
Why Support Strategies for Late Stage Matters
Understanding the complexities of late-stage dementia can be overwhelming, especially when it comes to appetite and eating habits. Caregivers often find themselves grappling with the challenges of mealtime, feeling the weight of their loved ones’ struggles. As cognitive decline and sensory changes intertwine, the simple act of eating can become a daunting task, leading to potential health risks.
This article aims to explore effective strategies to encourage eating and hydration. We want to offer caregivers valuable insights into creating supportive environments and adapting care approaches. It’s essential to recognize the emotional toll caregiving can take. How can caregivers navigate these challenges while ensuring the well-being of their loved ones?
By understanding these dynamics, caregivers can find ways to foster a nurturing atmosphere that promotes better eating habits. Together, we can address these concerns and provide the support needed to make mealtimes a little easier.
Understand Late-Stage Dementia and Its Effects on Appetite
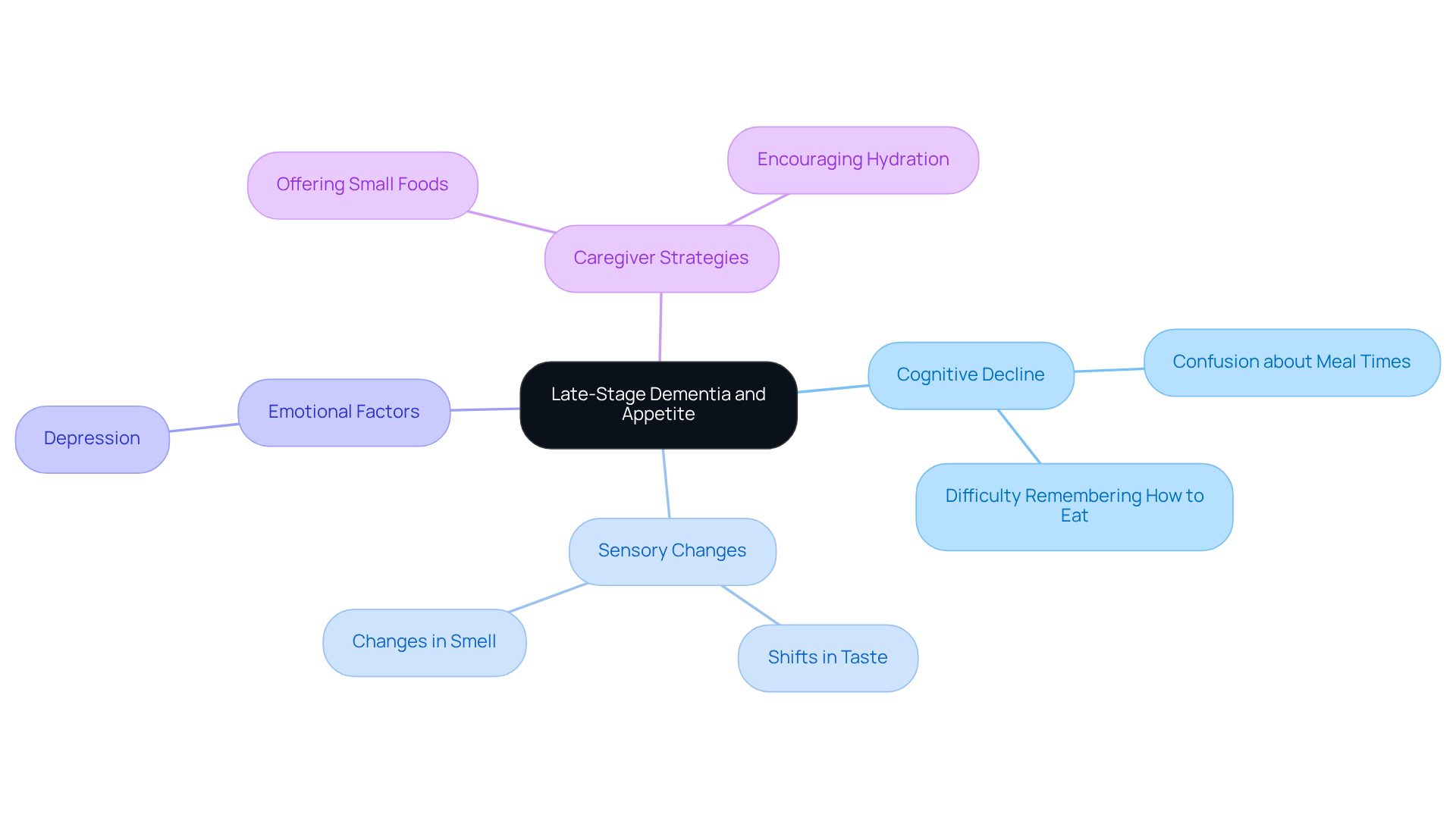
Late stage dementia not eating can profoundly affect how a person relates to meals, often leading to significant changes in their eating habits. Caregivers may notice that late stage dementia not eating is often accompanied by cognitive decline, causing confusion about meal times and difficulty remembering how to eat. Sensory changes, like shifts in taste and smell, can further lessen the appeal of meals.
It’s essential for caregivers to understand that these challenges arise from neurological impacts, not just behavioral choices. For instance, research indicates that up to 40% of individuals with Alzheimer’s experience depression, which is a known contributor to poor appetite. Additionally, swallowing difficulties, which are common in late stage dementia not eating, can complicate the eating process and increase the risk of choking or aspiration, potentially leading to serious health issues like pneumonia.
Recognizing these factors allows caregivers to approach mealtime with compassion and patience. The rejection of food may not be intentional in cases of late stage dementia not eating; it often reflects the individual’s struggle with the complexities of eating. By creating a supportive environment and using strategies such as offering small, favorite foods and encouraging hydration, caregivers can help ease these challenges and promote better nutritional intake.
Remember, you’re not alone in this journey. Many caregivers share similar experiences, and together, we can foster a nurturing atmosphere that prioritizes the well-being of those we care for.
Implement Strategies to Encourage Eating and Hydration
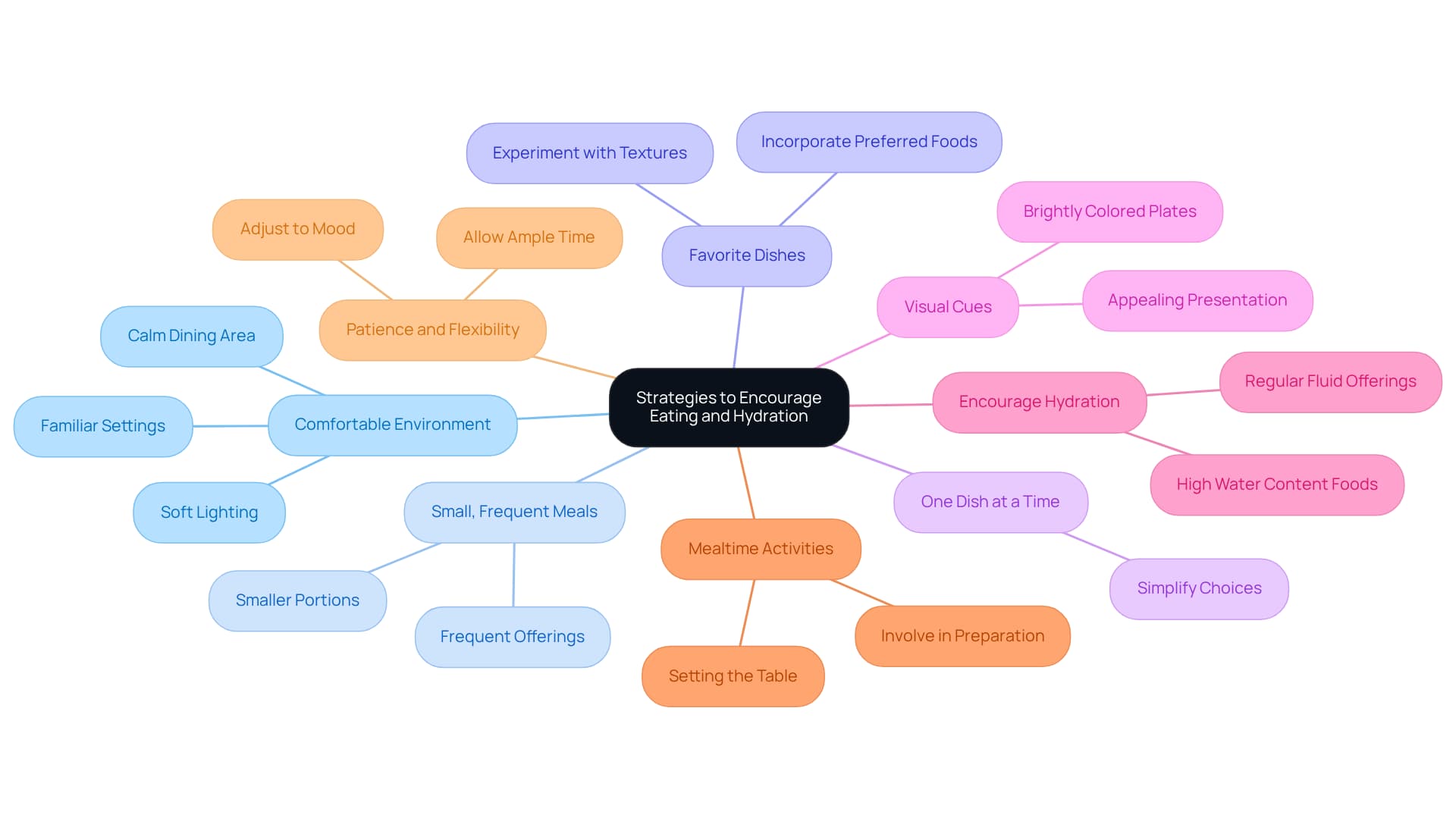
To encourage eating and hydration, caregivers can implement several effective strategies:
-
Create a Comfortable Environment: It’s essential to ensure the dining area is calm and free from distractions. Soft lighting and familiar settings can help ease anxiety and promote a sense of security.
-
Offer Small, Frequent Meals: Instead of three large meals, consider providing smaller portions throughout the day. This approach can make mealtime less daunting and more manageable for individuals experiencing late stage dementia not eating.
-
Incorporate Favorite Dishes: Incorporating favorite dishes can be beneficial, especially when considering that late stage dementia not eating can be influenced by using familiar and preferred items. Experimenting with different textures and flavors may help identify what appeals most to the individual.
-
Serve One Dish at a Time: Presenting one or two items at a time can simplify choices for the person with dementia, reducing feelings of being overwhelmed.
-
Use Visual Cues: Present food in an appealing manner. Brightly colored plates and utensils can enhance visual appeal and stimulate appetite, which may help address issues related to late stage dementia not eating, making mealtime more inviting.
-
Encourage Hydration: Offer fluids regularly, using cups that are easy to handle. Foods with high water content, like fruits and soups, can also help maintain hydration levels. Creative hydration strategies, such as offering visually appealing drinks, can enhance fluid intake.
-
Engage in Mealtime Activities: Involve the person in meal preparation or setting the table. This participation can create a sense of ownership and enjoyment during mealtimes.
-
Be Patient and Flexible: Allow ample time for meals and be ready to adjust according to the person's mood and preferences. Patience is key, as individuals with late stage dementia not eating may take longer to finish their meals.
As Carrie Madormo, a health writer, states, "To encourage your loved one to consume food, provide a comfortable environment and consider dining with them." This highlights the importance of creating a supportive atmosphere during mealtimes.
Monitor Changes and Adapt Care Approaches Accordingly
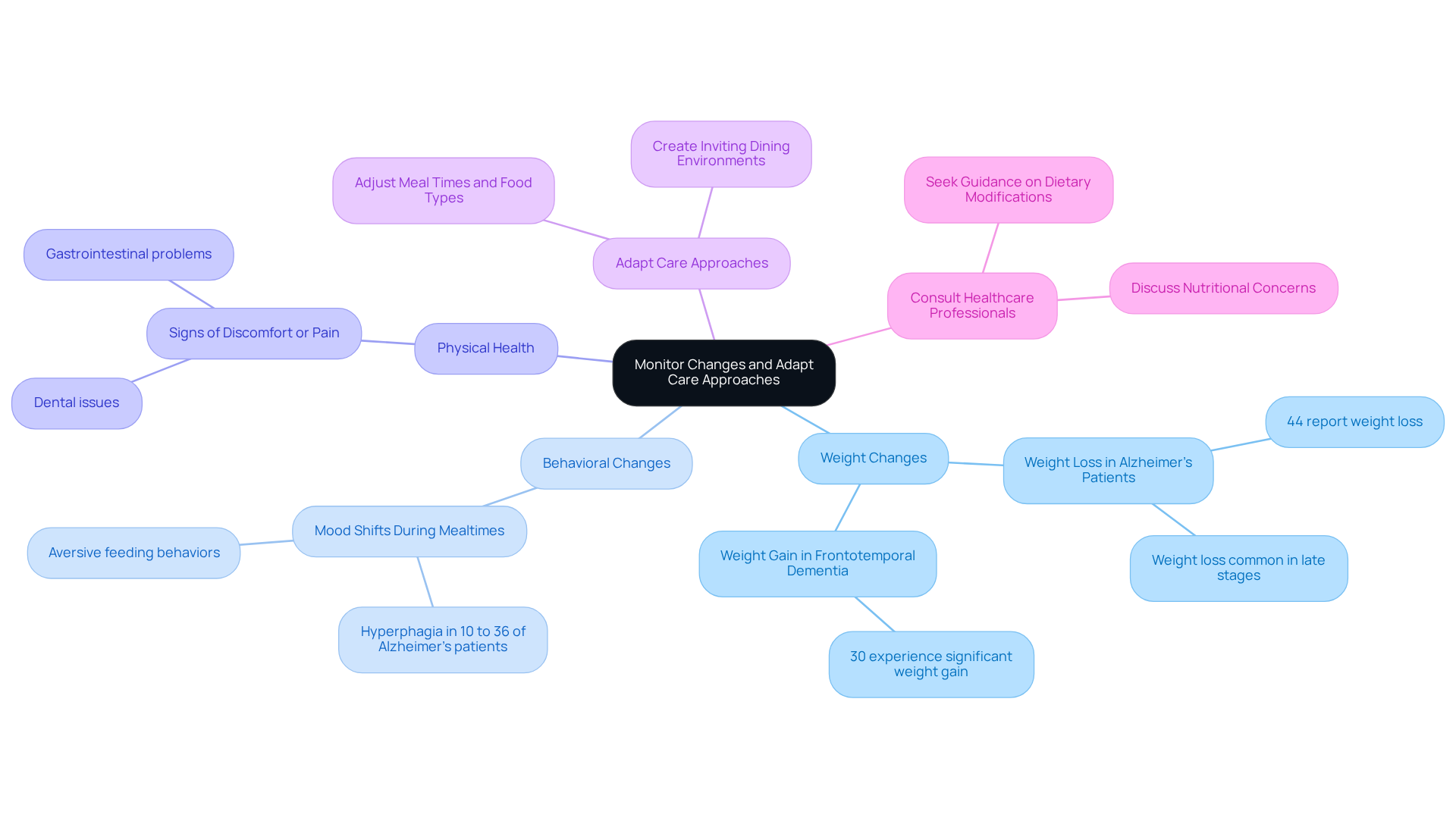
As caregivers, it's essential to monitor changes in eating habits and overall health, particularly when dealing with late stage dementia not eating. This vigilance can make a significant difference in the lives of those we care for. Here are some key indicators to monitor:
-
Weight Changes: Regularly checking weight can help identify significant fluctuations. Weight loss or gain often signals nutritional issues. Research indicates that weight fluctuations are common in individuals experiencing cognitive decline, with notable weight reduction seen in up to 44% of Alzheimer’s patients, especially in cases of late stage dementia not eating. It’s particularly concerning as weight loss tends to be most pronounced in the later stages of Huntington disease.
-
Behavioral Changes: Pay attention to any shifts in mood or behavior during mealtimes. These changes can greatly impact appetite and willingness to eat, particularly in cases of late stage dementia not eating. For example, hyperphagia has been reported in 10% to 36% of Alzheimer’s patients, while those with dementia may show aversive feeding behaviors, which can add to caregiver stress.
-
Physical Health: Be on the lookout for signs of discomfort or pain that might hinder eating, such as dental issues or gastrointestinal problems. These physical barriers can significantly affect a patient’s ability to consume adequate nutrition.
-
Adapt Care Approaches: If current strategies aren’t working, don’t hesitate to explore new methods. This might mean adjusting meal times, trying different food types, or creating a more inviting dining environment. Research shows that a pleasant and familiar dining atmosphere can encourage healthier habits. Remember, environmental modifications and caregiver support are vital for enhancing the dining experience and promoting nutritional intake.
-
Consult Healthcare Professionals: Keep the lines of communication open with healthcare providers about any concerns regarding nutrition and hydration. Seeking guidance on dietary modifications or supplements can be crucial, especially as cognitive decline progresses and nutritional needs change. Healthcare experts emphasize that late stage dementia not eating is associated with eating difficulties and dietary adjustments, highlighting the importance of recognizing early signs of nutritional challenges to enable timely interventions.
Manage Caregiver Stress and Emotional Well-Being
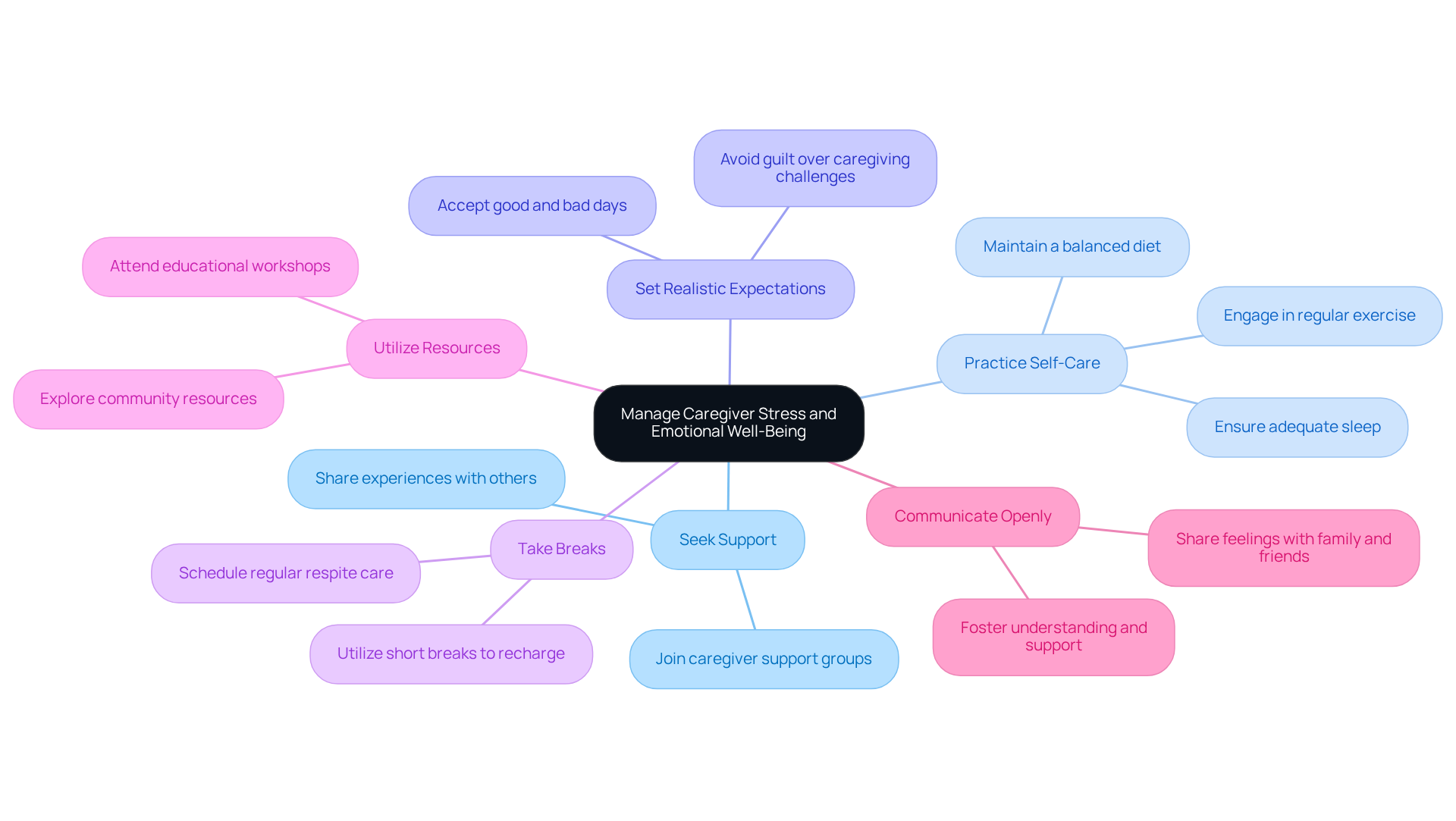
Caring for someone with late stage dementia not eating can be incredibly challenging, both emotionally and physically. It’s important to recognize the weight of this responsibility and the stress that often accompanies it. Here are some ways to help manage that stress and nurture your emotional well-being:
-
Seek Support: Connecting with others who understand your journey can be invaluable. Consider joining caregiver support groups where you can share experiences and gain insights from those in similar situations. You’re not alone in this.
-
Practice Self-Care: Remember to prioritize your own health. Engage in regular exercise, maintain a balanced diet, and ensure you’re getting enough sleep. Taking care of yourself is not just beneficial for you; it also enhances your ability to care for your loved one.
-
Set Realistic Expectations: It’s essential to understand that not every day will be perfect. Allow yourself the grace to experience both good and bad days without guilt. Embracing this reality can lighten your emotional load.
-
Take Breaks: Don’t underestimate the power of a break. Schedule regular respite care to recharge your batteries. Even short breaks can significantly reduce stress levels and help you return to your caregiving role with renewed energy.
-
Utilize Resources: Explore community resources available to you, such as counseling services or educational workshops. These can enhance your caregiving skills and build emotional resilience, making your journey a bit easier.
-
Communicate Openly: Sharing your feelings and concerns with family members or friends can alleviate emotional burdens. Open communication fosters understanding and support, reminding you that it’s okay to lean on others.
In this journey, remember that seeking help and taking care of yourself is not a sign of weakness; it’s a vital part of being a compassionate caregiver. You deserve support and understanding as you navigate this path.
Your Path Forward
Understanding the complexities of late-stage dementia and its impact on eating habits is crucial for caregivers. It’s essential to approach this with compassion, recognizing the neurological and emotional challenges faced by individuals in this stage. By fostering a supportive environment and implementing effective strategies, caregivers can significantly enhance the mealtime experience for those struggling with appetite loss.
Creating a comfortable dining space, offering small and frequent meals, and engaging individuals in mealtime activities are key insights that can make a difference. Monitoring changes in eating habits, weight, and overall health plays a vital role in adapting care approaches effectively. Remember, the emotional well-being of caregivers is paramount; their own health directly influences their ability to provide care.
Ultimately, caring for someone with late-stage dementia requires patience, understanding, and self-care. By employing these strategies and seeking support, caregivers can navigate this challenging path while prioritizing the nutritional needs and emotional well-being of both the individual and themselves. Embracing these practices not only promotes better eating habits but also fosters a nurturing atmosphere that honors the dignity of those affected by dementia.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5MTkxNDE3YTc1MDljMjI3ODFlOWZiOCIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What are the effects of late-stage dementia on appetite?
Late-stage dementia can lead to significant changes in eating habits, including confusion about meal times and difficulty remembering how to eat, which can profoundly affect a person's relationship with meals.
Why might individuals with late-stage dementia not eat?
Individuals may not eat due to cognitive decline, sensory changes that lessen the appeal of food, depression (which affects up to 40% of individuals with Alzheimer’s), and swallowing difficulties that complicate the eating process.
How do sensory changes impact eating in late-stage dementia?
Sensory changes, such as shifts in taste and smell, can reduce the appeal of meals, making individuals less interested in eating.
What health risks are associated with not eating in late-stage dementia?
Not eating can increase the risk of choking or aspiration, which may lead to serious health issues like pneumonia.
How can caregivers support individuals with late-stage dementia who are not eating?
Caregivers can create a supportive environment by offering small, favorite foods, encouraging hydration, and approaching mealtime with compassion and patience.
Is the rejection of food in late-stage dementia intentional?
No, the rejection of food is often not intentional; it typically reflects the individual's struggle with the complexities of eating due to their condition.
What is the importance of understanding the challenges related to eating in late-stage dementia?
Understanding these challenges allows caregivers to approach mealtime with empathy and to implement strategies that promote better nutritional intake and overall well-being.

