
What You Need to Know About Essential Strategies
Understanding the complexities of incontinence care presents a significant challenge for caregivers. This issue is not just about managing physical symptoms; it also impacts the emotional well-being of those they support. Caregivers often find themselves navigating various types of urinary leakage, each with its own set of difficulties. This can lead to feelings of frustration and overwhelm, making it essential to address both the physical and emotional aspects of care.
So, how can caregivers effectively manage these demands while also prioritizing their own self-care? The solution lies in implementing tailored strategies that address the unique needs of each individual. By focusing on practical approaches, caregivers can enhance the quality of life for those they support while also safeguarding their own emotional health.
Consider these actionable tips:
- Educate Yourself: Understanding the different types of incontinence can help you tailor your approach.
- Create a Support Network: Connecting with other caregivers can provide emotional support and practical advice.
- Prioritize Self-Care: Make time for your own well-being to prevent burnout.
By addressing these challenges head-on, caregivers can find a balance that promotes both effective incontinence management and personal well-being.
Understand the Types and Causes of Incontinence
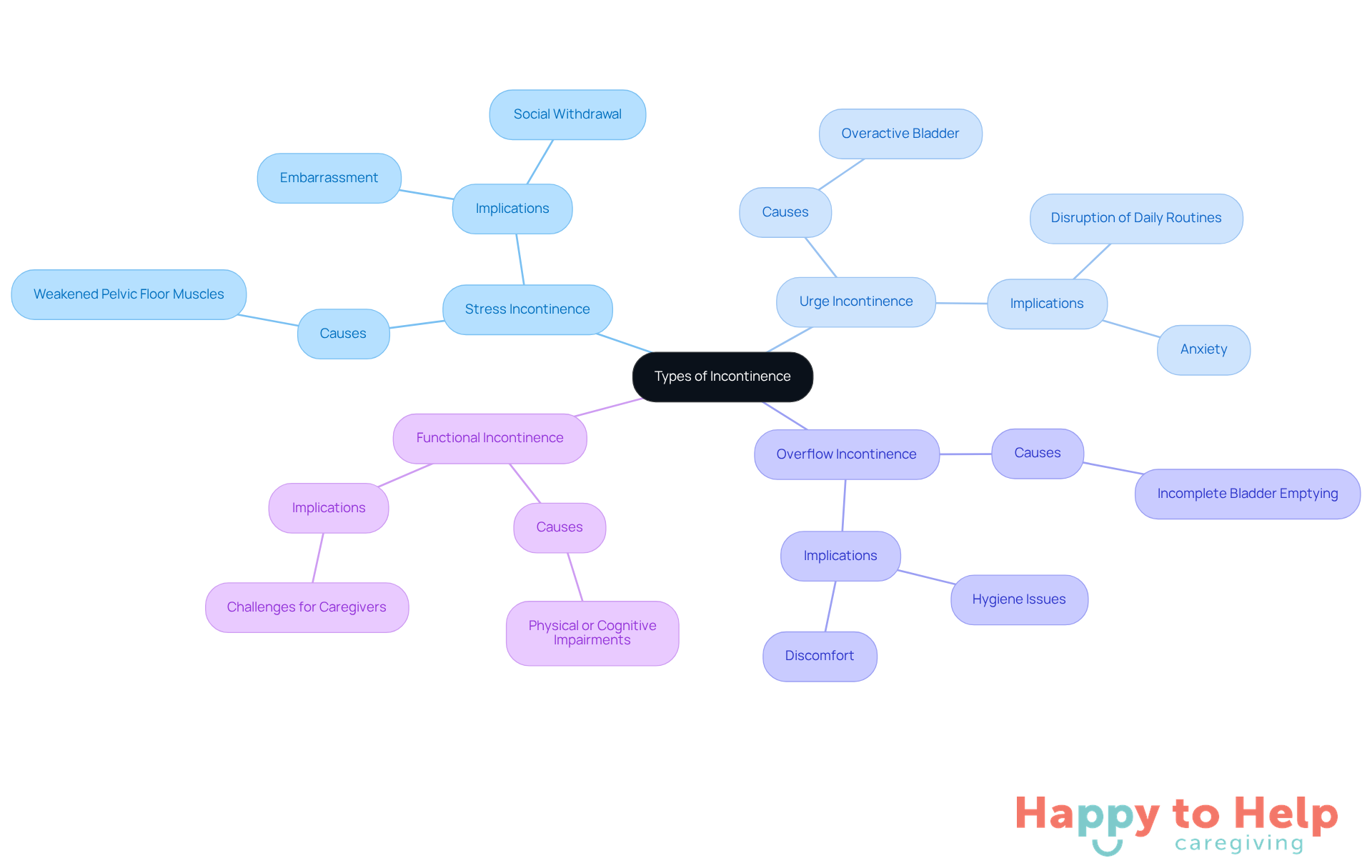
Urinary leakage presents a significant challenge for caregivers, manifesting in various forms: stress urinary leakage, urge urinary leakage, overflow urinary leakage, and functional urinary leakage. Understanding these types is crucial for effective care.
-
Stress Incontinence occurs when leakage happens during physical activities like coughing, sneezing, or exercising, primarily due to weakened pelvic floor muscles. This can lead to embarrassment and social withdrawal for those affected.
-
Urge Incontinence involves a sudden, intense urge to urinate that results in involuntary leakage. This condition is often linked to an overactive bladder, which can disrupt daily routines and lead to anxiety.
-
Overflow Incontinence arises when the bladder fails to empty completely, causing frequent or constant dribbling of urine. This can create hygiene issues and discomfort.
-
Functional Incontinence is characterized by physical or cognitive impairments that hinder timely access to the bathroom, despite normal bladder function. This can be particularly challenging for caregivers trying to assist individuals with mobility or cognitive issues.
For effective caregiver incontinence care, recognizing the type of urinary leakage is essential. It enables them to develop tailored strategies and interventions for caregiver incontinence care that meet the specific needs of the individual. By understanding these conditions, caregivers can enhance their caregiver incontinence care and improve the quality of life for those they care for.
Implement Effective Incontinence Management Techniques
Problem: Incontinence Management Challenges
Caregivers face significant challenges when managing incontinence, impacting both the individuals they care for and their own well-being. Accidents can lead to embarrassment and a loss of dignity, affecting self-esteem and quality of life.
Agitate: The Implications of Poor Management
Without effective strategies, individuals may struggle with bladder control, leading to increased anxiety and dependence on caregivers. This situation can create a cycle of frustration and helplessness, making caregiver incontinence care essential for caregivers to adopt effective management techniques.
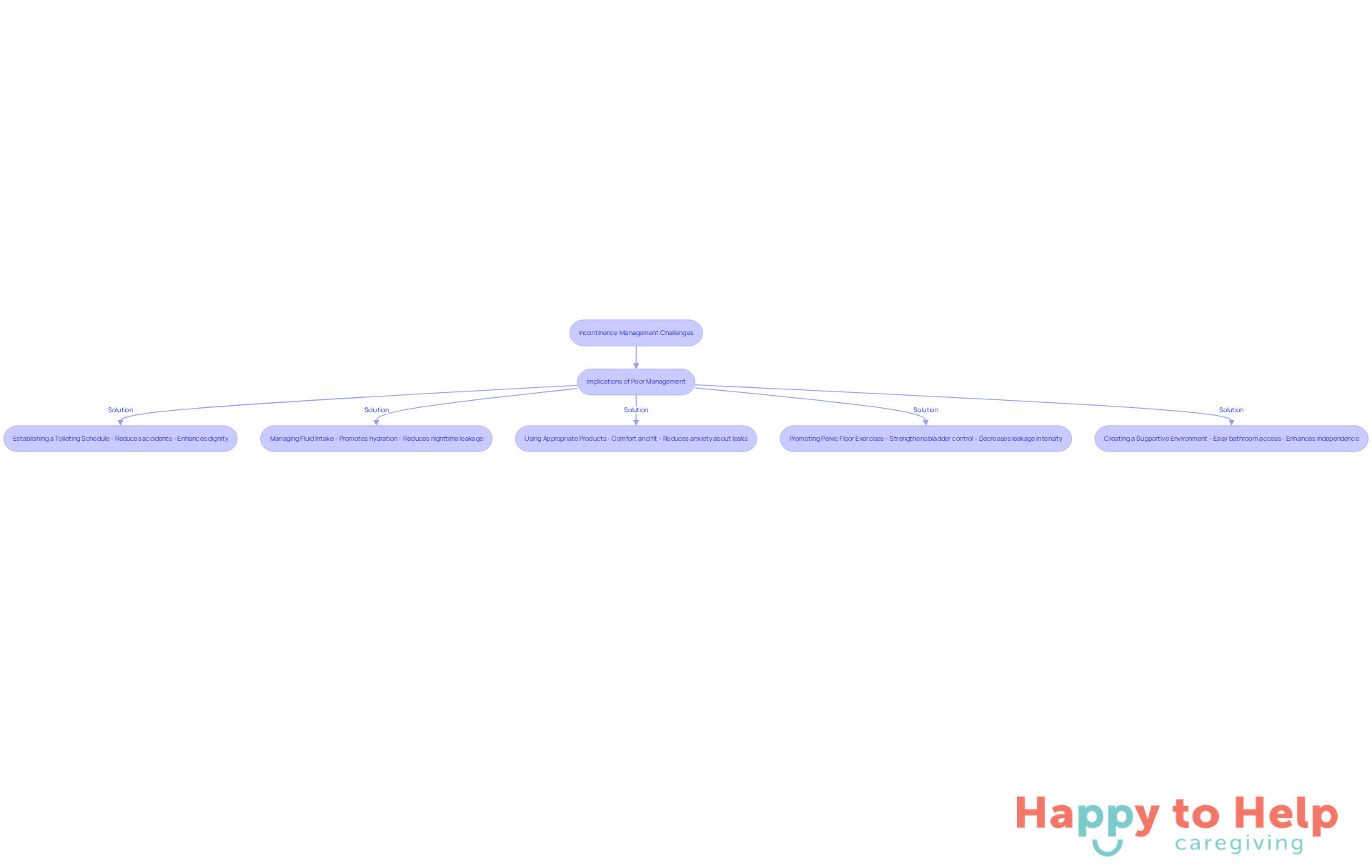
Solution: Effective Management Techniques
-
Establishing a Toileting Schedule: Implementing regular bathroom visits significantly reduces accidents and fosters a reliable routine. Caregivers have noted that structured toileting programs enhance dignity and improve residents' confidence in the context of caregiver incontinence care. A case study highlighted that residents following a customized voiding schedule experienced better control over bladder issues, leading to a more dignified living experience. Ronald Krinn, a Director of Clinical Business Development, states, "Scheduled toileting provides a chance to reinforce good hygiene practices or apply any barriers or moisturizers to improve skin integrity."
-
Managing Fluid Intake: Encouraging adequate hydration while monitoring fluid intake is crucial. In caregiver incontinence care, caregivers should promote hydration during the day but suggest reducing excessive intake before bedtime to alleviate nighttime leakage. This balance sustains overall health while addressing bladder control problems. Notably, studies show that 79% of participants experienced a reduction in bladder leaks by 50% or more when following structured toileting and fluid management strategies.
-
Using Appropriate Products: Choosing high-quality products for bladder control, such as pads or adult diapers, is essential. Products that fit well and provide comfort can significantly enhance the user's experience, reducing anxiety about leaks and promoting independence.
-
Promoting Pelvic Floor Exercises: Encouraging pelvic floor exercises, such as Kegels, can strengthen the muscles involved in bladder control. Caregivers frequently indicate that clients who participate in these exercises experience a decrease in the intensity of leakage, showcasing the effectiveness of caregiver incontinence care in enhancing quality of life.
-
Creating a Supportive Environment: Ensuring easy access to bathrooms is vital. To enhance safety and independence, caregiver incontinence care should include removing obstacles and considering the installation of grab bars. A nurturing atmosphere enables individuals to handle their condition more efficiently, promoting a sense of independence.
By integrating these strategies, caregiver incontinence care can significantly enhance the quality of life for individuals facing bladder control issues, making daily routines more manageable and dignified.
Foster Open Communication with Healthcare Providers
For caregivers, managing bladder control issues while providing caregiver incontinence care can be challenging, making effective communication with healthcare providers essential. Without clear communication, important details may be overlooked, leading to inadequate care and support.
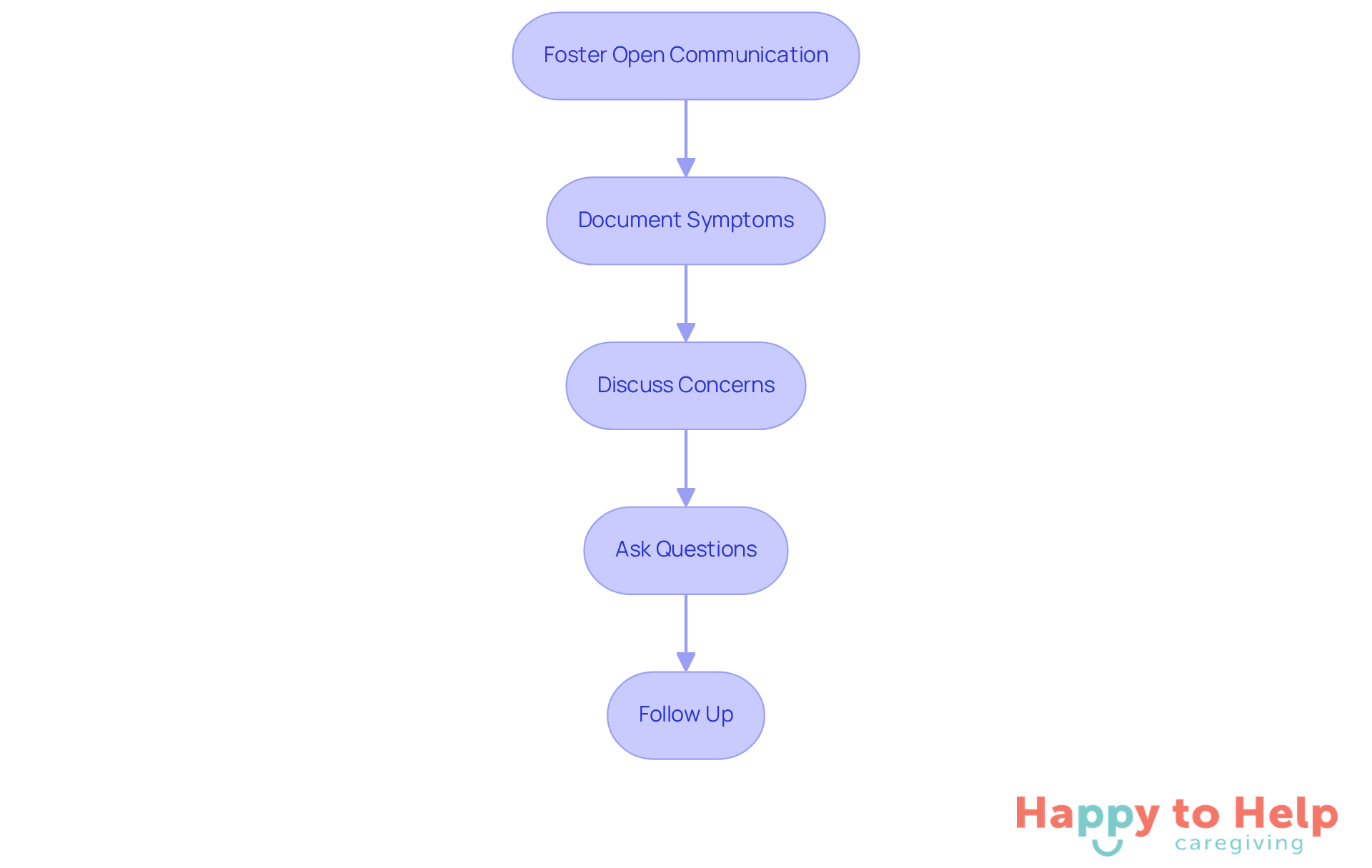
To tackle this problem, caregivers should take several actionable steps:
- Document Symptoms: Keep a detailed record of incontinence episodes, noting frequency, triggers, and any changes in behavior or health. This information is crucial for healthcare providers to understand the situation better.
- Discuss Concerns: Raise any issues related to the person's urinary difficulties during medical appointments. Ensure that all pertinent information is communicated to facilitate informed decision-making.
- Ask Questions: Inquire about treatment options, potential side effects of medications, and any recommended lifestyle changes that could improve the situation. This proactive approach can lead to better outcomes.
- Follow Up: Schedule regular follow-up appointments to monitor progress and adjust care plans as necessary. Ongoing support is vital for effective management of caregiver incontinence care issues.
Support Emotional Well-Being and Dignity in Care
Supporting the emotional well-being of individuals with bladder control issues is essential for enhancing their quality of life. Many face significant challenges, including stigma and feelings of helplessness. Research shows that 45% of people feel embarrassed about their condition, which can lead to isolation and shame. Additionally, 23% report experiencing feelings of helplessness. These emotional struggles highlight the need for effective strategies in caregiver incontinence care.
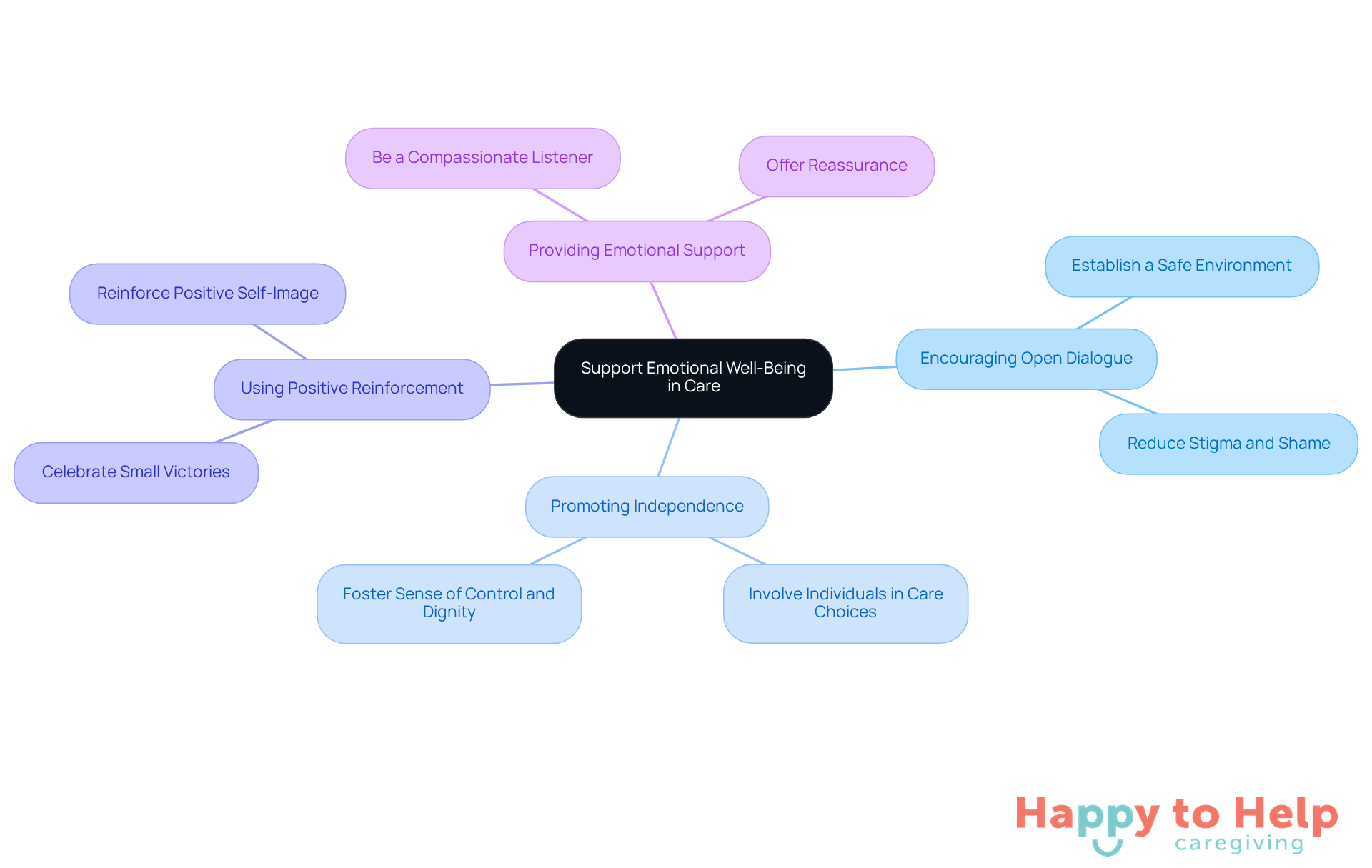
To address these challenges, caregivers can implement several key strategies:
- Encouraging Open Dialogue: Establish a safe environment where individuals can openly discuss their feelings about incontinence. This approach helps reduce the stigma and shame often associated with the condition, allowing for more honest conversations about their experiences and needs.
- Promoting Independence: Empower individuals by involving them in their care choices. This participation fosters a sense of control and dignity, which is crucial for emotional health. When people feel they have a say in their care, it can significantly enhance their self-esteem and overall well-being.
- Using Positive Reinforcement: Celebrate small victories in managing bladder control. Acknowledging progress, no matter how minor, reinforces a positive self-image and encourages continued efforts in care management. This method can help address feelings of helplessness.
- Providing Emotional Support: Be a compassionate listener and offer reassurance. Emotional support can ease feelings of shame and embarrassment, which are common among those facing urinary issues.
Real-life examples demonstrate the effectiveness of these strategies. Caregivers in incontinence care often encourage open conversations about bladder control, allowing individuals to feel more comfortable sharing their worries and leading to improved management of their condition. Psychologists emphasize the importance of fostering dignity in care. As Sarah Jenkins, Executive Director of NAFC, stated, "This data validates what patients have been communicating to us for years, that urinary issues impact both body and mind."
People are struggling daily with fear, shame, and isolation. It is crucial that emotional and mental health support becomes a standard aspect of urinary care, not an afterthought. By applying these approaches, caregiver incontinence care can create a supportive atmosphere that addresses the physical challenges of incontinence while promoting the emotional and mental health of individuals, nurturing a sense of dignity and respect throughout the care process.
Prioritize Self-Care for Caregivers
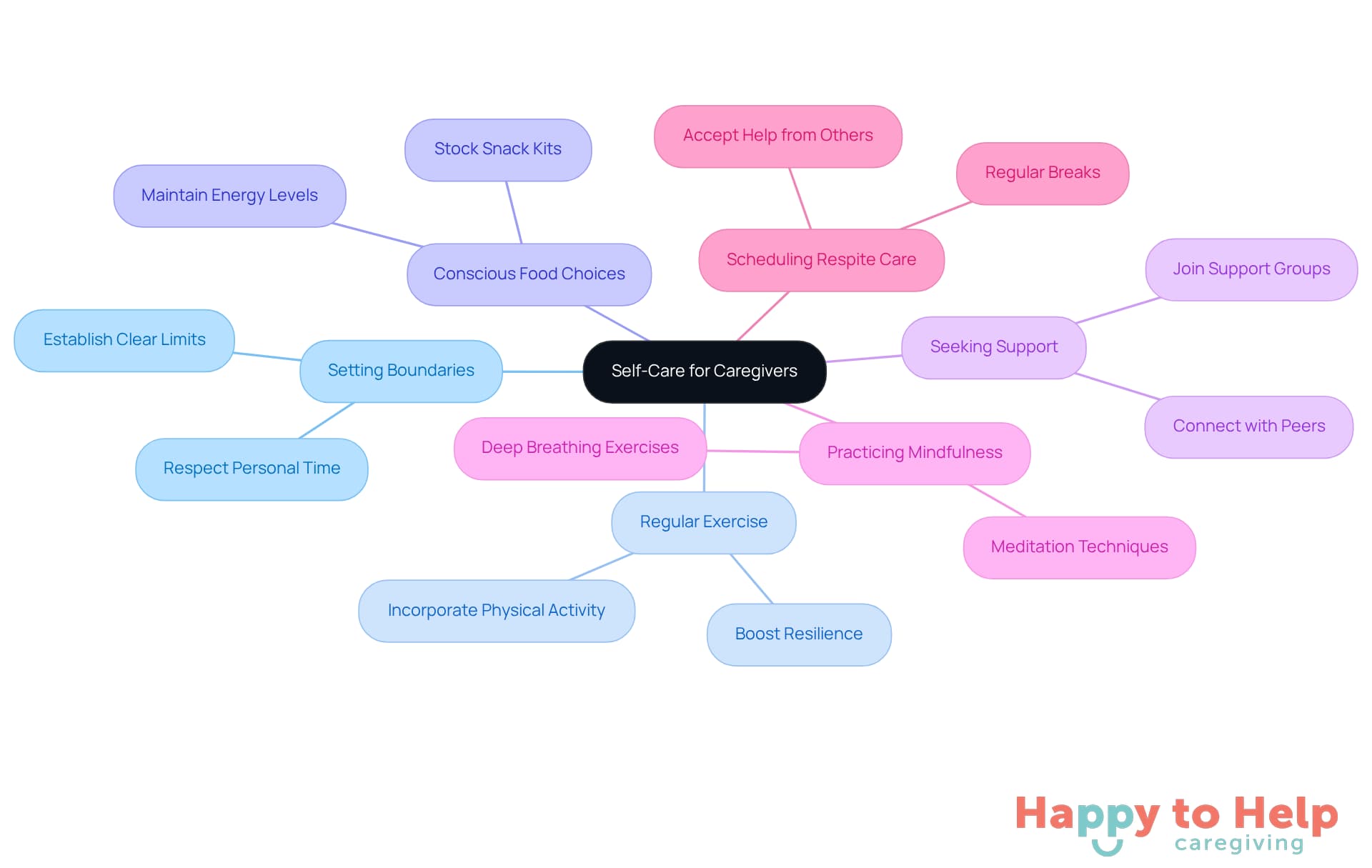
Caregivers face a significant challenge: prioritizing their own well-being while providing effective care. Neglecting self-care can lead to burnout and decreased effectiveness in their roles. To combat this, caregivers must implement practical strategies that support their mental and physical health.
One essential method is setting boundaries. Caregivers should establish clear limits to ensure their personal time is respected, allowing for necessary breaks from caregiving responsibilities. This practice not only helps maintain mental health but also fosters a more balanced caregiving experience.
Engaging in regular exercise is another vital strategy. Physical activity alleviates stress and enhances overall well-being, boosting resilience. For instance, caregivers who incorporate even brief periods of exercise into their routines often report feeling more energized and better equipped to tackle daily challenges. Jessica O. highlights the importance of conscious food choices, suggesting that keeping a snack kit stocked with nourishing options can help maintain energy levels during busy caregiving days.
Seeking support is equally important. Joining support groups or connecting with others in similar roles provides a platform to share experiences and coping strategies, alleviating feelings of isolation. Many caregivers find that discussing their challenges with peers helps them feel understood and less overwhelmed. Dr. Rush emphasizes the value of a supportive network, urging caregivers to recognize their support systems to ensure responsibilities are shared and manageable.
Practicing mindfulness techniques, such as meditation or deep breathing exercises, can significantly reduce stress and enhance emotional well-being. These practices encourage caregivers to take a moment for themselves, promoting a sense of calm amidst the demands of offering support.
Finally, scheduling regular respite care is essential for recharging and preventing burnout. By ensuring they have time to rest and rejuvenate, caregivers can maintain their effectiveness and compassion, ultimately benefiting both themselves and those they care for. Jennifer and Nathan G. shared how accepting help from friends and family made a significant difference in their caregiving journey, illustrating the importance of not bearing the burden alone.
Your Path Forward
Understanding and managing incontinence presents a significant challenge for caregivers. This issue not only affects the individuals experiencing it but also places a burden on those providing care. Without proper strategies, caregivers may struggle to maintain the dignity and independence of those they support, leading to frustration and emotional distress.
To address these challenges, caregivers can implement effective management techniques. The following strategies can significantly improve care:
- Establishing toileting schedules
- Managing fluid intake
- Promoting pelvic floor exercises
Additionally, fostering open communication with healthcare providers ensures caregivers have the necessary support and resources to meet the unique needs of their patients. Prioritizing emotional well-being and dignity is crucial, as these factors greatly influence the overall quality of life for individuals facing incontinence.
Ultimately, the importance of caregiver incontinence care cannot be overstated. Caregivers must also prioritize their own well-being through self-care practices, which helps them remain resilient and effective in their roles. By adopting these best practices, caregivers can create a supportive environment that addresses the physical challenges of incontinence while uplifting the emotional health of both caregivers and those they care for. Embracing these strategies leads to a more dignified, respectful, and compassionate caregiving experience for everyone involved.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5NDFmMzU2NDBkMmQ3ZTg4Njk3YTE1ZiIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What are the types of urinary incontinence?
The types of urinary incontinence include stress urinary leakage, urge urinary leakage, overflow urinary leakage, and functional urinary leakage.
What is stress incontinence?
Stress incontinence occurs when leakage happens during physical activities such as coughing, sneezing, or exercising, primarily due to weakened pelvic floor muscles.
What is urge incontinence?
Urge incontinence involves a sudden, intense urge to urinate that results in involuntary leakage, often linked to an overactive bladder.
What causes overflow incontinence?
Overflow incontinence arises when the bladder fails to empty completely, leading to frequent or constant dribbling of urine.
What is functional incontinence?
Functional incontinence is characterized by physical or cognitive impairments that hinder timely access to the bathroom, despite normal bladder function.
Why is it important for caregivers to recognize the type of urinary leakage?
Recognizing the type of urinary leakage is essential for caregivers to develop tailored strategies and interventions that meet the specific needs of the individual, enhancing their care and quality of life.
What are some challenges caregivers face in managing incontinence?
Caregivers face challenges such as accidents leading to embarrassment, loss of dignity, increased anxiety, and dependence on caregivers, which can affect both the individuals and the caregivers' well-being.
What is a toileting schedule and how does it help?
A toileting schedule involves implementing regular bathroom visits to reduce accidents and foster a reliable routine, enhancing dignity and confidence for individuals in caregiver incontinence care.
How can fluid intake management assist in incontinence care?
Managing fluid intake by encouraging hydration during the day and reducing excessive intake before bedtime can alleviate nighttime leakage while maintaining overall health.
What role do pelvic floor exercises play in managing incontinence?
Pelvic floor exercises, such as Kegels, can strengthen the muscles involved in bladder control, leading to a decrease in the intensity of leakage for individuals.
How can caregivers create a supportive environment for individuals with incontinence?
Caregivers can create a supportive environment by ensuring easy access to bathrooms, removing obstacles, and considering the installation of grab bars to enhance safety and independence.
List of Sources
- Understand the Types and Causes of Incontinence
- What causes urinary incontinence? | Bladder & Bowel Community (https://bladderandbowel.org/news/what-causes-urinary-incontinence)
- Low-impact yoga and exercise found to help older women manage urinary incontinence (https://med.stanford.edu/news/all-news/2024/09/yoga-exercise-incontinence.html)
- Types of Urinary Incontinence (https://news-medical.net/health/Types-of-Urinary-Incontinence.aspx)
- Bladder Disorders News (https://sciencedaily.com/news/health\_medicine/bladder\_disorders)
- New Device for Treating Urinary Incontinence Gives Patients More Control (https://hopkinsmedicine.org/news/articles/2025/03/new-device-for-treating-urinary-incontinence)
- Implement Effective Incontinence Management Techniques
- How Femtech Is Changing The Future Of Bladder Care (https://forbes.com/sites/geristengel/2025/10/27/uresta-tackles-stress-urinary-incontinence-with-femtech)
- New Device for Treating Urinary Incontinence Gives Patients More Control (https://hopkinsmedicine.org/news/articles/2025/03/new-device-for-treating-urinary-incontinence)
- Scheduled toileting: From incontinence to independence - Medline (https://medline.com/strategies/skin-health/scheduled-toileting-from-incontinence-to-independence)
- FDA grants 510(k) clearance to Revi System against urgency urinary incontinence | Contemporary OB/GYN (https://contemporaryobgyn.net/view/fda-grants-510-k-clearance-to-revi-system-against-urgency-urinary-incontinence)
- Foster Open Communication with Healthcare Providers
- Hospital Stay with Incontinence: A Practical Guide (https://becausemarket.com/blogs/news/hospital-stay-with-incontinence-a-practical-guide?srsltid=AfmBOorJUtVjINA6uweQeh6w9nNoT3EQYO1ROb09yBBI09QceQqvXZ1T)
- In home health, social determinants can predict urinary incontinence risk, study finds (https://mcknightshomecare.com/news/in-home-health-social-determinants-can-predict-urinary-incontinence-risk-study-finds)
- The Role of Healthcare Professionals in Incontinence Care - Forma-Care PRO (https://forma-care.co.uk/the-role-of-healthcare-professionals-in-incontinence-care)
- New Guidance for Ethical Urinary Incontinence Care for Older Adults - UCSF MedConnection (https://medconnection.ucsfhealth.org/news/new-guidance-for-ethical-urinary-incontinence-care-for-older-adults)
- Healthcare Providers' Perspectives on Communicating Incontinence and skin damage Information with Patients with dementia and their Family Caregivers: a descriptive study - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC5815364)
- Support Emotional Well-Being and Dignity in Care
- National Association for Continence Releases 6th Annual Survey: Mental Health Greatly Impacted By Incontinence (https://cbs42.com/business/press-releases/ein-presswire/869508331/national-association-for-continence-releases-6th-annual-survey-mental-health-greatly-impacted-by-incontinence)
- TENA Survey Reveals the Hidden Emotional Toll of Urinary Incontinence (https://fox40.com/business/press-releases/cision/20250514LN85727/tena-survey-reveals-the-hidden-emotional-toll-of-urinary-incontinence)
- NAFC Shines Light on the Connection Between Menopause and Incontinence in September/October 'We Count' Campaign (https://fox5sandiego.com/business/press-releases/ein-presswire/850429585/nafc-shines-light-on-the-connection-between-menopause-and-incontinence-in-september-october-we-count-campaign)
- The hidden side of incontinence: Mental health challenges - National Association For Continence (https://nafc.org/bhealth-blog/the-hidden-side-of-incontinence-mental-health-challenges)
- Can Urinary Incontinence Cause Depression? (https://flytetherapy.com/blogs/news/can-urinary-incontinence-cause-depression?srsltid=AfmBOoqYnt9ZQCi5Q9LCT6vewF8\_AAGGNJAKqT4DKfSJxOw23Q4L8MGW)
- Prioritize Self-Care for Caregivers
- 5 Self-Care Tips for Caregivers | United Way Worldwide (https://unitedway.org/news/5-self-care-tips-for-caregivers)
- Facebook (https://newsroom.clevelandclinic.org/2025/11/19/importance-of-self-care-for-family-caregivers)
- Self-Care Strategies for Brain Tumor Caregivers - National Brain Tumor Society (https://braintumor.org/news/self-care-strategies-for-brain-tumor-caregivers)
- Honoring America’s Family Caregivers, the Unseen Workforce Behind Our Health System - Medicare Rights Center (https://medicarerights.org/medicare-watch/2025/11/25/honoring-americas-family-caregivers-the-unseen-workforce-behind-our-health-system)
- AARP VI's Caring for the Caregiver Series Coming in 2025 (https://states.aarp.org/virgin-islands/aarp-vis-caring-for-the-caregiver-series-coming-in-2025)

