
For families in our service areas
For families in our service areas, this guide explains dementia care and how non-medical in-home caregiving can support care planning in East Idaho, Treasure Valley & Magic Valley, Northern Wasatch, North Central West Virginia, and Northeast Ohio.
What You Need to Know About 10 Strategies for Helping Elderly Not
Caring for elderly individuals with dementia presents unique challenges, particularly in maintaining a healthy diet. Cognitive decline can significantly affect appetite and eating habits, leaving caregivers to navigate a complex landscape filled with emotional and practical hurdles. This article explores ten effective strategies to stimulate appetite and encourage better eating practices among dementia patients. By implementing thoughtful interventions, caregivers can enhance both nutrition and quality of life.
What innovative approaches can caregivers adopt to transform mealtimes into supportive and enjoyable experiences for their loved ones?
Happy to Help Caregiving: Personalized In-Home Support for Dementia Patients
Caring for individuals with cognitive impairment presents significant challenges for both the affected individuals and their caregivers. These challenges can lead to feelings of isolation and stress, making it crucial to find effective support solutions.
Happy to Help Caregiving addresses these issues by offering tailored in-home assistance. Their services include:
- Companionship care
- Post-hospital recovery assistance
- Respite care
- Palliative support care
Each service is designed to enhance the quality of life for individuals with cognitive impairment, ensuring they receive compassionate care in a familiar environment. Caregivers are trained to develop individualized care plans that cater to the unique needs of each client, promoting independence and well-being. By focusing on personalized care, Happy to Help Caregiving helps alleviate the burdens faced by caregivers, allowing them to provide the best support possible.
Dementia-Friendly Mealtimes: Creating a Comfortable Eating Environment
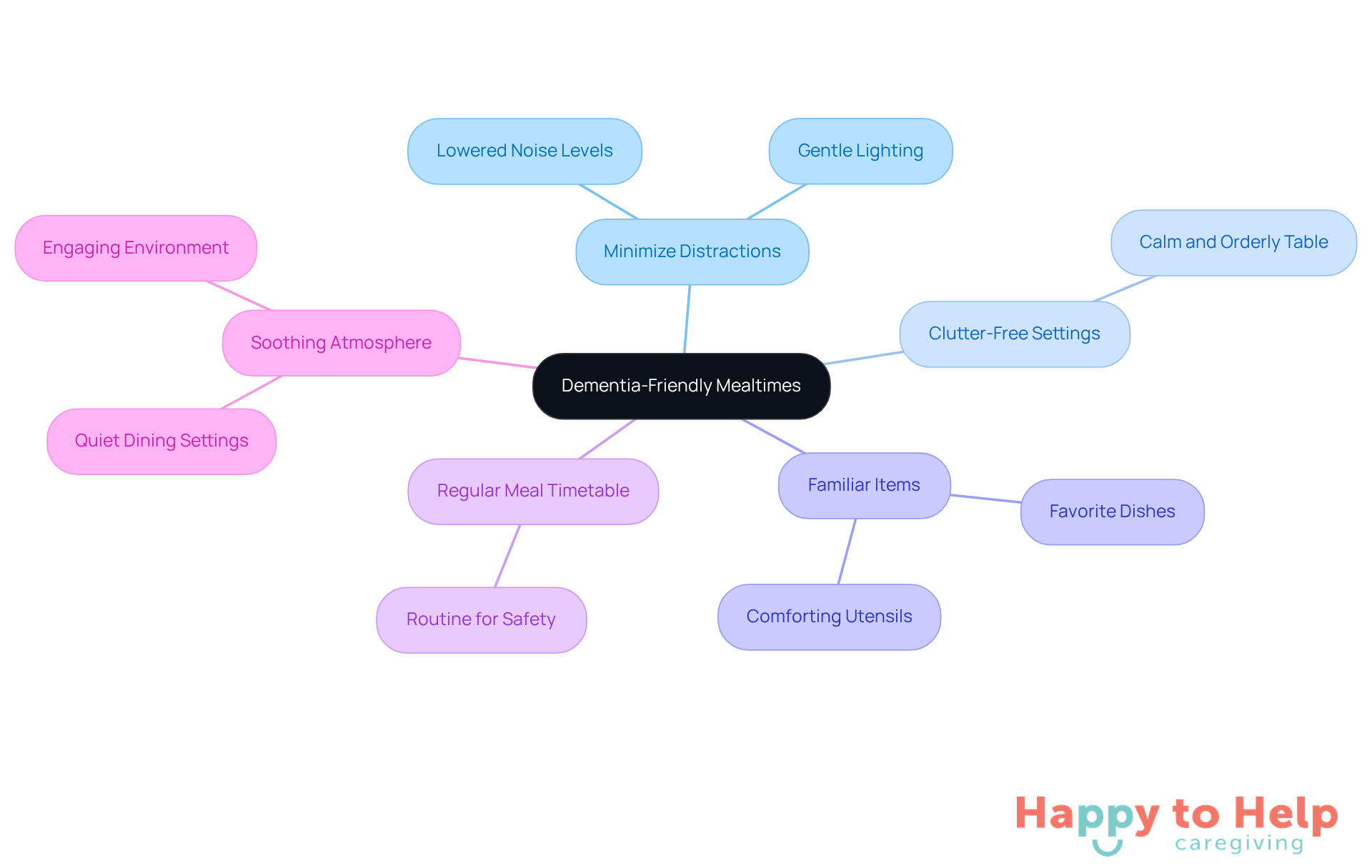
Creating a mealtime environment that addresses the issue of elderly not eating dementia is crucial for enhancing the dining experience of individuals with cognitive challenges. The problem lies in the distractions that can arise during meals, such as high noise levels and cluttered settings. These factors can significantly hinder the elderly not eating dementia individual's ability to focus on their food, leading to withdrawal or distress.
To address this issue, caregivers can implement several strategies. First, minimizing distractions through lowered noise levels and gentle lighting can greatly improve concentration. A clutter-free table setting promotes a sense of calm and order. Additionally, incorporating familiar items, like favorite dishes or utensils, can evoke positive memories and comfort, making the dining experience more enjoyable. As Isabella Morgia di Vicari observes, familiar foods can bring joy to individuals with cognitive decline, enhancing their overall experience.
Establishing a regular meal timetable is another essential solution. This routine fosters a feeling of safety for individuals with cognitive impairments. Research indicates that noisy environments can lead to distress, making it vital for caregivers to choose quieter dining settings. Edith Gendron highlights that loud restaurants can overwhelm individuals with advanced cognitive impairment, resulting in distress. Furthermore, geriatric specialists emphasize the importance of maintaining a soothing atmosphere to encourage engagement during meals.
By applying these strategies, caregivers can significantly enhance the mealtime experience for the elderly not eating dementia, promoting both nutrition and social interaction. With an estimated 720,000 Florida seniors projected to have Alzheimer's disease by 2025, the need for supportive environments is more crucial than ever.
Caregiver Engagement: Encouraging Appetite Through Companionship
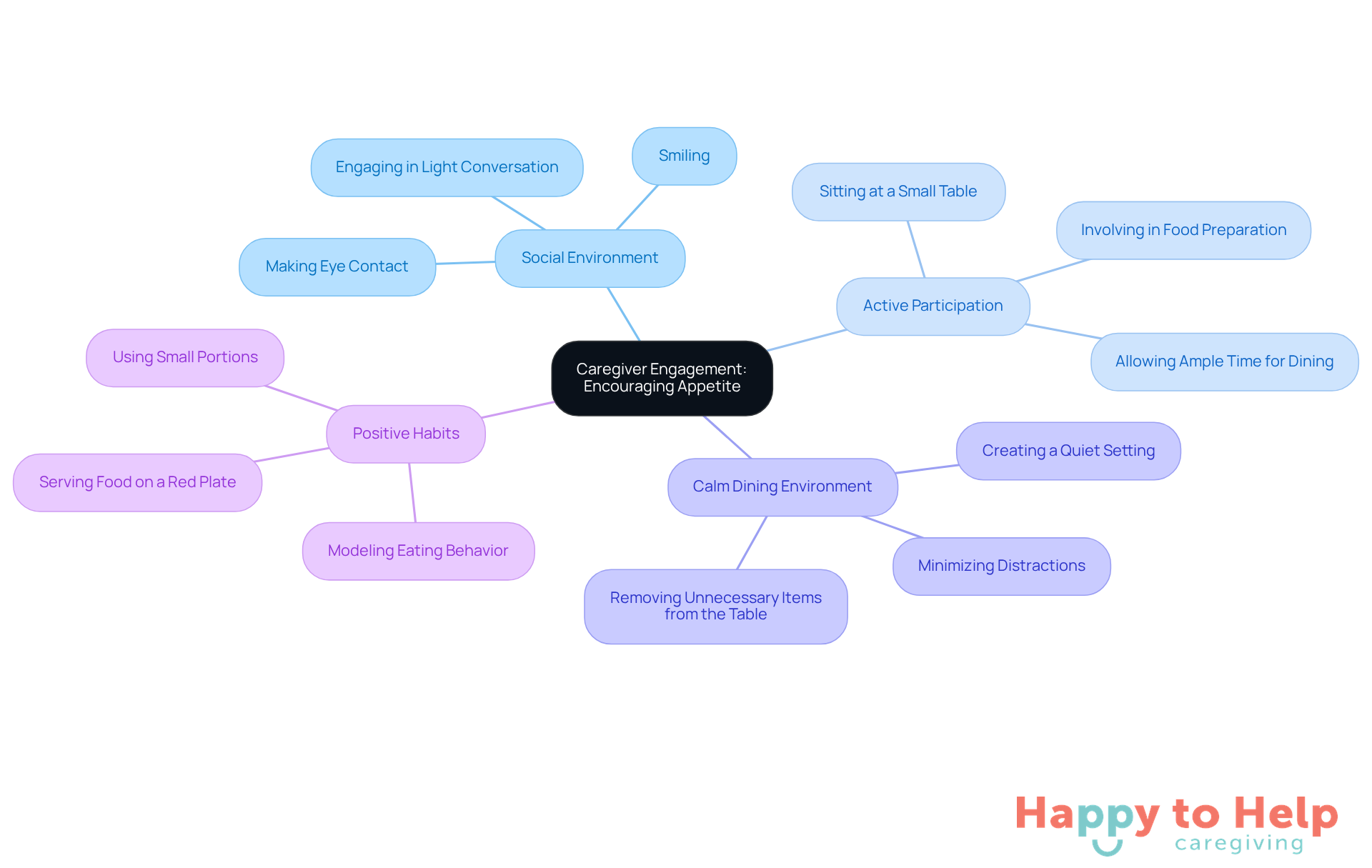
Caregiver involvement is essential in addressing the challenge of stimulating appetite among the elderly not eating due to dementia. Many caregivers face the difficulty of encouraging their elderly not eating dementia loved ones to eat, which can lead to nutritional deficiencies and a decline in overall health. This issue not only affects the individual but also places emotional strain on caregivers who want to provide the best support possible.
To tackle this problem, creating a social environment during meals can transform dining into a more enjoyable experience. Active participation from caregivers-through encouragement, companionship, and interaction-can significantly enhance the dining experience. Simple gestures like making eye contact, smiling, and engaging in light conversation help patients feel more connected and motivated to eat. Research indicates that companionship during meals can lead to increased food consumption; for instance, individuals with Alzheimer’s consumed 25% more food when served on a red plate, highlighting the impact of visual cues and social interaction on appetite.
Effective strategies for caregivers include:
- Sitting at a small table facing the loved one to promote companionship.
- Allowing ample time for dining to reduce stress.
- Involving the care recipient in food preparation to enhance their experience.
Additionally, creating a calm and distraction-free dining environment is crucial for minimizing interruptions during meals. By demonstrating positive eating habits and fostering a nurturing atmosphere, caregivers can effectively assist their loved ones, especially the elderly not eating due to dementia, in overcoming eating difficulties related to cognitive decline.
Nutritional Strategies: Best Foods to Stimulate Appetite in Dementia Patients
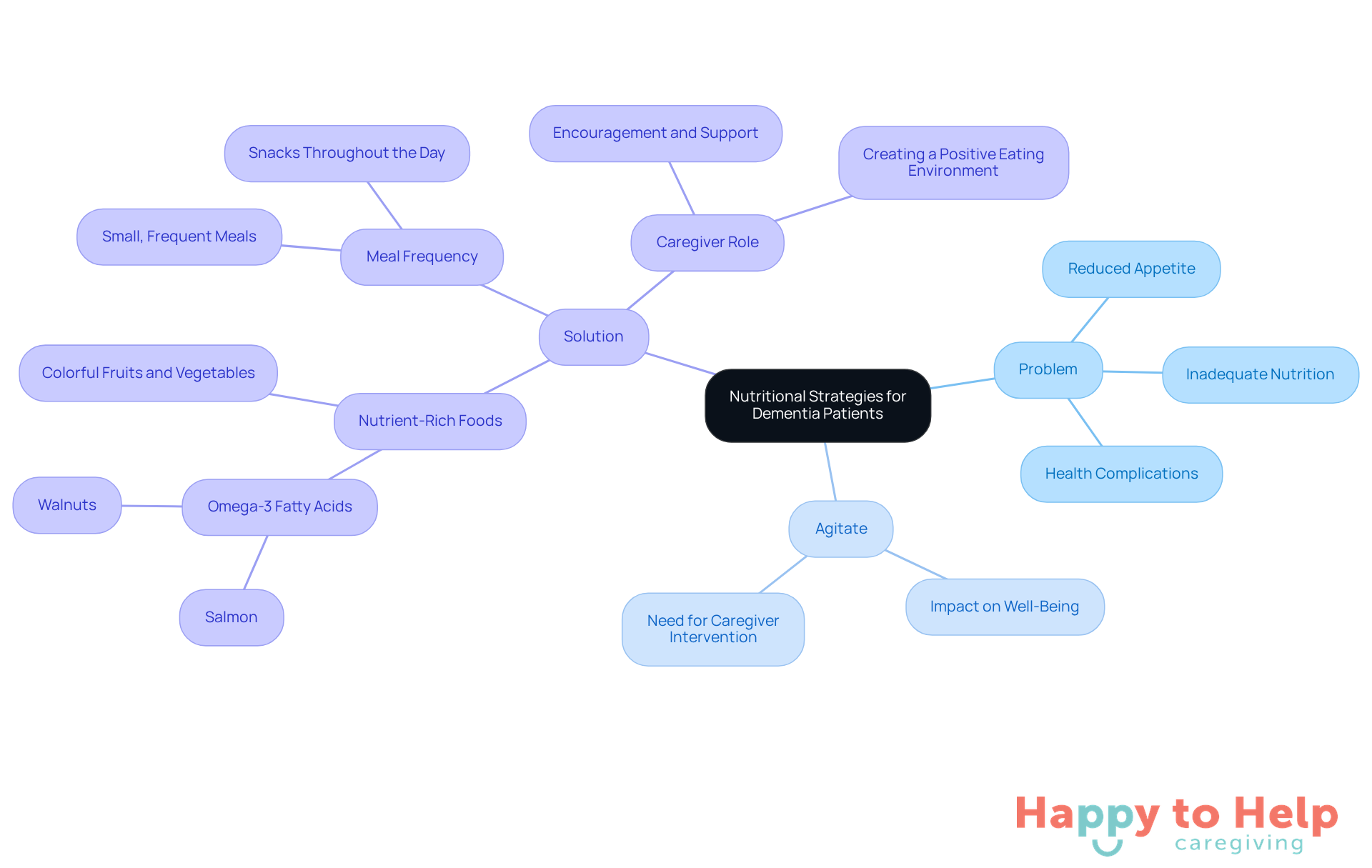
The elderly not eating dementia often experience a reduced appetite, which can result in inadequate nutrition and further health complications.
The issue of elderly not eating dementia can significantly impact their overall well-being, making it crucial for caregivers to address this decline in appetite effectively.
Solution: To encourage appetite, caregivers should focus on nutrient-rich foods that are visually appealing and easy to consume. Incorporating foods high in omega-3 fatty acids, like salmon and walnuts, can support brain health. Additionally, colorful fruits and vegetables not only enhance visual appeal but also provide essential nutrients.
- Offering small, frequent meals and snacks throughout the day can help maintain energy levels and promote eating.
- By implementing these strategies, caregivers can play a vital role in addressing the issue of elderly not eating due to dementia and improving their nutritional intake.
Addressing Health Issues: Identifying Causes of Poor Appetite in Dementia
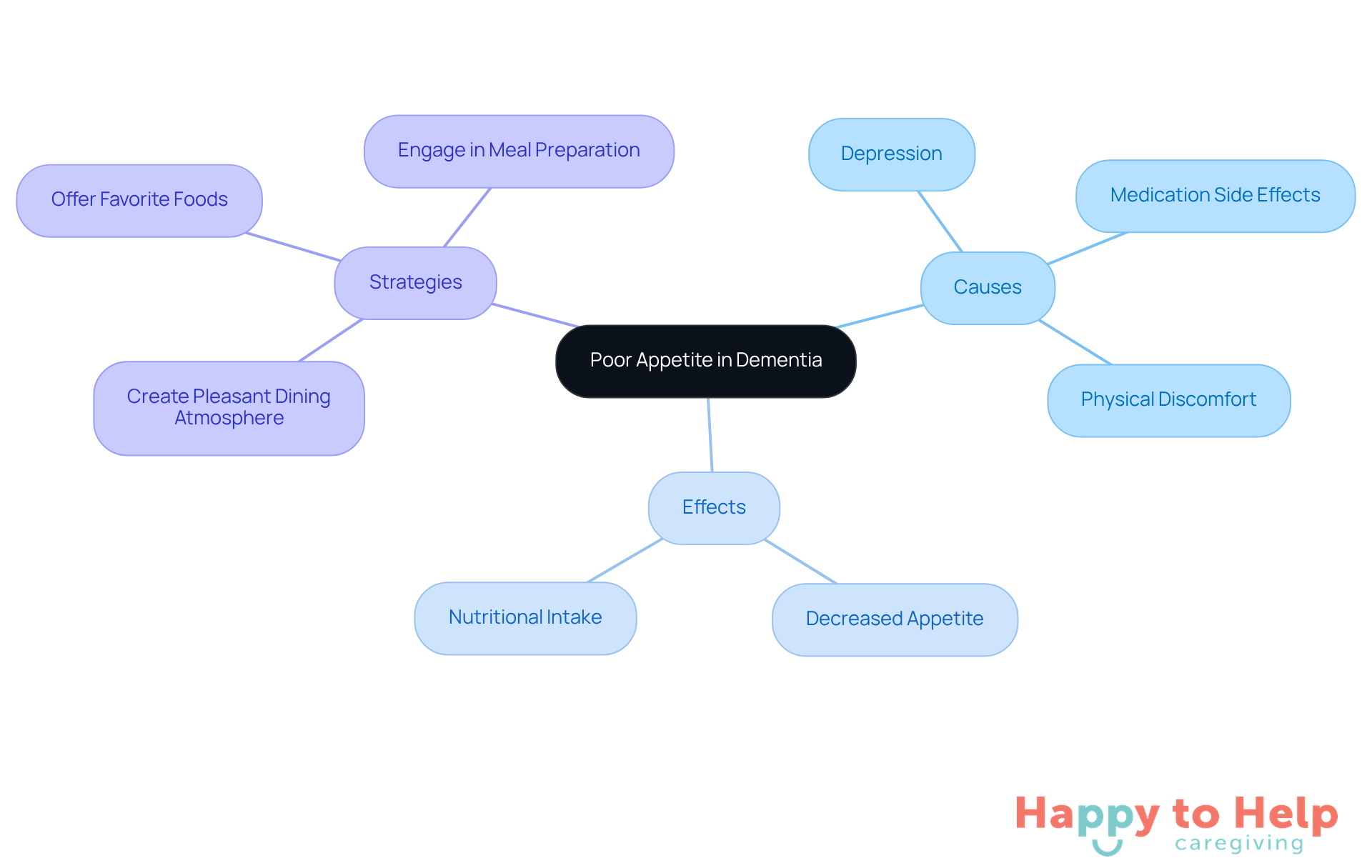
The issue of elderly not eating dementia presents a significant challenge for caregivers. This issue can arise from various health problems, such as depression, medication side effects, and physical discomfort. Caregivers must be vigilant, monitoring their loved ones for signs of pain or discomfort that may hinder eating. Regular consultations with healthcare providers are essential to identify and address these issues, ensuring that patients receive the necessary medical care and support.
Research shows that elderly not eating dementia can greatly affect their eating habits, often resulting in decreased appetite and nutritional intake. Healthcare providers stress the importance of tackling these emotional challenges alongside physical health. For example, managing medication side effects is vital, as certain drugs can suppress appetite or lead to gastrointestinal discomfort. Caregivers should discuss any changes in eating patterns with healthcare professionals to adjust treatment plans accordingly.
Moreover, recent studies indicate that weight loss medications like Wegovy and Ozempic may help alleviate appetite issues related to dementia. These drugs could assist in managing both weight and cognitive health, offering caregivers additional options to consider.
To effectively address poor appetite in dementia care, caregivers can implement several strategies:
- Create a pleasant dining atmosphere.
- Offer favorite foods.
- Ensure dishes are visually appealing.
Engaging patients in meal preparation can also spark interest in eating. By applying these strategies and maintaining open communication with healthcare providers, caregivers can significantly improve the nutritional well-being of their loved ones.
Hydration Management: Ensuring Adequate Fluid Intake for Dementia Patients
Hydration is a significant concern for individuals with cognitive impairments. Dehydration can worsen cognitive decline and lead to serious health issues. Caregivers face the challenge of ensuring adequate fluid intake to combat these risks.
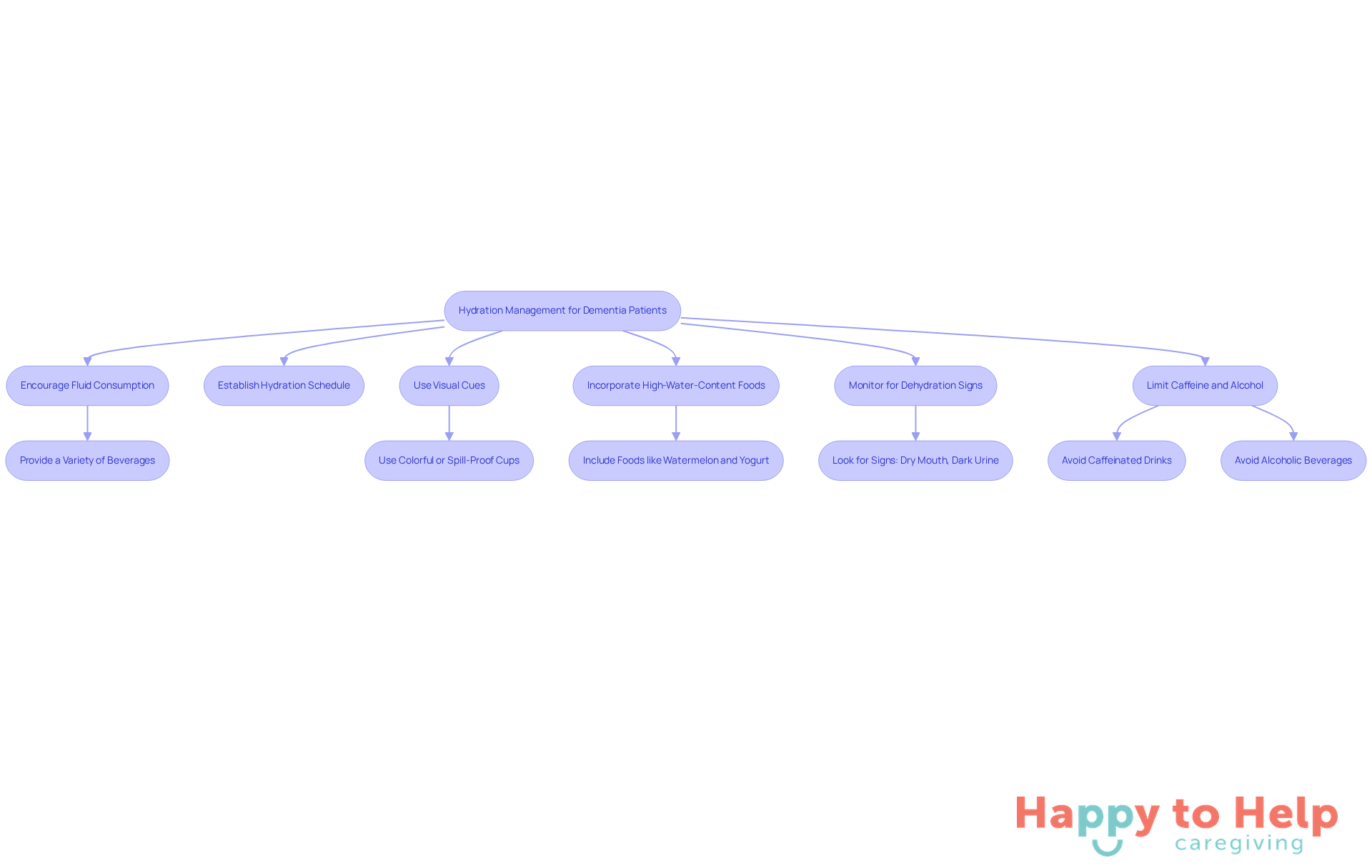
To address this problem, caregivers should actively encourage fluid consumption by providing a variety of beverages throughout the day. Options like water, herbal teas, and fruit-infused drinks can make hydration more appealing. It's generally recommended that individuals drink 6 to 8 cups or glasses of fluid daily to stay properly hydrated.
Establishing a hydration schedule can help create a routine, making it easier for individuals to remember to drink regularly. Visual cues, such as placing drinks in clear sight, serve as effective reminders. Additionally, using colorful or spill-proof cups can enhance the drinking experience.
Incorporating high-water-content foods - like watermelon, cucumbers, yogurt, and ice lollies - can also effectively supplement fluid intake. Caregivers should be vigilant for signs of dehydration, including dry mouth, dark urine, and fatigue, to ensure timely intervention.
Limiting caffeinated and alcoholic beverages is crucial, as these can contribute to dehydration. By implementing strategies such as hydration reminder applications and maintaining a hydration log, caregivers can significantly improve hydration levels in patients with cognitive impairments, ultimately enhancing their overall health and quality of life.
Mealtime Management: Practical Tips for Caregivers of Dementia Patients
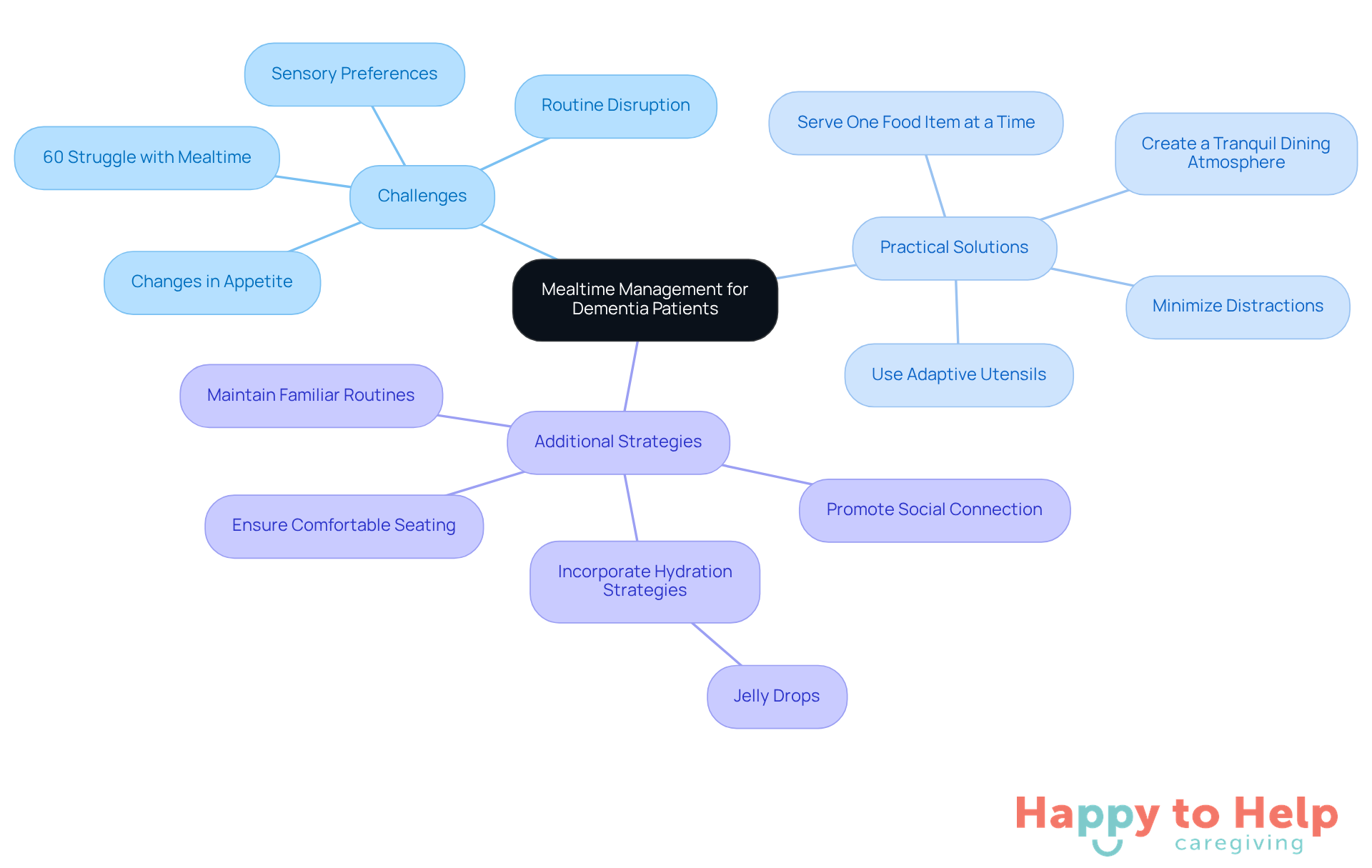
Effective mealtime management for caregivers is a significant challenge when dealing with elderly not eating dementia. Rushing through meals can heighten anxiety and lead to a decreased appetite, making it crucial to prioritize comfort and calm during this time. Research shows that 60% of elderly not eating dementia individuals living at home struggle with mealtime, which highlights the need for thoughtful strategies.
To address this issue, caregivers can implement several practical solutions:
- Serving one food item at a time can reduce confusion, allowing individuals to focus on each dish without feeling overwhelmed.
- Minimizing distractions is essential; turning off the television and ensuring a quiet dining area can create a more peaceful environment.
As Lisa Juckett, an expert in occupational therapy, emphasizes, "It comes down to keeping things simple. How do we keep that environment as simple as possible so people’s eyes and ears aren’t distracted and taking their attention away from their food?"
Establishing a tranquil dining atmosphere not only promotes healthier eating habits but is crucial for the elderly not eating dementia, as it also supports their emotional well-being. By applying these strategies, caregivers can significantly enhance the mealtime experience, fostering both nutrition and a sense of security for those they support. Furthermore, incorporating hydration strategies, such as providing Jelly Drops - which have assisted over 80,000 people with cognitive impairments - can further improve the mealtime experience.
Technology Tools: Enhancing Caregiver Support for Managing Eating Habits
Caregivers face significant challenges in monitoring the nutrition and hydration of elderly not eating dementia patients. This responsibility can lead to emotional strain and uncertainty, as ensuring proper eating habits is crucial for the well-being of elderly not eating dementia. With approximately 6.9 million Americans aged 65 and older living with cognitive decline, the need for effective solutions is more pressing than ever.
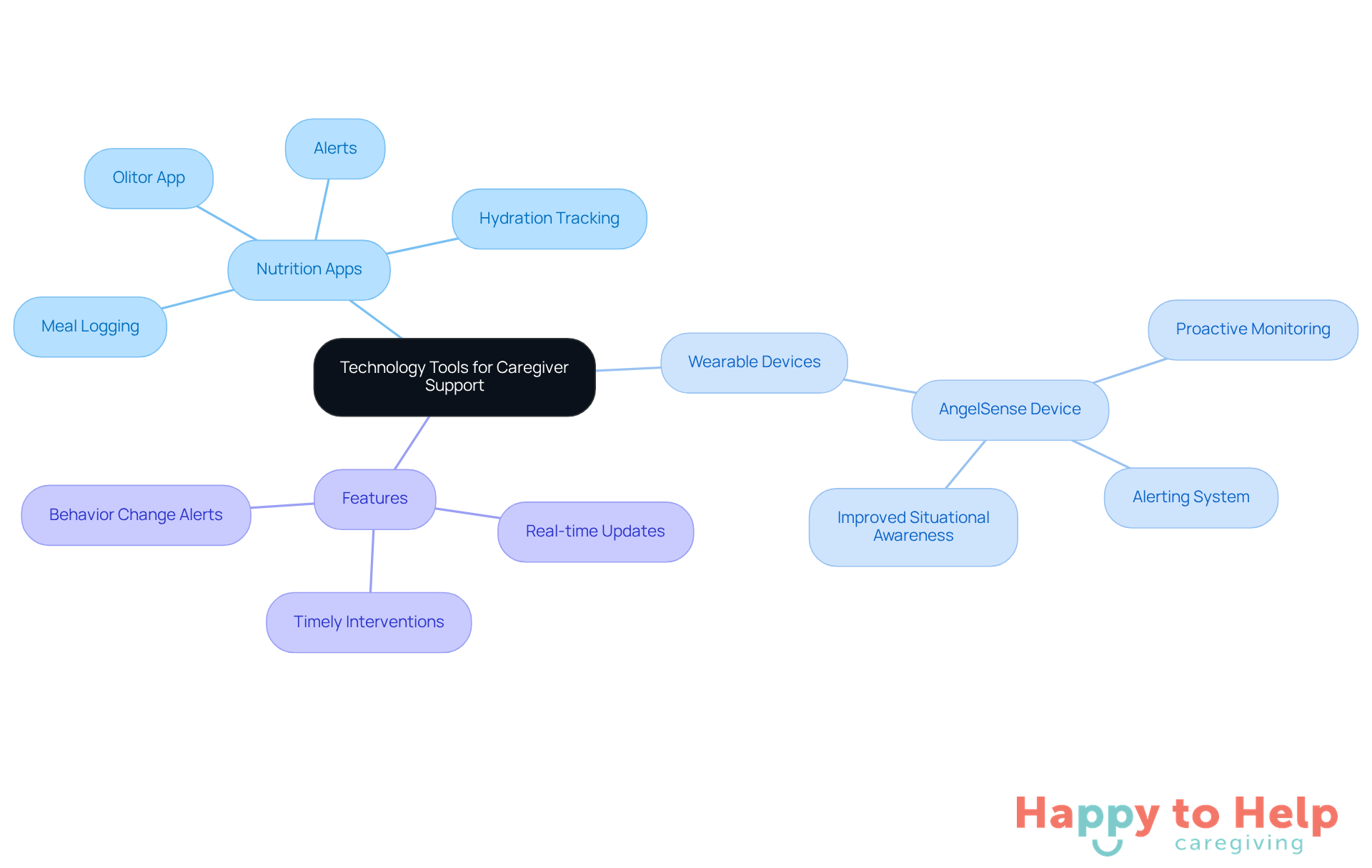
Innovative technology is stepping in to alleviate these burdens. Applications like the Olitor nutrition app allow caregivers to efficiently track food consumption and hydration. A recent pilot study highlighted that caregivers using wearable technology, such as the AngelSense device, reported improved situational awareness and reduced emotional strain. Notably, 70% of participants observed that their care recipients wore the device daily, showcasing its effectiveness in maintaining a routine.
Moreover, specialized apps are being developed to further assist in monitoring nutrition for elderly not eating dementia care. These applications often feature:
- Meal logging
- Hydration tracking
- Alerts for scheduled eating times
By providing real-time updates on dietary habits, these tools can significantly reduce the stress associated with ensuring proper nutrition for the elderly not eating dementia.
Wearable devices enhance this support by alerting caregivers to any changes in behavior or health status, enabling timely interventions. As Dr. Matthew Lee Smith states, "Connected care in a digital world comes with promise and peril," underscoring the importance of these advancements. By integrating technology into caregiving, families can find practical solutions that offer peace of mind while navigating the complexities of dementia care.
Family Involvement: Engaging Loved Ones in the Eating Process for Dementia Patients
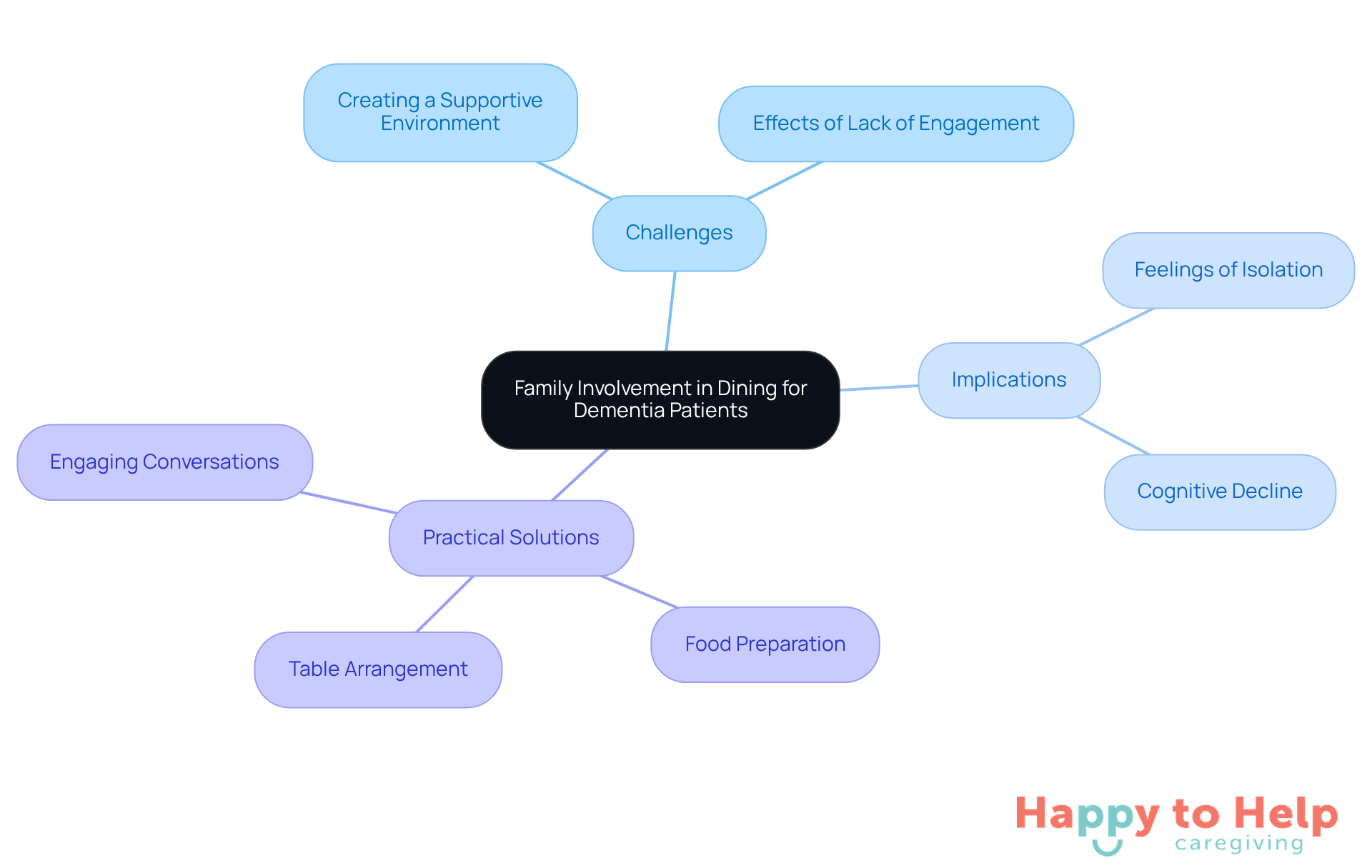
Engaging family members in the eating process presents a significant challenge for caregivers of those who are elderly not eating dementia. Many caregivers struggle to create a supportive dining environment that encourages participation and enhances the overall experience. This lack of engagement can result in elderly not eating dementia, which can lead to decreased appetite and a less enjoyable mealtime atmosphere.
The implications of not involving family members are profound. Without active participation, the elderly not eating dementia may feel isolated, which can exacerbate feelings of distress and cognitive decline. Studies indicate that consistent family involvement during meals can lead to better eating habits and a reduction in distress episodes among the elderly not eating dementia.
To address this issue, caregivers can implement several practical solutions:
- Encouraging family members to assist in food preparation
- Arranging the table
- Engaging in conversations during meals
This active involvement not only provides emotional support but also emphasizes the importance of communal dining. Family therapists note that such interactions create opportunities for connection, which are essential for preserving dignity and identity in individuals experiencing cognitive decline.
By creating a supportive environment, families can significantly enhance the quality of life for their elderly not eating dementia relatives. Making mealtimes a cherished part of the day can transform the dining experience, ensuring that individuals with dementia feel valued and engaged.
Emotional Support: Cultivating Patience and Understanding in Caregiving
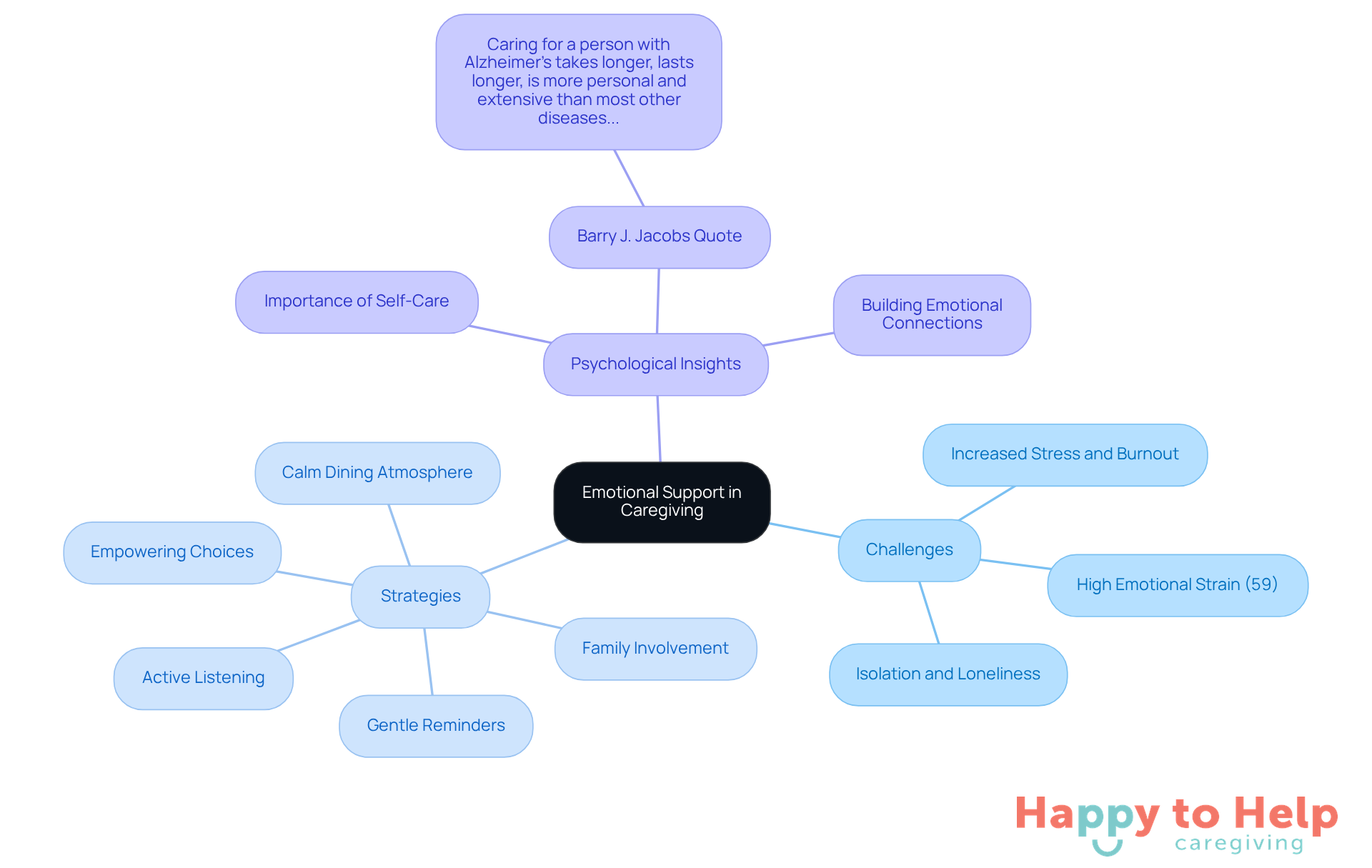
Emotional support is essential in caregiving for individuals with dementia. Caregivers often face the challenge of managing fluctuations in behavior and appetite, as these can be symptoms of elderly not eating dementia rather than intentional actions. This can lead to significant emotional stress, as highlighted by the fact that 59% of dementia supporters experience high emotional strain.
To address this issue, caregivers must cultivate patience and understanding. By taking the time to listen and validate feelings, they can create a supportive environment that encourages the elderly not eating dementia to engage with their meals. This approach not only reduces anxiety during mealtimes but also helps individuals feel more comfortable and secure.
Successful strategies include:
- Creating a calm dining atmosphere
- Offering choices to empower patients
- Using gentle reminders to encourage eating
Psychologists emphasize the importance of patience in caregiving. Barry J. Jacobs, a clinical psychologist, notes, "Looking after an individual with Alzheimer’s requires more time, endures longer, is more intimate and comprehensive than many other illnesses, and imposes a significant burden on the well-being of those providing support."
By prioritizing emotional well-being and acknowledging the challenges faced by caregivers, those providing assistance can significantly enhance the quality of life for their loved ones. Additionally, involving family members in the caregiving process through open communication can further support both caregivers and patients, ensuring a holistic approach to care.
Your Path Forward
Creating an environment that fosters healthy eating habits for elderly individuals with dementia is crucial for their well-being. Caregivers face the challenge of ensuring proper nutrition, which can significantly impact the quality of life for those they support. Without effective strategies, individuals may experience appetite loss and social isolation, exacerbating their condition.
To address these challenges, caregivers can implement several practical solutions:
- Reducing distractions during meals can help individuals focus on their food, enhancing their eating experience.
- Companionship plays a vital role in boosting appetite; having someone to share meals with can make a significant difference.
- It's also essential to address any underlying health issues that may affect eating habits, ensuring that individuals receive the care they need.
- Leveraging technology and involving family members in the mealtime process can further enrich the dining experience.
- For instance, using reminders or meal planning apps can help caregivers stay organized and attentive to their loved ones' needs.
- Engaging family members not only provides support but also fosters a sense of community during meals.
In conclusion, the challenges of ensuring proper nutrition for elderly individuals with dementia can be met with thoughtful strategies and compassionate care. Caregivers are encouraged to adopt these practices and remain vigilant in monitoring their loved ones' needs. By fostering a supportive and engaging mealtime environment, caregivers can help combat the issues of appetite loss and isolation, ultimately enhancing the lives of those affected by dementia.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5MjY2NjFjNWYwOGRhZjJjOGIyMWRmMCIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What services does Happy to Help Caregiving offer for dementia patients?
Happy to Help Caregiving offers tailored in-home assistance, including companionship care, post-hospital recovery assistance, respite care, and palliative support care.
How does Happy to Help Caregiving enhance the quality of life for individuals with cognitive impairment?
They develop individualized care plans that cater to each client's unique needs, promoting independence and well-being while providing compassionate care in a familiar environment.
What strategies can caregivers use to create a comfortable mealtime environment for individuals with dementia?
Caregivers can minimize distractions by lowering noise levels and using gentle lighting, maintaining a clutter-free table setting, incorporating familiar items, and establishing a regular meal timetable to foster a sense of safety.
Why is it important to create a distraction-free dining environment for elderly individuals with dementia?
A calm environment helps improve concentration, reduces distress, and encourages engagement during meals, which is essential for promoting nutrition and social interaction.
How can caregiver involvement impact the appetite of elderly individuals with dementia?
Active participation from caregivers, such as encouragement and companionship during meals, can significantly enhance the dining experience and stimulate appetite, leading to increased food consumption.
What are some effective strategies for caregivers to encourage eating among elderly individuals with dementia?
Strategies include sitting at a small table facing the loved one, allowing ample time for dining, involving the care recipient in food preparation, and creating a calm, distraction-free environment.
List of Sources
- Happy to Help Caregiving: Personalized In-Home Support for Dementia Patients
- Brief, personalized care sessions boost mood in dementia patients by 59 percent, study reveals (https://mcknights.com/news/brief-personalized-care-sessions-boost-mood-in-dementia-patients-by-59-percent-study-reveals)
- Transforming Dementia Care: Our Partnership with PocketRN's Revolutionary GUIDE Program - APAH Corporate (https://aplaceathome.com/blog/transforming-dementia-care-our-partnership-with-pocketrns-revolutionary-guide-program)
- The Alzheimer’s Association and Rippl Partner to Improve Quality Dementia Care and Caregiver Support (https://alz.org/news/2024/the-alzheimer-s-association-and-rippl-partner-to-improve-quality-dementia-care-and-caregiver-support)
- New Medicare program offers much-needed relief for caregivers of dementia patients (https://finance.yahoo.com/news/new-medicare-program-offers-much-needed-relief-for-caregivers-of-dementia-patients-203450020.html)
- Health in the Golden Years: A new idea for providing dementia care for super elderly (https://palmbeachpost.com/story/news/healthcare/2025/08/28/health-in-the-golden-years-dementia-care-poses-huge-challenge/84226729007)
- Dementia-Friendly Mealtimes: Creating a Comfortable Eating Environment
- Hildenborough care home launches dementia-friendly restaurant (https://bbc.com/news/articles/cp8j023er11o)
- Eating out is hard for seniors with dementia and their caregivers. Dementia-friendly dining makes it easier in Central Florida (https://cfpublic.org/2022-06-02/eating-out-is-hard-for-seniors-with-dementia-and-their-caregivers-dementia-friendly-dining-makes-it-easier)
- Hyllden Heights Launches Dementia-Friendly Dining Community Restaurant | Oakland Care Homes (https://oaklandcare.com/latest-news/hyllden-heights-launches-dementia-friendly-dining-community-restaurant)
- Dementia-friendly dining: This Brevard eatery staff trained to offer it. How does it work? (https://floridatoday.com/story/news/2025/07/06/viera-eatery-is-now-a-dementia-friendly-dining-spot-what-is-that/84453610007)
- Hollerbach’s German Restaurant joins Central Florida Dementia-Friendly Dining (https://orlandoweekly.com/food-drink/hollerbachs-german-restaurant-joins-central-florida-dementia-friendly-dining-37383118)
- Caregiver Engagement: Encouraging Appetite Through Companionship
- D-CARE study finds caregiver satisfaction higher with dementia care programs than usual care (https://uclahealth.org/news/release/d-care-study-finds-caregiver-satisfaction-higher-with)
- Nutrition and Dementia: How Caregivers Can Improve Mealtime (https://aarp.org/caregiving/medical/dementia-nutrition-loss-of-appetite)
- Thomas P. Raley Foundation gift fuels UC Davis dementia caregiver education and research (https://health.ucdavis.edu/news/headlines/thomas-p-raley-foundation-gift-fuels-uc-davis-dementia-caregiver-education-and-research/2025/11)
- McLean News | Partnering To Support Families Navigating Mental Health Conditions & Dementia (https://mcleanhospital.org/news/partnering-support-families-navigating-mental-health-conditions-dementia)
- Caregiver Experiences with Dementia-Related Feeding/Eating Difficulties - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10815734)
- Nutritional Strategies: Best Foods to Stimulate Appetite in Dementia Patients
- Best Foods For Dementia Patients To Eat: Guide For Caregivers - NCCDP (https://nccdp.org/best-foods-for-dementia-patients-to-eat-guide-for-caregivers)
- Foods for those with dementia: Examples and tips (https://medicalnewstoday.com/articles/best-foods-for-dementia-patients-to-eat)
- Appetite and dementia (https://alzheimers.org.uk/get-support/living-with-dementia/poor-appetite-dementia)
- MIND and Mediterranean diets linked to fewer signs of Alzheimer’s brain pathology (https://nia.nih.gov/news/mind-and-mediterranean-diets-linked-fewer-signs-alzheimers-brain-pathology)
- Addressing Health Issues: Identifying Causes of Poor Appetite in Dementia
- Weight Loss Drugs May Protect Against Alzheimer’s (https://alzinfo.org/articles/treatment/weight-loss-drugs-may-protect-against-alzheimers)
- Weight loss drug does not slow Alzheimer’s, says drug maker - Alzheimer's Research UK (https://alzheimersresearchuk.org/news/weight-loss-drug-does-not-slow-alzheimers-says-drug-maker)
- Could weight loss drugs help reduce dementia risk? Here's what new studies suggest. (https://cbsnews.com/news/weight-loss-drugs-reduce-dementia-risk)
- Weight-loss drug may slow Alzheimer’s decline (https://imperial.ac.uk/news/255214/weight-loss-drug-slow-alzheimers-decline)
- Could popular weight-loss drugs help treat addiction and dementia? (https://aamc.org/news/could-popular-weight-loss-drugs-help-treat-addiction-and-dementia)
- Hydration Management: Ensuring Adequate Fluid Intake for Dementia Patients
- Drinking, hydration and dementia (https://alzheimers.org.uk/get-support/living-with-dementia/drinking-hydration)
- Hydration Strategies for Adults With Dementia - Alden of Waterford (https://aldenwaterford.com/hydration-strategies-for-adults-with-dementia)
- Why Hydration Is Important for Seniors With Dementia and Tips To Ensure Adequate Intake (https://rightathome.net/blog/hydration-tips-for-seniors-with-dementia)
- Hydration and Dementia (https://ctmuhb.nhs.wales/wise-ctm/news-blog-events/hoot-blog/hydration-and-dementia)
- How to Help Older Adults with Alzheimer’s Stay Hydrated | Juniper Senior Living (https://junipercommunities.com/how-to-help-older-adults-with-alzheimers-stay-hydrated)
- Mealtime Management: Practical Tips for Caregivers of Dementia Patients
- Supporting someone with dementia to eat and drink (https://alzheimers.org.uk/get-support/living-with-dementia/improving-eating-experience-dementia)
- Researchers Pinpoint Strategies to Make Mealtime Easier for Dementia Patients and Caregivers | GreaterGood (https://greatergood.com/blogs/news/mealtime-strategies-dementia-patients)
- Helping caregivers help people with dementia eat at home (https://news.osu.edu/helping-caregivers-help-people-with-dementia-eat-at-home)
- Supporting Nutrition and Hydration | Dementia Adventure (https://dementiaadventure.org/news/supporting-nutrution-and-hydration)
- Technology Tools: Enhancing Caregiver Support for Managing Eating Habits
- Tech-enabled caregiving can help dementia patients stay at home — perhaps for too long (https://statnews.com/2025/11/24/dementia-caregiving-technology-assistance)
- Game-Changing Tech Tools for Dementia Caregivers - Windward Life Care (https://windwardlifecare.com/game-changing-tech-tools-for-dementia-caregivers)
- New NIA grant advances tools for dementia caregiving (https://news-medical.net/news/20251015/New-NIA-grant-advances-tools-for-dementia-caregiving.aspx)
- Advanced Wearable Technology Improves Support For People With Dementia And Their Caregivers (https://stories.tamu.edu/news/2025/02/18/advanced-wearable-technology-improves-support-for-people-with-dementia-and-their-caregivers)
- MSIM students create nutrition app for dementia patients (https://ischool.uw.edu/news/2022/06/msim-students-create-nutrition-app-dementia-patients)
- Family Involvement: Engaging Loved Ones in the Eating Process for Dementia Patients
- Caregiver Experiences with Dementia-Related Feeding/Eating Difficulties - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10815734)
- Care beyond kin: U-M study urges rethink as nontraditional caregivers step up in dementia care (https://ihpi.umich.edu/news-events/news/care-beyond-kin-u-m-study-urges-rethink-nontraditional-caregivers-step-dementia)
- Dementia care programs help, if caregivers can find them (https://cbsnews.com/news/alzheimers-dementia-care-programs-help-if-caregivers-can-find-them)
- The Role of Family Support in Dementia Care - Supportive Care (https://thesupportivecare.com/blog/role-of-family-support-in-dementia-care)
- Emotional Support: Cultivating Patience and Understanding in Caregiving
- The Importance of Emotional Support in Dementia Care - Morris Care (https://morriscare.co.uk/news/emotional-support-in-dementia-care)
- Helpline support eases stress for dementia caregivers | Penn Today (https://penntoday.upenn.edu/news/helpline-support-eases-stress-dementia-caregivers-penn-nursing)
- I Can’t Talk to My Ill Spouse. How Can I Get Support? (https://aarp.org/caregiving/basics/caregiver-find-emotional-support)
- Importance of Emotional Support for Caregivers & Tips for Providing It (https://cprguardian.com/blogs/latest-dementia-news-and-updates/importance-of-emotional-support-for-caregivers-tips-for-providing-it?srsltid=AfmBOoplhPLi6fjWpHPvj3U7s35eoGzhAvpVeGVBR86W8quRquZKwodN)
- Alzheimer’s Association Encourages Dementia Caregivers to Make Their Health and Well-Being an Equal Priority (https://alz.org/news/2024/november-national-family-caregivers-month)