
For families in our service areas
For families in our service areas, this guide explains dementia care and how non-medical in-home caregiving can support care planning in East Idaho, Treasure Valley & Magic Valley, Northern Wasatch, North Central West Virginia, and Northeast Ohio.
Understanding Your Options
Hallucinations can be a distressing experience for elderly individuals, even those without dementia. These episodes may present as visual, auditory, or tactile sensations, often leading to confusion and emotional turmoil. It's important to recognize the impact this can have, not just on the individuals but also on their caregivers.
These hallucinations can arise from various sources, such as:
- Medication side effects
- Sensory deprivation
- Underlying mental health issues
Understanding these causes is crucial. It allows caregivers to provide the necessary support and reassurance, helping to alleviate some of the stress and anxiety that can accompany these experiences.
By addressing these challenges with compassion, we can foster a nurturing environment for both the elderly and their caregivers. It's essential to manage these experiences thoughtfully, ensuring that everyone involved feels supported and understood. Remember, you’re not alone in this journey. There are resources and communities ready to help you navigate these difficult moments.
The Importance of Hallucinations in Elderly Without
Understanding the complexities of hallucinations in elderly individuals without dementia is essential for caregivers who often navigate these distressing experiences. These perceptual disturbances can take many forms—visual, auditory, and tactile—each presenting unique challenges that can deeply affect the quality of life for seniors.
As caregivers strive to provide the best support, it’s natural to feel overwhelmed. What causes these hallucinations? How can they be effectively managed? This guide aims to explore the nature of these hallucinations, their underlying causes, and practical strategies to create a supportive environment. Our goal is to empower caregivers, helping them enhance the well-being of their loved ones.
We understand that the journey can be tough, filled with moments of uncertainty and concern. But remember, you’re not alone in this. Together, we can navigate these challenges with compassion and care.
Define Hallucinations: Types and Characteristics
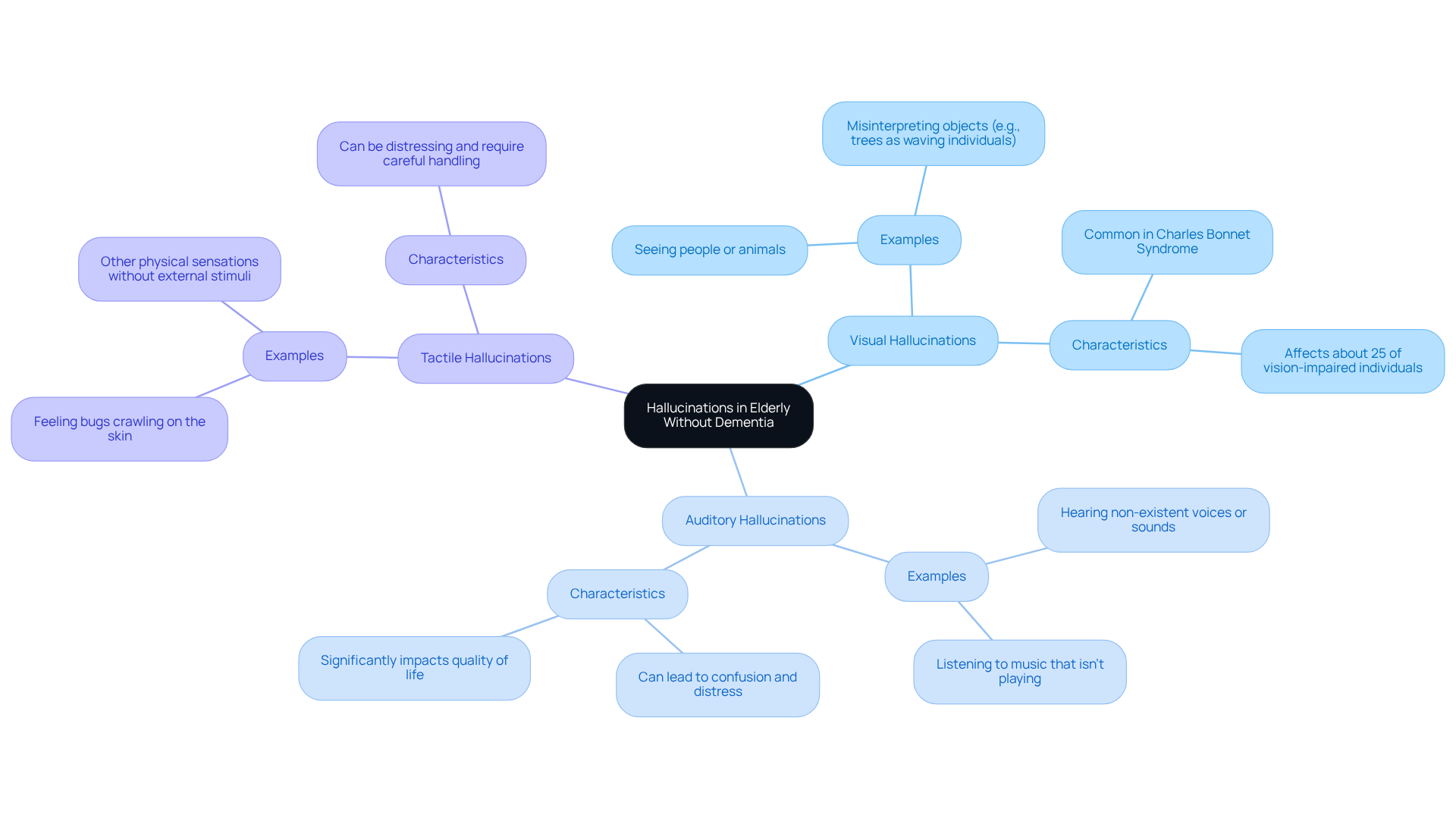
Hallucinations in elderly without dementia can be unsettling experiences that seem real but actually stem from the mind, impacting various senses. For our elderly loved ones, the most common types include:
-
Visual Hallucinations
These involve seeing things that aren’t there, like people, animals, or objects. Imagine a senior looking out their window and perceiving trees as waving individuals. It’s a vivid example of how visual misinterpretations can occur. Research indicates that visual distortions, such as hallucinations in elderly without dementia, are particularly common in conditions like Charles Bonnet Syndrome, affecting about 25% of those with vision impairment. -
Auditory Hallucinations
This type includes hearing sounds, voices, or music that don’t exist. Picture an elderly person hearing conversations or melodies that aren’t really there. This can lead to confusion and distress, making daily life more challenging. Studies show that hallucinations in elderly without dementia can significantly impact the quality of life for seniors, often heightening feelings of isolation. -
Tactile Hallucinations
These involve sensations on the skin, such as the feeling of bugs crawling, which can be quite distressing. Geriatric experts note that tactile illusions can be particularly troubling and may require careful handling to ensure the individual’s comfort.
The characteristics of perceptual disturbances, such as hallucinations in elderly without dementia, can vary widely, including how often they occur, how long they last, and the emotional responses they trigger. Some individuals may experience illusions occasionally, while others might face them more frequently. The emotional impact can range from comfort to distress, depending on the person’s perception and context. Lynne Katzmann, a geriatric expert, reminds us that perceptions can be affected by different factors, such as medication side effects, sensory impairments, and psychological conditions, which can contribute to hallucinations in elderly without dementia.
Understanding these traits is crucial for caregivers. It empowers them to provide the right support and comfort. By fostering an environment of compassion and understanding, caregivers can help alleviate the anxiety associated with sensory misperceptions, ensuring that seniors feel supported and valued.
Identify Causes of Hallucinations in the Elderly
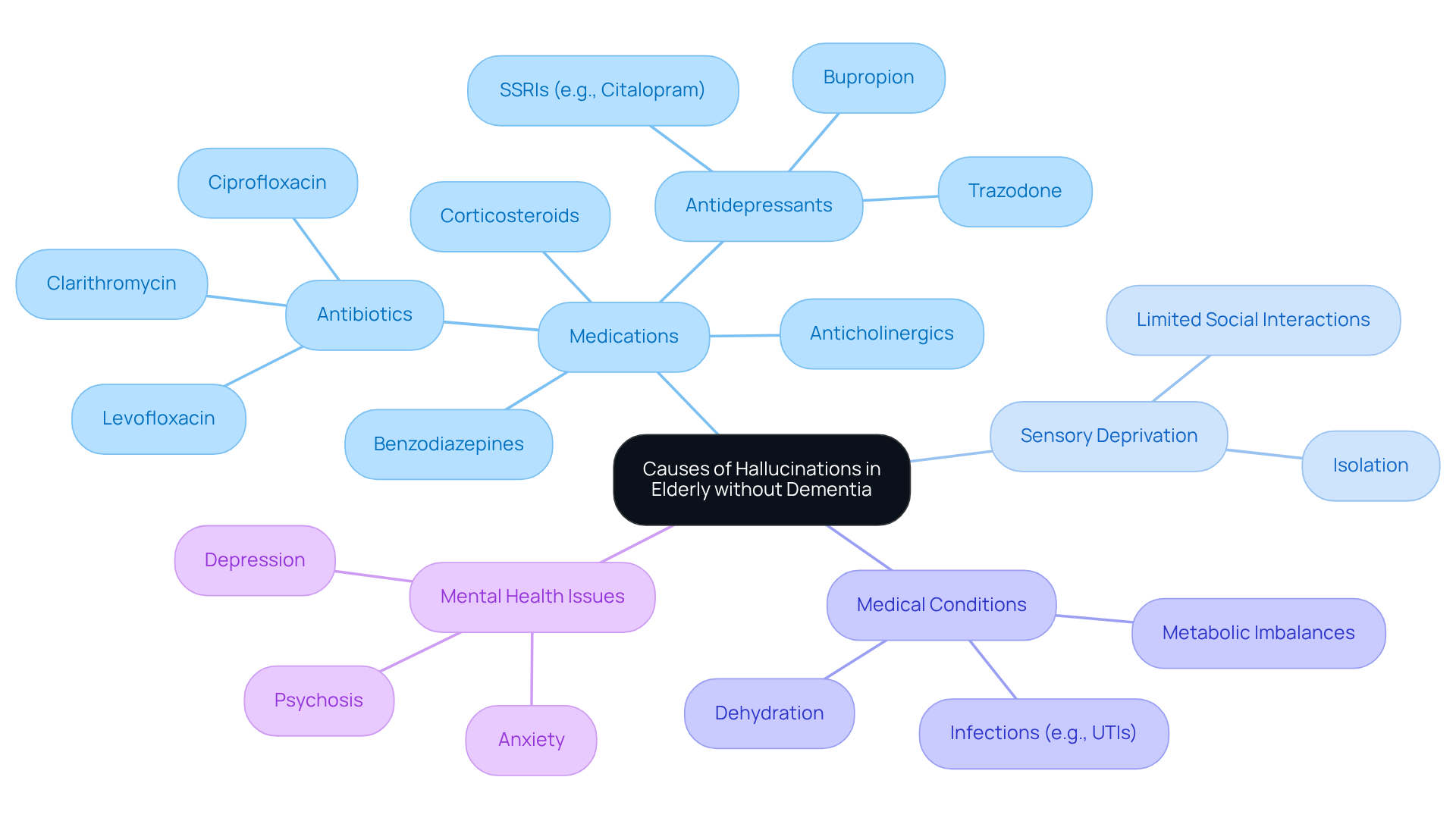
False perceptions, such as hallucinations in elderly without dementia, can be distressing for older adults. It’s important to understand the various factors that can contribute to hallucinations in elderly without dementia, as these experiences can significantly impact both the individual and their caregivers.
-
Medications can play a significant role. Some prescriptions, particularly those for pain, anxiety, or sleep disorders, may cause hallucinations in elderly without dementia as a side effect. Medications like corticosteroids, benzodiazepines, and certain antibiotics can alter brain chemistry, resulting in these unsettling perceptions.
-
Sensory deprivation is another factor to consider. When older adults lack visual or auditory stimulation, especially if they’re isolated or have limited social interactions, false perceptions can arise. Engaging in activities and maintaining social connections is vital for preventing these experiences and fostering a sense of belonging.
-
Medical conditions can also provoke hallucinations in elderly without dementia. Issues like infections, dehydration, or metabolic imbalances can lead to sudden changes in perception. For example, urinary tract infections are often linked to these shifts and require prompt medical attention. Dehydration, too, can lead to serious health concerns, including visual disturbances that should be treated as emergencies.
-
Mental health issues such as anxiety, depression, or psychosis can manifest as sensory disturbances, including hallucinations in elderly without dementia. Addressing these concerns is essential for effective management and support, ensuring that individuals feel understood and cared for.
Recognizing these causes allows caregivers to take proactive steps in managing the situation and seeking appropriate interventions. It’s equally important to acknowledge the emotional toll that false perceptions can have on both the elderly and their caregivers. By fostering a supportive environment, we can help alleviate some of the stress and anxiety associated with these experiences, creating a space where everyone feels valued and cared for.
Implement Care Strategies for Managing Hallucinations
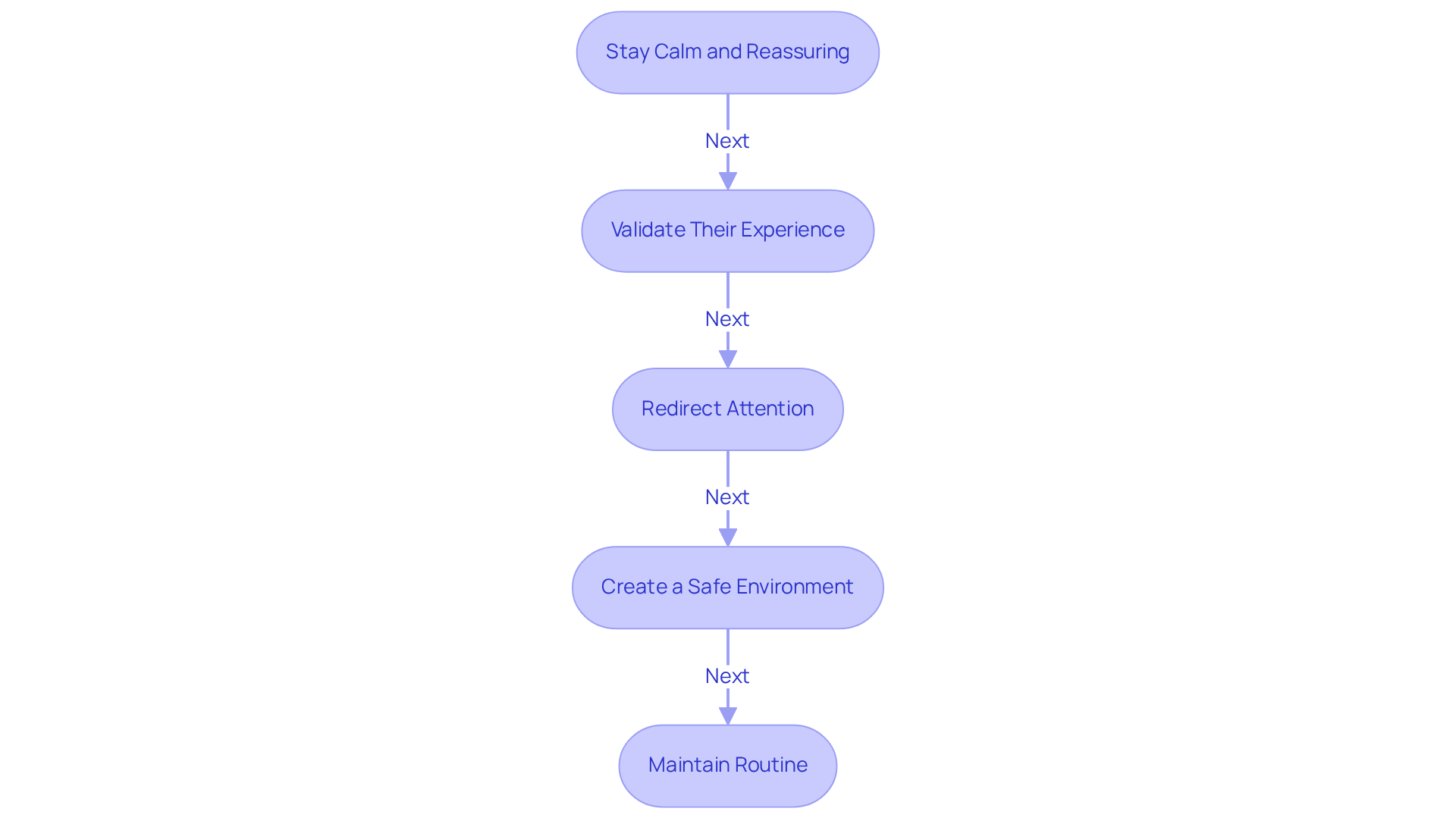
Managing hallucinations in elderly without dementia can be challenging, but there are caring strategies that can help.
-
Stay Calm and Reassuring: When approaching someone experiencing hallucinations, it’s important to remain calm. Use a soothing tone to help ease their anxiety.
-
Validate Their Experience: Acknowledge their feelings without reinforcing the false perception. You might say, "I understand that you see someone, but I don’t see them." This shows you care while gently guiding them back to reality.
-
Redirect Attention: Engaging the person in a different activity or conversation can help shift their focus away from the illusion. This simple act can provide a moment of relief.
-
Create a Safe Environment: Ensure their living space is safe and free from hazards. A secure environment can help prevent risks, especially if the person becomes agitated.
-
Maintain Routine: Establishing a consistent daily routine can offer a sense of stability and predictability, which may help reduce false perceptions.
These strategies can significantly enhance the quality of life for older adults who are dealing with hallucinations in elderly without dementia. Remember, you’re not alone in this journey; compassionate support is always available.
Recognize When to Seek Professional Assistance
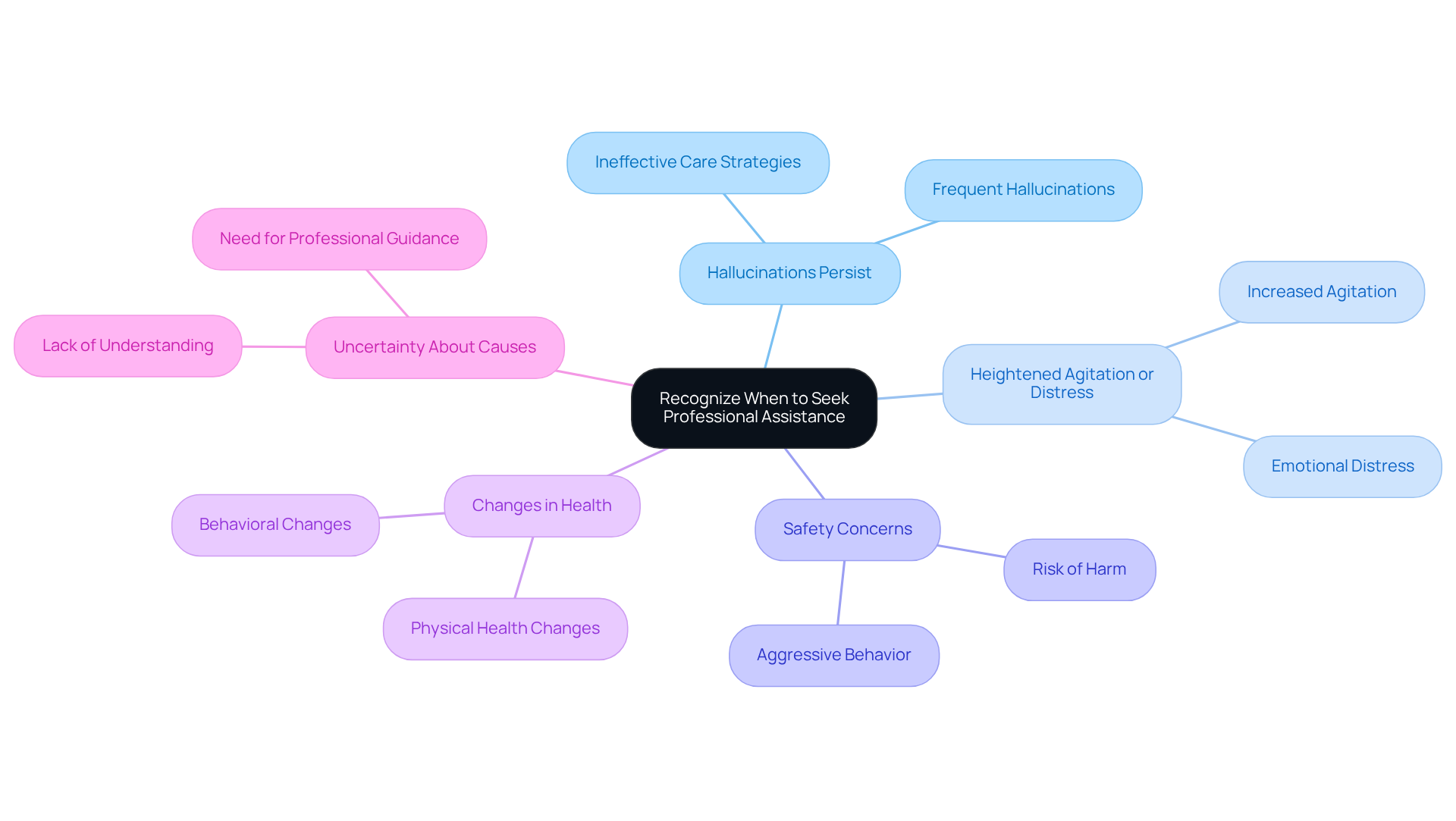
As caregivers, it’s essential to recognize when to seek professional assistance. Here are some situations that may warrant reaching out for help:
- Hallucinations Persist: If you notice that hallucinations are frequent and don’t seem to improve with your care strategies, it’s important to consult a professional.
- Heightened Agitation or Distress: When the person you’re caring for becomes increasingly agitated or distressed due to their sensory experiences, this can be a sign that they need additional support.
- Safety Concerns: If there’s a risk of harm to themselves or others—like wandering off or exhibiting aggressive behavior—don’t hesitate to seek help.
- Changes in Health: Noticeable changes in physical health or behavior that accompany these sensory experiences should not be overlooked.
- Uncertainty About Causes: If you find yourself unsure about the underlying causes of the hallucinations, reaching out for guidance can be incredibly beneficial.
In these challenging moments, consulting with a healthcare professional can provide valuable insights and potential treatment options. Remember, you’re not alone in this journey. Seeking help is a sign of strength, and it can lead to better outcomes for both you and the person you care for.
Key Takeaways for Caregivers
Understanding hallucinations in elderly individuals who do not have dementia is vital for caregivers who want to provide effective support. These experiences can show up as visual, auditory, or tactile perceptions, and they often require a compassionate approach to ease the distress they may bring. By recognizing that these hallucinations can arise from various factors—like medication side effects or sensory deprivation—caregivers can better meet the needs of their loved ones.
Key insights highlight the importance of:
- Identifying the types and causes of hallucinations
- Implementing effective care strategies
- Knowing when to seek professional help
Caregivers are encouraged to:
- Stay calm
- Validate the experiences of those they care for
- Create safe environments that foster a sense of security
Understanding when to reach out for professional assistance can significantly enhance the quality of life for both caregivers and the elderly individuals facing these challenges.
Ultimately, navigating hallucinations in elderly individuals without dementia emphasizes the need for empathy, education, and proactive care. By fostering an environment of understanding and support, caregivers can truly make a meaningful difference in the lives of their loved ones, ensuring they feel safe, valued, and understood. Taking these steps not only boosts the well-being of seniors but also strengthens the caregiver's ability to provide compassionate care amidst complex challenges.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5MDdmMGMzMjgwOGZmMDZiMWM5NTZiZCIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What are hallucinations in the elderly without dementia?
Hallucinations in the elderly without dementia are unsettling experiences that seem real but originate from the mind, affecting various senses.
What are the common types of hallucinations experienced by the elderly?
The most common types include visual hallucinations (seeing things that aren’t there), auditory hallucinations (hearing sounds or voices that don’t exist), and tactile hallucinations (feeling sensations on the skin, such as bugs crawling).
Can you give an example of visual hallucinations in the elderly?
An example of visual hallucinations is an elderly person looking out their window and perceiving trees as waving individuals, illustrating how visual misinterpretations can occur.
How prevalent are visual hallucinations in those with vision impairment?
Research indicates that visual distortions, such as hallucinations, are particularly common in conditions like Charles Bonnet Syndrome, affecting about 25% of individuals with vision impairment.
What are auditory hallucinations and how do they affect the elderly?
Auditory hallucinations involve hearing sounds, voices, or music that do not exist, which can lead to confusion and distress, significantly impacting the quality of life for seniors and heightening feelings of isolation.
What are tactile hallucinations and why can they be distressing?
Tactile hallucinations involve sensations on the skin, like feeling bugs crawling, which can be quite distressing and may require careful handling to ensure the individual’s comfort.
How do the characteristics of hallucinations vary among individuals?
The characteristics of hallucinations can vary widely, including frequency, duration, and emotional responses, ranging from comfort to distress based on individual perception and context.
What factors can contribute to hallucinations in the elderly without dementia?
Factors that can contribute to hallucinations include medication side effects, sensory impairments, and psychological conditions.
Why is understanding hallucinations important for caregivers?
Understanding hallucinations is crucial for caregivers as it empowers them to provide the right support and comfort, fostering an environment of compassion and understanding to alleviate anxiety associated with sensory misperceptions.