
For families in our service areas
For families in our service areas, this guide explains caregiving and how non-medical in-home caregiving can support care planning in East Idaho, Treasure Valley & Magic Valley, Northern Wasatch, North Central West Virginia, and Northeast Ohio.
The Importance of Implement Palliative Care for Elderly
Palliative care is a crucial yet often overlooked component of healthcare for the elderly. It addresses not only physical ailments but also the emotional and psychological challenges that seniors face. Caregivers, in their quest to improve the quality of life for their loved ones, encounter significant hurdles in providing this type of care.
The implications of neglecting palliative care can be profound. Without proper support, seniors may experience diminished dignity, loss of independence, and a lack of meaningful engagement in their daily lives. Caregivers often find themselves overwhelmed by the complexities of personalized care plans and effective communication, which can lead to frustration and burnout.
So, how can caregivers ensure they meet the unique needs of each elderly individual while providing the best possible support? Implementing palliative care at home can be a transformative solution. Here are some actionable tips:
- Assess individual needs: Regularly evaluate the physical, emotional, and psychological needs of the elderly person in your care.
- Communicate openly: Foster an environment where seniors feel comfortable expressing their needs and preferences.
- Collaborate with professionals: Engage healthcare providers to create a comprehensive care plan tailored to the individual.
- Encourage independence: Support seniors in maintaining their autonomy through activities they enjoy.
By focusing on these strategies, caregivers can navigate the complexities of palliative care, ensuring that their loved ones receive the compassionate support they deserve.
Define Palliative Care and Its Importance for the Elderly
Palliative treatment addresses a significant problem faced by caregivers: the challenge of ensuring quality of life for patients with serious illnesses. Many elderly individuals experience not only physical discomfort but also emotional and psychological distress, which can severely impact their overall well-being.
This lack of comprehensive support can lead to feelings of helplessness and isolation among seniors. Caregivers often struggle to meet these multifaceted needs, which can be overwhelming and stressful.
The solution lies in palliative care for elderly at home, which focuses on relieving symptoms, pain, and stress. By providing thorough assistance, hospice support enables seniors to maintain their dignity and independence. This approach allows them to engage in meaningful activities and cherish precious moments with family and friends.
Incorporating palliative care for elderly at home into caregiving strategies is essential for effectively managing chronic conditions. It enhances overall well-being and ensures that elderly patients can live as fully and comfortably as possible.
Assess Individual Needs and Preferences
To effectively implement palliative support, caregivers face a significant challenge: understanding the unique needs and preferences of elderly individuals. Without a comprehensive assessment, it becomes difficult to provide the tailored support that enhances their quality of life.
This process begins with a detailed evaluation of the individual’s medical history, current health status, and specific symptoms. Engaging in open conversations with the patient is essential. It helps caregivers grasp their wishes regarding treatment options, daily routines, and personal goals. Additionally, emotional and social needs, along with cultural or spiritual beliefs, must be considered, as these factors greatly impact the support provided.
Recording these insights creates a comprehensive profile that serves as the foundation for a tailored support strategy. This patient-centered approach to palliative care for elderly at home not only aligns with the preferences of older adults but also significantly enhances their overall quality of life. A recent survey revealed that 84% of older adults expressed interest in obtaining supportive treatment if faced with a serious illness, highlighting the importance of personalized support plans.
Furthermore, Dr. Adam Marks emphasizes the necessity for a deeper understanding of supportive treatment, clarifying that it is a standard component of care for serious illnesses. By integrating these insights, caregivers can ensure that the assistance provided is both effective and respectful of each individual’s unique circumstances.
Develop a Personalized Palliative Care Plan
Identifying individual needs in palliative care is crucial, yet many caregivers face challenges in addressing these effectively. Without a tailored approach, patients may experience unmanaged symptoms and emotional distress, impacting their quality of life.
To tackle this issue, caregivers should develop a personalized palliative strategy. This plan must outline specific objectives for care, including:
- Symptom management strategies
- Medication schedules
- Necessary interventions
Engaging a multidisciplinary team comprising healthcare providers, social workers, and family members ensures a holistic approach. This collaboration not only addresses medical needs but also incorporates emotional and spiritual support, providing resources for family caregivers.
Regular reviews and adjustments to the strategy are essential. As the patient's condition or preferences change, the care plan should evolve accordingly, ensuring that it remains relevant and effective.
Implement the Care Plan and Monitor Progress
With the strategy established, caregivers face a significant challenge: ensuring effective coordination among all involved. This is crucial for understanding roles and responsibilities, which directly impacts patient care. The implications of poor communication can lead to misunderstandings and inadequate support for the patient.
To address this issue, caregivers should consistently observe the patient's condition and the effectiveness of treatment interventions. Keeping detailed records of symptoms, medication effects, and any changes in the patient's emotional state is essential. Frequent check-ins with healthcare providers can facilitate discussions about progress and necessary adjustments to the treatment plan.
Encouraging open communication among family members and caregivers is vital to address any concerns or challenges that arise during implementation. It's important to note that all healthcare providers should possess the knowledge and abilities to deliver fundamental elements of supportive treatment. In fact, as highlighted by specialists in the field, fewer than 20,000 healthcare providers in the U.S. hold certifications or advanced qualifications in hospice and comfort management, underscoring the demand for skilled caregivers in these environments.
Dr. Kurt Merkelz emphasizes that a thorough, interdisciplinary strategy for end-of-life support is crucial for successful execution. To enhance caregiver effectiveness, employing tools like symptom tracking applications or coordination platforms can assist in monitoring progress and ensuring that the patient's needs are met efficiently.
Communicate with Family and Seek Support Resources
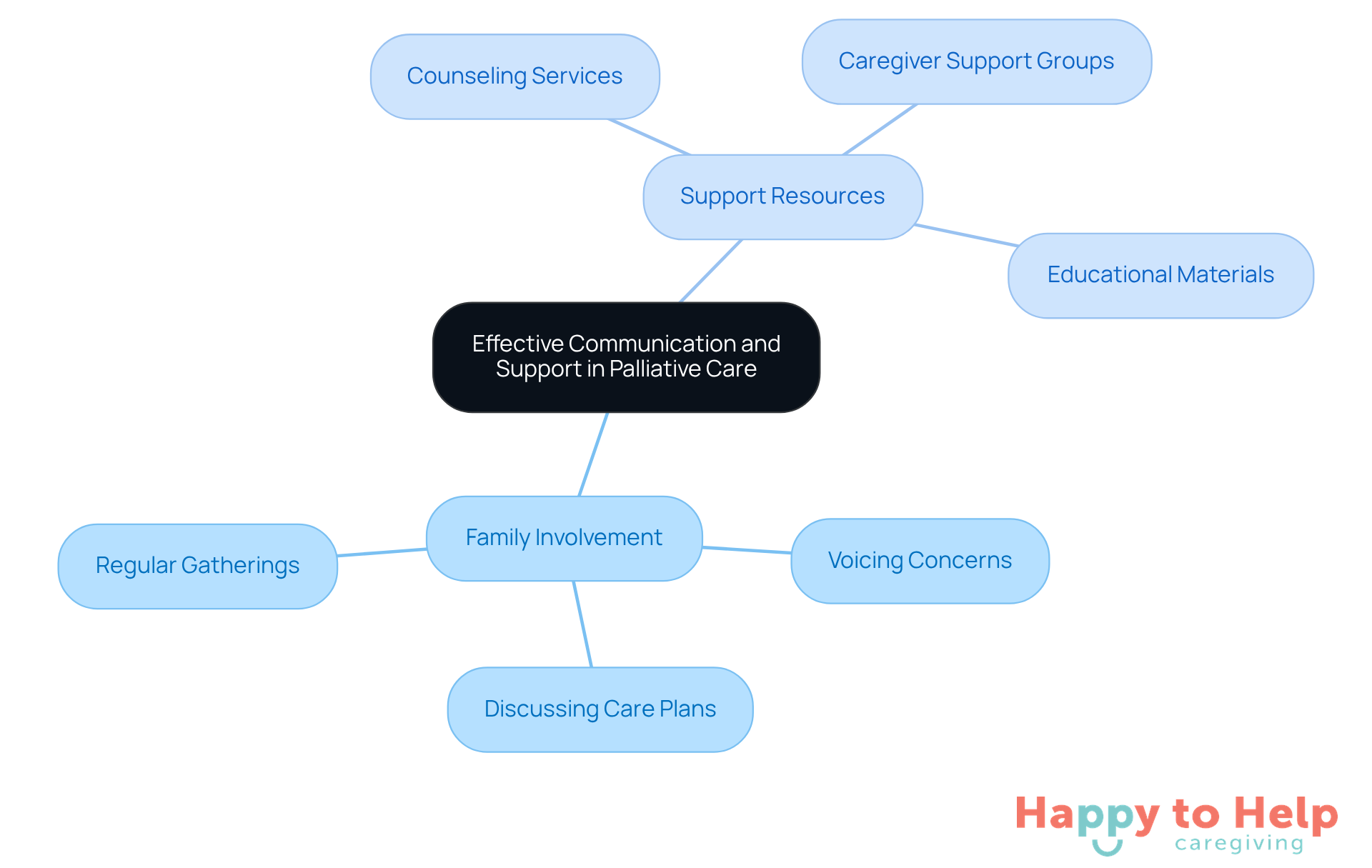
Effective communication is crucial in palliative care for elderly at home, particularly when involving relatives in the treatment process. The challenge arises when families feel disconnected from the care plan, leading to increased stress and uncertainty. Regular gatherings can address this issue by providing a platform to discuss the patient's condition, care plan, and necessary adjustments. This approach not only encourages relatives to voice their feelings and concerns but also fosters a supportive environment that enhances the caregiving experience.
To tackle the emotional strain, families should actively seek out support resources tailored to their needs. Counseling services, caregiver support groups, and educational materials serve as invaluable tools in navigating the complexities of caregiving. Research indicates that families utilizing these resources experience lower stress levels and greater satisfaction with the care provided. For example, 58.8% of grieving relatives reported receiving adequate help and support during their loved one's illness, highlighting the positive impact of accessible support systems.
By prioritizing communication and leveraging available support resources, such as caregiver support groups and educational materials, families can cultivate a more effective and compassionate care environment for elderly individuals through palliative care for elderly at home.
Key Takeaways for Caregivers
Implementing palliative care for the elderly at home presents a significant challenge for caregivers. Many face the daunting task of ensuring that seniors receive not only medical attention but also emotional support during difficult times. Without proper care, elderly individuals may experience increased discomfort and feelings of isolation, which can diminish their quality of life.
To address these issues, caregivers can focus on creating an environment that prioritizes dignity and independence for seniors. By emphasizing symptom relief and fostering meaningful connections with family and friends, caregivers can help elderly individuals cherish their remaining moments. This compassionate approach not only alleviates physical discomfort but also uplifts their spirits.
Key strategies for effective implementation include:
- Assessing individual needs
- Developing personalized care plans
- Maintaining open lines of communication with both patients and their families
Understanding the unique circumstances of each elderly person allows caregivers to tailor their support effectively. This leads to improved satisfaction and reduced feelings of isolation. Regular monitoring and collaboration with healthcare professionals ensure that care plans remain relevant and effective as conditions evolve.
Ultimately, the importance of palliative care for the elderly cannot be overstated. It represents a compassionate response to the complexities of aging and serious illness. By embracing these practices, caregivers can cultivate a nurturing atmosphere that addresses medical needs while uplifting the spirit of the elderly, making a profound difference in their lives.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5MjdhNWU2MjUyZjAyYmU4ZDQ3YzY4OSIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What is palliative care and why is it important for the elderly?
Palliative care addresses the challenge of ensuring quality of life for elderly patients with serious illnesses by relieving symptoms, pain, and stress. It is important because it helps seniors maintain their dignity and independence while managing physical discomfort and emotional distress.
How does palliative care benefit elderly individuals at home?
Palliative care for the elderly at home enhances overall well-being by providing thorough support that allows seniors to engage in meaningful activities and cherish moments with family and friends, ultimately helping them live as fully and comfortably as possible.
What challenges do caregivers face when implementing palliative care for the elderly?
Caregivers face the challenge of understanding the unique needs and preferences of elderly individuals. Without a comprehensive assessment of their medical history, health status, and personal goals, it becomes difficult to provide tailored support that enhances quality of life.
What steps are involved in assessing the needs of elderly individuals for palliative care?
The assessment process involves a detailed evaluation of the individual’s medical history, current health status, and specific symptoms. Caregivers should engage in open conversations with the patient to understand their treatment preferences, daily routines, and emotional, social, cultural, or spiritual needs.
Why is a patient-centered approach important in palliative care?
A patient-centered approach is important because it aligns care with the preferences of older adults, significantly enhancing their overall quality of life. It ensures that the support provided is effective and respectful of each individual's unique circumstances.
What does recent research indicate about the interest of older adults in supportive treatment?
A recent survey revealed that 84% of older adults expressed interest in obtaining supportive treatment if faced with a serious illness, highlighting the importance of personalized support plans in palliative care.
List of Sources
- Define Palliative Care and Its Importance for the Elderly
- Support for Serious Illness (https://newsinhealth.nih.gov/2025/07/support-serious-illness)
- Study: Few With Advanced Cancer Receive Palliative Care (https://breastcancer.org/news/study-palliative-care-underused-end-of-life)
- Many older adults receiving home care do not receive palliative care before death (https://hospitalnews.com/many-older-adults-receiving-home-care-do-not-receive-palliative-care-before-death)
- Can palliative care consults in hospitals improve end-of-life care? (https://nia.nih.gov/news/can-palliative-care-consults-hospitals-improve-end-life-care)
- Assess Individual Needs and Preferences
- Older adults receiving home care are missing out on palliative care: study (https://mcknights.com/news/older-adults-receiving-home-care-are-missing-out-on-palliative-care-study)
- Nursing homes ‘can’t escape’ need for increased palliative care access: researchers (https://mcknights.com/news/nursing-homes-cant-escape-need-for-increased-palliative-care-access-researchers)
- Palliative care and hospice poll reveals major gaps (https://ihpi.umich.edu/news-events/news/palliative-care-and-hospice-poll-reveals-major-gaps)
- As elderly population swells, some doctors see benefits of palliative care in the ER (https://pbs.org/newshour/health/elderly-population-swells-doctors-see-benefits-palliative-care-er)
- Bringing Palliative Care to Nursing Homes (https://hospicenews.com/2025/06/23/bringing-palliative-care-to-nursing-homes)
- Develop a Personalized Palliative Care Plan
- Creating a Care Plan to Support Your Goals (https://getpalliativecare.org/creating-a-care-plan-to-support-your-goals)
- Personalised palliative care for older adults with cancer (https://ucd.ie/medicine/news/2025/personalisedpalliativecareforolderadultswithcancer)
- Carelon Health Executive: A ‘Quadruple Aim’ to Palliative Care Sustainability (https://hospicenews.com/2025/09/22/carelon-health-executive-a-quadruple-aim-to-palliative-care-sustainability)
- Palliative Care Program Supports Patients and Families (https://elcaminohealth.org/newsroom/palliative-care-program-supports-patients-and-families)
- Implement the Care Plan and Monitor Progress
- ‘Rehabbed to Death’: Bringing More Palliative, Hospice Care to SNFs (https://hospicenews.com/2025/11/26/rehabbed-to-death-bringing-more-palliative-hospice-care-to-snfs)
- Home-based palliative care has grown in popularity, but expertise lags, report finds (https://mcknightshomecare.com/news/home-based-palliative-care-has-grown-in-popularity-but-expertise-lags-report-finds)
- Palliative Care and Hospice: How Can We Overcome Barriers to Their Use? (https://chausa.org/news-and-publications/publications/health-progress/archives/fall-2023/palliative-care-and-hospice-how-can-we-overcome-barriers-to-their-use)
- The Pitfalls That Derail Home Health Providers’ New Palliative Care Efforts (https://homehealthcarenews.com/2025/10/the-pitfalls-that-derail-home-health-providers-new-palliative-care-efforts)
- Communicate with Family and Seek Support Resources
- ‘Let’s Talk’: How to Help Families Have Difficult Conversations (https://yalemedicine.org/news/palliative-care)
- Communication in Palliative Care (https://news.cuanschutz.edu/graduate-school/communication-in-palliative-care)
- Palliative Care News | Living with Serious Illness | Get Palliative Care (https://getpalliativecare.org/news)
- Support received by family members before, at and after an ill person’s death - BMC Palliative Care (https://bmcpalliatcare.biomedcentral.com/articles/10.1186/s12904-021-00800-8)
- Caregiver Statistics: Demographics (https://caregiver.org/resource/caregiver-statistics-demographics)