
Understanding Effective Strategies for Alzheimer
Addressing the eating challenges faced by individuals with Alzheimer's disease is a pressing concern for caregivers. Refusal to eat can lead to serious health risks, making it crucial to understand the underlying causes. These causes can range from cognitive decline to emotional distress, and recognizing them can empower caregivers to implement effective strategies that encourage better eating habits.
However, the complexity of these issues raises an important question: how can caregivers create a supportive environment that fosters appetite and enhances the overall mealtime experience? By focusing on practical solutions, caregivers can significantly improve the eating habits of those affected. This article will explore actionable strategies that caregivers can adopt to create a more positive and engaging mealtime atmosphere.
Identify Causes of Eating Refusal in Alzheimer's Patients
The challenge of eating refusal in individuals is often referred to as Alzheimer's disease not eating, which presents a significant challenge for caregivers. This issue often stems from a complex interplay of cognitive decline, sensory changes, and emotional factors. As cognitive abilities deteriorate, individuals with Alzheimer's disease not eating may become confused about food and the act of eating, leading to refusal. Additionally, sensory alterations, particularly reduced taste and smell, can make food less appealing, complicating dining experiences further.
Emotional factors, such as depression and anxiety, can significantly diminish appetite, which is a concern for those facing Alzheimer's disease not eating. This makes it crucial for caregivers to remain vigilant and attentive to the individual's needs. By closely observing behavior and preferences, caregivers can identify patterns that may trigger eating refusal, especially in cases of Alzheimer's disease not eating. For instance, if an individual exhibits restlessness during meals, it may be beneficial to evaluate the eating environment or the types of food being offered.
Understanding these underlying causes allows caregivers to effectively tailor their approaches to the challenges posed by Alzheimer's disease not eating. Here are some actionable tips to foster a more positive mealtime experience:
- Evaluate the environment: Ensure the dining area is calm and free from distractions.
- Adapt food choices: Offer foods that are visually appealing and aromatic to stimulate appetite.
- Monitor behavior: Keep track of any signs of discomfort or disinterest during meals.
By implementing these strategies, caregivers can create a more supportive and enjoyable dining experience for individuals with Alzheimer's.
Implement Strategies to Encourage Eating
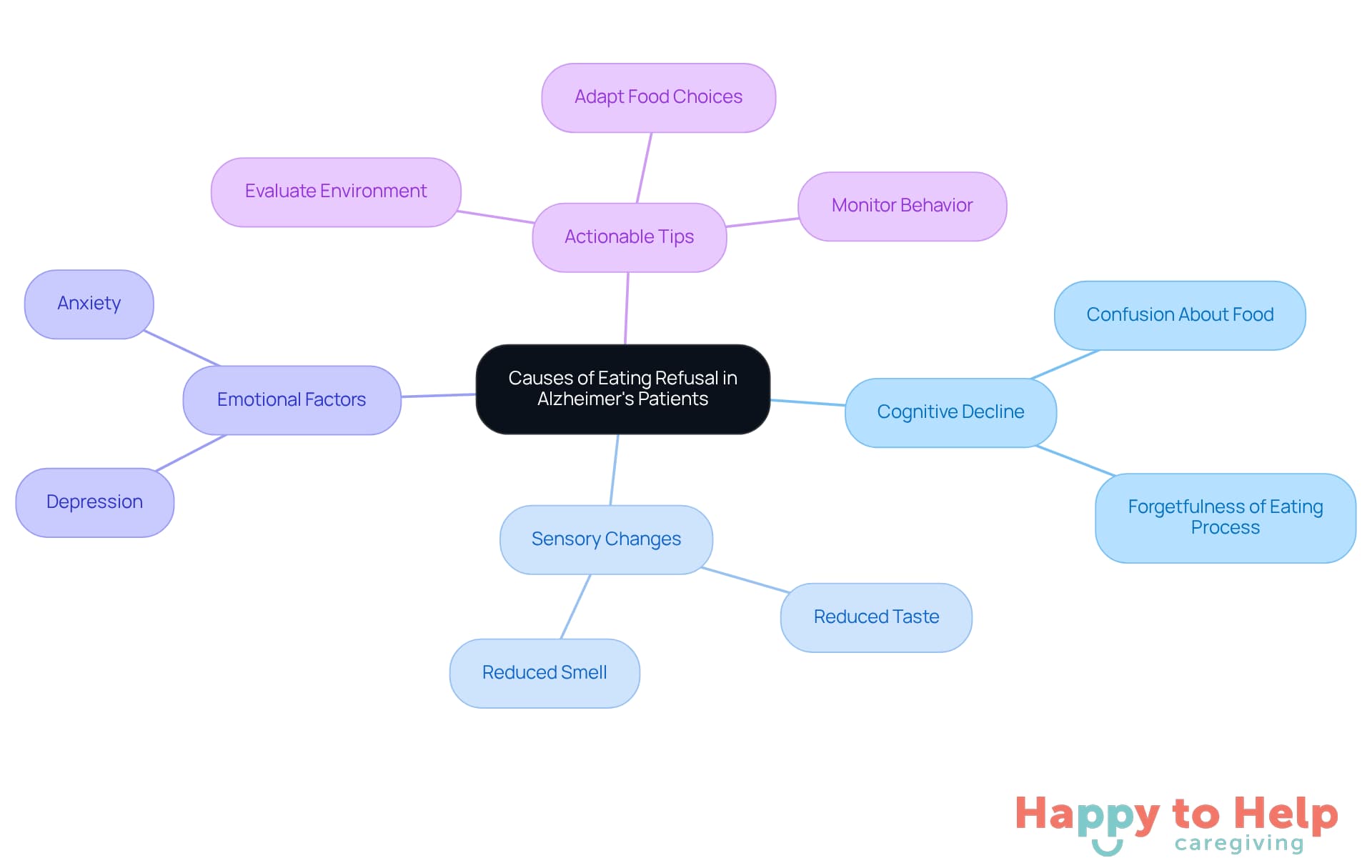
Alzheimer's disease not eating can lead to significant challenges for caregivers due to the eating difficulties among patients. These challenges associated with Alzheimer's disease not eating not only affect the patient's nutritional intake but can also lead to frustration and stress during mealtimes. To address these issues, caregivers can implement several effective strategies:
- Provide Smaller, Frequent Portions: Instead of three large servings, offer smaller, more frequent portions to reduce overwhelm and enhance intake.
- Enhance Food Appeal: Use colorful plates and visually appealing presentations to stimulate interest. Incorporate favorite foods and flavors to make meals more enticing.
- Limit Distractions: Create a calm dining atmosphere by minimizing noise and distractions, which can help the patient concentrate on eating.
- Incorporate Familiar Routines: Establish consistent dining routines to provide a sense of security and predictability.
- Engage in Social Eating: Encourage family members to join meals, as social interaction can enhance appetite and enjoyment.
By implementing these strategies, caregivers can address the challenges of Alzheimer's disease not eating and create a more positive and effective eating experience for patients.
Create a Supportive Mealtime Environment
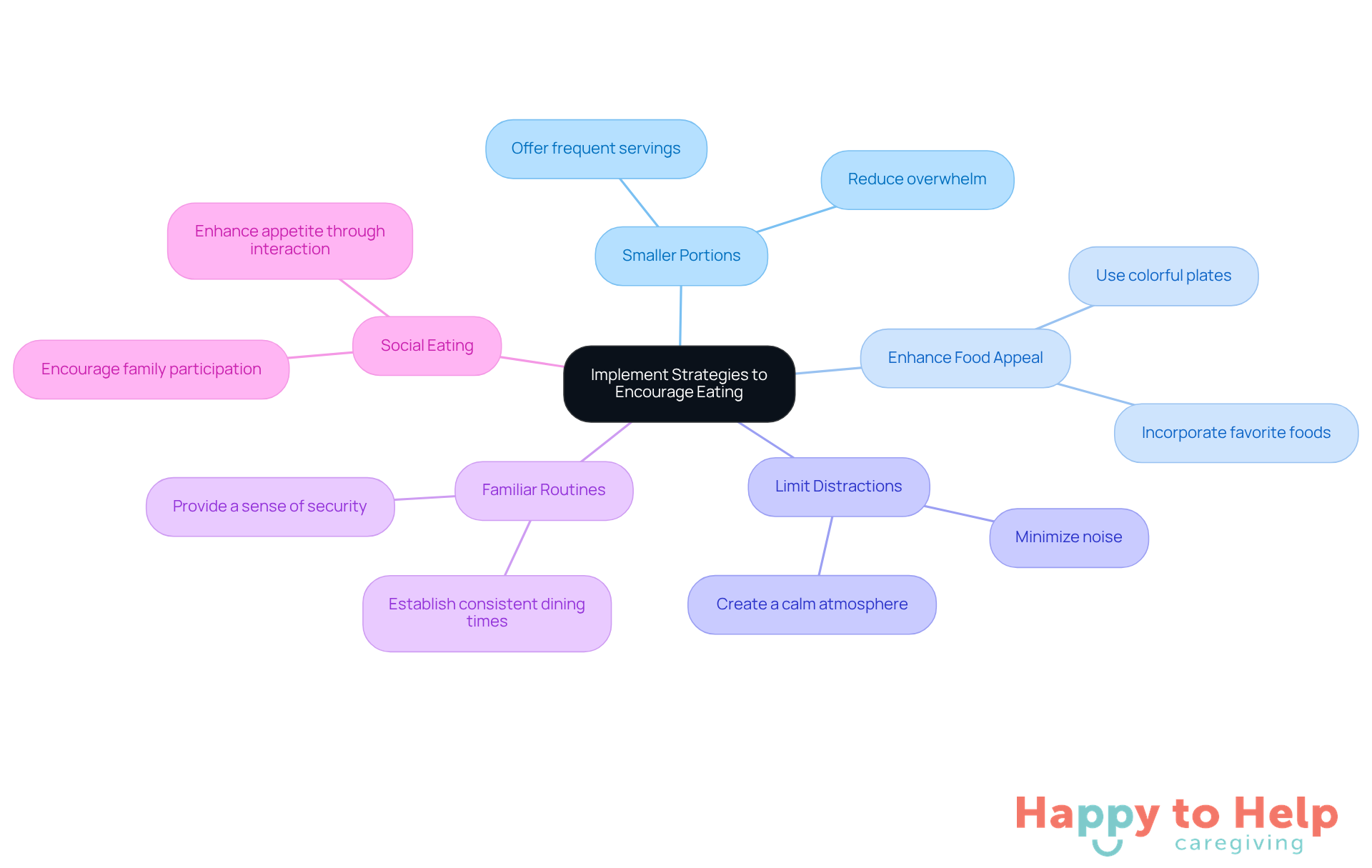
Creating a supportive mealtime environment is crucial for addressing the issue of Alzheimer's disease not eating and enhancing the overall eating experience of individuals. Caregivers often face challenges in ensuring that mealtimes are both enjoyable and nutritious. Here are some key elements to consider:
-
Comfortable Seating: Providing seating that is both comfortable and accessible is essential. This allows patients to eat without physical strain, promoting a more enjoyable dining experience. Occupational therapists stress that appropriate seating can greatly influence the capacity of elderly individuals to participate in dining activities effectively. As one occupational therapist observed, "Comfortable seating is essential for allowing seniors to concentrate on their food instead of their discomfort."
-
Appropriate Lighting: Utilizing soft, natural lighting helps create a warm and inviting atmosphere, which can alleviate anxiety during mealtime. Studies show that ideal lighting conditions not only boost mood but also enhance cognitive function, facilitating concentration during dining.
-
Simple Table Settings: Keeping table settings uncomplicated is vital to prevent overwhelming the patient. Utilizing contrasting colors for dishes and food can enhance visibility, facilitating recognition for individuals with dementia and motivating them to eat. Additionally, using simple table settings can reduce confusion, allowing for a more relaxed dining experience.
-
Engaging Activities: Incorporating gentle conversation or soothing music during dining can foster a pleasant ambiance. Involving individuals in light conversations or playing soothing music can improve their overall dining experience, making mealtimes more enjoyable. Caregivers should also provide gentle cues or demonstrations to help individuals, particularly those facing challenges like Alzheimer's disease not eating, ensuring that they feel supported during dining.
-
Encourage Independence: Allowing individuals to take part in food preparation or serving can promote a sense of control and involvement. This involvement not only promotes dignity but also encourages a positive attitude towards eating, which is essential for maintaining nutrition. Caregivers should be understanding and allow ample time for the person to complete their meal without rushing.
By concentrating on these aspects, caregivers can establish a supportive mealtime atmosphere that addresses the nutritional requirements and emotional wellness of individuals with dementia.
Recognize When to Seek Professional Assistance
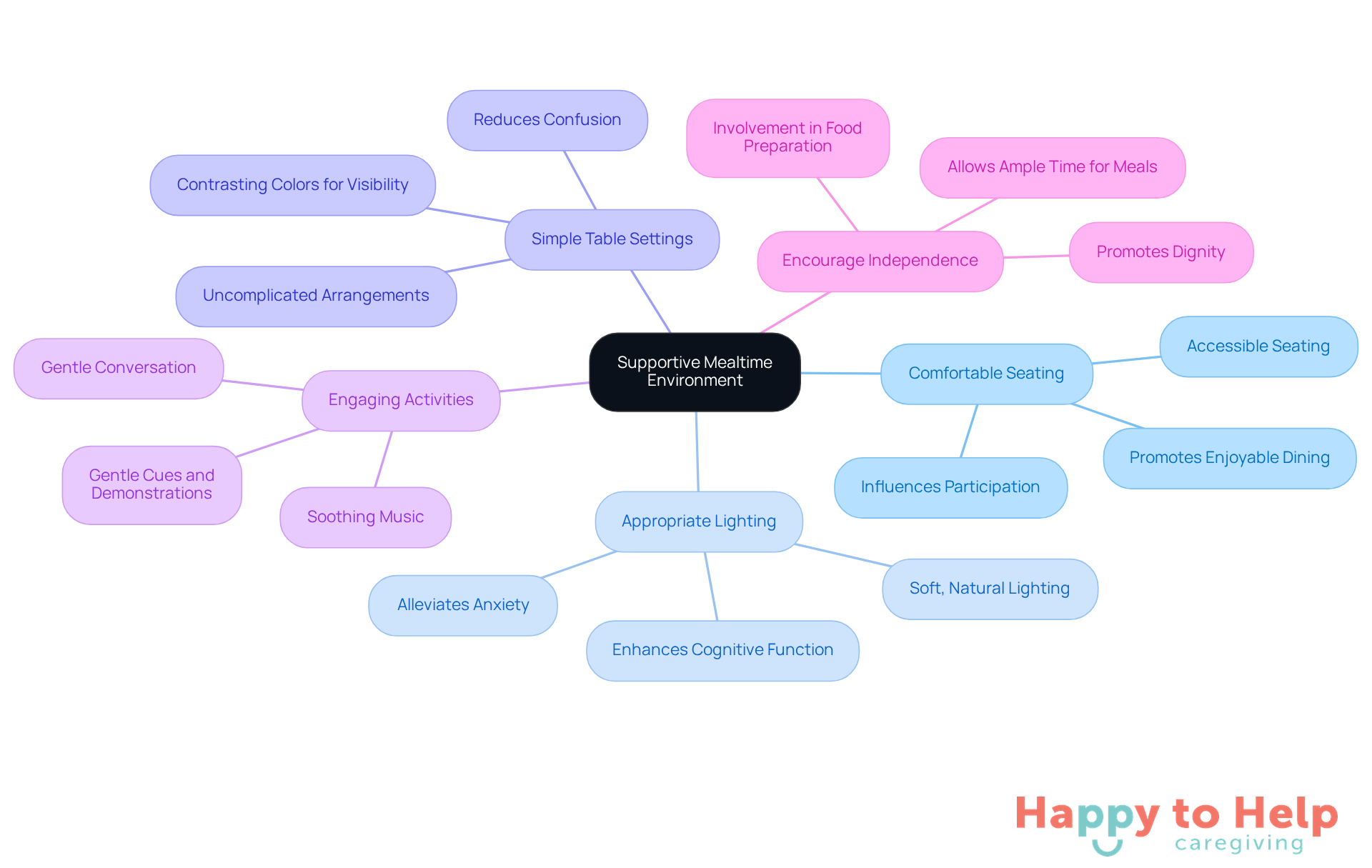
Caregivers face significant challenges when it comes to managing the eating difficulties associated with Alzheimer's disease not eating in individuals with dementia. Recognizing the signs that suggest the need for professional help is crucial. Here are some key indicators to watch for:
-
Significant Weight Loss: A notable decrease of 5% or more of initial body weight within a year is common among individuals with severe dementia. In fact, 93.8% of those with advanced Alzheimer's disease not eating are underweight. This can signal serious health concerns that necessitate medical evaluation.
-
If an individual consistently refuses meals or shows a marked lack of interest in food, it may indicate underlying issues such as Alzheimer's disease not eating. Consulting with a healthcare provider is warranted in these cases.
-
Physical Symptoms: Signs of dehydration, such as a dry mouth or reduced urine output, require immediate attention. These symptoms can lead to further complications if not addressed promptly.
-
Difficulty Swallowing: Symptoms of dysphagia affect up to 91.8% of individuals with severe cognitive impairment and 45.7% of all participants. Expert evaluation is essential to avoid choking and ensure safe eating habits.
-
Behavioral Changes: Sudden shifts in behavior during mealtimes, including increased agitation or confusion, may reflect underlying health problems that need to be addressed.
Recognizing these signs early can significantly impact the nutritional status and overall well-being of individuals not eating due to Alzheimer's disease. Caregivers should remain vigilant and proactive in seeking help when these indicators arise.
Moving Forward with Effective Strategies for Alzheimer
Addressing the issue of eating refusal in individuals with Alzheimer's disease presents a significant challenge for caregivers. This problem is multifaceted, stemming from cognitive decline and emotional factors that complicate mealtime experiences. The implications are profound, as inadequate nutrition can lead to further health complications and diminished quality of life.
To tackle this issue effectively, caregivers can implement several practical strategies:
- Creating a supportive environment is crucial; this includes enhancing the appeal of food and fostering a positive dining atmosphere.
- Offering smaller portions can make meals less overwhelming.
- Engaging in social eating can encourage participation and enjoyment.
- Caregivers should remain vigilant in recognizing when professional assistance is necessary, as early intervention can prevent complications and support the well-being of patients.
Ultimately, addressing eating issues in Alzheimer's patients is not just about nutrition; it significantly impacts emotional health and overall quality of life. By being proactive and attentive, caregivers can transform mealtime into a nurturing experience that supports both the body and spirit.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5M2Y1MDgwMTQ3ZTIwZjE1ODJjOWRkNyIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What is the main issue discussed in the article regarding Alzheimer's patients?
The article discusses the challenge of eating refusal in individuals with Alzheimer's disease, which can be a significant concern for caregivers.
What are the primary causes of eating refusal in Alzheimer's patients?
Eating refusal in Alzheimer's patients often results from cognitive decline, sensory changes, and emotional factors, such as confusion about food, reduced taste and smell, depression, and anxiety.
How does cognitive decline affect eating habits in Alzheimer's patients?
As cognitive abilities deteriorate, individuals may become confused about food and the act of eating, leading to refusal to eat.
What sensory changes can impact eating in Alzheimer's patients?
Sensory alterations, particularly reduced taste and smell, can make food less appealing and complicate the dining experience for individuals with Alzheimer's.
How do emotional factors influence appetite in Alzheimer's patients?
Emotional factors such as depression and anxiety can significantly diminish appetite, making it difficult for individuals with Alzheimer's to eat.
What should caregivers do to address eating refusal in Alzheimer's patients?
Caregivers should remain vigilant, observe behavior and preferences, and identify patterns that may trigger eating refusal.
What specific signs should caregivers monitor during mealtime?
Caregivers should monitor for signs of discomfort or disinterest, such as restlessness during meals.
What strategies can caregivers implement to improve mealtime experiences for Alzheimer's patients?
Caregivers can evaluate the dining environment, adapt food choices to be more visually appealing and aromatic, and monitor behavior during meals to create a supportive dining experience.
List of Sources
- Identify Causes of Eating Refusal in Alzheimer's Patients
- 80 Quotes About Loving Someone With Alzheimer's (https://parade.com/1178790/kaitlin-vogel/alzheimers-quotes)
- Caregiver Experiences with Dementia-Related Feeding/Eating Difficulties | MDPI (https://mdpi.com/2227-9032/12/2/133)
- When People With Alzheimer’s Stop Eating (https://beingpatient.com/why-do-alzheimers-patients-stop-eating)
- (https://belleviecare.co.uk/support-advice/dementia-quotes-to-lift-your-spirits)
- Create a Supportive Mealtime Environment
- Helping caregivers help people with dementia eat at home (https://news.osu.edu/helping-caregivers-help-people-with-dementia-eat-at-home)
- Simple Mealtime Strategies for Dementia Caregivers (https://physioinq.com.au/blog/simple-mealtime-strategies-for-dementia-caregivers)
- Better lighting can boost sleep, mood in dementia patients | ASU News (https://news.asu.edu/20250909-health-and-medicine-better-lighting-can-boost-sleep-mood-dementia-patients)
- Tips for Caregivers: Helping People With Alzheimer’s Disease Eat Well (https://nia.nih.gov/health/alzheimers-caregiving/tips-caregivers-helping-people-alzheimers-disease-eat-well)
- Supporting someone with dementia to eat and drink (https://alzheimers.org.uk/get-support/living-with-dementia/improving-eating-experience-dementia)
- Recognize When to Seek Professional Assistance
- Patient Information: Eating and Swallowing Problems in People With Advanced Dementia (https://jamanetwork.com/journals/jama/fullarticle/2835480)
- What Should You Do If Alzheimer's Patients Are Not Eating? - NCCDP (https://nccdp.org/what-should-you-do-if-alzheimers-patients-are-not-eating)
- Signs for Early Detection of Dysphagia in Older Adults with Severe Alzheimer's Disease (https://sciencedirect.com/science/article/pii/S1279770723012897)
- Weight loss in Alzheimer disease (https://sciencedirect.com/science/article/pii/S000291652307034X)
- Chewing and Swallowing Problems Related to Alzheimer’s Disease (https://webmd.com/alzheimers/chewing-swallowing-problems)

