
The Importance of Address Dementia and Hunger in
Dementia significantly impacts appetite, presenting a complex challenge that can jeopardize the nutritional well-being of individuals in care. Caregivers often face the daunting task of ensuring proper nutrition while navigating the cognitive decline that alters hunger cues and food preferences. This can lead to potential malnutrition, which is a serious concern.
How can caregivers effectively tackle these intertwined challenges of dementia and hunger? Addressing this issue is crucial for fostering healthier eating habits and improving the quality of life for those they support. This guide explores actionable strategies that caregivers can implement to:
- Create a supportive mealtime environment
- Enhance communication
- Promote better nutrition for individuals facing these difficulties
Understand the Impact of Dementia on Appetite
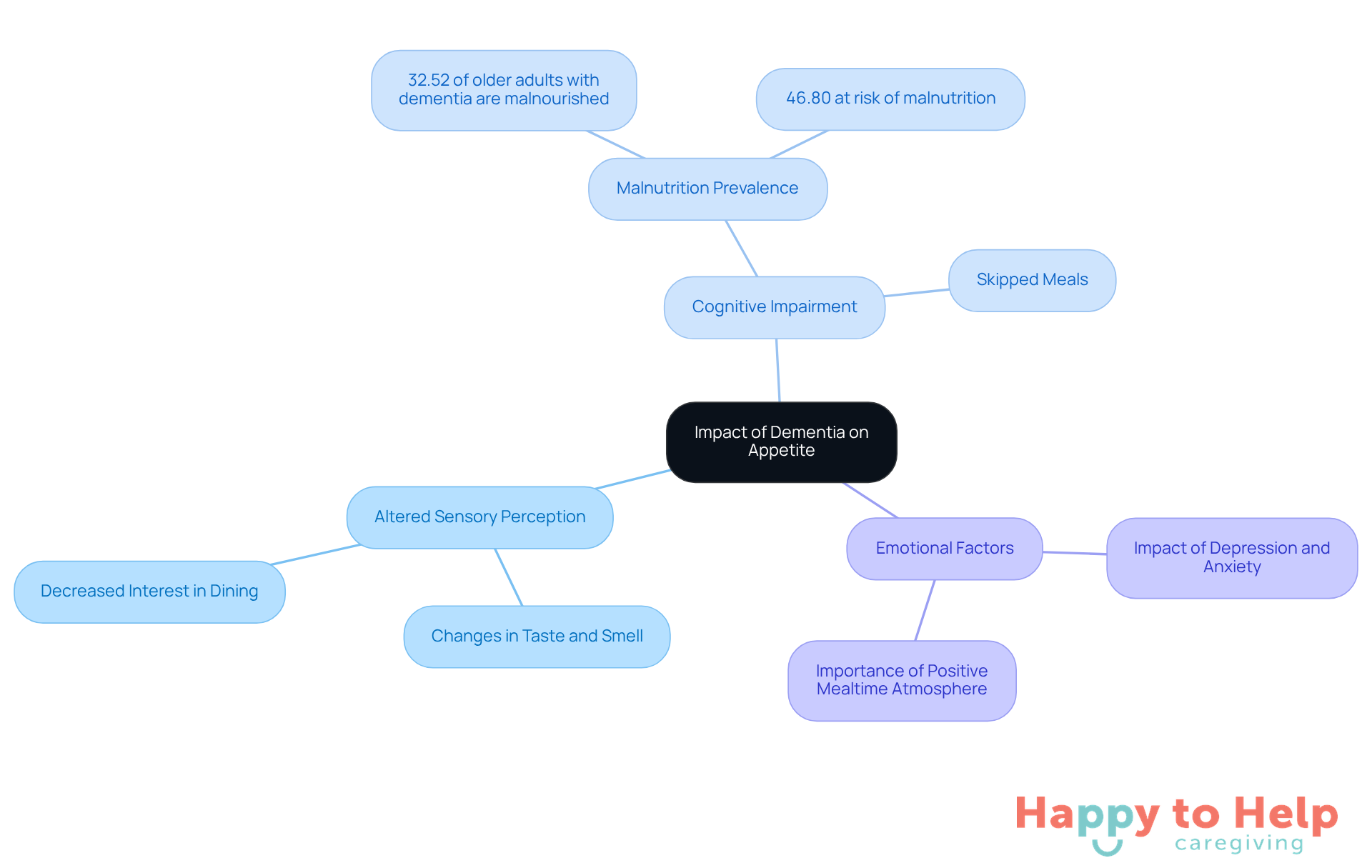
Dementia significantly impacts a person's appetite, highlighting the connection between dementia and hunger due to changes in brain function that affect taste and smell perceptions. Research indicates that approximately 32.52% of older adults with cognitive impairment are malnourished, with nearly 46.80% at risk of malnutrition. These statistics highlight a critical problem: caregivers must recognize that individuals experiencing dementia and hunger may not only forget to eat but may also fail to recognize their hunger cues altogether.
Emotional factors, such as depression and anxiety, can further suppress appetite, making it essential for caregivers to foster a positive mealtime atmosphere.
-
Altered Sensory Perception: Changes in taste and smell can make dishes less appealing, leading to decreased interest in dining.
-
Cognitive impairment, including issues related to dementia and hunger, can lead to skipped meals and worsen nutritional deficiencies.
-
Emotional Factors: Feelings of sadness or anxiety can diminish appetite, underscoring the importance of creating a supportive and enjoyable dining experience.
Real-world examples illustrate these challenges. Caregivers have observed that people with cognitive decline may acquire new food preferences or lose interest in dishes they previously liked. This requires experimentation with flavors and dining settings. By understanding these dynamics, caregivers can implement tailored strategies that address the unique needs of those they support, ultimately enhancing their overall well-being.
Identify Signs of Appetite Changes in Patients
Caregivers face a significant challenge when it comes to monitoring changes in eating habits, as these can signal underlying health issues. Recognizing these changes is crucial for ensuring the well-being of those in their care.
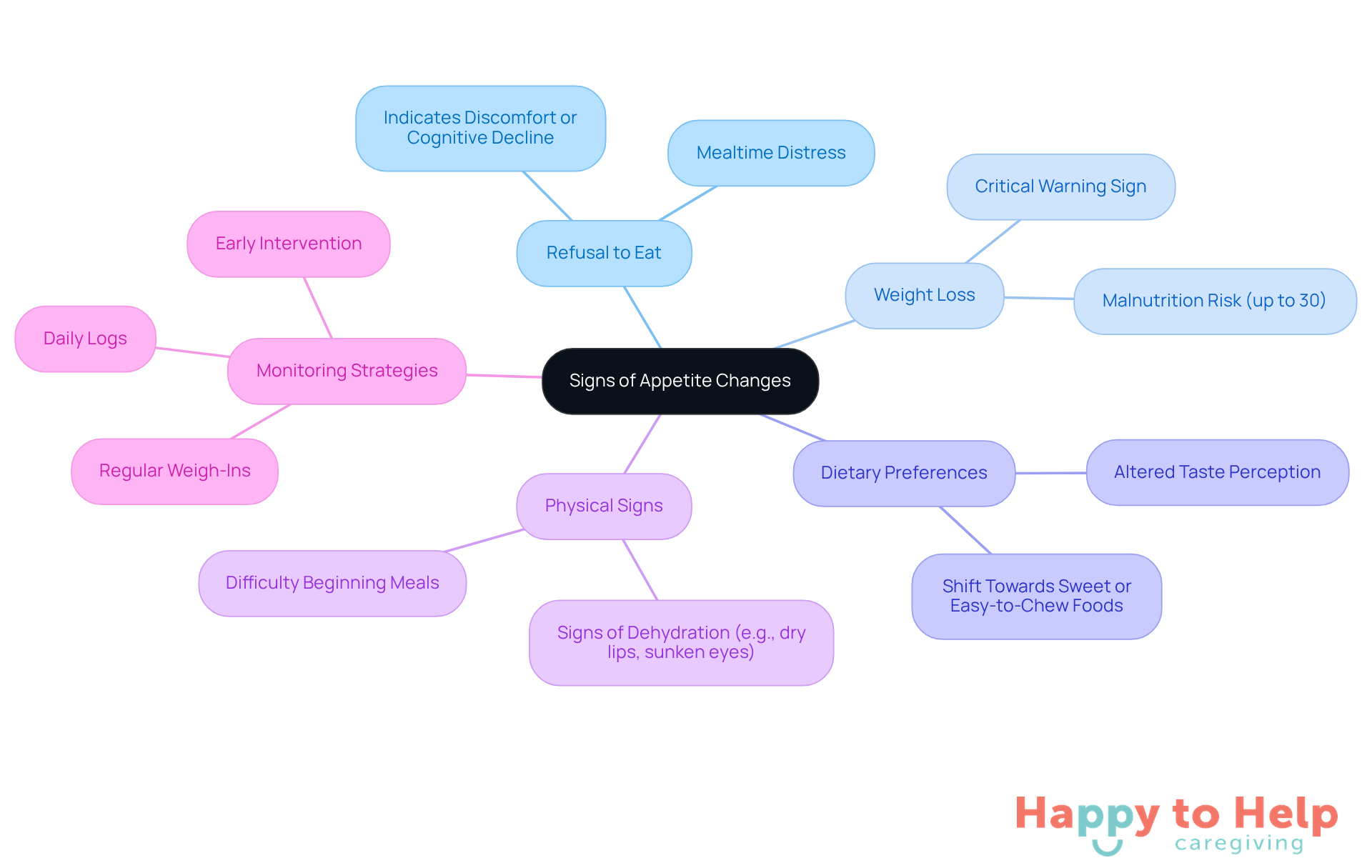
Problem: One major concern is the refusal to eat. A consistent refusal of meals or snacks can indicate discomfort or cognitive decline. Additionally, weight loss is a critical warning sign; noticeable weight loss over a short period should never be overlooked. Research indicates that many patients with dementia and hunger experience considerable weight loss, with up to 30% confronting malnutrition.
Agitate: Changes in dietary preferences can also be alarming. A shift towards specific types of cuisine, especially sweet or easy-to-chew options, may reflect alterations in sensory perception and cognitive function. Dementia often alters taste perception, leading individuals to prefer stronger flavors or unusual combinations. Furthermore, caregivers should be vigilant for physical signs of dehydration, such as dry lips or sunken eyes, which can complicate nutritional intake.
Solution: To effectively monitor these issues, caregivers can implement several strategies. Daily logs are invaluable; maintaining a record of food intake and any behavioral changes related to eating can provide insights into the individual's nutritional status. Regular weigh-ins are also essential. Weekly weigh-ins can help track significant weight changes, allowing for timely interventions when necessary. Early intervention is crucial, as poor nutrition can accelerate cognitive decline.
By recognizing these signs and employing effective monitoring methods, caregivers can better support the nutritional needs of individuals facing challenges related to dementia and hunger, ultimately enhancing their quality of life.
Implement Strategies to Encourage Healthy Eating
To promote healthy eating among individuals, caregivers face a significant challenge related to dementia and hunger. Many individuals may struggle with appetite and nutrition due to issues related to dementia and hunger, which can lead to further health complications.
-
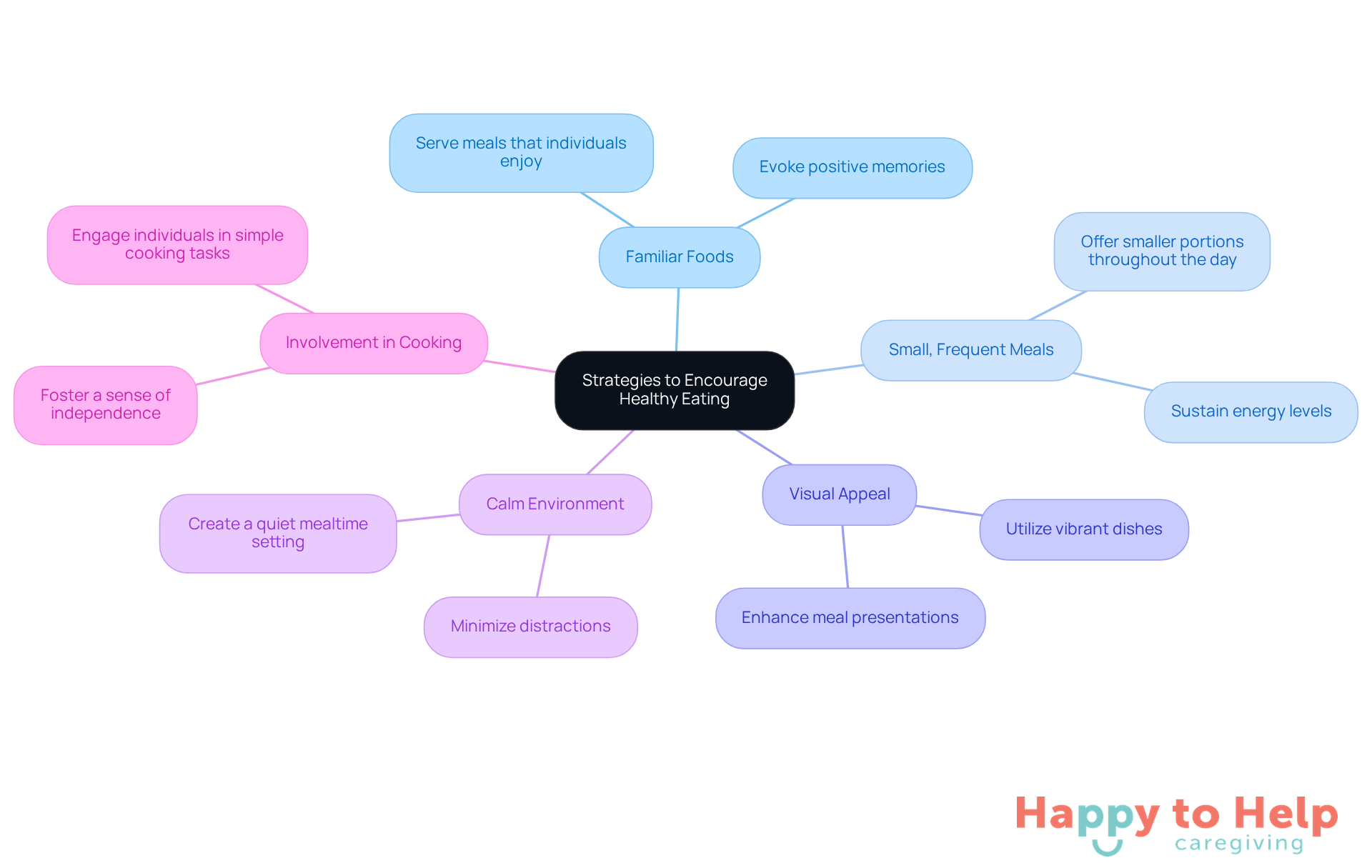
Familiar Foods: Serving meals that individuals enjoy and recognize can significantly stimulate appetite. Familiarity with certain foods can evoke positive memories and feelings, making mealtimes more enjoyable.
-
Small, Frequent Meals: Offering smaller portions more frequently throughout the day can prevent individuals from feeling overwhelmed. This method not only reduces the strain of substantial portions but also assists in sustaining energy levels and nutritional consumption.
-
Visual Appeal: Utilizing vibrant dishes and contrasting hues for meals can enhance the visual allure of presentations. A visually stimulating presentation encourages people to engage with their food, making the dining experience more inviting.
-
Calm Environment: Creating a quiet, distraction-free mealtime setting is crucial. Minimizing background noise and visual disturbances enables individuals to concentrate on their food, which can aid in reducing anxiety and confusion.
Additionally, caregivers can incorporate snacks between meals to help increase overall caloric intake, ensuring that individuals receive adequate nutrition throughout the day. Involving individuals in cooking tasks can also boost their interest in nutrition. Simple tasks, such as choosing ingredients or arranging food, foster a sense of independence and connection to the meal.
By applying these strategies, caregivers can create a supportive and pleasant dining atmosphere that promotes healthy eating practices for individuals facing dementia and hunger. With over 6 million Americans believed to be affected by cognitive decline, these strategies are crucial for ensuring their nutritional needs are fulfilled. For example, Anna's 84-year-old mother, diagnosed with Alzheimer's-related cognitive decline, benefits from familiar foods and a calm mealtime atmosphere. Furthermore, caregivers may consider utilizing services such as Meals on Wheels to provide nutritious food directly to their loved ones' residences, guaranteeing they obtain the vital vitamins and minerals required for their well-being.
Create a Supportive Mealtime Environment
Establishing a nurturing mealtime atmosphere is crucial for improving the dining experience for people with cognitive decline. Caregivers often face the challenge of ensuring that mealtimes are not only nutritious but also enjoyable and stress-free for individuals experiencing dementia and hunger. Without a supportive environment, these individuals may feel anxious or overwhelmed, which can negatively impact their eating habits and lead to challenges associated with dementia and hunger.
To address this issue, here are key strategies to consider:
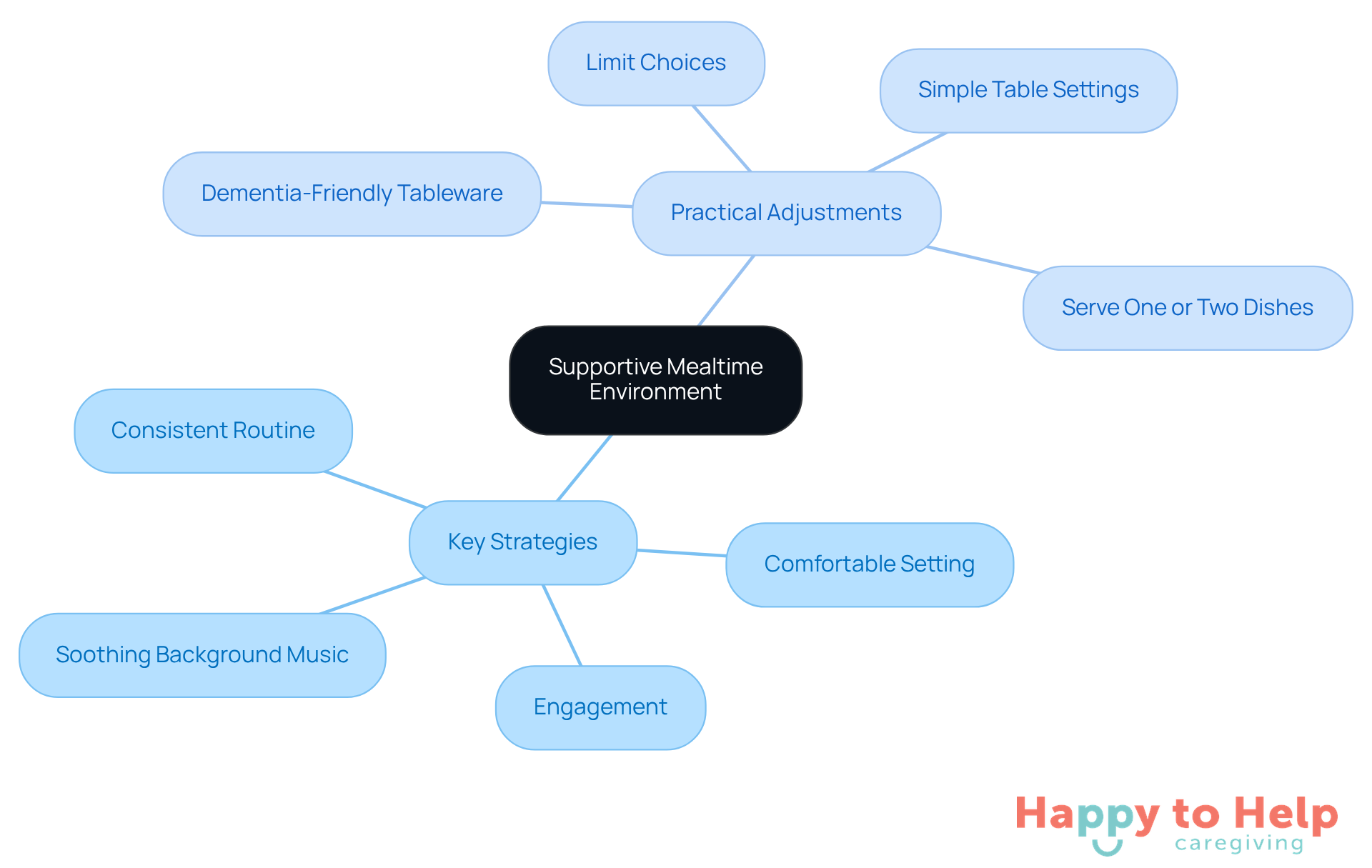
- Consistent Routine: Establishing a regular mealtime by serving meals at the same time each day fosters predictability. This routine helps individuals cope with dementia and hunger, making them feel more secure and improving their overall eating habits.
- Comfortable Setting: Ensure that the dining area is comfortable, well-lit, and free from clutter. A familiar and inviting environment can significantly enhance the mealtime experience.
- Soothing Background Music: Playing gentle tunes can create a tranquil ambiance, enhancing dining experiences and reducing stress for those who may feel uneasy or disoriented.
- Engagement: Encourage conversation about pleasant topics during dining. This not only makes the experience more enjoyable but also helps stimulate cognitive function and social interaction.
Practical Adjustments:
- Use Simple Table Settings: Avoid overly complicated table settings that may confuse the individual. A straightforward setup can help them concentrate on the food itself.
- Limit Choices: Offer two or three meal options to prevent decision fatigue. This method streamlines the process and can result in improved dietary selections. As mentioned by the Alzheimer's Society, restricting options can assist those facing dementia and hunger in preventing feelings of being overwhelmed.
- Serve One or Two Dishes at a Time: Presenting one or two dishes at a time instead of a full plate can lessen overwhelm and make it simpler for people to savor their dining experience. This strategy aligns with the toolkit launched in 2024, which emphasizes practical adjustments for mealtime.
- Utilize Dementia-Friendly Tableware: Using colored plates that contrast with the food can aid visibility, making it easier for people to see and engage with their meals. This simple adjustment can significantly enhance the dining experience.
By employing these strategies, caregivers can establish a supportive mealtime atmosphere that fosters dignity, safety, and enjoyment for people experiencing cognitive decline.
Enhance Communication to Address Hunger Needs
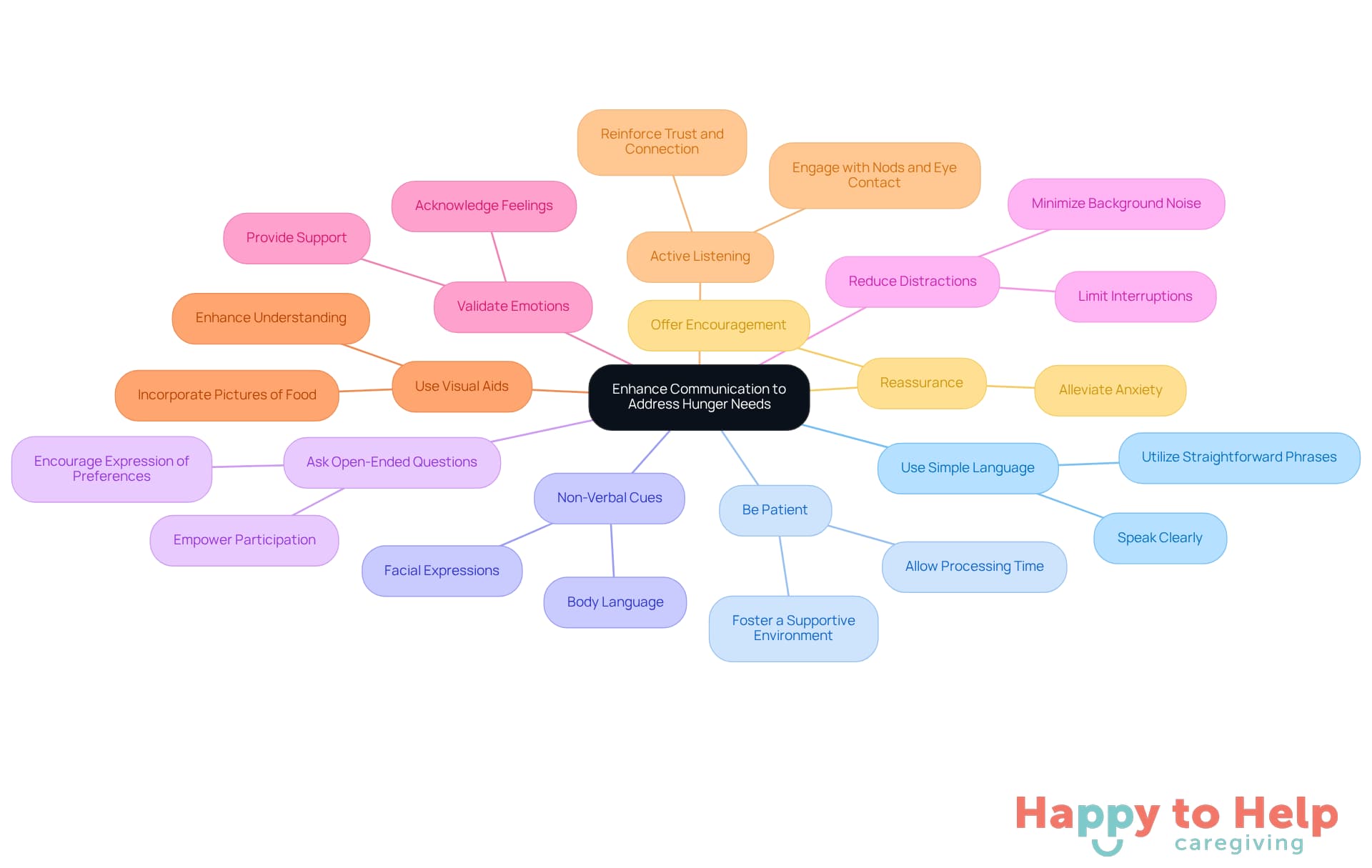
Effective communication is essential for understanding and addressing the needs of people experiencing dementia and hunger. Caregivers often face challenges in this area, which can lead to misunderstandings and unmet needs. To improve interactions, caregivers can employ several key techniques:
- Use Simple Language: Speak clearly and utilize straightforward phrases to convey messages. This helps reduce confusion and ensures that the person can grasp the information being shared.
- Be Patient: Allow ample time for the person to process information and respond. This patience fosters a supportive environment where they feel comfortable expressing their needs.
- Non-Verbal Cues: Pay close attention to body language and facial expressions, as these can provide valuable insights into their feelings about meals and mealtimes.
- Ask Open-Ended Questions: Encourage the person to express their preferences by posing questions like, 'What would you like to eat today?' This approach empowers them to participate in their care actively.
- Reduce Distractions: Minimize background noise and other interruptions during mealtimes to help the person concentrate on the meal and the discussion.
- Validate Emotions: Recognize and affirm the emotions of those with cognitive impairment, as this can assist them in feeling understood and supported.
- Use Visual Aids: Incorporate visual aids, such as pictures of food, to enhance understanding and engagement during mealtimes.
Additionally, caregivers can implement these communication techniques:
- Active Listening: Demonstrate that you are engaged by nodding and maintaining eye contact, which reinforces trust and connection.
- Reassurance: Offer reassurance and encouragement to alleviate anxiety surrounding mealtimes. A calm demeanor can significantly enhance the dining experience for individuals with dementia.
By implementing these strategies, caregivers can create a more effective and compassionate caregiving environment, ultimately improving the quality of life for those they support.
Key Takeaways for Caregivers
Addressing the intersection of dementia and hunger in caregiving presents a significant challenge. Caregivers often face the dual problem of ensuring proper nutrition while navigating the complexities of dementia, which can profoundly affect appetite and eating habits. This situation not only impacts the physical health of those they care for but also their emotional well-being.
Recognizing the signs of appetite changes is crucial. Caregivers must be aware of how dementia can alter eating behaviors, leading to potential nutritional deficiencies. This awareness can agitate the situation, as inadequate nutrition can exacerbate cognitive decline and diminish quality of life.
To combat these challenges, caregivers can implement several practical solutions:
- Monitoring dietary preferences and utilizing familiar foods can encourage healthy eating.
- Creating calm dining environments promotes engagement and comfort, making mealtimes more enjoyable.
- Effective communication techniques empower caregivers to better understand and meet the needs of individuals experiencing cognitive decline, transforming mealtimes into positive experiences rather than sources of stress.
Ultimately, caregivers hold the responsibility to cultivate an environment that supports both the nutritional and emotional needs of individuals with dementia. By adopting these strategies, they can significantly enhance the quality of life for those they support. Every meal can become not just about sustenance, but also about dignity, connection, and joy. Embracing these practices can lead to profound improvements in the daily lives of individuals facing the challenges of dementia and hunger.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5NDFmMzRhMTE4MTVjMDQxY2UzNWU1OCIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
How does dementia affect appetite?
Dementia significantly impacts appetite due to changes in brain function that affect taste and smell perceptions. Individuals with dementia may forget to eat or fail to recognize their hunger cues, leading to malnutrition.
What are the statistics regarding malnutrition in older adults with cognitive impairment?
Approximately 32.52% of older adults with cognitive impairment are malnourished, and nearly 46.80% are at risk of malnutrition.
What emotional factors can suppress appetite in individuals with dementia?
Emotional factors such as depression and anxiety can further suppress appetite, making it essential for caregivers to create a positive mealtime atmosphere.
What sensory changes affect the eating habits of those with dementia?
Alterations in taste and smell can make food less appealing, leading to decreased interest in dining and potentially causing individuals to acquire new food preferences or lose interest in previously liked dishes.
What signs should caregivers look for regarding appetite changes in dementia patients?
Caregivers should monitor for consistent refusal to eat, noticeable weight loss, changes in dietary preferences, and physical signs of dehydration, such as dry lips or sunken eyes.
Why is it important to recognize changes in eating habits for individuals with dementia?
Recognizing changes in eating habits is crucial as they can signal underlying health issues, including cognitive decline and malnutrition.
What strategies can caregivers implement to monitor appetite changes effectively?
Caregivers can maintain daily logs of food intake and behavioral changes, conduct regular weigh-ins to track significant weight changes, and intervene early to address poor nutrition.
How can poor nutrition impact individuals with dementia?
Poor nutrition can accelerate cognitive decline, making it vital for caregivers to support the nutritional needs of those facing challenges related to dementia and hunger.
List of Sources
- Understand the Impact of Dementia on Appetite
- Malnutrition and Dementia: What Clinical Trials Are Revealing (https://researchforyou.co.uk/mac-news/malnutrition-and-dementia-what-clinical-trials-are-revealing)
- Can Dementia Cause Weight Loss? | Sewell, NJ (https://junipercommunities.com/can-dementia-cause-weight-loss)
- ADI - Nutrition and dementia (https://alzint.org/resource/nutrition-and-dementia)
- Meta-analysis and moderator analysis of the prevalence of malnutrition and malnutrition risk among older adults with dementia (https://sciencedirect.com/science/article/abs/pii/S0020748923002134)
- Changes in eating habits and food preference (https://alzheimers.org.uk/get-support/living-with-dementia/changes-eating-habits-food-preference)
- Identify Signs of Appetite Changes in Patients
- The Family Caregiver - Appetite and Dementia (LMTAAA) (https://lmtaaa.org/the-family-caregiver---appetite-and-dementia)
- Appetite Loss in Memory Care: Warning Signs & Solutions (https://irisseniorliving.com/senior-living/tx/dallas/dickason-ave/blog/appetite-loss-in-memory-care-warning-signs-solutions)
- These changes in eating habits can be a warning sign of dementia and Alzheimer’s disease, experts say (https://thestar.com/life/health-wellness/these-changes-in-eating-habits-can-be-a-warning-sign-of-dementia-and-alzheimers-disease/article\_2aa898b8-fe5b-11ee-af7a-ef7e3b5398b5.html)
- Sudden diet change could be 'first symptom' of dementia, doctors warn (https://dailymail.co.uk/health/article-14730665/Sudden-diet-cravings-changes-dementia-symptom-early.html)
- Implement Strategies to Encourage Healthy Eating
- Food for Thought: Nutrition for People Living With Dementia (https://caregiver.org/resource/food-for-thought-nutrition-for-people-living-with-dementia)
- Tips for Caregivers: Helping People With Alzheimer’s Disease Eat Well (https://nia.nih.gov/health/alzheimers-caregiving/tips-caregivers-helping-people-alzheimers-disease-eat-well)
- Fostering the Enjoyment of Eating through Inclusive Strategies for People Living with Dementia | Global Brain Health Institute (https://gbhi.org/news-publications/fostering-enjoyment-eating-through-inclusive-strategies-people-living-dementia)
- Helping caregivers help people with dementia eat at home (https://sciencedaily.com/releases/2024/02/240215113556.htm)
- Create a Supportive Mealtime Environment
- Simple Mealtime Strategies for Dementia Caregivers (https://physioinq.com.au/blog/simple-mealtime-strategies-for-dementia-caregivers)
- Supporting someone with dementia to eat and drink (https://alzheimers.org.uk/get-support/living-with-dementia/improving-eating-experience-dementia)
- Fostering the Enjoyment of Eating through Inclusive Strategies for People Living with Dementia | Global Brain Health Institute (https://gbhi.org/news-publications/fostering-enjoyment-eating-through-inclusive-strategies-people-living-dementia)
- Helping caregivers help people with dementia eat at home (https://sciencedaily.com/releases/2024/02/240215113556.htm)
- Supporting Residents with Dementia Through Therapeutic Hospitality and Culinary Wellness (https://providermagazine.com/Articles/Guest-Columns/Pages/2022/Supporting-Residents-with-Dementia-Through-Therapeutic-Hospitality-and-Culinary-Wellness.aspx)
- Enhance Communication to Address Hunger Needs
- Study offers guidance for communicating with loved ones living with dementia (https://news-medical.net/news/20250827/Study-offers-guidance-for-communicating-with-loved-ones-living-with-dementia.aspx)
- How To Communicate With Dementia Patients (https://trualta.com/resources/blog/how-to-communicate-with-dementia-patients)
- Home for the Holidays: Experts Share Tips for Communicating and Connecting When a Loved One Has Dementia (https://prnewswire.com/news-releases/home-for-the-holidays-experts-share-tips-for-communicating-and-connecting-when-a-loved-one-has-dementia-302617530.html)

