
The Importance of Live-In Nurses Enhance Care
The landscape of caregiving is evolving, presenting significant challenges for families as they care for loved ones. This shift highlights the need for personalized, compassionate support, which is essential for maintaining family dynamics and individual well-being.
As families navigate these complexities, the role of live-in nurses becomes increasingly vital. These dedicated professionals can transform the caregiving experience, alleviating the burdens faced by families. In this article, we will explore ten compelling ways live-in nurses enhance care for family caregivers, focusing on the emotional, physical, and logistical benefits they provide.
How can live-in nurses make a difference? By integrating their expertise into the caregiving process, they offer practical solutions that can significantly improve the quality of care and support for families.
Happy to Help Caregiving: Personalized Live-In Nursing Services
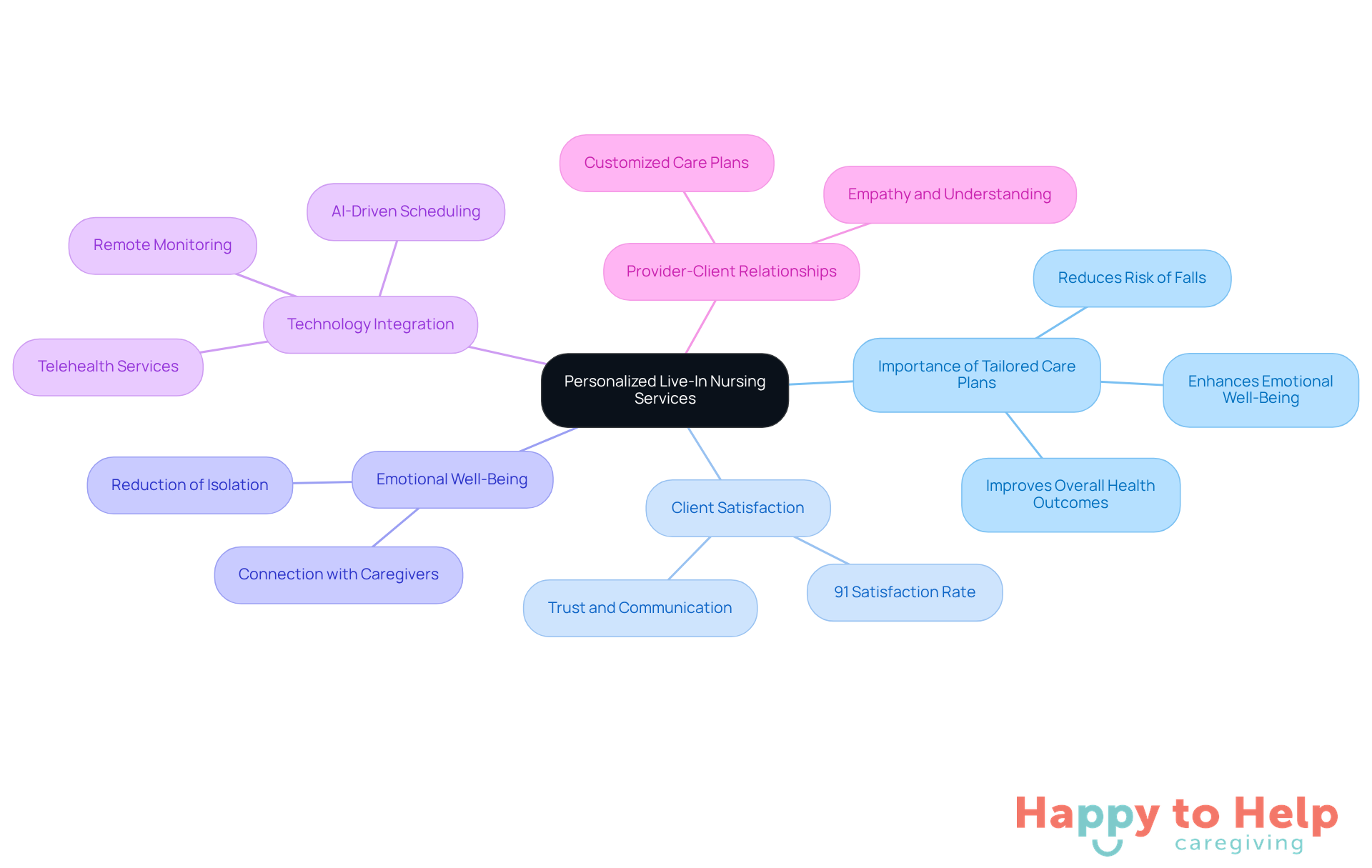
Happy to Help Caregiving addresses a significant problem in the caregiving industry: the lack of personalized support for individuals in need of live in nurses. This gap can lead to feelings of discomfort and insecurity for clients in their own homes. Tailored care plans are essential to ensure that assistance is not only professional but also empathetic, allowing individuals to feel safe and at ease.
The implications of inadequate personalized support are profound. Research indicates that 91% of home support recipients report satisfaction with their providers, underscoring the importance of individualized attention. Live in nurses provide customization that enhances emotional well-being and improves overall health outcomes. For instance, personalized assistance can significantly reduce the risk of falls, a common concern for older adults, as trained support providers offer mobility aid and closely monitor daily activities.
As we look toward 2025, the landscape of personalized support from live in nurses is evolving. There is a growing emphasis on integrating technology to enhance service delivery. Innovations such as AI-driven scheduling and remote monitoring are becoming essential, allowing support providers to focus on more complex tasks while ensuring that individuals receive timely and appropriate assistance. This shift reflects a commitment to maintaining high service standards while adapting to the changing needs of the aging population.
At Happy to Help Caregiving, support providers consistently highlight the importance of tailored care plans. These plans not only improve the quality of care but also strengthen the relationship between providers and clients. This connection is vital, fostering trust and encouraging open communication, which ultimately leads to better health outcomes and a more rewarding caregiving experience.
Emotional Support: Enhancing Quality of Life Through Compassionate Care
Emotional isolation is a significant challenge for many patients, particularly seniors and individuals with special needs. This isolation can lead to feelings of loneliness and negatively impact mental well-being.
Live in nurses play a vital role in addressing this issue by providing crucial emotional support. Through meaningful conversations, engaging activities, and companionship, these caregivers help reduce feelings of isolation and promote a sense of belonging and security.
To enhance the quality of life for patients, caregivers can implement several strategies:
- Engage in regular conversations to foster connection.
- Participate in activities that interest the patient, encouraging interaction and joy.
- Provide companionship to create a supportive environment.
By focusing on these areas, caregivers can significantly improve the emotional well-being of those they care for.
Post-Hospital Recovery: Ensuring Safe Transitions with Live-In Nurses
Problem: Transitioning home after hospitalization can be a daunting experience for clients and their families. The uncertainty of recovery and the need for ongoing care can lead to significant stress and anxiety.
Agitate: Families often worry about whether their loved ones will receive the necessary support during this critical time. Without proper assistance, the risk of complications can increase, making recovery more challenging.
The solution involves live-in nurses, who play a crucial role in ensuring safe transitions for clients returning home. They provide extensive support, including:
- Monitoring vital signs
- Managing medications
- Assisting with daily activities
This not only aids in recovery but also offers families peace of mind, knowing their loved ones are in capable hands.
Companionship Care: Combating Loneliness with Live-In Support
Problem: Loneliness among seniors is a significant issue that can lead to serious health risks.
Agitate: Research shows that loneliness can be as harmful as smoking fifteen cigarettes a day. It not only affects emotional well-being but also contributes to physical decline. Seniors who feel isolated are at a higher risk of health complications, making it crucial to address this issue.
Companionship care provided by live in nurses is essential in alleviating loneliness. By actively engaging seniors in meaningful conversations, hobbies, and social activities, caregivers can nurture vital connections that enhance emotional well-being. Regular interaction not only reduces feelings of isolation but also promotes physical activity and cognitive engagement, both of which are crucial for maintaining overall health.
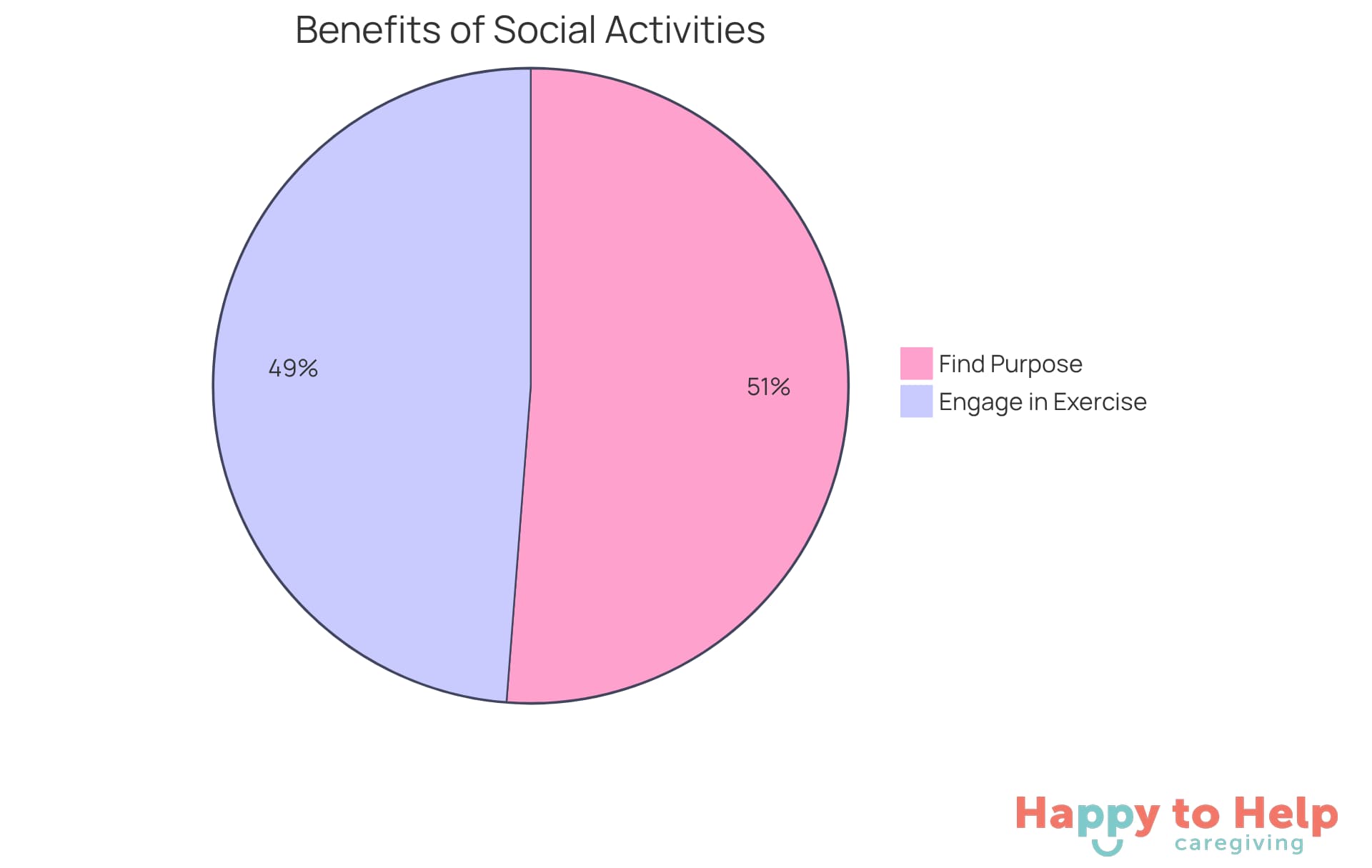
Statistics reveal that seniors participating in social activities are:
- 20% more likely to engage in physical exercise
- 21% more likely to find purpose in their daily lives
Furthermore, the release of oxytocin during these interactions lowers stress levels and supports heart health, while also encouraging the formation of new neural pathways linked to memory retention.
Incorporating live in nurses for companionship care can significantly improve the quality of life for older individuals, ensuring they remain active and engaged.
24/7 Availability: The Flexibility of Live-In Nursing Care
A significant challenge faced by caregivers is the anxiety stemming from the lack of constant support for their loved ones. This concern can weigh heavily on families, as they often worry about their relatives being alone, especially during the night. The emotional toll of caregiving can be profound, leading to stress and uncertainty.
Fortunately, live in nurses provide a practical solution. With 24/7 availability, caregivers can rest assured that their loved ones are never alone. This constant support allows for immediate assistance, whether it’s day or night, alleviating anxiety and providing a sense of security. Families can focus on their own lives, knowing that help is always just a moment away.
Numerous households have reported that having live in nurses has transformed their caregiving experience. As one relative noted, "Having a support person around the clock has transformed everything for us; we can finally breathe knowing someone is always there for Mom." This arrangement not only enhances the quality of life for clients but also offers vital emotional support for families navigating the complexities of caregiving.
Statistics reinforce the value of such services; recent data shows that 91% of supporters express satisfaction with home health services. This highlights the importance of flexible service schedules that cater to individual needs. As demand for these services continues to rise, the ability to adjust support schedules is increasingly recognized as a crucial aspect of effective home health assistance.
Respite Care: Supporting Family Caregivers with Live-In Nurses
Live-in nurses play a crucial role in providing relief services for household caregivers, delivering essential assistance that allows them to take necessary breaks from their caregiving responsibilities. This break is vital for relatives, enabling them to rest, manage personal errands, or simply rejuvenate. By providing expert support during these times, live-in nurses guarantee that clients receive top-notch care, while also enhancing the overall health and well-being of both clients and their loved ones.
The challenges faced by family caregivers are significant. Approximately 63 million individuals in the U.S. provide unpaid labor valued at around $600 billion annually, often leading to considerable burnout. The financial burden of caregiving can be overwhelming, with estimates suggesting that caregivers spend over $2,000 each month on necessary items and services not covered by insurance. The opportunity for caregivers to step away, even briefly, can alleviate stress and enhance their mental well-being, ultimately improving their ability to provide support.
As many caregivers emphasize, taking breaks is essential. One caregiver noted, "I understood that I required time for myself to be a better helper." Another shared, "It’s hard to care for someone else when you’re running on empty." These sentiments highlight the importance of integrating live-in nurses into caregiving, as they provide the necessary support that allows caregivers to maintain their own well-being while ensuring their loved ones receive compassionate and expert attention.
Recent legislative initiatives, such as the Respite Care and Resources for Everyone Act, aim to enhance support for family caregivers, recognizing the critical need for respite services. This ongoing commitment to improving caregiver support underscores the importance of professional assistance in alleviating the burdens faced by family caregivers.
Palliative Support: Compassionate Care for Chronic Illnesses
Palliative support provided by live-in nurses tackles a significant issue: many individuals dealing with chronic illnesses do not receive sufficient care. Research shows that an estimated 56.8 million people require palliative support each year, yet only about 14% receive it. This gap not only exacerbates physical symptoms but also leaves emotional and psychological needs unmet, diminishing overall quality of life.
The implications of this issue are profound. Without proper support, patients may experience increased discomfort and distress, leading to more frequent hospital admissions and lower satisfaction with their care. As Scott Nguy, Vice President of Nurse Practitioner Education, emphasizes, "I want to improve how we assist people with serious illness receive the appropriate support, at the right time."
So, what can be done? Live-in nurses play a crucial role in creating individualized support plans that prioritize dignity and respect. By fostering an environment of empathetic assistance, they ensure that clients receive the comprehensive attention they deserve. This commitment is essential, especially as the World Health Organization recognizes palliative support as a core element of health systems.
To enhance health outcomes, it is vital to tackle the barriers preventing access to palliative support. This includes advocating for more resources and awareness, which can lead to fewer hospital admissions and improved patient satisfaction. As palliative support continues to evolve, the dedication of live-in nurses remains a cornerstone of effective chronic illness management, providing compassionate, personalized care.
Expertise and Training: Ensuring Quality Care from Live-In Nurses
Caregivers often face significant challenges when it comes to providing high-quality support for their loved ones. One major issue is the lack of specialized training, which can lead to inadequate care and increased stress for both caregivers and patients. Without proper knowledge in areas like medication management and chronic illness treatment, the quality of care can suffer, impacting health outcomes and overall satisfaction.
To address these challenges, a viable solution is offered by live-in nurses. They possess comprehensive training and specialized knowledge necessary for live-in nurses to deliver high-quality support. Their expertise includes essential aspects such as:
- Medication management
- Chronic illness treatment
- Emotional support
This ensures they can meet the varied needs of those they serve efficiently. Studies show that specialized training greatly improves the quality of service, resulting in better health outcomes and higher patient satisfaction.
Families can take comfort in knowing that their loved ones are cared for by professionals who are not only skilled but also deeply compassionate and committed to improving their clients' quality of life. As nursing experts emphasize, continuous education and training are essential in upholding high standards of service. Well-trained personnel are crucial in promoting a supportive and healing atmosphere, making a significant difference in the lives of those they care for.
Technology Integration: Enhancing Home Care with Live-In Nursing
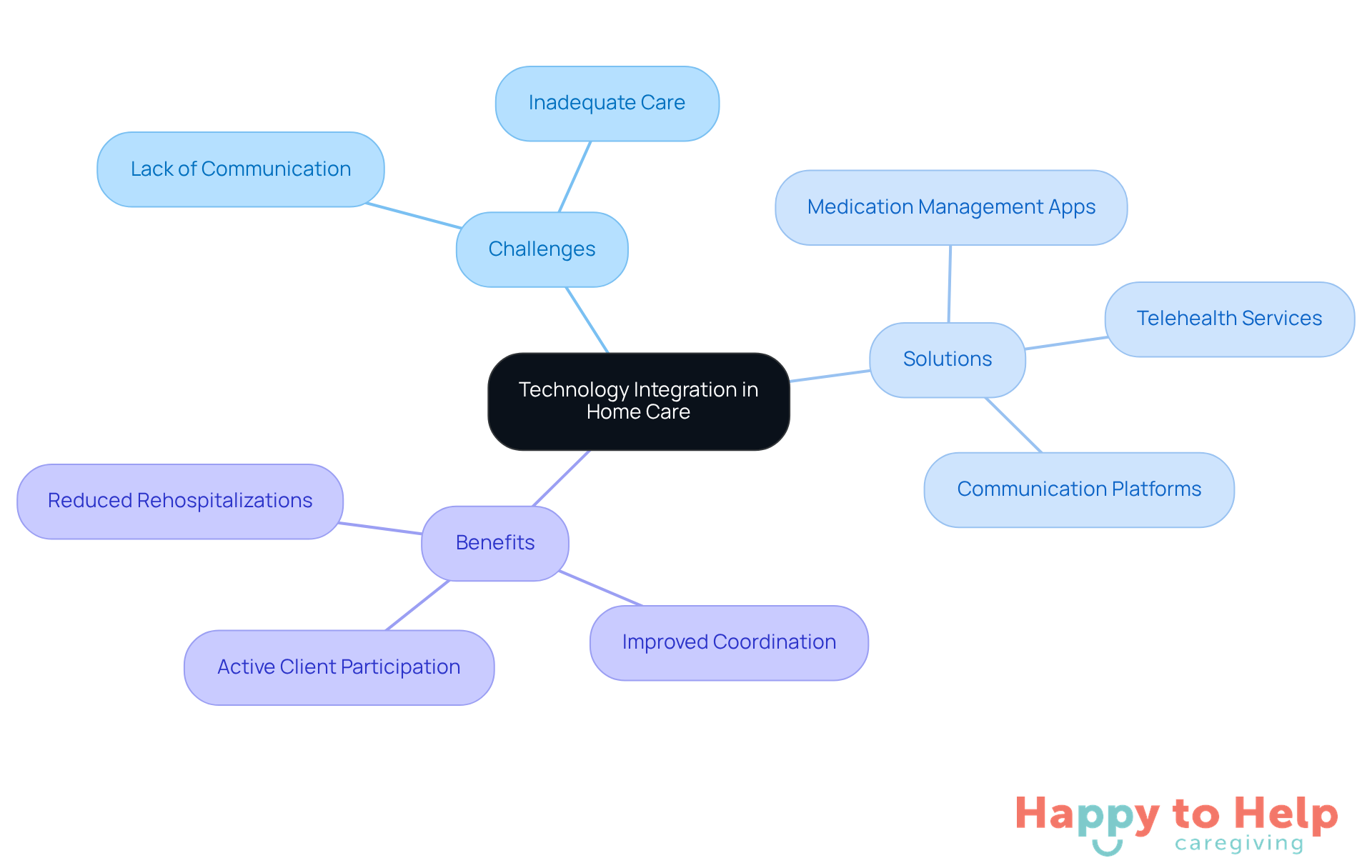
The challenge of providing effective support from live in nurses often stems from a lack of technological integration. Caregivers face difficulties in managing patients' health and keeping families informed, which can lead to miscommunication and inadequate care. This situation not only affects the quality of care but also leaves clients feeling disconnected from their health management.
To address these issues, incorporating technology into caregiving can significantly enhance the overall experience. Tools like telehealth services, medication management applications, and communication platforms empower caregivers to oversee patients' health more effectively. These technologies facilitate better coordination of services and enable clients to take an active role in their health management.
Statistics reveal that telehealth can reduce rehospitalizations by up to 90%, underscoring its effectiveness for live in nurses. Experts in healthcare technology emphasize that adopting telehealth services for live in nurses in home environments is crucial for promoting better communication and ensuring timely interventions.
As the demand for home care continues to grow, the expansion of telehealth services is set to transform the landscape, making care more accessible and efficient for both households and support providers.
Family Dynamics: The Positive Impact of Live-In Nurses on Caregiving
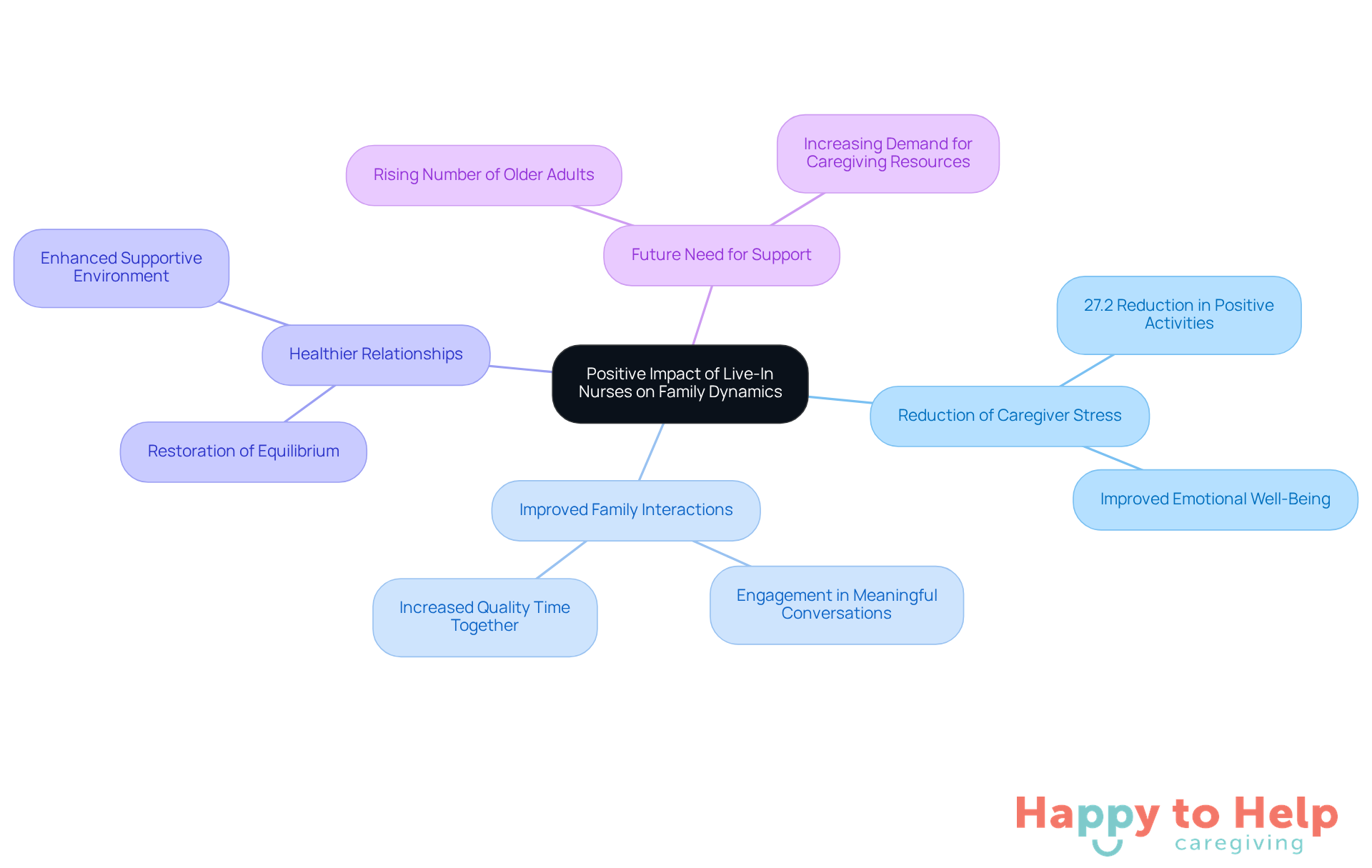
Caregiving can be a heavy burden for many families, often leading to strained relationships and increased stress. According to Coughlin, J., caregivers frequently experience a 27.2% reduction in positive activities in their lives due to these responsibilities. This highlights the pressing need for external support to alleviate this strain.
Live in nurses provide a viable solution, significantly improving household dynamics. By alleviating the caregiving burden, these professionals allow family members to shift their focus from daily responsibilities to nurturing their connections with loved ones. As a result, households experience healthier interactions and reduced stress levels, which are crucial during challenging times.
Successful examples illustrate how live in nurses can transform relationships. Families report engaging in meaningful conversations and activities that were previously overshadowed by caregiving duties. Counselors emphasize that reducing caregiver stress is essential for maintaining healthy relational dynamics. As noted by a domestic therapist, "Professional support restores equilibrium, enabling those who provide assistance to prioritize their emotional well-being and relationships."
This holistic approach not only benefits caregivers but also enhances the entire household, fostering a supportive environment where everyone can thrive. With the anticipated rise in the number of adults aged 85 and older by 2050, the role of live in nurses in supporting family dynamics will become increasingly vital.
Key Takeaways for Caregivers
Caregiving can be an overwhelming responsibility, often leading to significant stress and emotional strain for family caregivers. The demands of providing care can take a toll on their well-being, making it essential to seek effective solutions that alleviate these burdens.
Live-in nurses offer a practical solution to this problem. By providing personalized care plans, emotional support, and around-the-clock assistance, they not only help reduce the pressures of caregiving but also create a nurturing environment where clients can thrive. This support is crucial, especially during post-hospital recovery and for companionship care, where emotional connections can significantly enhance the quality of life.
Moreover, the integration of technology in live-in nursing services can improve health management, ensuring that caregivers have the tools they need to provide effective care. Tailored care and professional training are vital components that ensure high-quality support, addressing the unique needs of each family.
As the demand for compassionate and personalized care continues to rise, families should view live-in nursing services as a vital resource rather than just assistance. Embracing this approach can lead to a more balanced and fulfilling caregiving experience, ultimately fostering a supportive atmosphere where everyone can flourish. By considering the benefits of live-in nurses, families can enhance their quality of life and strengthen their relationships.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5Mjc5NGVlMjI0NDc2YzA3YjhmODliMiIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What problem does Happy to Help Caregiving address in the caregiving industry?
Happy to Help Caregiving addresses the lack of personalized support for individuals in need of live-in nurses, which can lead to discomfort and insecurity for clients in their own homes.
Why are tailored care plans important in caregiving?
Tailored care plans are essential because they ensure assistance is both professional and empathetic, allowing individuals to feel safe and at ease while enhancing emotional well-being and improving overall health outcomes.
What percentage of home support recipients report satisfaction with their providers?
Research indicates that 91% of home support recipients report satisfaction with their providers.
How can personalized assistance benefit older adults?
Personalized assistance can significantly reduce the risk of falls, as trained support providers offer mobility aid and closely monitor daily activities.
What technological innovations are being integrated into personalized support for live-in nurses?
Innovations such as AI-driven scheduling and remote monitoring are being integrated to enhance service delivery, allowing support providers to focus on more complex tasks while ensuring timely assistance.
How do tailored care plans impact the relationship between providers and clients?
Tailored care plans improve the quality of care and strengthen the relationship between providers and clients, fostering trust and encouraging open communication, which leads to better health outcomes.
What challenge do many patients, especially seniors, face regarding emotional well-being?
Many patients face emotional isolation, which can lead to feelings of loneliness and negatively impact their mental well-being.
How do live-in nurses help with emotional support?
Live-in nurses provide crucial emotional support through meaningful conversations, engaging activities, and companionship, helping to reduce feelings of isolation and promote a sense of belonging and security.
What strategies can caregivers implement to enhance the quality of life for patients?
Caregivers can engage in regular conversations, participate in activities that interest the patient, and provide companionship to create a supportive environment.
What issues do clients and families face when transitioning home after hospitalization?
Clients and families often experience stress and anxiety due to uncertainty about recovery and the need for ongoing care, leading to worries about whether their loved ones will receive the necessary support.
What role do live-in nurses play in post-hospital recovery?
Live-in nurses provide extensive support during the transition home, including monitoring vital signs, managing medications, and assisting with daily activities, which aids in recovery and offers families peace of mind.
List of Sources
- Happy to Help Caregiving: Personalized Live-In Nursing Services
- Top 5 Home Care Trends of 2025 - Family & Nursing Care (https://familynursingcare.com/top-5-home-care-trends-of-2025)
- Home Care Statistics In 2025: Key Insights In Home Care (https://sagapixel.com/marketing/home-care-statistics)
- State of home care in 2025 (https://mcknightshomecare.com/state-of-home-care-in-2025)
- 2025 Home Care Statistics: Trends & Insights To Know (https://premierhcinc.com/blog/home-care-statistics)
- How 3 Top Trends Have Shaped Home-Based Care This Year (https://homehealthcarenews.com/2025/08/how-3-top-trends-have-shaped-home-based-care-this-year)
- Emotional Support: Enhancing Quality of Life Through Compassionate Care
- 10 Benefits of Professional Companion Services for Family Caregivers - Happy To Help (https://happytohelpcaregiving.com/10-benefits-of-professional-companion-services-for-family-caregivers)
- Companionship Services: Combatting Senior Loneliness in 2025 (https://bestsunshinehomecare.com/companionship-services-senior-loneliness-2025)
- Mental health of older adults (https://who.int/news-room/fact-sheets/detail/mental-health-of-older-adults)
- Benefits of Companion Care for Seniors in California - 2025 (https://findinghomecare.net/benefits-of-companion-care-for-seniors)
- The Unbeatable Benefits of Companion Care for Seniors (https://comforcare.com/massachusetts/canton/resources/blog/the-unbeatable-benefits-of-companion-care-for-seniors)
- Post-Hospital Recovery: Ensuring Safe Transitions with Live-In Nurses
- Sent Home To Heal, Patients Avoid Wait for Rehab Home Beds - KFF Health News (https://kffhealthnews.org/news/article/patients-rehab-at-home-unclog-hospital-bed-nursing-home-waiting-list)
- Navigating The Transition: From Hospital To Home Care: What Families Should Know - New York Health Care (https://nyhc.com/navigating-the-transition-from-hospital-to-home-care-what-families-should-know)
- Home Care Impact on Recovery of Patient (A Statistics Report) (https://lovinghomecareinc.com/home-care-recovery-statistics)
- Hospital-at-Home Interventions vs In-Hospital Stay for Patients With Chronic Disease Who Present to the Emergency Department: A Systematic Review and Meta-analysis - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC8188269)
- The Family Perspective on Hospital to Home Transitions: A Qualitative Study (https://publications.aap.org/pediatrics/article/136/6/e1539/33897/The-Family-Perspective-on-Hospital-to-Home)
- Companionship Care: Combating Loneliness with Live-In Support
- Companion Care at Home Reduces Loneliness for Seniors During the Holidays (https://lifesathomecare.com/companion-care-at-home-reduces-loneliness-for-seniors-during-the-holidays)
- McKnight's article: Research shows senior care facilities can reverse loneliness (https://wisconsinillinoisseniorhousing.org/blog/mcknight-s-article-research-shows-senior-care-facilities-can-reverse-loneliness)
- 1 in 3 older adults still experience loneliness and isolation (https://michiganmedicine.org/health-lab/1-3-older-adults-still-experience-loneliness-and-isolation)
- U.S. News Survey Finds Senior Living Reduces Loneliness (https://sunriseseniorliving.com/resources/caregivers-and-families/senior-living-reduces-loneliness)
- Trends in Loneliness Among Older Adults from 2018-2023 (https://ihpi.umich.edu/national-poll-healthy-aging/reports-and-resources/trends-loneliness-among-older-adults-2018-2023)
- 24/7 Availability: The Flexibility of Live-In Nursing Care
- The Caregiving Landscape: Data & Insights on the Caregiver Experience in the U.S. (https://caregiveraction.org/caregiver-statistics)
- 52 Eye-Opening Home Health Statistics: Insights for 2025 (https://boosthomehealth.com/home-health-statistics)
- National Alliance for Caregiving: Caregiving in the US 2025 Report (https://johnahartford.org/resources/view/national-alliance-for-caregiving-caregiving-in-the-us-2025-report)
- The Difference Between 24-Hour Care & Live-In Care (https://corewoodcare.com/news/24-hour-vs-live-in-care)
- Caregiver Statistics: Demographics (https://caregiver.org/resource/caregiver-statistics-demographics)
- Respite Care: Supporting Family Caregivers with Live-In Nurses
- A bill in Congress would return $5,000 to millions of family caregivers every year, but will it pass? (https://cbsnews.com/newyork/news/credit-for-caring-act-family-caregiver-tax-credit)
- Funding Opportunity: National Lifespan Respite Care Program State Program Enhancement Grants | ACL Administration for Community Living (https://acl.gov/news-and-events/announcements/national-lifespan-respite-care-program-state-program-enhancement)
- New Bill: Senator Edward J. Markey introduces S. 3231: Respite Care and Resources for Everyone Act | AMGN Stock News (https://quiverquant.com/news/New+Bill:+Senator+Edward+J.+Markey+introduces+S.+3231:+Respite+Care+and+Resources+for+Everyone+Act)
- Federal budget committee greenlights millions in spending for family caregivers, respite services (https://mcknightshomecare.com/news/federal-budget-committee-greenlights-millions-in-spending-for-family-caregivers-respite-services)
- Palliative Support: Compassionate Care for Chronic Illnesses
- Palliative care (https://who.int/news-room/fact-sheets/detail/palliative-care)
- Nurturing a Community of Caregivers: Scott’s Story (https://advancingexpertcare.org/news/nurturing-a-community-of-caregivers-scotts-story)
- Importance of Palliative Care - A PBS News Hour “Brief but Spectacular” Series (https://cambiahealthfoundation.org/posts/blog/2021-05-11/importance-of-palliative-care---a-pbs-news-hour-brief-b.html)
- Expertise and Training: Ensuring Quality Care from Live-In Nurses
- 85 Nursing Quotes: Words of Wisdom for Nurses | USAHS (https://usa.edu/blog/nursing-quotes)
- The State of Training in Home-Based Care: Key Takeaways (https://homehealthcarenews.com/2023/10/the-state-of-training-in-home-based-care-key-takeaways)
- AAG Health - HR in Healthcare: 61 Statistics and Trends for 2025 (https://aag.health/post/hr-in-healthcare-statistics-trends)
- Fact Sheet: Strengthening the Health Care Workforce | AHA (https://aha.org/fact-sheets/2021-05-26-fact-sheet-strengthening-health-care-workforce)
- Technology Integration: Enhancing Home Care with Live-In Nursing
- Technology Archives (https://skillednursingnews.com/category/technology)
- Can AI care for your loved ones in their old age? (https://bbc.com/news/articles/c62z5yl2l1lo)
- How Nursing Technology Is Enhancing Patient Care | ANA (https://nursingworld.org/content-hub/resources/workplace/how-technology-is-changing-the-nursing-industry)
- Products - Data Briefs - Number 445 - October 2022 (https://cdc.gov/nchs/products/databriefs/db445.htm)
- ‘Perfect storm’ hitting assisted living requires leveraging technology to improve outcomes (https://mcknightsseniorliving.com/news/perfect-storm-hitting-assisted-living-requires-leveraging-technology-to-improve-outcomes)
- Family Dynamics: The Positive Impact of Live-In Nurses on Caregiving
- Fact Sheet: Trends in Family Care for Older Americans (https://prb.org/resources/fact-sheet-trends-in-family-care-for-older-americans)
- The National Alliance for Caregiving and AARP Release Caregiving Report - CAPC - News Bites (https://capc.org/blog/new-data-on-family-caregivers-in-the-us)
- Caregiver Statistics: Demographics (https://caregiver.org/resource/caregiver-statistics-demographics)
- Caregiving Statistics US 2025: Insights for Family Caregivers (https://zencaregiving.org/caregiving-statistics-us-2025)

