
Why Dehydration in Seniors: Risks and Matters
Understanding the complexities of hydration is crucial, especially as individuals age. Dehydration presents a significant risk for seniors - often overlooked yet capable of leading to serious health complications.
This article delves into the underlying factors contributing to dehydration in older adults. Caregivers play a vital role in ensuring their loved ones maintain optimal hydration levels. So, how can caregivers effectively combat this silent threat and promote better health outcomes for seniors?
The Problem
Dehydration is a common issue among older adults, often exacerbated by factors such as reduced thirst sensation, certain medications, and health conditions.
The Implications
The consequences of dehydration can be severe, leading to confusion, urinary tract infections, and even hospitalization. It’s essential for caregivers to recognize these risks and take proactive measures.
The Solution
Here are some actionable strategies caregivers can implement:
- Encourage regular fluid intake: Remind seniors to drink water throughout the day, even if they don’t feel thirsty.
- Incorporate hydrating foods: Include fruits and vegetables with high water content in their diet, such as cucumbers, oranges, and watermelon.
- Monitor fluid loss: Keep an eye on signs of dehydration, such as dry mouth or decreased urine output.
By understanding the complexities of hydration and taking these steps, caregivers can help ensure that their loved ones stay healthy and hydrated.
Define Dehydration and Its Impact on Seniors
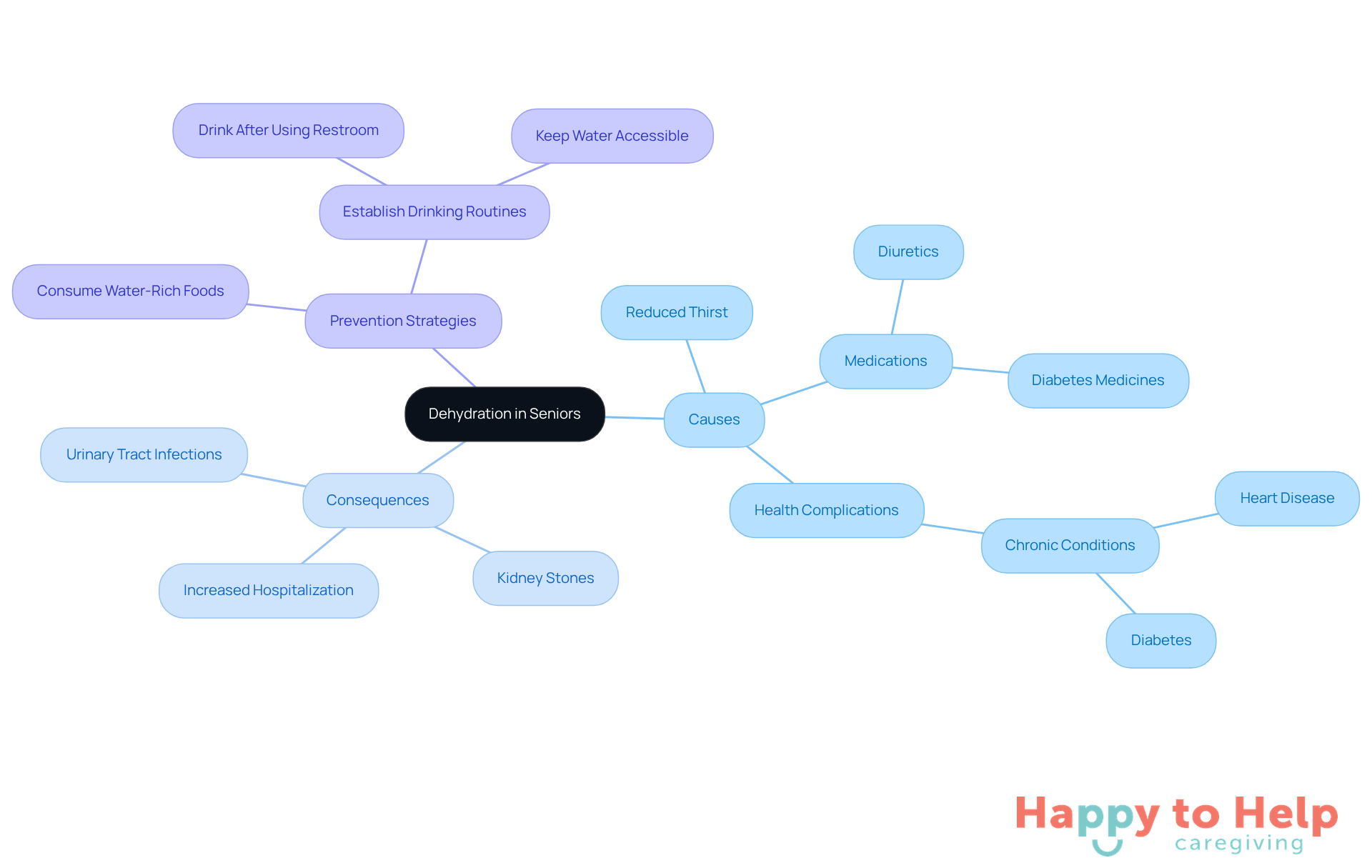
Dehydration seniors face is a significant issue, occurring when the body loses more moisture than it takes in. This imbalance can lead to serious health complications, including dry mouth, fatigue, and confusion. The challenge of dehydration in seniors is compounded by the reduced sense of thirst that often accompanies aging, making it difficult for them to recognize their need for fluids.
Studies indicate that up to 40% of seniors experience dehydration, which can result in severe health problems like urinary tract infections, kidney stones, and increased hospitalization rates. For instance, a meta-analysis found that 24% of older adults are dehydrated, with even higher rates among those in long-term care facilities. Additionally, common medications, such as diuretics, can exacerbate fluid loss, thereby increasing the risk of dehydration.
The consequences of dehydration extend beyond immediate discomfort; they can worsen existing health conditions and significantly impact overall health outcomes. To combat this issue, caregivers should encourage seniors to:
- Consume water-rich foods
- Establish regular drinking routines, such as having a glass of water after using the restroom
Monitoring hydration levels is essential to prevent serious health consequences and address dehydration seniors may experience, promoting their overall well-being. By implementing these strategies, caregivers can help ensure that older adults maintain adequate hydration and support their overall health.
Explore the Increased Risks of Dehydration in Older Adults
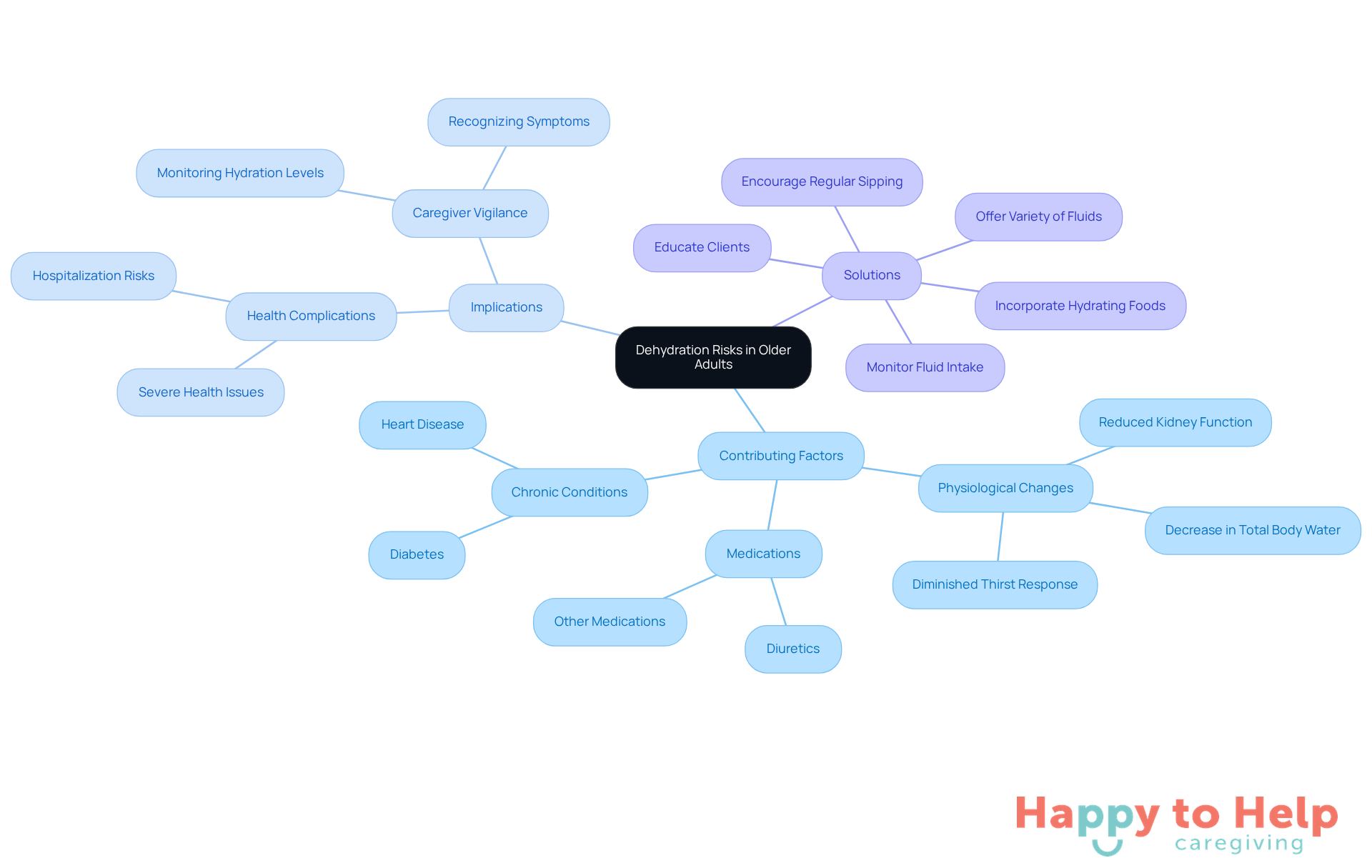
Older individuals are at significant risk of dehydration due to several factors. The problem lies in physiological changes that occur with aging, such as a decrease in total body water, reduced kidney function, and a diminished thirst response. Additionally, many seniors take medications like diuretics that can exacerbate dehydration. Chronic conditions, including diabetes and heart disease, further increase these risks.
The implications of these changes are serious. Caregivers must be vigilant, as dehydration can lead to severe health complications. Understanding these factors is crucial for monitoring hydration levels effectively.
The solution involves proactive measures. Caregivers should regularly assess hydration status and encourage fluid intake. Here are some actionable tips:
- Monitor daily fluid intake and output.
- Offer a variety of fluids to make hydration more appealing.
- Educate clients about the importance of staying hydrated.
By recognizing the challenges and implementing these strategies, caregivers can better support the hydration needs of seniors, preventing dehydration.
Examine Age-Related Changes in Water Balance Regulation
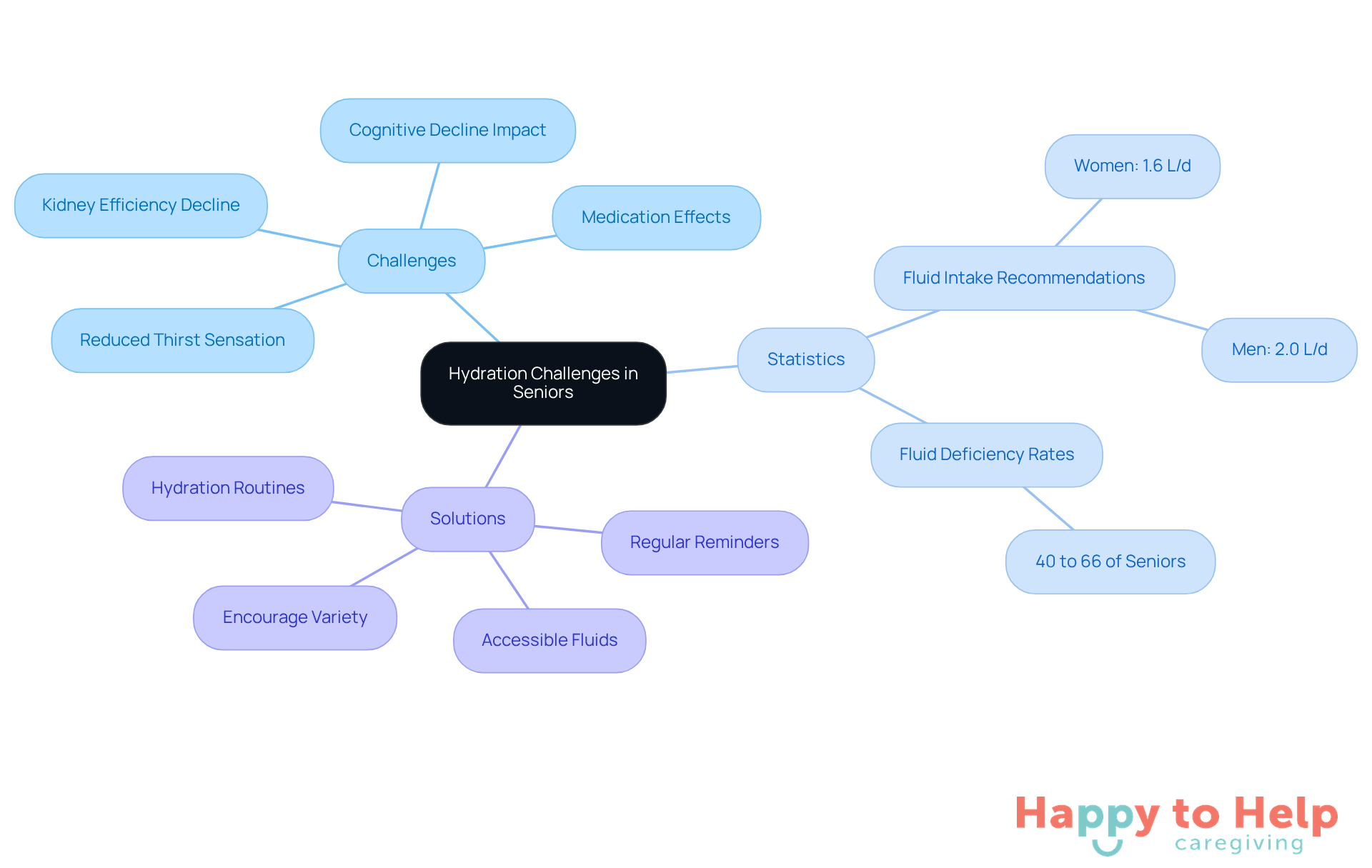
As individuals age, they face significant challenges in maintaining proper hydration. The efficiency of their kidneys in conserving water declines, and the hormonal responses that trigger thirst become less effective. This means that dehydration seniors may not recognize their need for hydration, even when their bodies signal dehydration. Alarmingly, studies indicate that healthy seniors report feeling less thirsty after periods without water compared to younger individuals.
This reduced thirst sensation can lead to serious consequences. The capacity to eliminate excess water diminishes, which may result in fluid overload in certain situations. According to the European Food Safety Authority, senior women should aim for at least 1.6 liters and senior men at least 2.0 liters of fluids daily to stay hydrated. Yet, fluid deficiency among seniors varies from 40% to 66%, highlighting the urgency of this issue. Expert Anne Vanderbilt notes, "By the time a senior experiences thirst, that’s already a sign of early dehydration."
To address these challenges, caregivers must adopt a proactive approach to hydration. Here are some practical solutions:
- Regular Reminders: Set up a schedule for hydration breaks throughout the day.
- Accessible Fluids: Ensure that water and other fluids are readily available.
- Encourage Variety: Offer a range of beverages, including flavored water, to make hydration more appealing.
Understanding these challenges is crucial for caregivers and families. By providing support and reminders, they can help older adults maintain adequate fluid intake and prevent dehydration.
Implement Effective Strategies to Prevent Dehydration
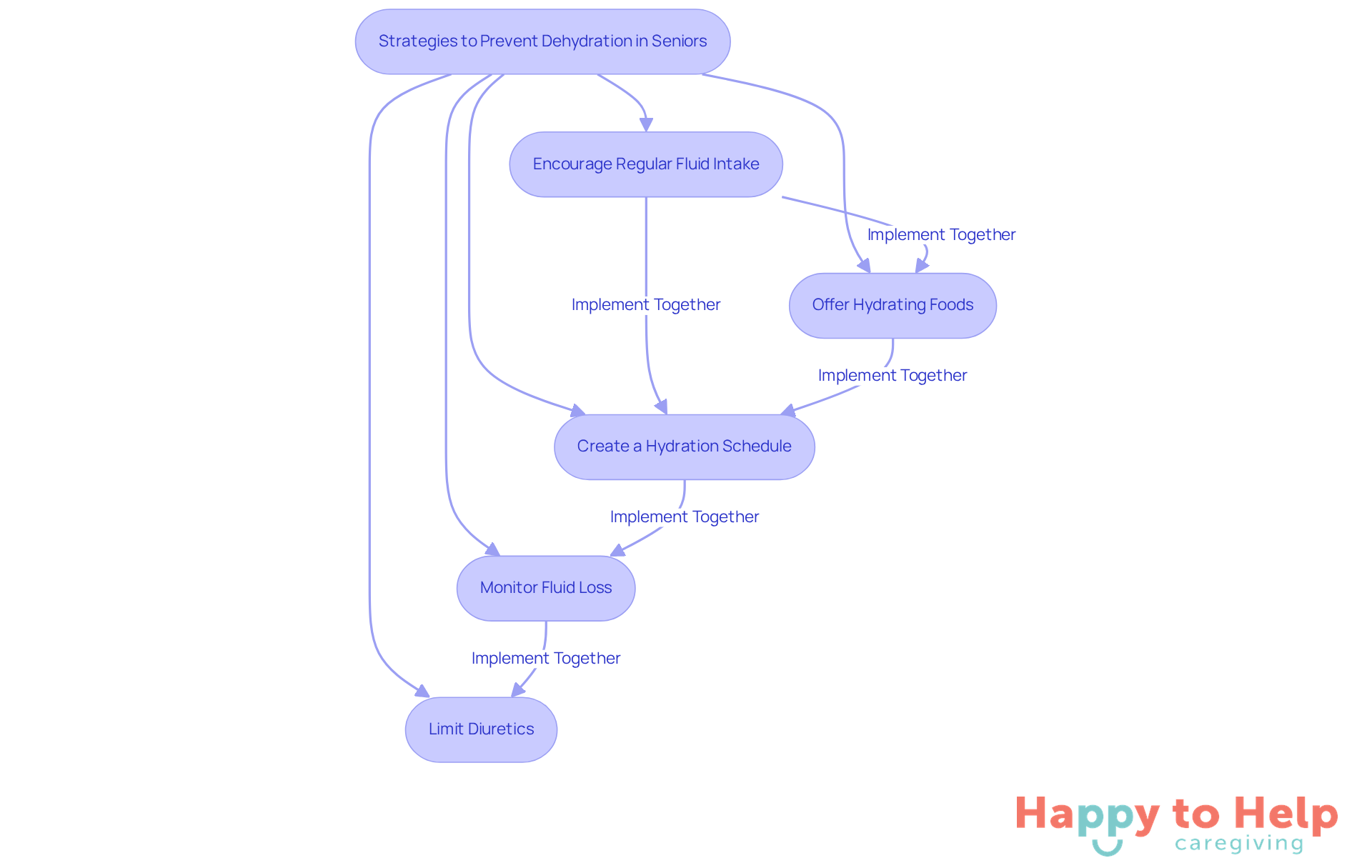
To effectively prevent dehydration seniors, caregivers face a significant challenge. Older adults often have diminished thirst perception and fewer water reserves, making them more susceptible to dehydration seniors. This can lead to serious health complications, including confusion and fatigue. Therefore, it’s crucial for caregivers to prioritize hydration.
-
Encourage Regular Fluid Intake: Aim for a daily fluid intake of 13 cups for men and 9 cups for women, adjusting based on individual activity levels and environmental conditions. Regular reminders can help ensure seniors meet their hydration needs.
-
Offer Hydrating Foods: Incorporate fruits and vegetables with high water content, such as watermelon, cucumbers, and oranges, into meals and snacks. These foods can significantly boost hydration levels.
-
Create a Hydration Schedule: Establish a routine by setting reminders for seniors to drink water throughout the day, especially during meals and after taking medications. Using phone alarms or written notes can effectively prompt regular hydration.
-
Monitor Fluid Loss: Stay alert for signs of dehydration, including dry mouth, headaches, dark urine, fatigue, and confusion. Taking immediate action if these symptoms arise is essential for maintaining health.
-
Limit Diuretics: Consult with healthcare providers about minimizing medications that may lead to increased moisture loss. Discuss specific medications that could affect fluid balance to ensure hydration is prioritized.
By implementing these strategies, caregivers can significantly enhance the hydration and overall health of seniors, which helps in reducing the risk of dehydration seniors-related complications.
Key Takeaways for Caregivers
Dehydration in seniors is a significant health concern that requires immediate attention. Older adults often face diminished thirst perception and physiological changes that make it difficult to stay properly hydrated. This places a heavy burden on caregivers, who must ensure that seniors receive adequate fluids to maintain their health and well-being.
Statistics reveal alarming dehydration rates among older adults, highlighting the urgent need for action. Factors such as medications and the natural aging process contribute to this risk, making it essential for caregivers to adopt a comprehensive approach.
- Monitoring hydration levels
- Establishing regular drinking routines
- Including hydrating foods in seniors' diets
are effective strategies to combat dehydration.
Ultimately, the responsibility for preventing dehydration falls on caregivers and family members. By recognizing the signs of dehydration and implementing effective hydration strategies, caregivers can significantly improve the health and quality of life for seniors. Prioritizing hydration not only protects against immediate health issues but also supports long-term well-being, making it crucial to focus on these efforts in the care of older adults.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5Mjc5NGU5MTE3NGVkN2UzNDc1ZmU1MCIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What is dehydration and how does it affect seniors?
Dehydration occurs when the body loses more moisture than it takes in, leading to serious health complications such as dry mouth, fatigue, and confusion. In seniors, dehydration is especially concerning due to a reduced sense of thirst, making it difficult for them to recognize their need for fluids.
How common is dehydration among seniors?
Studies indicate that up to 40% of seniors experience dehydration. A meta-analysis found that 24% of older adults are dehydrated, with even higher rates among those in long-term care facilities.
What are the potential health complications associated with dehydration in seniors?
Dehydration can lead to severe health problems such as urinary tract infections, kidney stones, and increased hospitalization rates. It can also worsen existing health conditions and significantly impact overall health outcomes.
What factors contribute to dehydration in older adults?
Contributing factors include a reduced sense of thirst that often accompanies aging, as well as the effects of common medications, such as diuretics, which can exacerbate fluid loss.
What strategies can caregivers implement to help prevent dehydration in seniors?
Caregivers can encourage seniors to consume water-rich foods and establish regular drinking routines, such as having a glass of water after using the restroom.
Why is monitoring hydration levels important for seniors?
Monitoring hydration levels is essential to prevent serious health consequences and address dehydration, promoting overall well-being in older adults.
List of Sources
- Define Dehydration and Its Impact on Seniors
- Dehydration in middle-aged and older adults may lead to attention challenges | Penn State University (https://psu.edu/news/health-and-human-development/story/dehydration-middle-aged-and-older-adults-may-lead-attention)
- Trends in Dehydration in Older People: Identifying Landmark Scientific Contributions (https://mdpi.com/2072-6643/17/2/204)
- Hydration and older adults: Why water matters more as you age (https://uclahealth.org/news/article/hydration-and-older-adults-why-water-matters-more-you-age)
- Explore the Increased Risks of Dehydration in Older Adults
- The Connection Between Age and Dehydration Risk (https://health.clevelandclinic.org/drink-up-dehydration-is-an-often-overlooked-health-risk-for-seniors)
- Hydration and older adults: Why water matters more as you age (https://uclahealth.org/news/article/hydration-and-older-adults-why-water-matters-more-you-age)
- Why Should Older Adults Stay Hydrated? (https://ncoa.org/article/10-reasons-why-hydration-is-important)
- Study finds a lack of adequate hydration among the elderly (https://newsroom.ucla.edu/releases/study-finds-a-lack-of-adequate-hydration-among-the-elderly)
- Examine Age-Related Changes in Water Balance Regulation
- What Older Adults Need to Know About Hydration (https://health.usnews.com/health-care/patient-advice/articles/what-older-adults-need-to-know-about-hydration)
- The Connection Between Age and Dehydration Risk (https://health.clevelandclinic.org/drink-up-dehydration-is-an-often-overlooked-health-risk-for-seniors)
- Hydration and older adults: Why water matters more as you age (https://uclahealth.org/news/article/hydration-and-older-adults-why-water-matters-more-you-age)
- Hydration Status in Older Adults: Current Knowledge and Future Challenges - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10255140)
- Link between hydration and aging (https://nih.gov/news-events/nih-research-matters/link-between-hydration-aging)
- Implement Effective Strategies to Prevent Dehydration
- Seniors Should Boost Their Water Intake; Here Are 6 Ways (https://morningstarseniorliving.com/seniors-should-boost-their-water-intake-here-are-6-ways)
- Hydration and older adults: Why water matters more as you age (https://uclahealth.org/news/article/hydration-and-older-adults-why-water-matters-more-you-age)
- 4 Hydration Tips for Older Adults | Home Health Care (https://phoenixhomehc.com/news/hydration-tips-for-older-adults)
- How Older Adults Can Avoid Dehydration (https://umms.org/bwmc/news/2021/how-older-adults-can-avoid-dehydration)
- Fast Facts: Data on Water Consumption (https://cdc.gov/nutrition/php/data-research/fast-facts-water-consumption.html)

