
Why Tackle Dementia and Eating Issues: Matters
Dementia profoundly alters an individual’s relationship with food, leading to a range of eating challenges that can be distressing for both patients and caregivers. Caregivers often face significant hurdles during mealtimes, which can create stress and frustration. These challenges not only affect the nutritional intake of those they care for but also impact the emotional well-being of both parties.
As caregivers navigate these complexities, they have the opportunity to implement effective strategies that enhance nutrition and improve the overall dining experience. By transforming daily challenges into moments of connection and comfort, caregivers can foster a more positive atmosphere during meals. This approach not only addresses the immediate issues but also strengthens the bond between caregiver and patient.
Understand the Impact of Dementia on Eating Behaviors
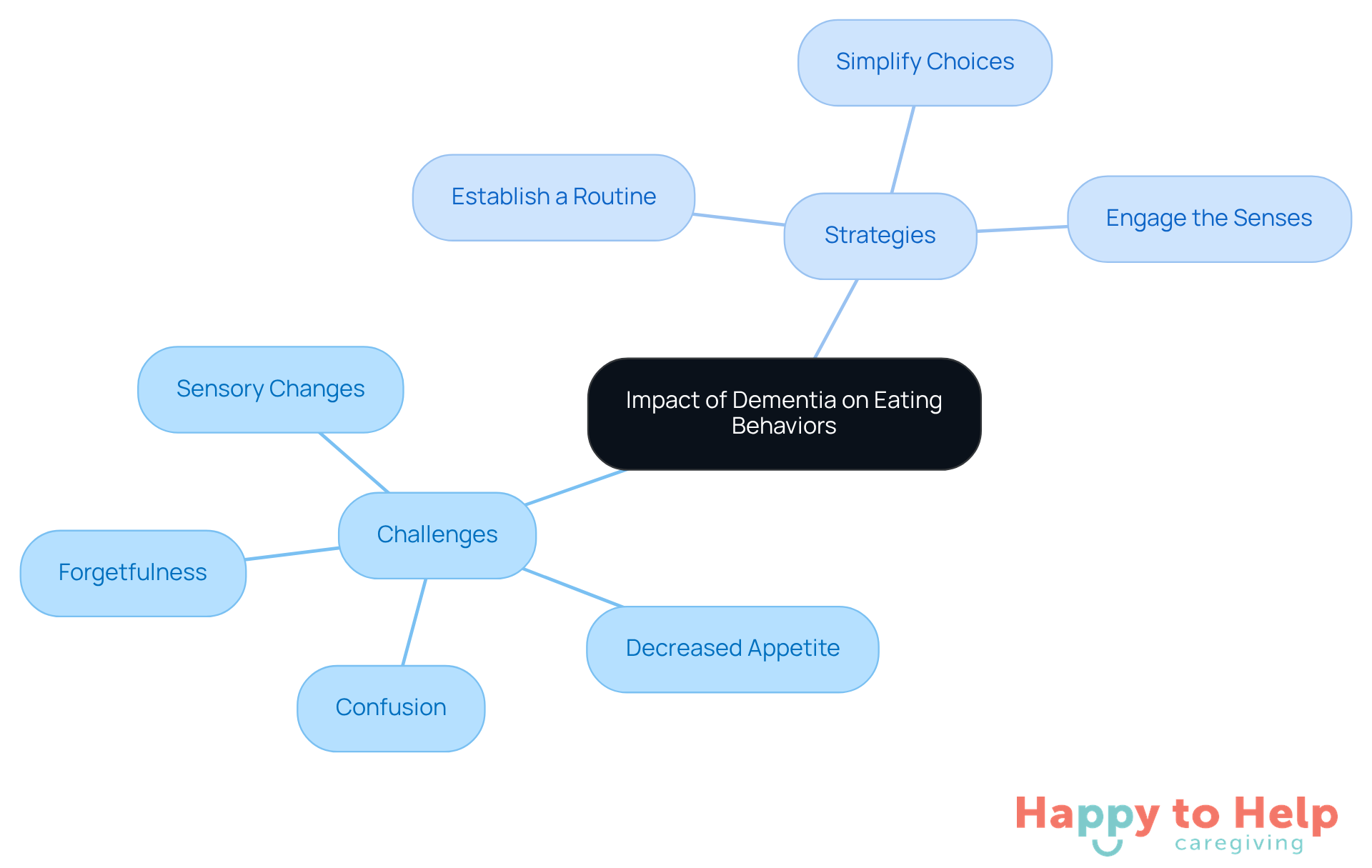
Dementia and eating issues significantly affect a person's relationship with food, leading to various eating challenges. Caregivers often encounter problems such as forgetfulness about mealtimes, decreased appetite, and confusion over dietary preferences. For example, individuals may forget if they’ve eaten or struggle to recognize familiar foods. Additionally, sensory changes, like shifts in taste and smell, can make once-loved meals unappealing.
These issues can create discomfort and distress during meals, potentially exacerbating dementia and eating issues. Caregivers need to be vigilant for signs of discomfort, as these can worsen the eating experience. By recognizing these challenges, caregivers can approach mealtimes with empathy and implement tailored strategies that address the unique needs of those they care for, particularly regarding dementia and eating issues.
To enhance the dining experience, caregivers can consider the following actionable tips:
- Establish a routine: Consistent mealtimes can help individuals with dementia remember when to eat.
- Simplify choices: Offer a limited selection of familiar foods to reduce confusion.
- Engage the senses: Present meals attractively and consider the individual's sensory preferences.
This compassionate approach not only improves the dining experience but also fosters a sense of security and comfort for those navigating the complexities of dementia.
Implement Strategies to Encourage Healthy Eating
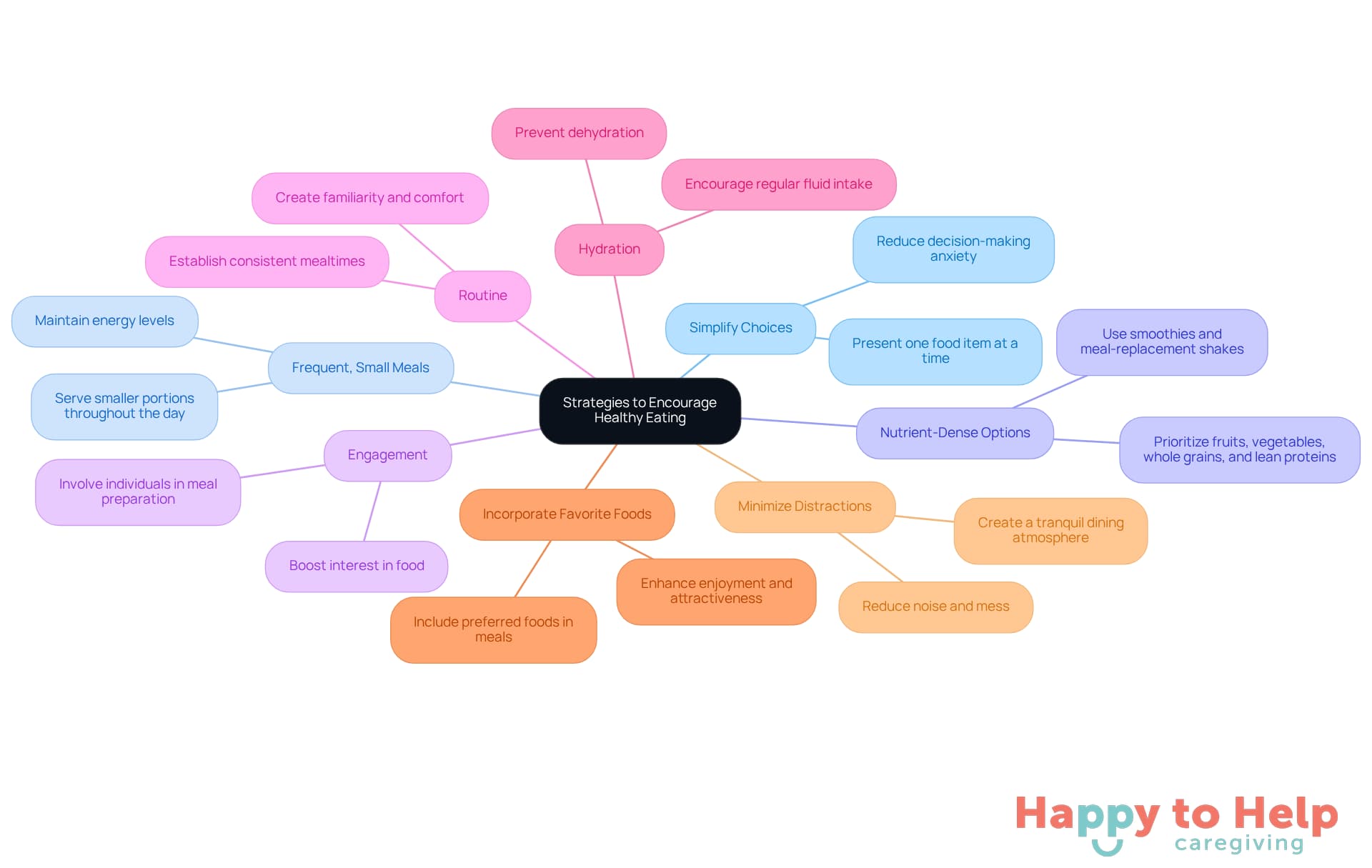
To promote healthy eating among individuals with dementia, caregivers face a significant challenge. Many individuals may struggle with appetite and nutrition, which can lead to health complications. However, there are effective strategies caregivers can adopt to address this issue:
-
Simplify Choices: Present one food item at a time. This minimizes overwhelm and helps the individual concentrate on their dining experience, reducing anxiety associated with decision-making.
-
Frequent, Small Meals: Instead of serving three large meals, offer smaller, more frequent meals throughout the day. This approach can help maintain energy levels and stimulate appetite, making eating feel less daunting.
-
Nutrient-Dense Options: Prioritize items abundant in nutrients, such as fruits, vegetables, whole grains, and lean proteins. Smoothies and meal-replacement shakes can be particularly beneficial, as they are easy to consume and packed with essential nutrients.
-
Engagement: Involve the person in meal preparation whenever possible. This involvement can boost their interest in cuisine and make mealtimes more enjoyable.
-
Routine: Establish a consistent mealtime routine to foster familiarity and comfort. A predictable schedule can help stimulate appetite and create a more relaxed dining experience.
-
Hydration: Encourage regular fluid intake by reminding individuals to drink water, juice, or other fluids throughout the day. This helps prevent dehydration and supports overall health.
-
Incorporate Favorite Foods: Include preferred foods in dishes to enhance enjoyment and attractiveness, which can help stimulate appetite.
-
Minimize Distractions: Establish a tranquil dining atmosphere by decreasing noise and mess. This enables the person to concentrate on their food without superfluous distractions.
Create a Dementia-Friendly Mealtime Environment
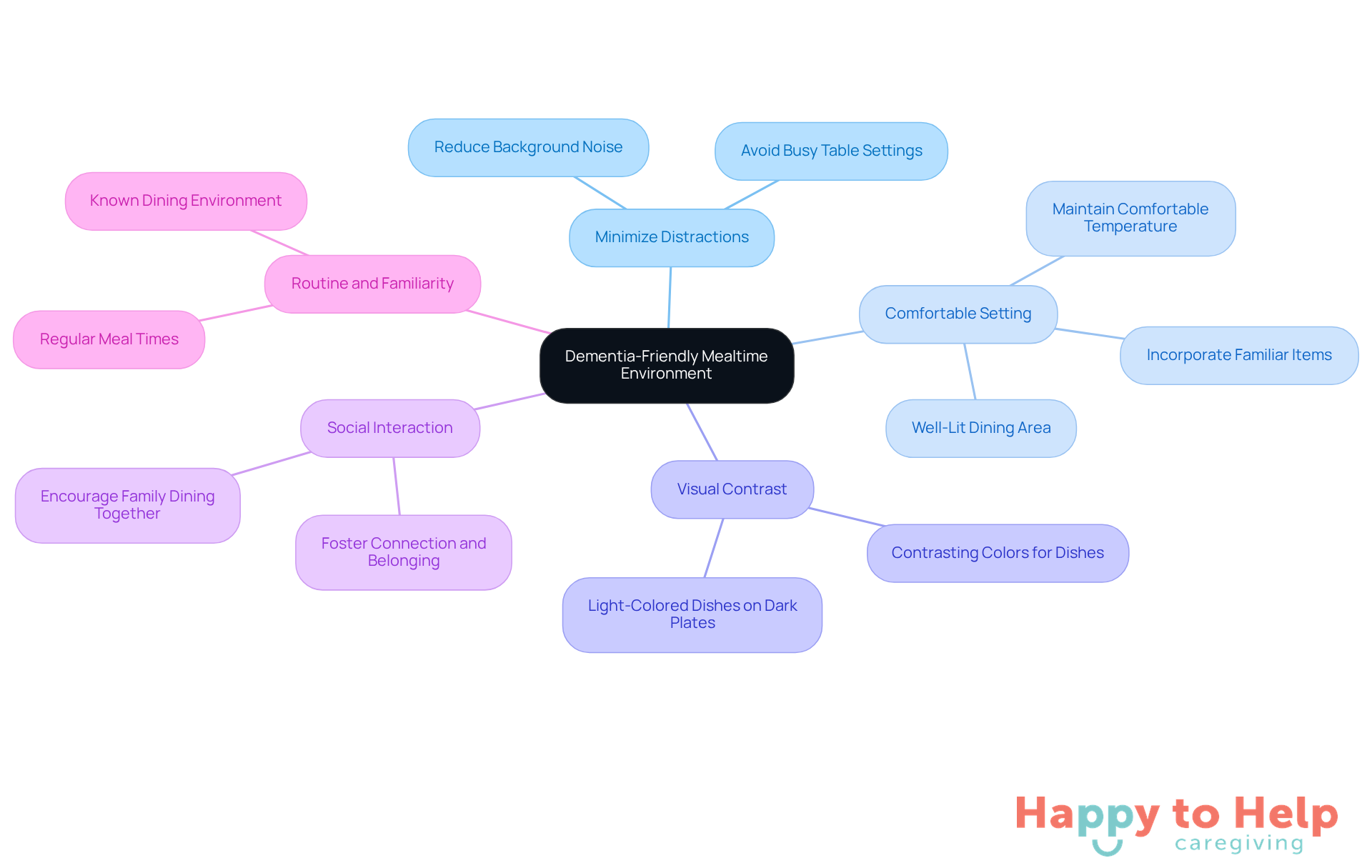
Creating a dementia-friendly mealtime environment presents a significant challenge for caregivers. Many individuals living with dementia and eating issues face difficulties related to nutrition, with approximately 50% experiencing these challenges within eight years of disease onset. This situation can lead to skipped meals, forgotten eating habits, and a general decline in nutritional health. Therefore, it’s crucial to implement strategies that can transform mealtimes into a more enjoyable and manageable experience.
-
Minimize Distractions: Reducing background noise and visual clutter is essential for helping individuals concentrate on their food. Turn off the television and avoid busy table settings to create a calm atmosphere.
-
Comfortable Setting: Ensure the dining area is well-lit and maintained at a comfortable temperature. Incorporating familiar items and decorations can provide additional comfort and reassurance.
-
Visual Contrast: Utilizing contrasting colors for dishes and items can enhance visual appeal and aid in identification. For example, presenting light-colored dishes on dark plates can make dining experiences more appealing and easier to identify.
-
Social Interaction: Encouraging family members or caregivers to dine together with the person can significantly enhance the mealtime experience. Social interaction not only stimulates appetite but also fosters a sense of connection and belonging.
-
Routine and Familiarity: Providing food at regular times daily in a known environment contributes to a feeling of safety and consistency, which is especially advantageous for people with dementia.
Implementing these strategies supports the nutritional needs and overall well-being of those facing dementia and eating issues. As one expert noted, "A person with dementia may skip food, forget how to eat or forget that they have already consumed," highlighting the importance of creating supportive environments.
Address Common Eating Challenges in Dementia Care
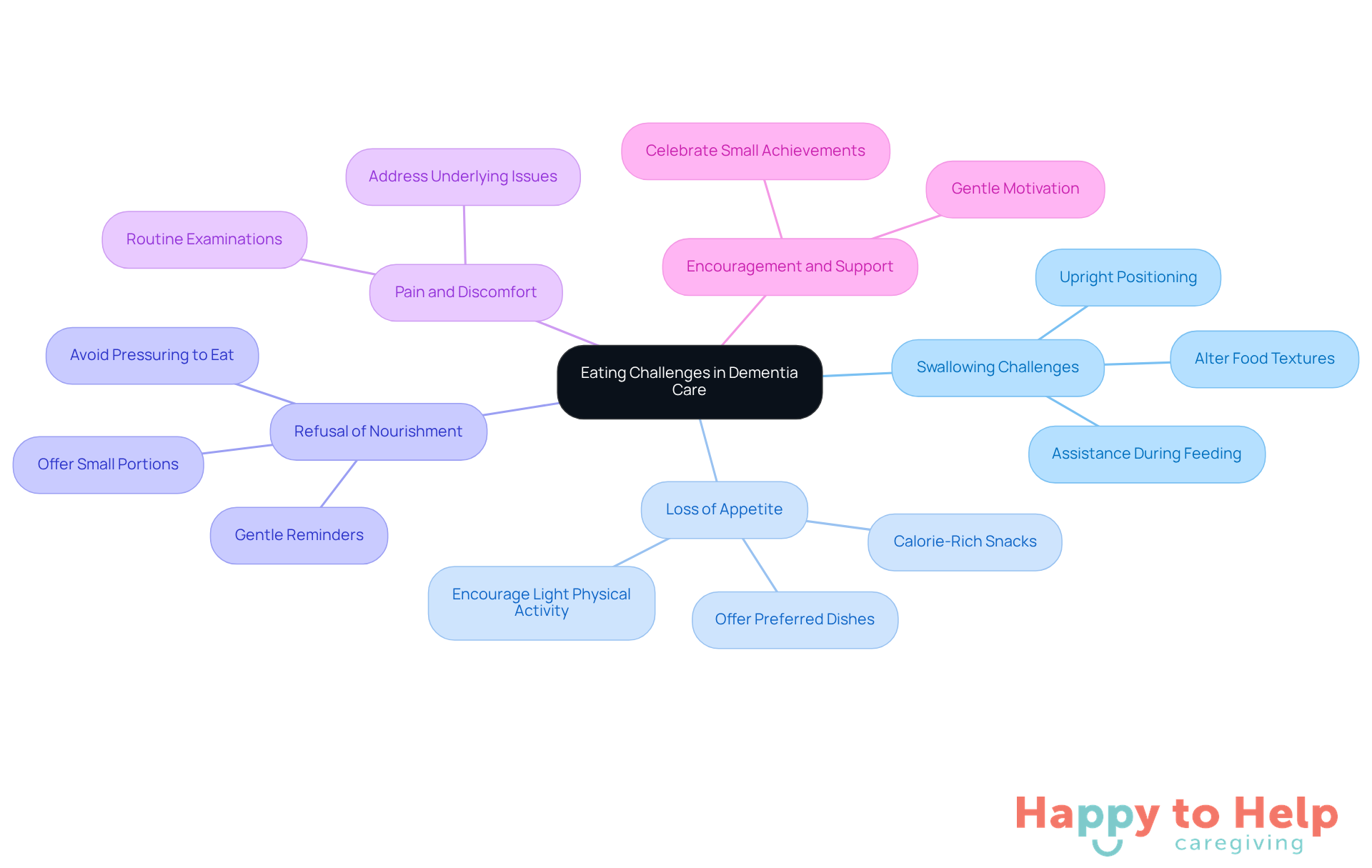
Common challenges related to dementia and eating issues in care include difficulty swallowing, loss of appetite, and refusal of meals. These dementia and eating issues can significantly impact the well-being of individuals with dementia and create stress for caregivers. Here are strategies to address these challenges:
-
Swallowing Challenges: For individuals experiencing dysphagia, consider altering the textures of foods, such as offering pureed dishes. Ensure they are positioned upright during meals. Research indicates that over 90% of people with dementia require some form of assistance during feeding, with 90.3% of caregivers observing similar needs. This underscores the importance of tailored support during mealtimes.
-
Loss of Appetite: If a decrease in appetite is noticeable, try offering preferred dishes or calorie-rich snacks between meals. Encouraging light physical activity can also help boost appetite, making it essential to involve individuals in gentle exercises.
-
Refusal of Nourishment: If the person declines food, avoid pressuring them to eat. Instead, offer small portions and allow them to eat at their own pace. Gentle reminders can be beneficial, and it’s crucial to refrain from offering food when the person is upset, as this may lead to further refusal.
-
Pain and Discomfort: Address any underlying pain or discomfort that may affect eating, such as dental issues or gastrointestinal problems. Routine examinations can help identify these issues, ensuring that the individual is comfortable during meals.
-
Encouragement and Support: Provide gentle motivation and assistance during dining, celebrating small achievements to foster a positive dining experience. As one caregiver noted, "Celebrating even the smallest victories can make a significant difference in motivation and enjoyment during meals."
By implementing these strategies, caregivers can better assist individuals facing dementia and eating issues, enhancing their dining experiences and overall well-being. Additionally, referencing case studies that discuss strategies to prevent overeating can offer real-life examples of effective management of eating challenges, further enhancing the practical application of these strategies.
Moving Forward with Tackle Dementia and Eating Issues:
Addressing the intersection of dementia and eating challenges is crucial for enhancing the quality of life for those affected. Caregivers face significant hurdles in ensuring that mealtimes are comforting rather than distressing. These challenges can lead to frustration and anxiety for both caregivers and individuals with dementia, making it essential to find effective strategies.
To tackle these issues, caregivers can implement thoughtful approaches tailored to the unique needs of individuals with dementia. Key strategies include:
- Establishing routines
- Simplifying choices
- Creating a supportive mealtime environment
- Engaging the senses
- Minimizing distractions
- Encouraging social interaction
These strategies can transform the dining experience, making it more enjoyable and less stressful.
Additionally, addressing specific challenges like swallowing difficulties and loss of appetite through personalized approaches can lead to more positive outcomes. By fostering a compassionate atmosphere during mealtimes, caregivers not only aid in nutrition but also strengthen emotional connections with those they support.
Caregivers are encouraged to embrace these strategies, as they enhance the dining experience and contribute to the overall well-being of individuals facing dementia. The journey may be challenging, but with the right tools and mindset, caregivers can make a meaningful difference in the lives of those they care for.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5MjBmZDc2N2I4YTJhOGJkNzc1MGJkYSIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
How does dementia affect eating behaviors?
Dementia can lead to various eating challenges, including forgetfulness about mealtimes, decreased appetite, and confusion over dietary preferences. Individuals may forget if they’ve eaten or struggle to recognize familiar foods.
What sensory changes might occur in individuals with dementia that affect their eating?
Individuals with dementia may experience shifts in taste and smell, making once-loved meals unappealing, which can further complicate their eating habits.
What signs should caregivers look for that indicate discomfort during meals?
Caregivers should be vigilant for signs of discomfort, as these can worsen the eating experience and may include expressions of distress or refusal to eat.
What strategies can caregivers implement to improve mealtime experiences for individuals with dementia?
Caregivers can establish a routine with consistent mealtimes, simplify choices by offering a limited selection of familiar foods, and engage the senses by presenting meals attractively while considering individual sensory preferences.
Why is it important for caregivers to approach mealtimes with empathy?
A compassionate approach to mealtimes improves the dining experience and fosters a sense of security and comfort for individuals navigating the complexities of dementia.
List of Sources
- Understand the Impact of Dementia on Eating Behaviors
- 4 Inspiring Quotes for Caring for a Loved One With Alzheimer’s | myALZteam (https://myalzteam.com/resources/inspiring-quotes-for-caring-for-a-loved-one-with-alzheimers)
- Caregiver Dementia Quotes (Encouragement For Dementia Caregivers) (https://optoceutics.com/caregiver-dementia-quotes-encouragement-dementia-caregivers?srsltid=AfmBOopgCfSAXMTmWb07FZbpKaYGW\_9UN7Ah64a4o3Z4kFD7bVz\_Hb3i)
- CaringBridge (https://caringbridge.org/resources/inspirational-quotes-on-caregiving)
- (https://belleviecare.co.uk/support-advice/dementia-quotes-to-lift-your-spirits)
- 27 Inspirational Quotes for Caregivers (https://ultimatecareny.com/resources/27-quotes-for-caregivers)
- Implement Strategies to Encourage Healthy Eating
- Meal time (https://alzheimer.ca/en/help-information/im-caring-person-living-dementia/providing-day-day-care/meal-time)
- 7 Caretaker Tips for Getting Dementia Patients to Eat (https://verywellhealth.com/how-to-get-dementia-patients-to-eat-11711215)
- Eating and dementia (https://dementia.org.au/living-dementia/home-life/eating-and-dementia)
- Create a Dementia-Friendly Mealtime Environment
- (https://belleviecare.co.uk/support-advice/dementia-quotes-to-lift-your-spirits)
- 7 Caretaker Tips for Getting Dementia Patients to Eat (https://verywellhealth.com/how-to-get-dementia-patients-to-eat-11711215)
- Meal time (https://alzheimer.ca/en/help-information/im-caring-person-living-dementia/providing-day-day-care/meal-time)
- Caregiver Experiences with Dementia-Related Feeding/Eating Difficulties - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10815734)
- Address Common Eating Challenges in Dementia Care
- Dunblane dementia friendly group brings hope and friendship during COVID-19 - Health and Social Care Alliance Scotland (https://alliance-scotland.org.uk/blog/case\_studies/dunblane-dementia-friendly-group-brings-hope-and-friendship-during-covid-19)
- Caregiver Experiences with Dementia-Related Feeding/Eating Difficulties - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10815734)
- Appetite and dementia (https://alzheimers.org.uk/get-support/living-with-dementia/poor-appetite-dementia)
- Development and Implementation of an Anticipatory Care Calendar for people with learning disabilities or dementia - Quality in Care Awards Programme (https://qualityincare.org/case\_studies/development\_and\_implementation\_of\_an\_anticipatory\_care\_calendar\_for\_people\_with\_learning\_disabilities\_or\_dementia)

