
What You Need to Know About Manage Delirium Sundowning: Essential
Delirium sundowning can be a daunting challenge for caregivers. It often brings about increased confusion and agitation in the late afternoon and evening, especially for those living with dementia. This experience can be overwhelming, not just for the individuals affected but also for their caregivers, who bear the emotional weight of these distressing episodes.
Understanding this phenomenon is essential. It affects the well-being of your loved ones and places immense strain on you as a caregiver. You might find yourself feeling stressed, anxious, or even burnt out. How can you effectively manage these moments while still providing a supportive environment?
This article explores essential strategies and resources designed to empower you. By navigating the complexities of delirium sundowning, you can enhance the quality of life for both yourself and your loved ones. Remember, you are not alone in this journey, and there are ways to find relief and support.
Understand Delirium Sundowning: Definition and Symptoms
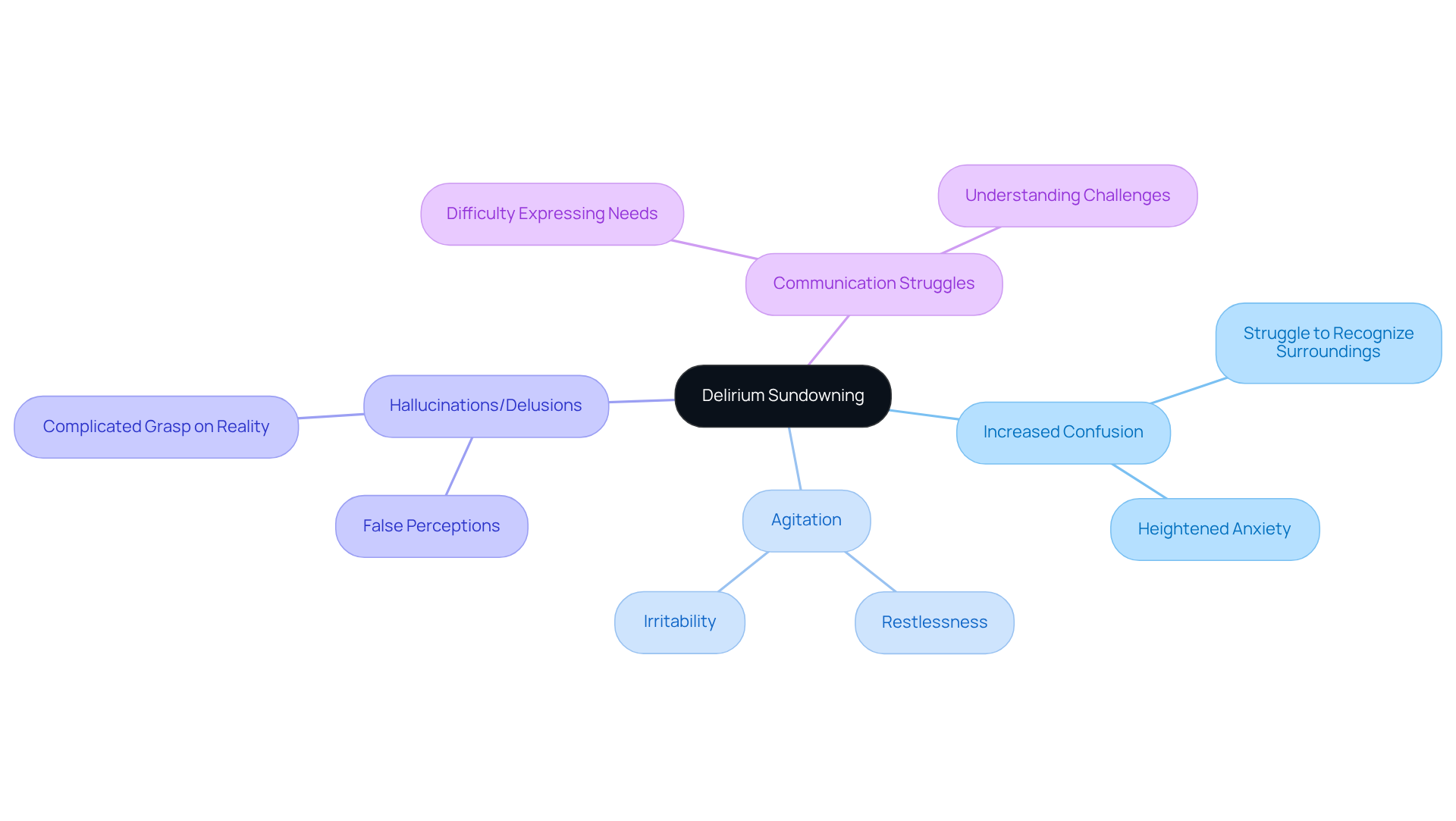
Experiencing delirium sundowning can be particularly challenging, especially for caregivers. Delirium sundowning often brings increased confusion, agitation, and disorientation, particularly in the late afternoon or evening. This is especially true for those living with dementia or cognitive impairments.
-
Increased confusion is common. Individuals may struggle to recognize familiar surroundings or loved ones, which can lead to heightened anxiety.
-
Agitation often intensifies during this time. Restlessness and irritability can make it difficult for caregivers to maintain a calm environment, adding to the stress of the situation.
-
Some may even experience hallucinations or delusions. These false perceptions can complicate their grasp on reality, making it even harder for them to feel secure.
-
Communication can also become a struggle. They might find it tough to express their needs or understand what others are saying, which can lead to feelings of frustration and isolation.
Recognizing these symptoms early is crucial for caregivers. It allows for the implementation of effective strategies to reduce distress and create a safer, more supportive environment. Recent studies underscore the importance of maintaining a predictable routine and ensuring ample exposure to natural light during the day. These practices can help ease the symptoms associated with delirium sundowning.
Moreover, geriatric specialists stress the need to monitor for underlying health issues, such as infections or medication side effects, which can worsen confusion and agitation. By understanding the nuances of delirium at twilight, caregivers can provide better support for their loved ones, ultimately enhancing their overall quality of life.
Remember, you’re not alone in this journey. Many caregivers share similar experiences, and there are resources available to help you navigate these challenges with compassion and care.
Identify Causes and Triggers of Delirium Sundowning
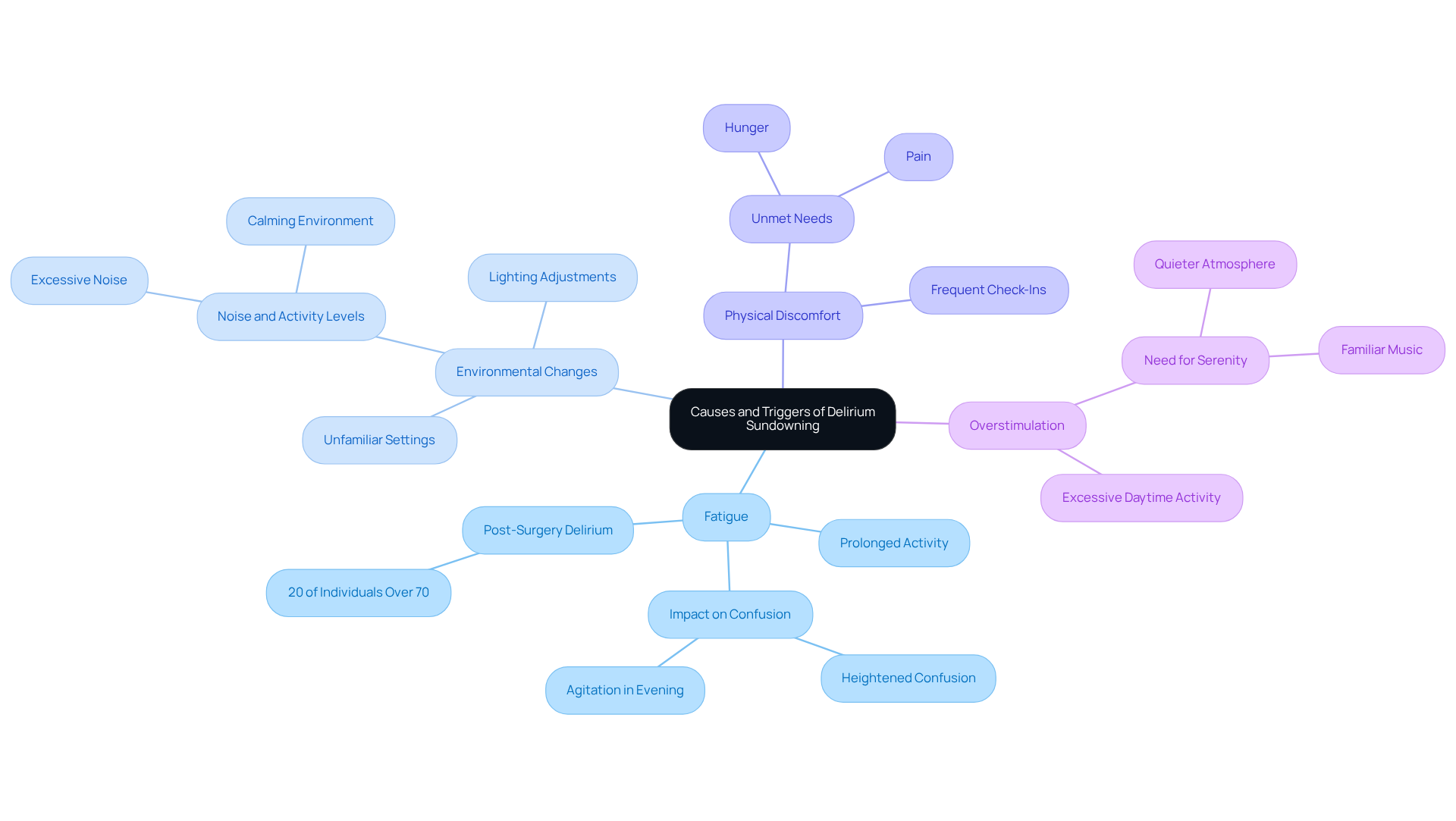
Delirium sundowning can be influenced by several key factors that caregivers should be aware of:
-
Fatigue: Prolonged activity throughout the day can lead to exhaustion. This often heightens confusion and agitation during the evening, which is referred to as delirium sundowning. It’s important to note that up to 20% of individuals over age 70 may experience delirium after elective surgery. Managing fatigue is crucial for their well-being.
-
Environmental Changes: Dimming lights or introducing unfamiliar settings can provoke anxiety and disorientation. Caregivers should strive to maintain a consistent and calming environment. Excessive noise or activity during the day can lead to increased agitation, which may trigger delirium sundowning as evening approaches, so creating a peaceful space is essential.
-
Physical Discomfort: Unmet needs such as hunger, pain, or other forms of discomfort can significantly worsen symptoms related to evening confusion. Frequent check-ins with loved ones are vital, as confusion during the evening may sometimes be a way of expressing these unmet needs.
-
Overstimulation: Excessive noise or activity during the day can lead to increased agitation as evening approaches. A quieter, more serene atmosphere in the late hours is necessary. Techniques like playing familiar music or providing sufficient lighting can help foster a soothing environment.
As caregivers, it’s important to closely observe your loved ones to identify specific triggers and make necessary environmental adjustments. Frequent interaction is recommended to reorient and reassure patients experiencing delirium sundowning. By actively overseeing these elements, you can create a more nurturing and pleasant atmosphere for those facing delirium at dusk.
Implement Strategies to Manage Delirium Sundowning
Managing delirium sundowning presents a challenging journey for caregivers, characterized by emotional ups and downs. It’s important to recognize the stress and burnout that often accompany this role. But there are effective strategies that can help ease these burdens and create a more supportive environment for both caregivers and those they care for.
-
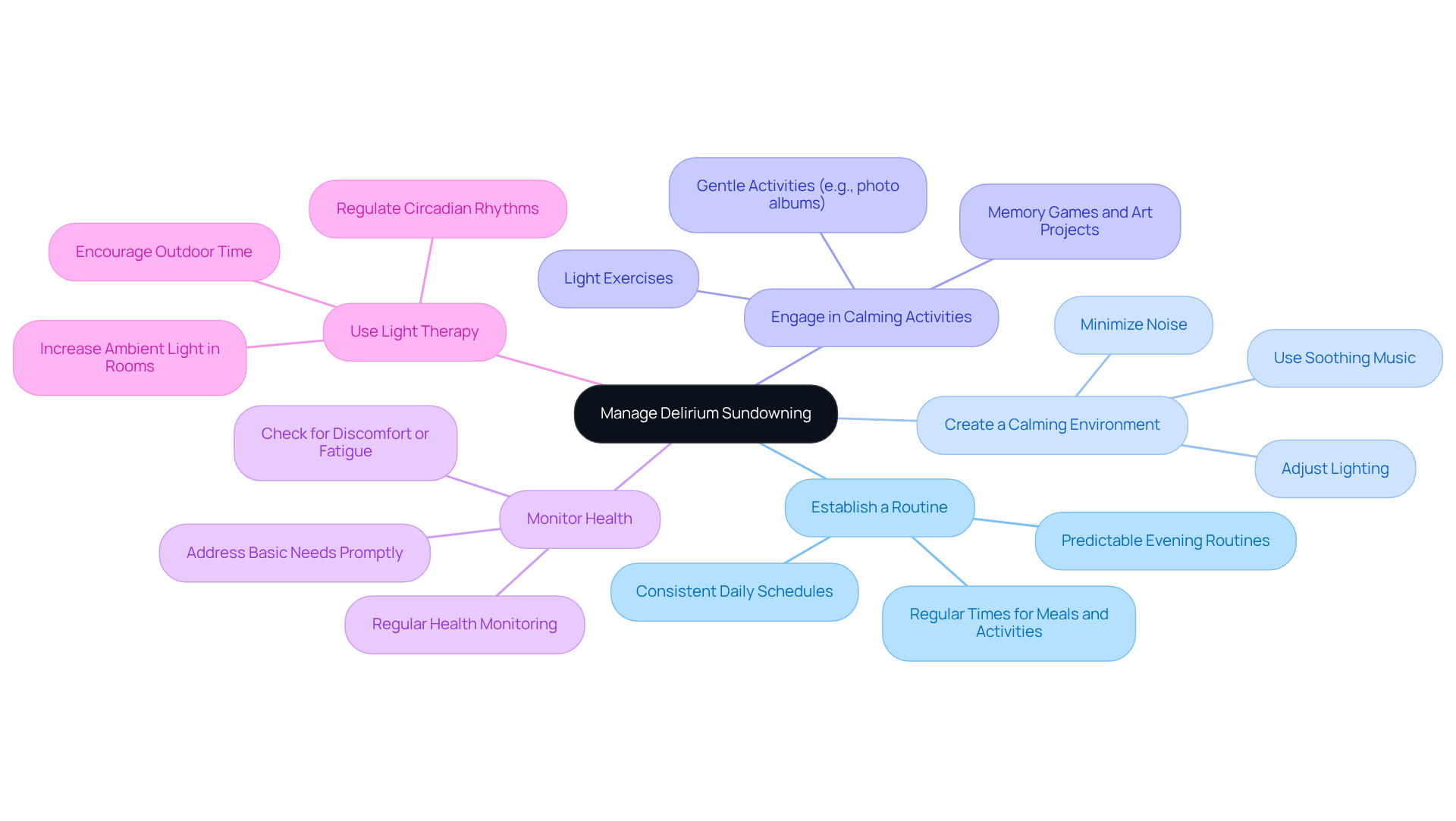
Establish a Routine: Creating consistent daily schedules for meals, activities, and bedtime can foster a sense of security and predictability. This is especially crucial for individuals with dementia. A reliable routine can significantly reduce anxiety and confusion during the evening hours, making the experience less overwhelming.
-
Create a Calming Environment: Adjusting the lighting to softer, warmer tones, minimizing noise, and playing soothing music can transform the atmosphere into a tranquil haven. These simple changes can alleviate feelings of confusion and anxiety, making evenings more manageable. As noted by The Landing Alexandria, "While delirium sundowning may be distressing, it can be effectively managed with the right setting, structured routines, and compassionate care."
-
Engage in Calming Activities: Incorporating gentle activities like looking through photo albums, listening to soft music, or participating in light exercises can provide comfort. Offering mentally stimulating yet soothing options, such as memory games or art projects, can serve as a distraction during challenging moments, bringing a sense of peace.
-
Monitor Health: Regularly checking for signs of discomfort, hunger, or fatigue is essential. Addressing these needs promptly can prevent increased agitation and enhance overall well-being. When caregivers are attentive to these basic physical needs, it creates a more harmonious environment.
-
Use Light Therapy: Exposure to natural light during the day plays a vital role in regulating circadian rhythms. Encouraging outdoor time or simply sitting by windows can help reinforce daytime alertness and improve sleep quality at night, ultimately easing evening-related symptoms.
By applying these compassionate strategies, caregivers can cultivate a supportive atmosphere that diminishes the effects of evening confusion. This not only enhances the quality of life for those receiving assistance but also brings a sense of fulfillment and peace to the caregivers themselves.
Access Resources and Support for Caregivers
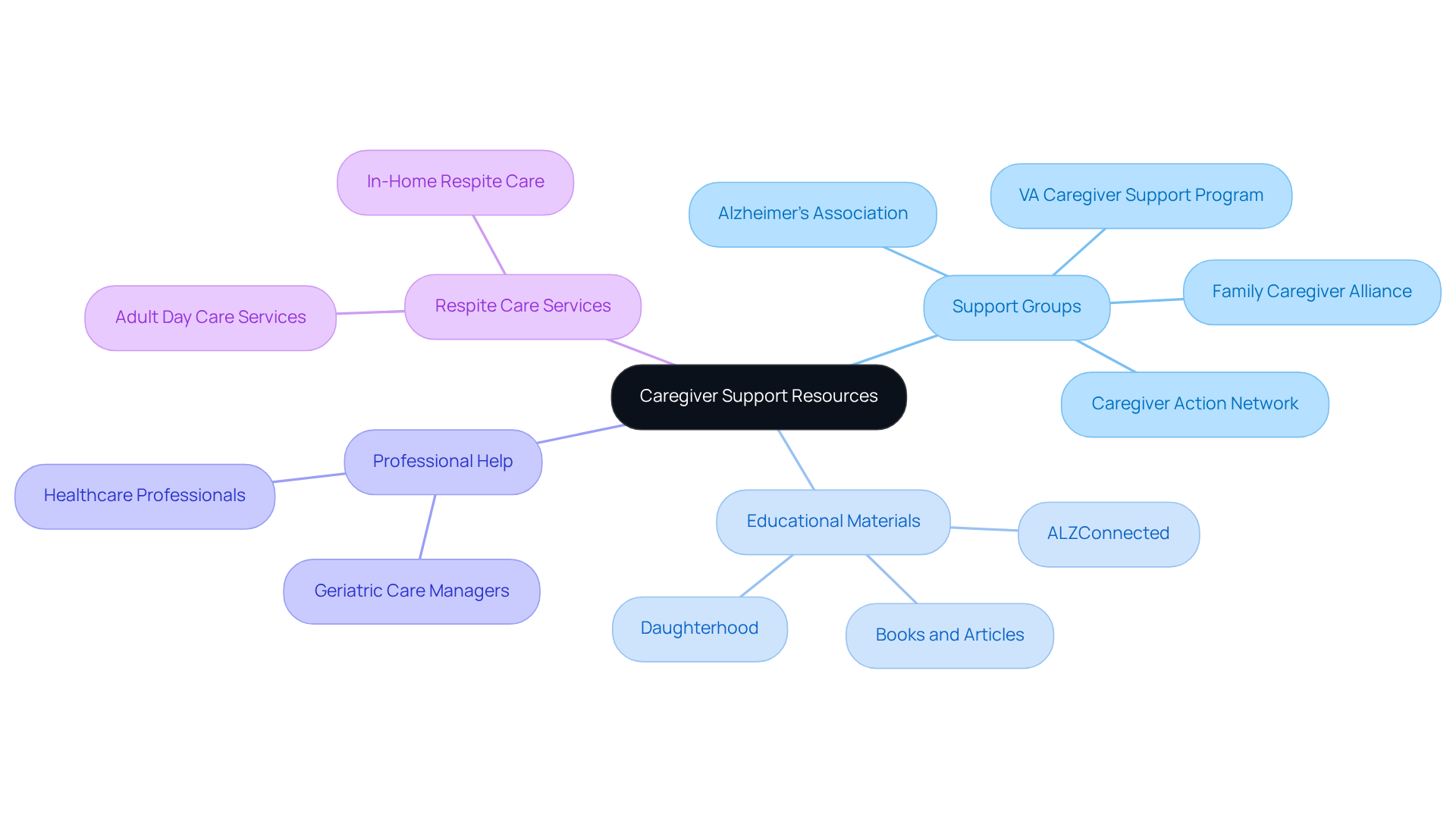
Caregivers often encounter overwhelming challenges, particularly when dealing with delirium sundowning. It’s crucial to seek support and resources that can help navigate these emotional waters. Joining support groups, like those offered by the Alzheimer’s Association or the Caregiver Action Network, can provide invaluable emotional assistance. These groups foster connections through shared experiences, reminding caregivers that they are not alone. As one leader aptly put it, "having a network of fellow supporters can make all the difference in managing the challenges of providing care."
Educational materials, such as books, articles, and online resources, can also shed light on effective caregiving strategies. For example, platforms like ALZConnected create a welcoming space for caregivers to ask questions and share advice, deepening their understanding of dementia-related challenges. Additionally, the VA Caregiver Support Program offers tailored services for those assisting veterans, broadening the support options available.
Professional help is equally important. Consulting healthcare professionals or geriatric care managers can provide personalized advice and support that cater to individual situations.
Moreover, utilizing respite care services is essential for caregivers. Research shows that respite assistance can significantly reduce stress and enhance overall well-being. This allows caregivers to recharge and return to their roles with renewed energy. By tapping into these resources, caregivers can not only enhance their skills but also alleviate the stress that often accompanies caregiving. Ultimately, this fosters a more supportive environment for both themselves and their loved ones.
Taking the Next Steps
Understanding and managing delirium sundowning is crucial for caregivers who face the unique challenges it brings. The late afternoon and evening hours can be particularly distressing for individuals experiencing confusion and agitation, especially those with cognitive impairments. Recognizing these symptoms and implementing effective strategies can help caregivers create a more supportive environment, enhancing the quality of life for both themselves and their loved ones.
Establishing a consistent routine, creating a calming atmosphere, and monitoring health needs are key points highlighted in this guide. Recognizing triggers such as fatigue, environmental changes, and overstimulation can significantly ease the effects of delirium sundowning. Moreover, accessing resources and support networks can provide caregivers with the emotional assistance and practical tools necessary to navigate these challenges.
Ultimately, the journey of caregiving doesn’t have to be traveled alone. Embracing available resources, connecting with support groups, and employing compassionate care strategies can transform the experience of managing delirium sundowning into one of empowerment and fulfillment. Caregivers are encouraged to take proactive steps, as their well-being directly influences the care they provide. This nurturing environment benefits everyone involved, fostering a sense of community and support.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5MWJjOGExYzQzNjZlYWM0YzJlMThhZCIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What is delirium sundowning?
Delirium sundowning is a phenomenon characterized by increased confusion, agitation, and disorientation that often occurs in the late afternoon or evening, particularly in individuals living with dementia or cognitive impairments.
What symptoms are associated with delirium sundowning?
Symptoms include increased confusion, agitation, restlessness, irritability, hallucinations or delusions, and difficulties in communication.
How does delirium sundowning affect communication?
Individuals may struggle to express their needs or understand what others are saying, leading to feelings of frustration and isolation.
Why is it important for caregivers to recognize symptoms of delirium sundowning early?
Early recognition allows caregivers to implement effective strategies to reduce distress and create a safer, more supportive environment for those affected.
What strategies can help manage symptoms of delirium sundowning?
Maintaining a predictable routine and ensuring ample exposure to natural light during the day can help ease symptoms associated with delirium sundowning.
What underlying health issues should caregivers monitor for in individuals experiencing delirium sundowning?
Caregivers should monitor for underlying health issues such as infections or medication side effects, as these can worsen confusion and agitation.
How can caregivers find support while managing delirium sundowning?
Caregivers can seek resources and connect with others who share similar experiences to navigate the challenges of delirium sundowning with compassion and care.

