
The Importance of Dementia Patient Seeing Things: Causes
Understanding the complexities of dementia can be daunting, particularly when it comes to the distressing phenomenon of hallucinations. Caregivers often face the challenge of a loved one seeing things that aren't there, which can evoke a whirlwind of emotions. This situation not only affects the individual experiencing the hallucinations but also significantly impacts the emotional well-being of caregivers.
Navigating this challenging terrain requires a grasp of the underlying causes and effective coping strategies. How can caregivers ensure their own emotional health while supporting their loved ones? This article delves into the intricacies of hallucinations in dementia patients, offering insights and practical approaches to foster a supportive environment amidst the confusion.
Key Points to Consider:
- Recognize the Problem: Hallucinations can lead to distress for both patients and caregivers.
- Understand the Implications: The emotional toll on caregivers can be significant, affecting their ability to provide care.
- Explore Solutions: Implementing coping strategies can help manage the situation effectively.
Define Hallucinations in Dementia
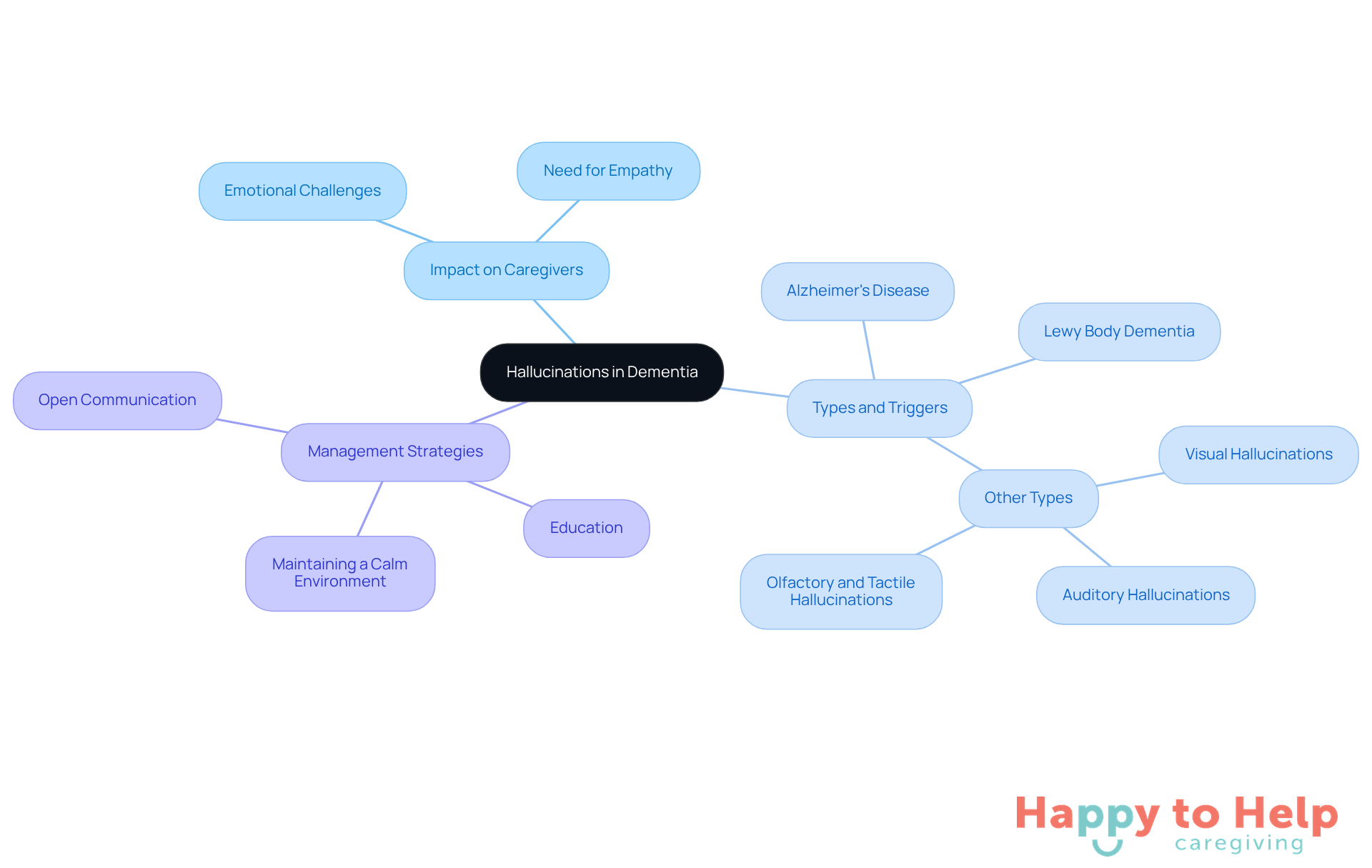
Hallucinations in cognitive decline present a significant challenge for caregivers. These sensory experiences can result in a dementia patient seeing things that aren't present, such as nonexistent people or hearing voices that aren't there. This issue is particularly prevalent in conditions like Lewy body dementia and Alzheimer's disease, especially in a dementia patient seeing things.
Understanding these hallucinations is crucial for caregivers. They not only affect the individual experiencing them but also impact the emotional landscape of caregiving. Caregivers must recognize that these experiences can evoke strong emotions, making it essential to respond with empathy and support.
To effectively manage these situations, caregivers can implement several strategies:
- Educate themselves about the types of hallucinations and their triggers.
- Maintain a calm environment to help reduce anxiety for the individual.
- Engage in open communication, reassuring the person that they are safe and supported.
By acknowledging the reality of hallucinations and responding appropriately, caregivers can significantly improve the quality of care and emotional well-being for those experiencing cognitive decline.
Identify Causes of Hallucinations
The challenges faced by individuals and their caregivers significantly increase when a dementia patient is seeing things due to cognitive decline. These disturbances can arise from various factors, complicating the caregiving experience. Understanding these factors is crucial for developing effective coping strategies and providing compassionate care for a dementia patient seeing things.
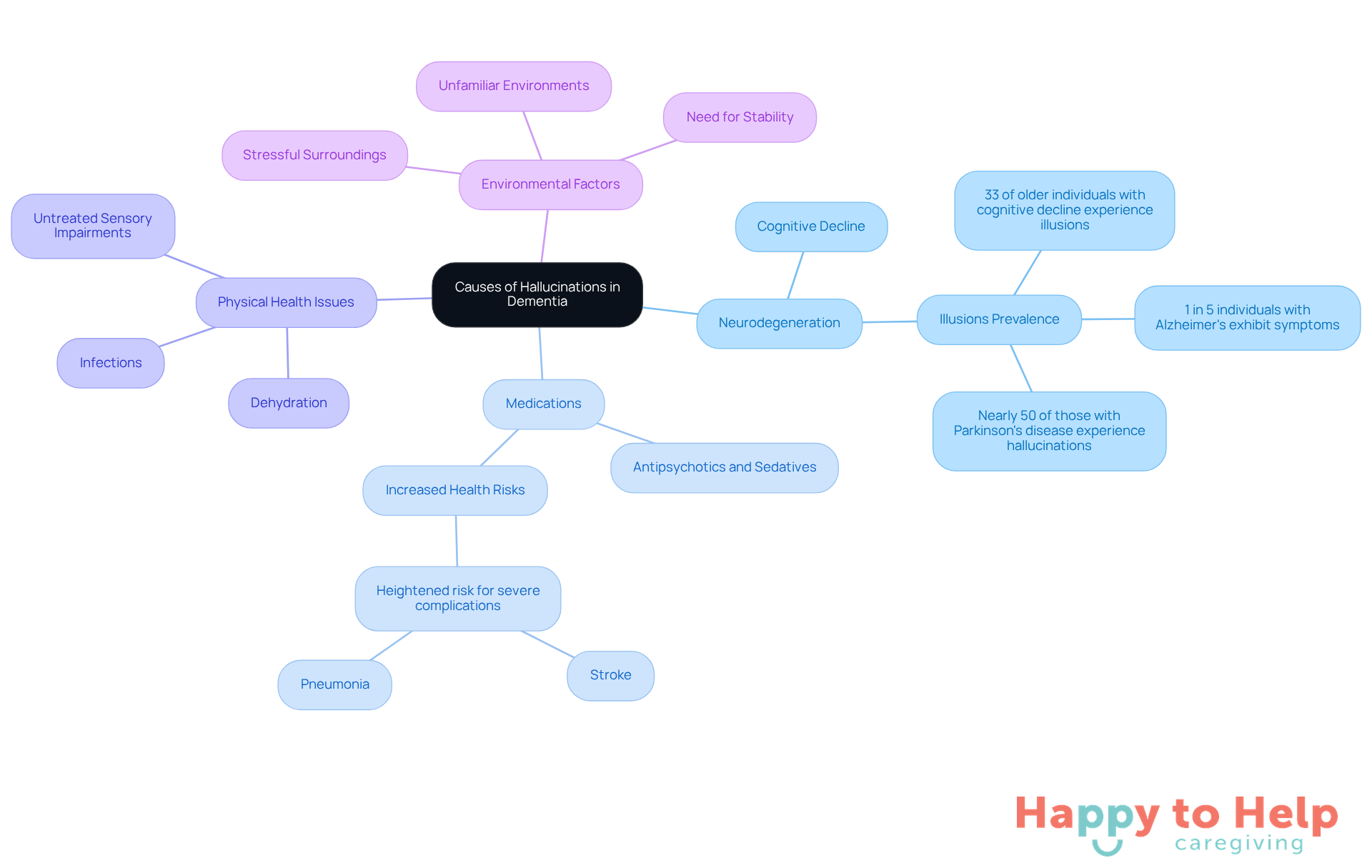
Problem: Neurodegeneration is a primary contributor. Structural and functional changes in the brain associated with dementia can lead to a dementia patient seeing things in a way that misinterprets sensory information. Studies indicate that around 33% of older individuals with cognitive decline experience illusions. Alarmingly, one in five individuals with Alzheimer's and nearly half of those with Parkinson's disease also exhibit symptoms, such as a dementia patient seeing things, highlighting the widespread nature of this concern.
Agitate: Medications can exacerbate these issues. Certain drugs, particularly antipsychotics and sedatives, may result in a dementia patient seeing things as visual or auditory distortions among their side effects. Research shows that newly prescribed antipsychotic patients with cognitive impairment face a heightened risk for severe health complications, including stroke and pneumonia. As Angela Taylor emphasizes, there is a pressing need for better treatment and management strategies for those experiencing perceptual disturbances, such as a dementia patient seeing things, to improve their lives.
Solution: Caregivers must also consider physical health issues. Conditions like dehydration, infections, or untreated sensory impairments can worsen distorted perceptions. Vigilance in monitoring the overall health of loved ones is essential, particularly when a dementia patient is seeing things, to mitigate these risks.
Environmental factors play a role too. In stressful or unfamiliar surroundings, a dementia patient seeing things may experience distorted perceptions. Creating a stable and comforting atmosphere is crucial. Caregivers should strive to maintain a sense of familiarity, as this can significantly impact the well-being of individuals experiencing cognitive decline.
By addressing these elements, caregivers can help reduce the discomfort linked to sensory disturbances and enhance the quality of life for those affected.
Implement Coping Strategies for Caregivers
Caregivers face significant challenges when managing situations involving a dementia patient seeing things. These episodes can lead to increased stress and feelings of frustration, not only for the caregivers of a dementia patient seeing things but also for the individuals experiencing them. Statistics reveal that caregivers often report stress levels three times greater than those caring for individuals without dementia, highlighting the emotional toll of these experiences.
To effectively manage these challenges, caregivers can implement several strategies:
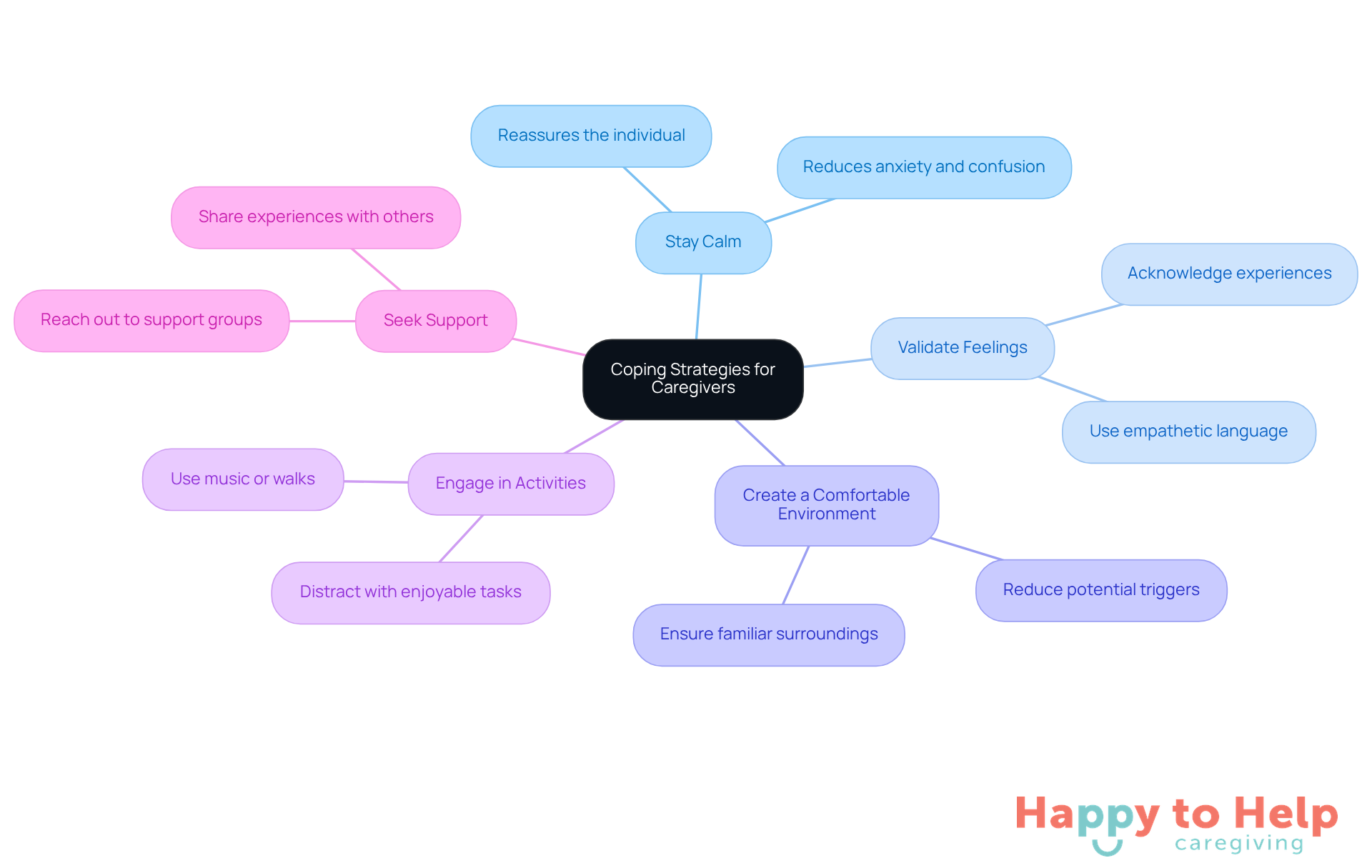
- Stay Calm: Maintaining a calm demeanor during hallucinations is crucial. This approach reassures the individual with dementia, helping to reduce their anxiety and confusion.
- Validate Feelings: Acknowledge the person's feelings without disputing their experiences. For instance, if a dementia patient is seeing things and perceives someone who isn't present, you might say, 'I understand that as a dementia patient seeing things, that must be confusing for you.' This validation can help them feel heard and understood.
- Create a Comfortable Environment: Ensure that the surroundings are calm and familiar, which can help reduce potential triggers for altered perceptions. A soothing environment can significantly reduce the frequency and intensity of these episodes.
- Engage in Activities: Distracting the individual with enjoyable activities, such as listening to music or going for a walk, can redirect their focus and alleviate distress caused by perceptual disturbances.
- Seek Support: Caregivers should not hesitate to reach out for help from support groups or mental health professionals. Sharing experiences and coping strategies with others can provide valuable insights and emotional relief.
Furthermore, the economic strain linked to dementia-related psychosis (DRP) is considerable. Individuals experiencing DRP face healthcare expenses that are notably greater than those of dementia-only individuals. By employing these strategies, caregivers can foster a more supportive atmosphere for both themselves and the individuals they assist, ultimately enhancing the quality of life for everyone involved.
Consult Healthcare Professionals for Support
When episodes of altered perception occur in dementia patients seeing things and become frequent or distressing, caregivers face a significant challenge. It’s crucial to seek guidance from healthcare professionals to ensure the best care for their loved ones.
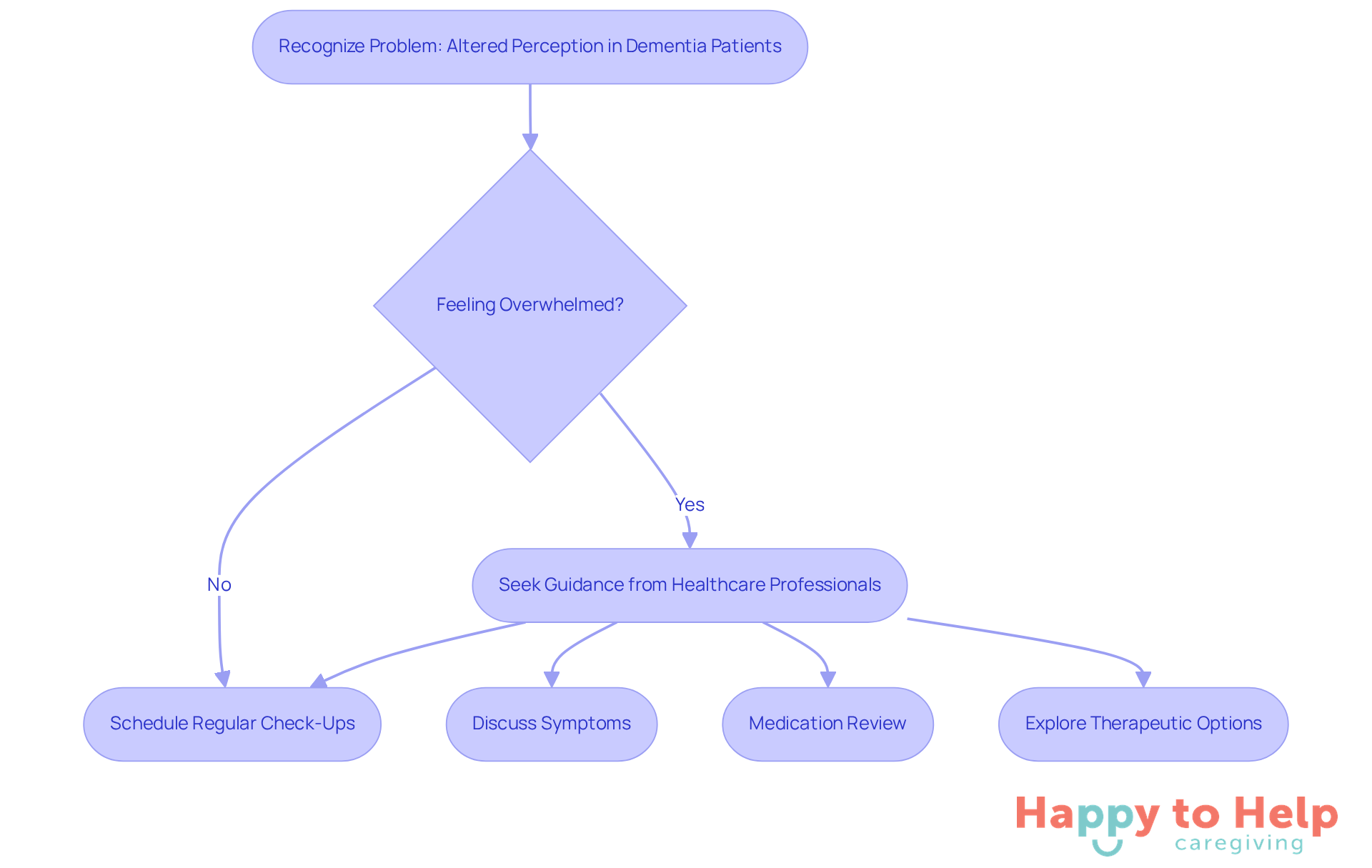
Problem: Many caregivers may feel overwhelmed by the behavioral changes and symptoms that arise in dementia patients. This can lead to increased stress and uncertainty about how to manage these situations effectively.
Agitate: Notably, only 16 percent of seniors report receiving regular assessments for memory or thinking issues. This statistic highlights a critical gap in care, emphasizing the importance of proactive measures to monitor symptoms and evaluate medication effects.
Solution: Here are essential steps caregivers can take:
- Schedule Regular Check-Ups: Consistent appointments with healthcare providers are vital for monitoring symptoms and evaluating the effects of medications. Regular assessments can significantly enhance the quality of care and ensure timely interventions.
- Discuss Symptoms: Caregivers should communicate any behavioral changes or new symptoms to the healthcare provider. This information is critical for accurate diagnosis and effective treatment planning.
- Medication Review: Request a thorough assessment of current medications from the healthcare provider to identify any that may contribute to a dementia patient seeing things. Adjustments to medication regimens may be necessary to alleviate symptoms.
- Explore Therapeutic Options: Inquire about non-pharmacological interventions, such as cognitive behavioral therapy or environmental modifications, which can be effective in managing hallucinations. These approaches can offer extra assistance and enhance the overall well-being of the individual. Additionally, utilizing resources like the Dementia Care Planning Toolkit can assist caregivers in creating personalized care plans that evolve with the patient's needs.
Your Path Forward
Understanding the complexities of hallucinations in dementia patients is crucial for effective care and support. These sensory experiences - seeing or hearing things that aren't there - create significant challenges for both patients and their caregivers. By recognizing the nature and causes of these hallucinations, caregivers can better navigate the emotional and practical hurdles they encounter.
Hallucinations often stem from factors like neurodegeneration, medication side effects, and environmental influences. This highlights the need for education and awareness. Caregivers should maintain a calm and familiar environment while validating the feelings of those affected. Implementing effective coping strategies, such as engaging in comforting activities and seeking support from healthcare professionals, can greatly enhance the quality of life for both caregivers and patients.
Addressing hallucinations in dementia patients requires a compassionate and proactive approach. Caregivers must remain vigilant about their loved ones' health and well-being, seek professional guidance when necessary, and utilize available resources. By fostering a supportive atmosphere and equipping themselves with knowledge and strategies, caregivers can navigate the challenges of dementia with greater confidence and effectiveness, ultimately improving the lives of those they care for.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5M2Y1MDk5Njk1NDdlMzRlNWE0ZWU2ZCIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What are hallucinations in dementia?
Hallucinations in dementia are sensory experiences where a patient perceives things that aren't present, such as seeing nonexistent people or hearing voices that aren't there.
In which types of dementia are hallucinations particularly common?
Hallucinations are particularly prevalent in conditions like Lewy body dementia and Alzheimer's disease.
Why is it important for caregivers to understand hallucinations in dementia?
Understanding hallucinations is crucial for caregivers because they not only affect the individual experiencing them but also impact the emotional landscape of caregiving.
How can hallucinations affect caregivers?
Hallucinations can evoke strong emotions in dementia patients, making it essential for caregivers to respond with empathy and support.
What strategies can caregivers use to manage hallucinations in dementia patients?
Caregivers can manage hallucinations by educating themselves about the types and triggers of hallucinations, maintaining a calm environment, and engaging in open communication to reassure the individual that they are safe and supported.
How can acknowledging hallucinations improve care for dementia patients?
By acknowledging the reality of hallucinations and responding appropriately, caregivers can significantly improve the quality of care and emotional well-being for those experiencing cognitive decline.
List of Sources
- Define Hallucinations in Dementia
- Understanding Hallucinations in Dementia - Penn Memory Center (https://pennmemorycenter.org/understanding-hallucinations-in-dementia)
- Medicare claims data underestimate hallucinations in older adults with dementia - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC8816965)
- Coping with hallucinations in a person with dementia (https://dementiauk.org/news/coping-with-hallucinations-in-a-person-with-dementia)
- Anti-sickness drug being trialled for dementia-related hallucinations (https://ucl.ac.uk/news/2022/aug/anti-sickness-drug-being-trialled-dementia-related-hallucinations)
- Incidence of and risk factors for hallucinations and delusions in patients with probable AD | Neurology (https://neurology.org/doi/10.1212/WNL.54.10.1965)
- Identify Causes of Hallucinations
- Survey Shows Significant Burden of Visual Hallucinations and Paranoid Delusions for People With Dementia (https://practicalneurology.com/news/survey-shows-significant-burden-of-visual-hallucinations-and-paranoid-delusions-for-people-with-dementia/2469337)
- Medicare claims data underestimate hallucinations in older adults with dementia - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC8816965)
- Antipsychotics for dementia linked to more harms than previously acknowledged - Alzheimer's Research UK (https://alzheimersresearchuk.org/news/antipsychotics-for-dementia-linked-to-more-harms-than-previously-acknowledged)
- People with Dementia and Caregivers Share the Significant Burden of Visual Hallucinations and Paranoid Delusions, New Survey Highlights (https://acadia.com/en-us/media/news-releases/people-dementia-and-caregivers-share-significant-burden-visual)
- 17 Quotes About Living with Schizophrenia (https://psychcentral.com/schizophrenia/quotes-on-living-with-schizophrenia)
- Implement Coping Strategies for Caregivers
- Coping and adaptation to dementia family caregiving: A pilot study (https://sciencedirect.com/science/article/abs/pii/S0197457220302524)
- Burden of illness among patients with dementia-related psychosis - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10391020)
- Coping with hallucinations in a person with dementia (https://dementiauk.org/news/coping-with-hallucinations-in-a-person-with-dementia)
- Dementia Related Psychosis: Four Caregiver Facts You Need to Know - The San Fernando Valley Sun (https://sanfernandosun.com/2020/11/29/dementia-related-psychosis-four-caregiver-facts-you-need-to-know)
- Consult Healthcare Professionals for Support
- The Importance of Patient-Centered Care for People Living with Dementia and Their Caregivers (https://forhealthconsulting.umassmed.edu/the-importance-of-patient-centered-care-for-people-living-with-dementia-and-their-caregivers)
- New Alzheimer's Association Report Shows Significant Disconnect Between Seniors, Physicians When It Comes to Cognitive Assessment (https://alz.org/news/2019/new-alzheimer-s-association-report-shows-significant-disconnect-between-seniors-physicians-when)
- Bridging Gaps in Dementia Care: PAs as Champions of Early Detection and Support Bridging Gaps in Dementia Care: PAs as Champions of Early Detection and Support (https://aapa.org/news-central/2025/11/bridging-gaps-in-dementia-care-pas-as-champions-of-early-detection-and-support)
- Value-based care model GUIDEs a future for dementia care for senior living (https://mcknightsseniorliving.com/news/value-based-care-model-guides-a-future-for-dementia-care-for-senior-living)
- The Importance of Regular Check-ups: | SJPP (https://sjpp.org/news/the-importance-of-regular-check-ups)

