process by encouraging seniors to wear their prescribed glasses.
Additionally, implementing home modifications can greatly enhance visibility and safety. Consider improving lighting in key areas and reducing glare to create a safer environment for seniors. These practical steps can help mitigate the risks associated with vision impairment.
Chronic Health Conditions: How Ongoing Illnesses Increase Fall Risk
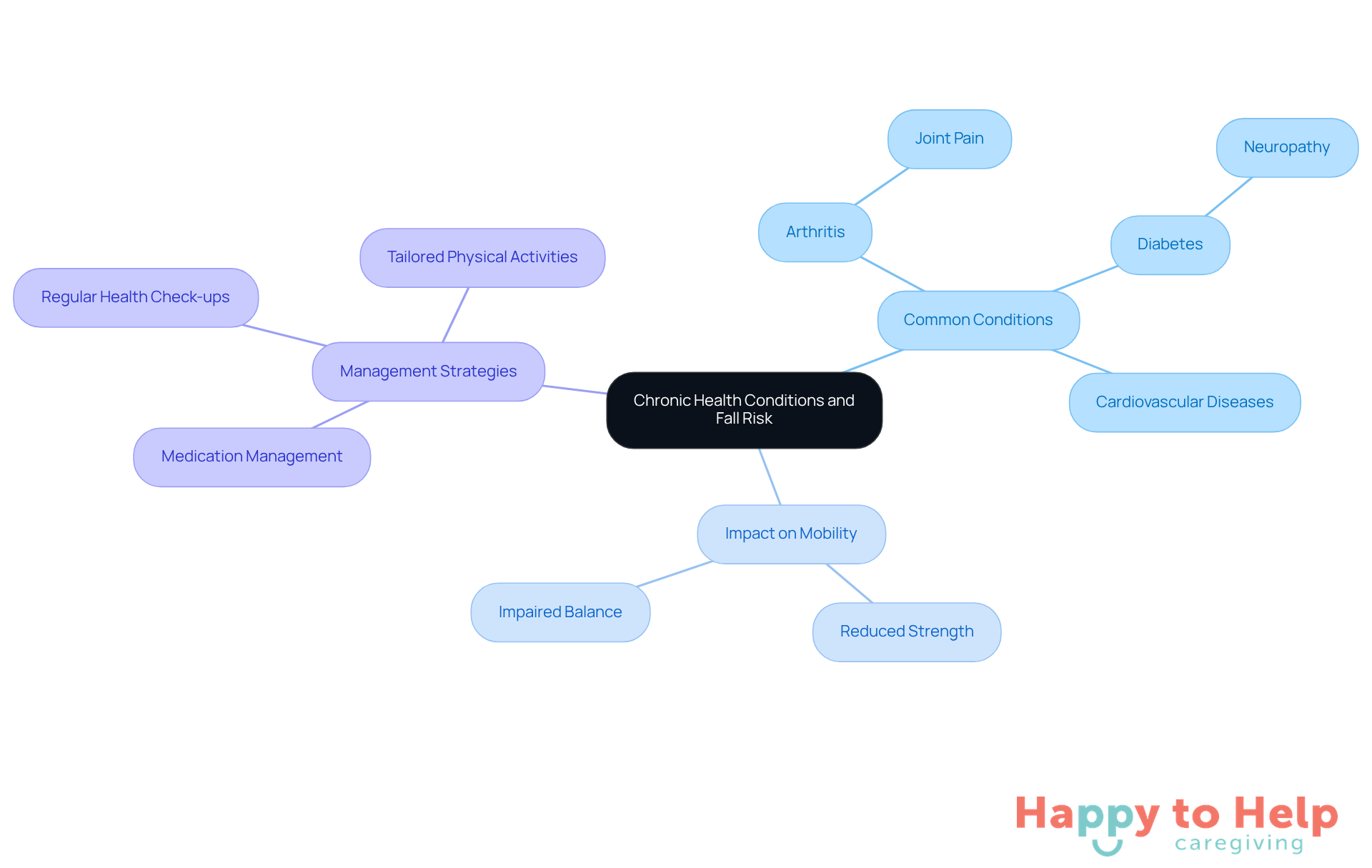
Chronic health issues, such as arthritis, diabetes, and cardiovascular diseases, are some of the most common causes of falls in the elderly, significantly increasing their risk. These conditions negatively impact mobility, strength, and balance, which are among the most common causes of falls in the elderly. For example, individuals with arthritis often experience joint pain that limits their ability to move safely. Similarly, those with diabetes may face neuropathy, complicating their stability even further.
The implications are serious. Studies indicate that middle-aged individuals with a history of chronic illness and previous falls are at a staggering 189% greater chance of injury from tumbles, which are among the most common causes of falls in the elderly, compared to those without such a background. Moreover, there is a clear linear relationship between the number of chronic illnesses and the likelihood of injury from a fall, which are recognized as some of the most common causes of falls in the elderly, highlighting the growing threat associated with multiple chronic conditions.
To address these challenges, caregivers can take proactive steps. Collaborating closely with healthcare providers is essential for effective management of these conditions. This partnership can include:
- Medication management
- Regular health check-ups
- Promoting tailored physical activities that align with the individual's capabilities
As one healthcare provider noted, "Proactive management of chronic illnesses is essential to reducing fall-related injuries and fostering a safer living environment for our elderly patients." By prioritizing these health concerns, caregivers can significantly reduce the risk of accidents, ultimately creating a safer living environment for their loved ones.
Balance and Coordination Issues: Age-Related Declines That Lead to Falls
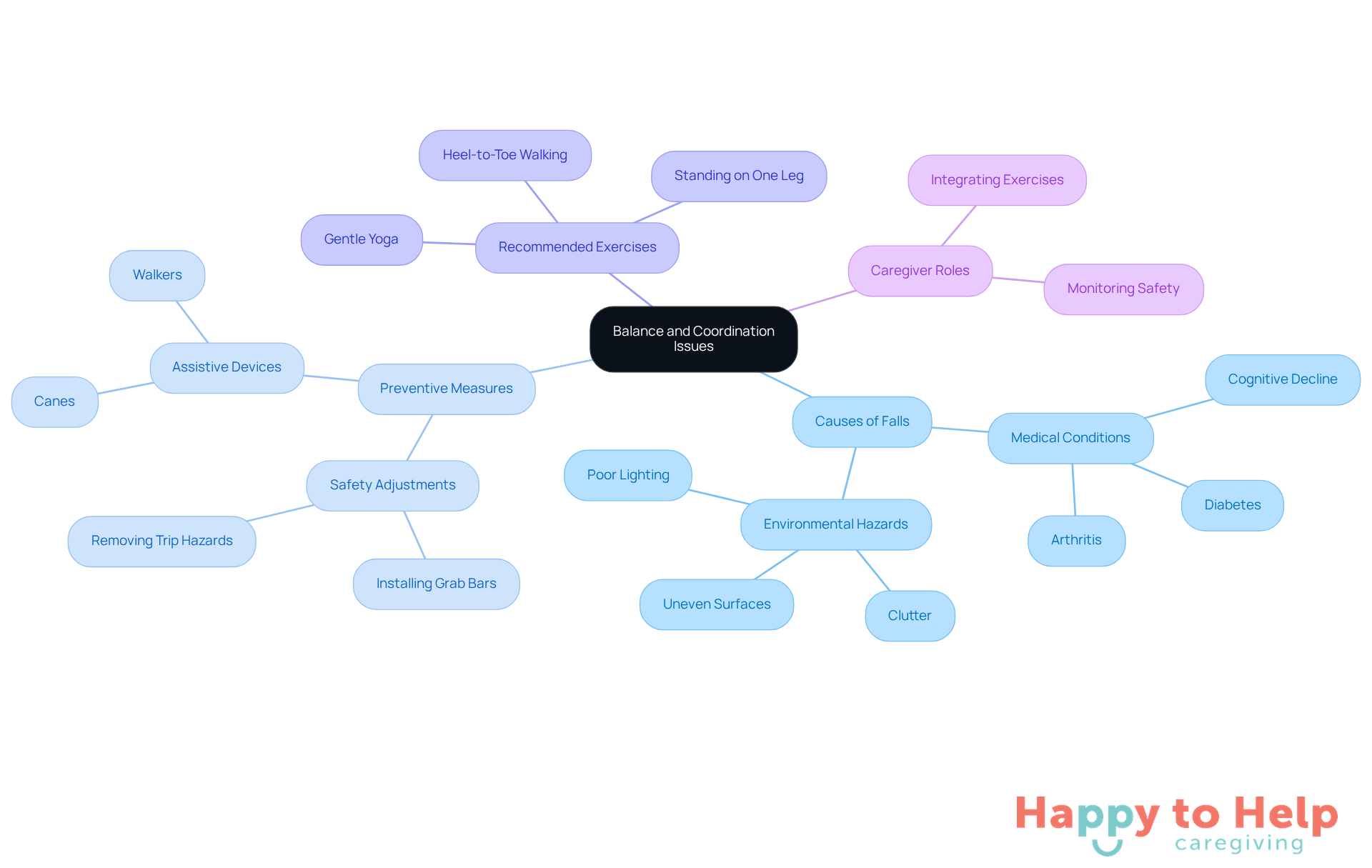
As people age, they often experience a decline in stability and coordination, which are among the most common causes of falls in the elderly. In fact, nearly 3 million emergency department visits occur each year due to accidents among older adults. This statistic underscores the urgent need to address this issue.
To combat this problem, engaging in balance training activities - such as tai chi or specific strength training programs - can enhance stability and reduce the likelihood of falls. Research indicates that those who participate in balance training experience improved coordination and strength, both essential for safe movement.
Caregivers are crucial in helping seniors integrate these exercises into their daily routines, which fosters better balance and boosts confidence. Additionally, using assistive devices like canes or walkers can provide vital support, especially for individuals with significant mobility challenges. Physical therapists often recommend exercises like:
- Heel-to-toe walking
- Standing on one leg
- Gentle yoga
to improve balance and coordination. These activities not only enhance physical stability but also contribute to overall well-being, allowing seniors to maintain their independence and quality of life.
Moreover, caregivers must be aware of the most common causes of falls in the elderly, which include medical conditions such as diabetes, arthritis, and cognitive decline. Making safety adjustments at home - like installing grab bars and removing trip hazards - is essential for preventing accidents. By proactively addressing balance and coordination challenges through targeted exercises and support, caregivers can significantly lower the risk of the most common causes of falls in the elderly, creating a safer living environment for seniors.
Psychological Factors: The Impact of Fear on Fall Risk in Seniors
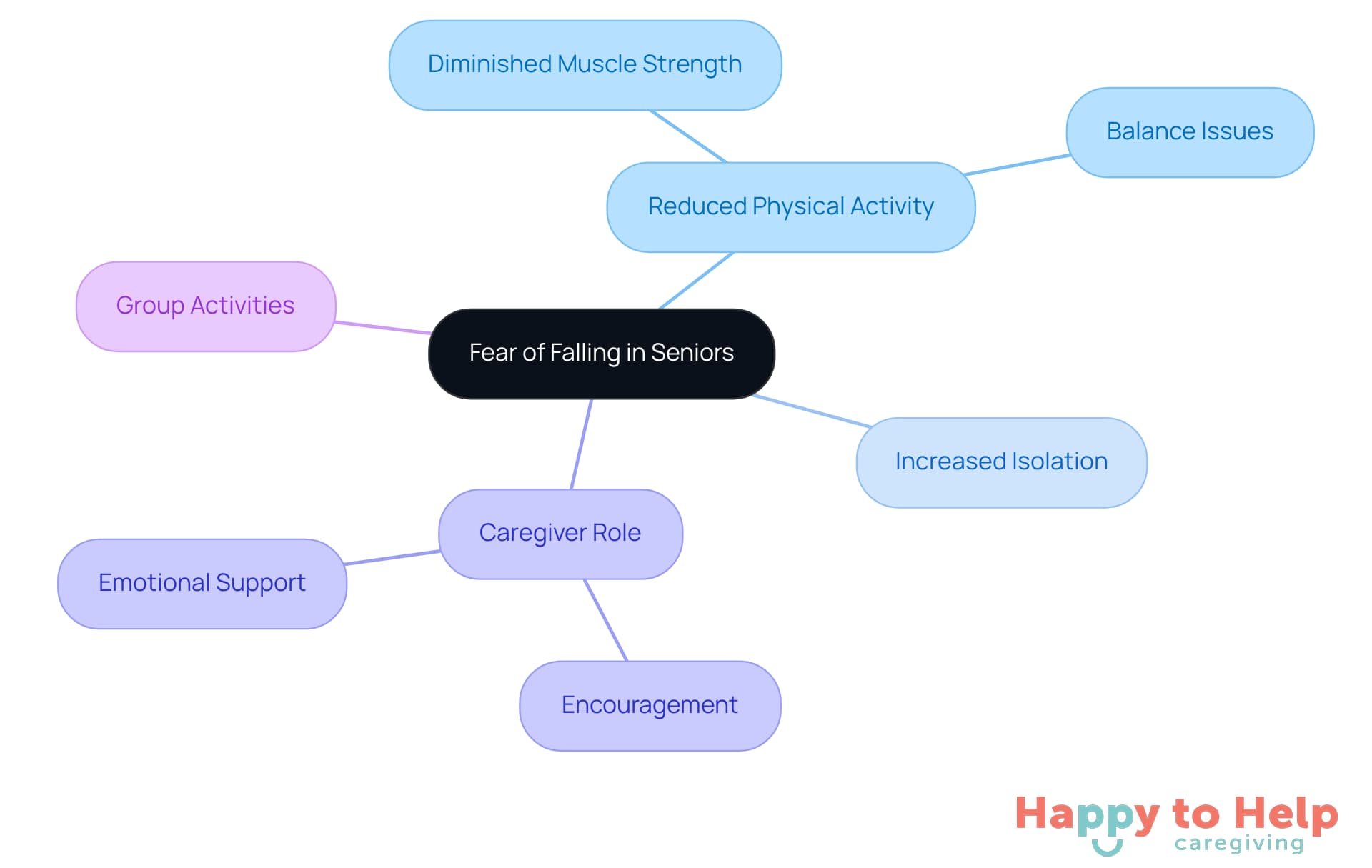
Fear of falling is a significant psychological issue for older adults. This fear often leads to reduced physical activity and increased isolation, creating a troubling cycle. As activity decreases, the most common causes of falls in the elderly, including diminished muscle strength and balance, are heightened.
Caregivers play a crucial role in breaking this cycle. They can encourage seniors to participate in safe physical activities, which not only helps improve strength and balance but also fosters a sense of community. Providing emotional support is equally important, as it helps build confidence in older adults.
Engaging in group activities or classes focused on balance and strength can alleviate fears and promote social interaction. These settings offer a supportive environment where seniors can connect with peers while working on their physical health. By implementing these strategies, caregivers can significantly enhance the well-being of older adults and reduce the fear of falling.
Improper Footwear: How Shoes Can Contribute to Fall Risk
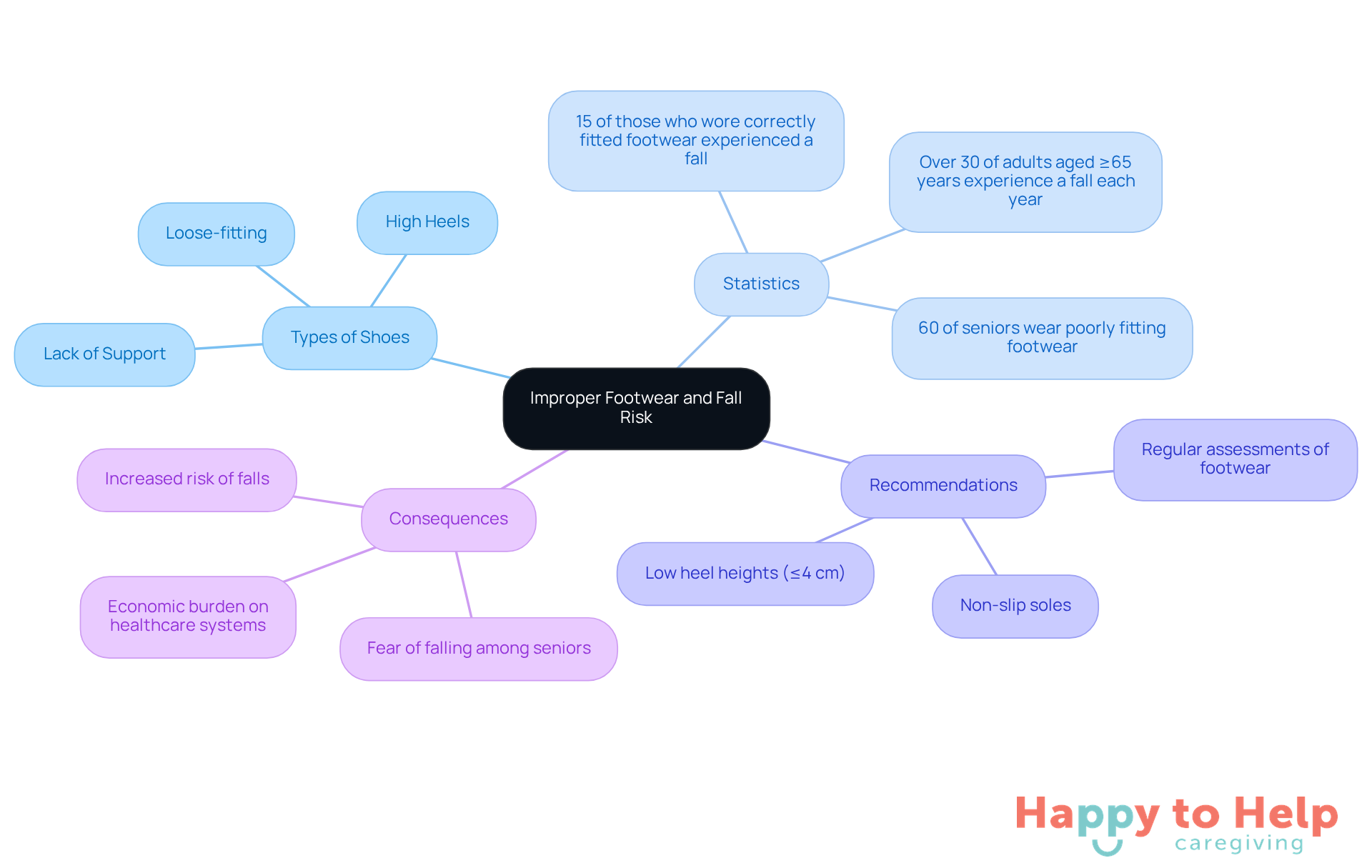
Inappropriate shoes significantly increase the risk of accidents among seniors. Loose-fitting shoes, high heels, and those lacking adequate support are considered some of the most common causes of falls in the elderly, as they can destabilize individuals and increase their risk of falling. Recent statistics reveal that about 60% of seniors wear poorly fitting footwear, which can lead to a higher incidence of tumbles.
To address this issue, caregivers should encourage seniors to choose shoes with non-slip soles. Effective tread patterns and materials are essential for enhancing slip resistance. Additionally, low heel heights (ideally ≤4 cm) are crucial for maintaining balance and stability, while heels higher than this can shift the body's center of mass and contribute to the most common causes of falls in the elderly.
Regular assessments of footwear for signs of wear and tear are vital, as worn-out shoes can severely compromise safety. By emphasizing the importance of suitable shoes and ensuring proper support, caregivers can play a significant role in reducing hazards and improving the overall well-being of elderly individuals.
Regular Health Assessments: Essential for Fall Prevention in the Elderly
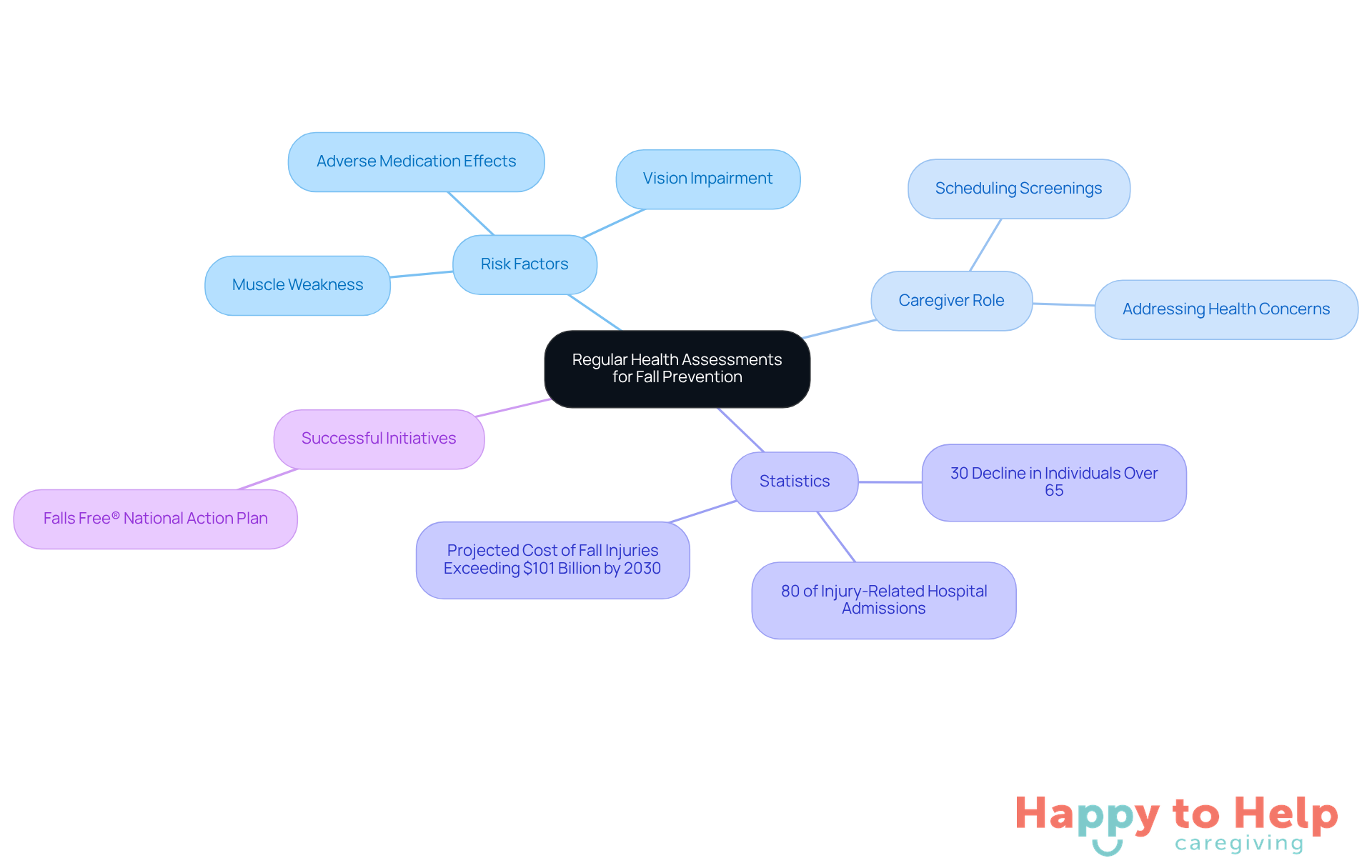
Routine health evaluations are crucial for preventing the most common causes of falls in the elderly. They help identify significant risk factors, which are among the most common causes of falls in the elderly, such as muscle weakness, vision impairment, and adverse medication effects. Alarmingly, research shows that about 30% of individuals over 65 experience a decline each year globally. This statistic highlights the urgent need for regular check-ups.
Caregivers play a vital role in this process. By working closely with healthcare providers, they can schedule regular screenings and assessments, ensuring that any emerging health concerns are addressed promptly. As Hoong Phang, Managing Director & Physiotherapist, states, "The most common causes of falls in the elderly are responsible for 80% of injury-related hospital admissions for people over 65." This underscores the necessity of proactive health management.
Successful health screening initiatives, such as the Falls Free® National Action Plan, have proven effective in reducing slip incidents. These initiatives showcase efficient strategies for prevention. By prioritizing these evaluations, caregivers can significantly enhance the well-being of seniors and mitigate the most common causes of falls in the elderly. This proactive approach also addresses the projected cost of treating fall-related injuries among older adults, which is expected to surpass $101 billion by 2030.
Making the Right Choice
Addressing the most common causes of falls in the elderly is essential for safeguarding their health and well-being. Falls can result from various factors, including muscle weakness, medication side effects, environmental hazards, and psychological influences. Each of these elements significantly increases fall risk, making it crucial for caregivers and family members to understand these challenges.
To mitigate these risks, caregivers can implement targeted strategies. The following are vital:
- Personalized caregiving
- Regular health assessments
- Proactive measures such as strength training and home modifications
- Encouraging physical activity
- Ensuring proper footwear
- Managing medications effectively
The collaborative efforts of caregivers and healthcare professionals can make a substantial difference in preventing injuries and maintaining the quality of life for older adults.
Ultimately, fostering a safe and supportive environment is vital in reducing the incidence of falls among seniors. By prioritizing fall prevention strategies, caregivers can empower elderly individuals to lead fulfilling lives while minimizing the dangers that come with aging. Emphasizing education, awareness, and tailored support will not only enhance safety but also promote the overall well-being of this vulnerable population.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5MjNhMGI5YzVlZWQyYmRiNTU3YmYyNCIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What is the main problem addressed by Happy to Help Caregiving?
The main problem is the high incidence of falls among seniors, which often leads to serious injuries or fatalities, severely impacting their independence and emotional well-being.
How does Happy to Help Caregiving aim to prevent falls?
Happy to Help Caregiving provides personalized in-home support by assessing individual needs and creating tailored care plans that promote safety and independence for seniors.
What strategies do caregivers implement to enhance safety for seniors?
Caregivers assist with mobility, encourage safe practices at home, regularly assess home environments for hazards, and promote physical activities that improve strength and balance.
What role does muscle weakness play in fall risk for seniors?
Muscle weakness is a significant contributor to falls in the elderly, with nearly 30% of older adults experiencing considerable muscle deterioration, particularly in the lower body, affecting their balance and stability.
What types of exercises can help combat muscle weakness in seniors?
Effective exercises include resistance training, chair rises, and balance-focused activities like Tai Chi, which can enhance muscle mass and functional strength.
How can medication side effects increase fall risk in seniors?
Certain medications, such as sedatives, antidepressants, and high blood pressure medications, can cause dizziness, drowsiness, or confusion, increasing the risk of falls.
What should caregivers do to manage medications for seniors?
Caregivers should regularly evaluate medications, consult healthcare professionals about potential side effects, adjust dosages if necessary, and maintain an updated list of medications to ensure safer management.
What is polypharmacy, and how does it relate to fall risks in older adults?
Polypharmacy refers to older adults taking multiple medications, which can compound side effects and increase the risk of falls, with approximately 43% of individuals over 65 being on several prescriptions.
Why is it important for seniors to engage in strength training?
Engaging in strength training helps improve stability, functional strength, and overall quality of life, reducing the risk of falls and promoting greater independence.
What is the significance of discussing medication risks with healthcare professionals?
Discussing medication risks with primary care physicians is crucial to ensure that the benefits of medications outweigh the potential hazards, especially in preventing falls among seniors.
List of Sources
- Happy to Help Caregiving: Personalized In-Home Support to Prevent Falls
- New Enhancements to In-Home Fall Prevention Program (https://vnshealth.org/about/newsroom/articles/new-enhancements-to-in-home-fall-prevention-program)
- Facts About Falls (https://cdc.gov/falls/data-research/facts-stats)
- Get the Facts on Falls Prevention (https://ncoa.org/article/get-the-facts-on-falls-prevention)
- Receipt of Caregiving and Fall Risk in U.S. Community-Dwelling Older Adults - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC5352465)
- Fall-prevention program can help reduce harmful in-home falls by nearly 40% | WashU Medicine (https://medicine.washu.edu/news/fall-prevention-program-can-help-reduce-dangerous-in-home-tumbles-by-nearly-40)
- Muscle Weakness: A Major Contributor to Fall Risk in Seniors
- Facts About Falls (https://cdc.gov/falls/data-research/facts-stats)
- Reducing fall risk for aging adults – what works and why | VCU Health (https://vcuhealth.org/news/reducing-fall-risk-for-aging-adults--what-works-and-why)
- Slower-walking older adults at risk for falls benefit the most from a home-based exercise program (https://vchri.ca/stories/2025/11/15/slower-walking-older-adults-risk-falls-benefit-most-home-based-exercise-program)
- Falls in Older Adults - Geriatrics - Merck Manual Professional Edition (https://merckmanuals.com/professional/geriatrics/falls-in-older-adults/falls-in-older-adults)
- Medication Side Effects: How Prescriptions Can Increase Fall Risk
- Common prescription drugs linked to surge in fall-related death rates among seniors (https://foxnews.com/health/common-prescription-drugs-linked-surge-fall-related-death-rates-among-seniors)
- Risky Prescribing and the Epidemic of Deaths From Falls (https://jamanetwork.com/journals/jama-health-forum/fullarticle/2837039)
- Medications That Increase Fall Risk in Older Adults - WTOP News (https://wtop.com/news/2025/10/medications-that-increase-fall-risk-in-older-adults)
- Environmental Hazards: Identifying Home Risks That Lead to Falls
- Facts About Falls (https://cdc.gov/falls/data-research/facts-stats)
- How to Prevent Falls with Home Safety Modifications (https://ncoa.org/article/how-to-prevent-falls-with-home-safety-modifications)
- Get the Facts on Falls Prevention (https://ncoa.org/article/get-the-facts-on-falls-prevention)
- Reducing fall risk for aging adults – what works and why | VCU Health (https://vcuhealth.org/news/reducing-fall-risk-for-aging-adults--what-works-and-why)
- Falls in the Elderly at Home – Common Causes & Prevention (https://tuckermanrehab.com/education/elderly-falls-at-home-causes-prevention)
- Vision Impairment: The Link Between Poor Sight and Increased Fall Risk
- Comprehensive Geriatric Assessment (Chapter 3) - Reichel's Care of the Elderly (https://cambridge.org/core/books/reichels-care-of-the-elderly/comprehensive-geriatric-assessment/0B010C92AFE1FE8FB5C332B87F7EBC0E)
- Population Prevalence of Vision Impairment in US Adults 71 Years and Older (https://jamanetwork.com/journals/jamaophthalmology/fullarticle/2800246)
- Get the Facts on Falls Prevention (https://ncoa.org/article/get-the-facts-on-falls-prevention)
- Falls Among Persons Aged ≥65 Years With and Without Severe Vision Impairment — United States, 2014 | MMWR (https://cdc.gov/mmwr/volumes/65/wr/mm6517a2.htm)
- Link between eye examinations and fall prevention in older adults (https://aoa.org/news/clinical-eye-care/public-health/link-between-eye-examinations-and-fall-prevention-in-older-adults)
- Chronic Health Conditions: How Ongoing Illnesses Increase Fall Risk
- Get the Facts on Falls Prevention (https://ncoa.org/article/get-the-facts-on-falls-prevention)
- A prospective cohort study of the impact of chronic disease on fall injuries in middle-aged and older adults - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10350885)
- Older Adult Falls Data (https://cdc.gov/falls/data-research)
- Chronic Illness Quotes That Inspire Strength and Resilience - Denver Family Counseling Services (https://denverfamilycounselingservices.com/chronic-illness-quotes)
- Balance and Coordination Issues: Age-Related Declines That Lead to Falls
- Facts About Falls (https://cdc.gov/falls/data-research/facts-stats)
- Reducing fall risk for aging adults – what works and why | VCU Health (https://vcuhealth.org/news/reducing-fall-risk-for-aging-adults--what-works-and-why)
- Get the Facts on Falls Prevention (https://ncoa.org/article/get-the-facts-on-falls-prevention)
- Strength Training & Balance Exercises Can Help Prevent Falls (https://mcleodhealth.org/news-entry/strength-training-and-balance-exercises-can-help-prevent-falls)
- Improper Footwear: How Shoes Can Contribute to Fall Risk
- Enhancing Footwear Safety for Fall Prevention in Older Adults: A Comprehensive Review of Design Features - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC11217662)
- Fall Prevention for Older Adults Starts with Safer Shoes (https://foxrehab.org/safe-footwear-older-adult-fall-risk)
- Many Falls Are Preventable. These Tips Can Help. (https://nytimes.com/2025/06/11/well/fall-prevention-tips.html)
- From Rugs to Routines: Fall Prevention for Seniors (https://silvermaples.org/from-rugs-to-routines-fall-prevention-for-seniors)
- Regular Health Assessments: Essential for Fall Prevention in the Elderly
- Facts About Falls (https://cdc.gov/falls/data-research/facts-stats)
- Supreme Court ruling could affect falls risk assessments, interventions for older adults (https://mcknightsseniorliving.com/news/supreme-court-ruling-could-affect-falls-risk-assessments-interventions-for-older-adults)
- Get the Facts on Falls Prevention (https://ncoa.org/article/get-the-facts-on-falls-prevention)
- News | APTA-Backed Legislation Beefs Up Falls Screening, Prevention by PTs in Medicare (https://apta.org/news/2024/03/12/falls-legislation-safe-act)
- Ten Concerning Statistics on Falls in the Elderly (https://propelphysiotherapy.com/healthy-aging/preventing-falls-in-the-elderly)