
What to Expect
Caring for older adults can be challenging, especially when it comes to their digestion. As caregivers, it’s essential to recognize the emotional weight of this responsibility. Many caregivers feel stressed and overwhelmed, but there are ways to ease these burdens.
Focusing on dietary changes can make a significant difference. Increasing fiber intake and ensuring proper hydration are vital steps. Alongside these dietary adjustments, incorporating regular physical activity and managing stress can greatly improve digestive health. These strategies not only help address common digestive challenges faced by older adults but also promote better nutrient absorption and overall gastrointestinal well-being.
Remember, you’re not alone in this journey. Many caregivers share similar experiences, and it’s okay to seek support. By making these changes, you’re taking a compassionate step towards enhancing the quality of life for those you care for.
Let’s embrace these strategies together, knowing that every small change contributes to a healthier, happier life for our loved ones.
What You Need to Know About Improve Digestion in Old Age: 4
As the body ages, the complexities of digestion become more pronounced, presenting unique challenges for caregivers. It’s not just about addressing discomfort; it’s about enhancing the overall well-being of older adults. Caregivers often feel the weight of this responsibility, especially with the risk of gastrointestinal disorders and changes in appetite looming. Navigating these intricacies requires both knowledge and compassion.
How can caregivers effectively implement dietary and lifestyle changes that truly make a difference in the digestive health of their loved ones? This question resonates deeply, as it reflects the desire to provide the best care possible. By understanding the emotional and practical support available, caregivers can find reassurance and encouragement in their journey.
Understand How Aging Affects Digestion
As we age, it is important to learn how to improve digestion in old age, as our digestive systems undergo significant changes that can affect our overall health. It’s important to recognize these shifts, especially for caregivers who are dedicated to supporting their loved ones.
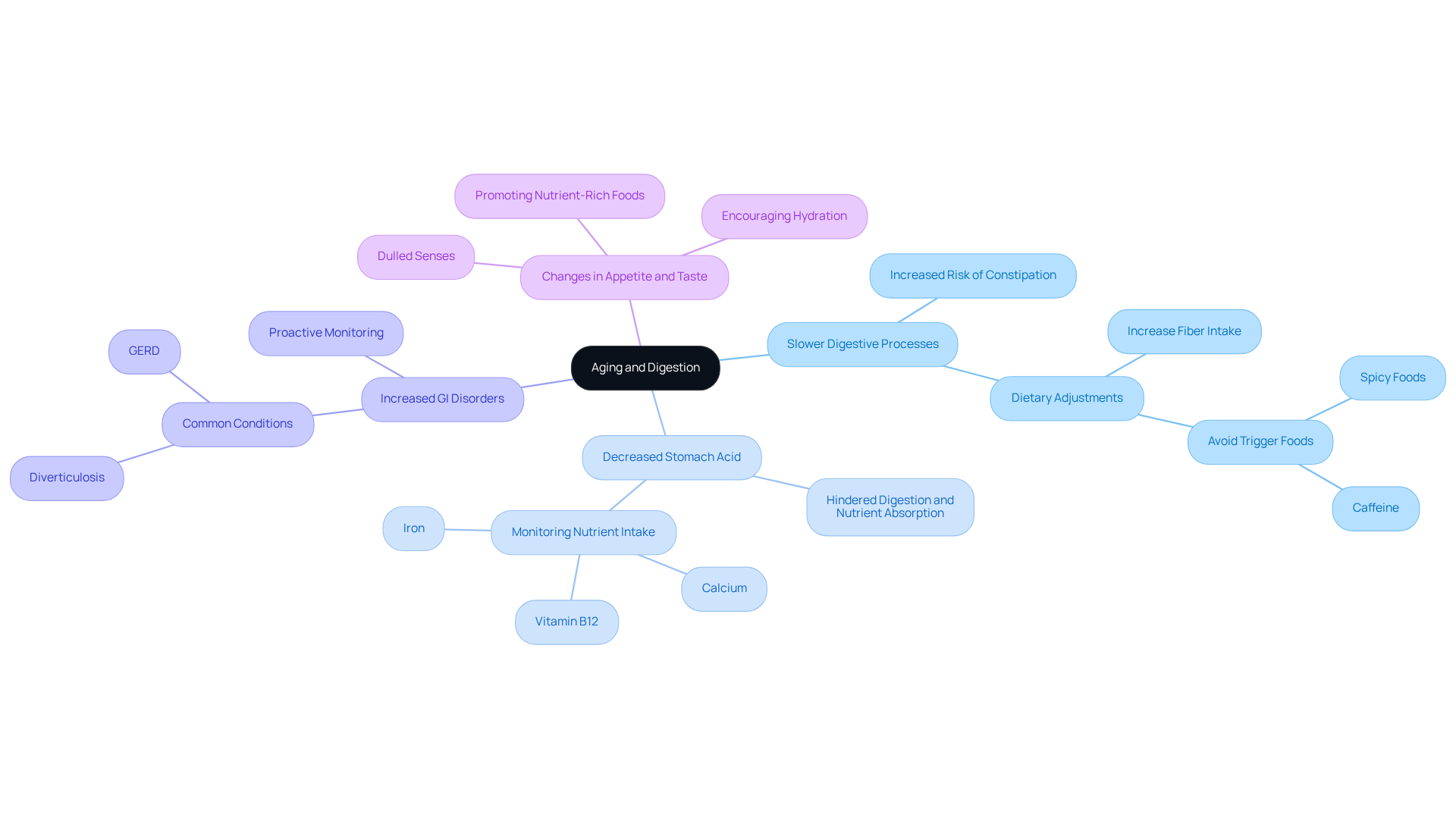
One major change is the slower digestive processes. The gastrointestinal (GI) tract tends to slow down, leading to slower food transit and an increased risk of constipation. This can cause discomfort, and caregivers should be mindful of this. Simple dietary adjustments, including how to improve digestion in old age by boosting fiber intake through fruits, vegetables, and whole grains, can make a difference. It’s also wise to avoid triggers such as spicy foods and caffeine to help promote regularity and ease.
Another factor is the decreased stomach acid production. As we age, our bodies often produce less stomach acid, which can hinder digestion and nutrient absorption. This decline might lead to bloating and indigestion, which emphasizes the need for knowledge on how to improve digestion in old age. Caregivers should keep a close eye on dietary intake, ensuring that individuals receive enough essential nutrients, particularly vitamins and minerals like B12, calcium, and iron, which are crucial for maintaining well-being.
Older adults also face an increased risk of gastrointestinal disorders. Conditions like diverticulosis and gastroesophageal reflux disease (GERD) become more common with age. It’s essential for caregivers to be attentive and proactive in monitoring their patients' digestive health, particularly in understanding how to improve digestion in old age, as these issues can significantly impact quality of life.
Lastly, the changes in appetite and taste can be quite challenging. Aging can dull our senses of taste and smell, which may lead to a decreased appetite. Caregivers can help by promoting nutrient-rich foods that appeal to the senses that remain. Encouraging hydration and regular physical activity can also support gastrointestinal health.
By recognizing these changes, caregivers can provide better assistance to those in their care, which includes understanding how to improve digestion in old age and promoting overall well-being. Remember, you’re not alone in this journey; support is available, and together, we can navigate these challenges with compassion and understanding.
Adopt Dietary Changes for Better Digestion
Caring for older adults can be a challenging journey, especially when figuring out how to improve digestion in old age. As caregivers, it’s essential to understand the emotional and practical support you can provide. Here are some dietary strategies that can make a significant difference:
-
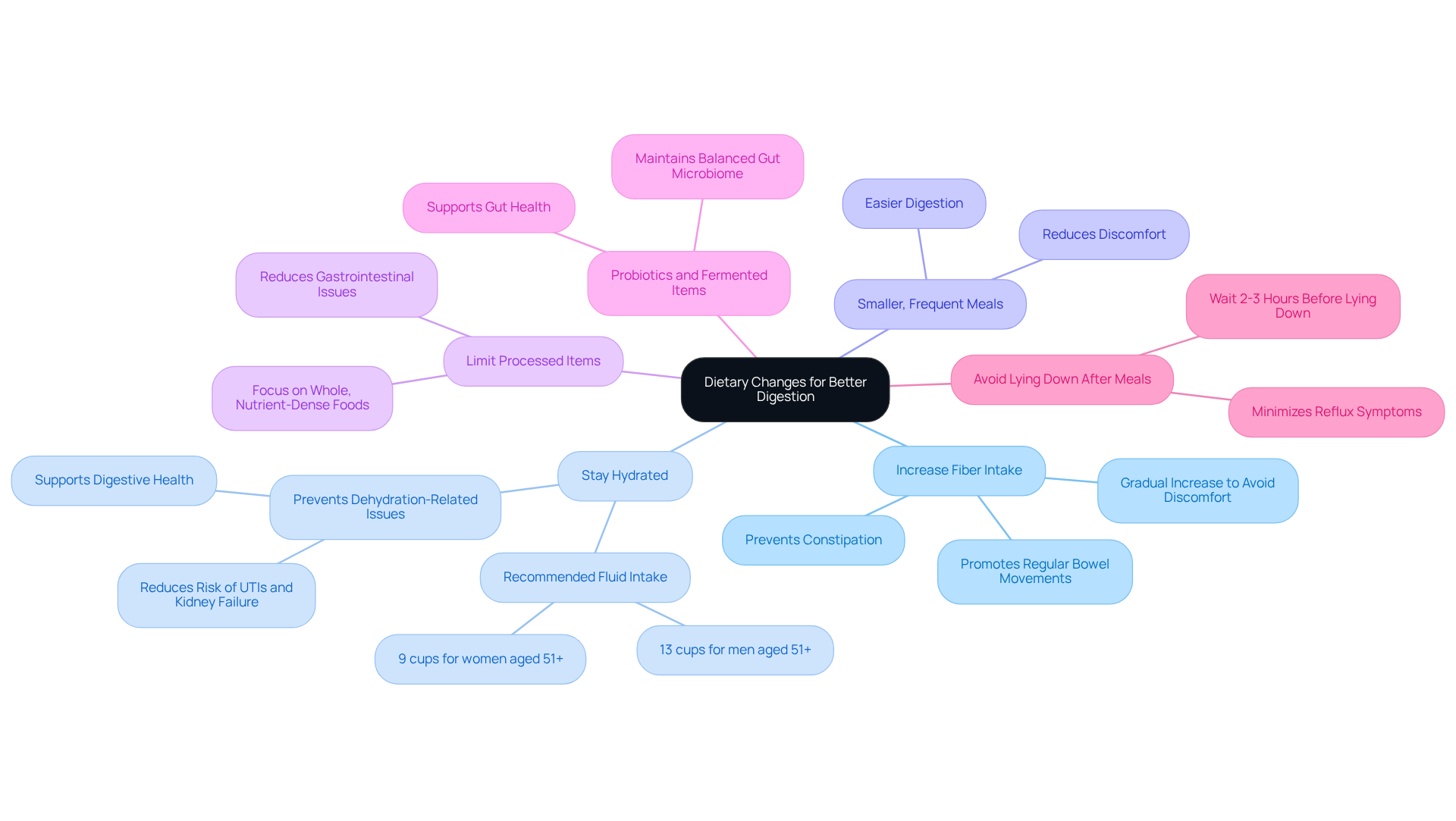
Increase Fiber Intake: Think about incorporating high-fiber foods like whole grains, fruits, vegetables, and legumes into their meals. Fiber plays a vital role in how to improve digestion in old age by promoting regular bowel movements and preventing constipation, which is a common concern for seniors. Gradually increasing fiber can help avoid discomfort like gas and bloating, which can happen if it’s introduced too quickly.
-
Stay Hydrated: Encourage your clients to drink plenty of fluids, especially water. Staying hydrated is essential when considering how to improve digestion in old age and also helps prevent dehydration. The National Academy of Medicine suggests about 13 cups of fluids daily for men and 9 cups for women aged 51 and older. It’s important to remember that many older adults may be chronically underhydrated, which can lead to serious health issues like urinary tract infections and kidney failure. Adequate hydration is crucial when considering how to improve digestion in old age, as dehydration can worsen constipation and lead to further complications.
-
Smaller, Frequent Meals: Suggest that they try smaller, more frequent meals instead of three large ones. This approach can help their digestive system process food more easily and reduce discomfort, providing insights on how to improve digestion in old age, especially since the gastrointestinal system tends to slow down with age.
-
Limit Processed Items: Encourage a decrease in high-fat and processed foods, as these can hinder digestion and contribute to gastrointestinal issues. Focusing on whole, nutrient-dense foods is essential for understanding how to improve digestion in old age.
-
Probiotics and Fermented Items: Incorporating probiotic-rich foods like yogurt, kefir, and sauerkraut can be beneficial for gut health. These foods can provide insights on how to improve digestion in old age and help maintain a balanced gut microbiome, which is essential for overall well-being.
-
Avoid Lying Down After Meals: Gently remind individuals to avoid lying down right after eating, as this can worsen reflux symptoms. Experts suggest waiting two to three hours after eating before lying down to minimize discomfort.
By implementing these dietary modifications, you can significantly enhance the health and well-being of those you care for. Remember, every small change can lead to a happier, healthier life.
Incorporate Lifestyle Modifications to Support Digestion
Caring for someone can be a challenging journey, and it’s important to remember that you’re not alone in this. Alongside dietary changes, there are several lifestyle modifications that can make a significant difference in your loved one’s well-being.
-
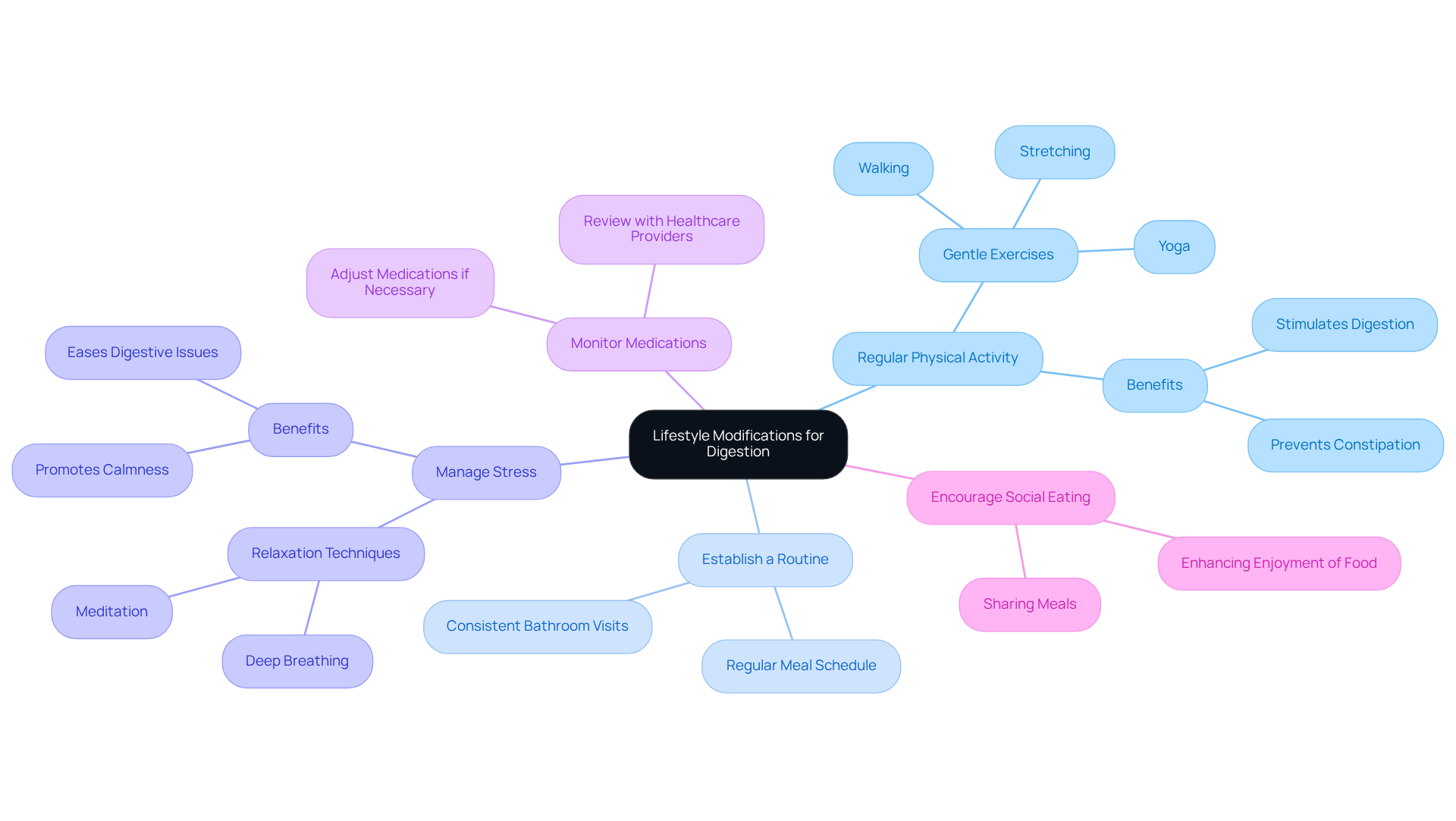
Regular Physical Activity: Gentle exercises like walking, stretching, or yoga can be incredibly beneficial. These activities not only stimulate digestion but also demonstrate how to improve digestion in old age and help prevent constipation, making daily life a bit easier.
-
Establish a Routine: Encouraging a regular schedule for meals and bathroom visits can promote gastrointestinal consistency. This simple step can bring comfort and predictability to your loved one’s day.
-
Managing stress is essential when considering how to improve digestion in old age, as stress can take a toll on digestion. It’s essential to help individuals discover relaxation techniques, such as deep breathing or meditation, to ease their stress levels. A calm mind often leads to a healthier body.
-
Monitor Medications: Some medications can impact digestion. Collaborating with healthcare providers to review and adjust medications can help minimize gastrointestinal side effects, ensuring your loved one feels their best.
-
Encourage Social Eating: Sharing meals with others can enhance the enjoyment of food and stimulate appetite. This is especially important for seniors who may find themselves eating alone.
By incorporating these lifestyle changes, you can greatly improve your loved one’s wellness and overall quality of life as part of learning how to improve digestion in old age. Remember, every small step counts, and your compassionate care makes a world of difference.
Monitor and Adjust Care Plans for Optimal Digestive Health
To ensure optimal digestive health, caregivers can take several compassionate steps:
-
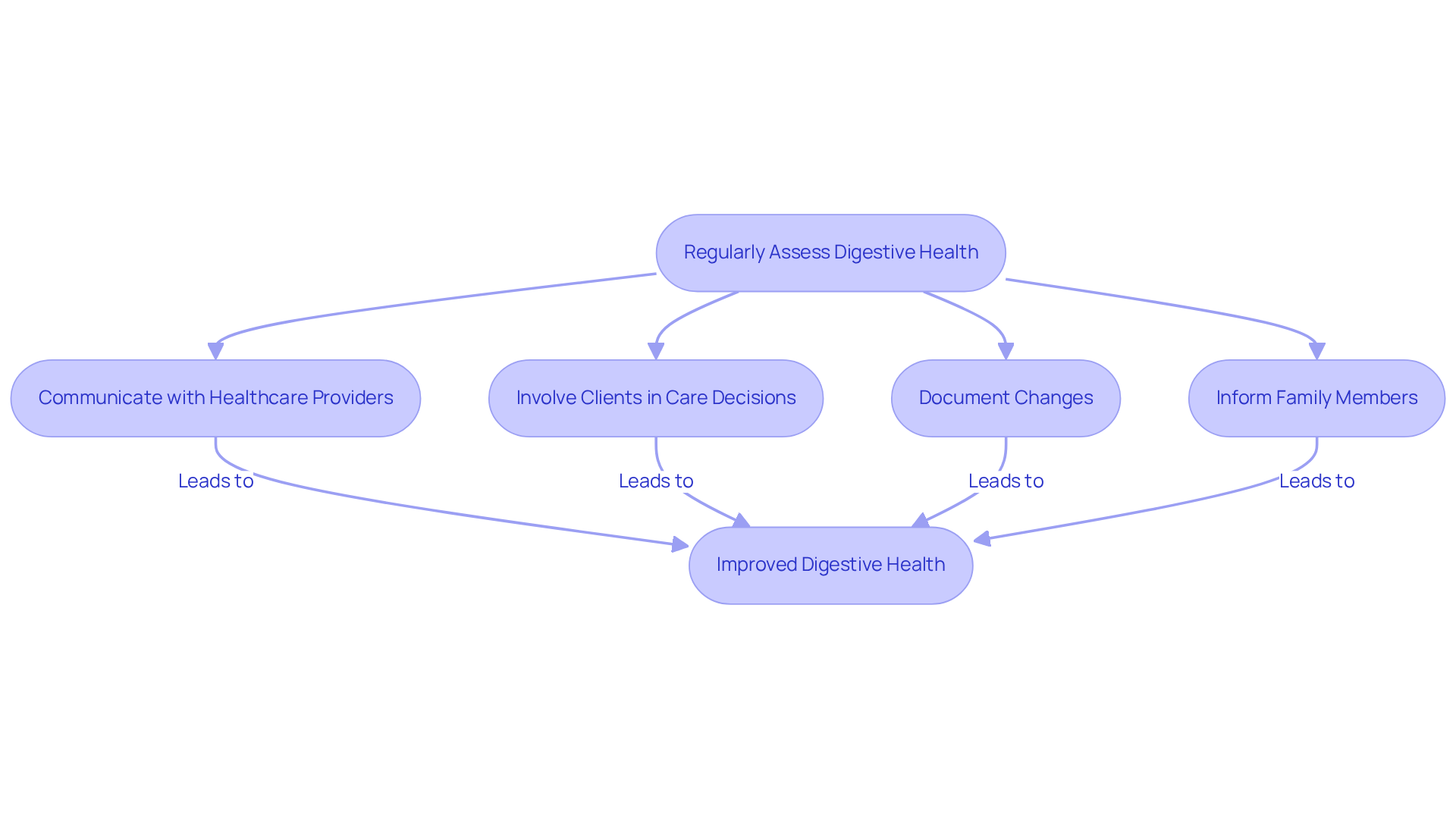
Regularly Assess Digestive Health: It’s important to keep an eye on clients for symptoms like constipation, bloating, or discomfort. Adjusting care plans as needed can make a significant difference. With about 85% of older adults living with at least one chronic medical condition, proactive monitoring is essential. This helps identify issues early and facilitates timely interventions, easing the stress for both caregivers and clients.
-
Communicate with Healthcare Providers: Establishing open lines of communication with doctors and dietitians is crucial. As highlighted by the NIH National Institute on Aging, "Effective communication can help build satisfying relationships with older patients to best manage their care." This ensures that care plans align with medical recommendations and dietary needs, which is vital for understanding how to improve digestion in old age effectively.
-
Involve Clients in Care Decisions: Engaging clients in discussions about their care plans and preferences empowers them. This involvement nurtures a sense of control over their wellness, positively influencing their overall well-being. It’s about making them feel heard and valued in their journey.
-
Document Changes: Keeping detailed records of dietary changes, symptoms, and adjustments to care plans is essential. This documentation helps recognize patterns and guides future care choices, ultimately leading to improved well-being outcomes. It’s a way to reflect on progress and adapt as needed.
-
Inform Family Members: Sharing information with family members about their loved one's gastrointestinal well-being is important. Letting them know how they can assist with dietary and lifestyle adjustments at home enhances support and encourages adherence to recommended changes. Family involvement can make a world of difference.
By actively monitoring and adjusting care plans, caregivers can ensure that their clients receive the best possible support on how to improve digestion in old age. This leads to an improved quality of life and overall well-being. Real-world examples of successful adjustments to care plans can further illustrate the importance of these strategies, showcasing how effective communication with healthcare providers can lead to better outcomes. Remember, you’re not alone in this journey; together, we can make a meaningful impact.
Your Path Forward
Understanding how to improve digestion in old age is crucial for caregivers. The aging process brings about various changes that can significantly affect an individual's digestive health. By recognizing these changes, caregivers can take meaningful steps to support their loved ones, helping them maintain a healthy and comfortable lifestyle.
This article highlights several key strategies to enhance digestion in older adults:
-
Simple dietary modifications:
- Increasing fiber intake
- Staying hydrated
- Choosing smaller, more frequent meals
-
Lifestyle adjustments:
- Regular physical activity
- Stress management
- Social eating
It's essential for caregivers to monitor and adjust care plans, allowing them to respond effectively to the unique needs of each individual.
Ultimately, the well-being of older adults relies on a blend of compassionate care, informed dietary choices, and supportive lifestyle practices. By implementing these strategies, caregivers can truly make a difference in the quality of life for those they support. Embracing these insights not only fosters better digestive health but also nurtures a sense of connection and understanding throughout the caregiving journey.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5MDk0MmEwMTcxNjIzNWZjMWEzZDM5ZiIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
How does aging affect the digestive system?
As we age, the digestive system undergoes significant changes, including slower digestive processes, decreased stomach acid production, and an increased risk of gastrointestinal disorders, all of which can impact overall health.
What are some common digestive issues faced by older adults?
Older adults may experience slower food transit, constipation, bloating, indigestion, and an increased risk of gastrointestinal disorders like diverticulosis and gastroesophageal reflux disease (GERD).
How can dietary adjustments improve digestion in old age?
Simple dietary adjustments such as increasing fiber intake through fruits, vegetables, and whole grains can help improve digestion. It's also advisable to avoid triggers like spicy foods and caffeine.
Why is stomach acid production important for digestion in older adults?
Stomach acid is crucial for digestion and nutrient absorption. A decrease in stomach acid production with age can hinder these processes, potentially leading to bloating and indigestion.
What nutrients should caregivers ensure older adults receive?
Caregivers should ensure that older adults receive essential nutrients, particularly vitamins and minerals like B12, calcium, and iron, which are important for maintaining well-being.
How can caregivers support older adults with changes in appetite and taste?
Caregivers can promote nutrient-rich foods that appeal to the senses that remain, encourage hydration, and support regular physical activity to help maintain gastrointestinal health.
What role do caregivers play in managing digestive health for older adults?
Caregivers should monitor their patients' digestive health, recognize changes in digestion, and provide support through dietary adjustments and promoting overall well-being.

