
For families in our service areas
For families in our service areas, this guide explains caregiving and how non-medical in-home caregiving can support care planning in East Idaho, Treasure Valley & Magic Valley, Northern Wasatch, North Central West Virginia, and Northeast Ohio.
What You Need to Know About How Elderly Stop Eating Affects Life
The challenge of appetite loss among the elderly is a pressing concern that can drastically influence their life expectancy. Aging individuals often face various physiological, medical, and psychological hurdles that contribute to decreased food and fluid intake. This issue not only affects their health but also raises critical questions about how caregivers can effectively support their loved ones in maintaining proper nutrition and hydration.
Understanding the underlying factors is essential. For instance, changes in taste and smell, medication side effects, and mental health issues can all play a role in appetite loss. These changes can lead to malnutrition and dehydration, which significantly impact the well-being of seniors. Caregivers must recognize these implications to provide the necessary support.
So, what can caregivers do? Here are some actionable strategies:
- Encourage small, frequent meals instead of three large ones to make eating less daunting.
- Enhance the dining experience by creating a pleasant atmosphere, such as using colorful plates or playing soft music.
- Incorporate favorite foods to stimulate appetite and make meals more enjoyable.
- Stay hydrated by offering a variety of fluids, including water, herbal teas, and broths.
By implementing these strategies, caregivers can combat appetite loss and enhance the well-being of seniors, ultimately safeguarding their longevity.
Explore Reasons for Appetite Loss in the Elderly
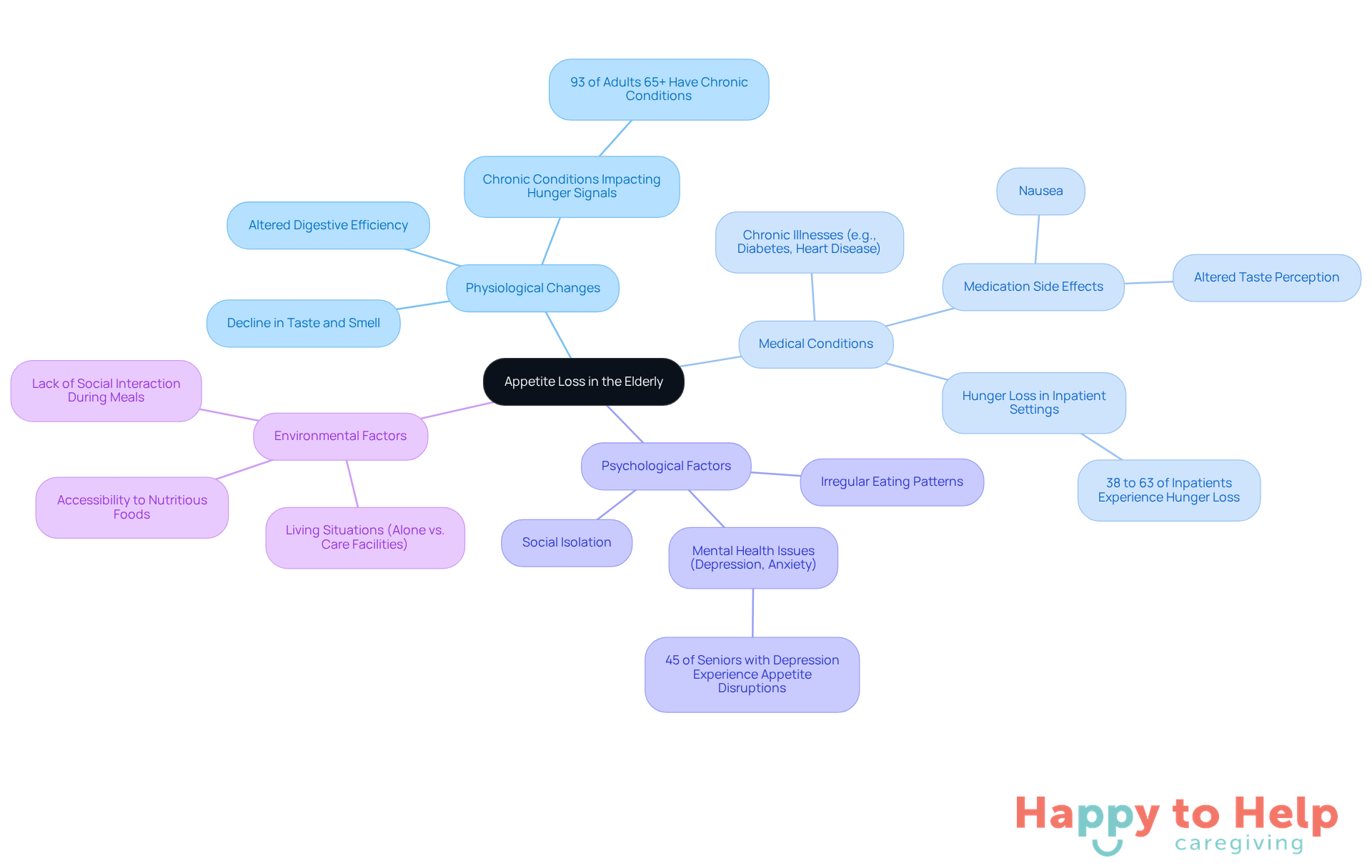
The issue of appetite loss in the elderly can significantly impact their life expectancy, as it often leads to the elderly stop eating and drinking.
-
Physiological Changes: Aging often brings a decline in taste and smell, diminishing food appeal. Research shows that nearly 93% of adults aged 65 and older have at least one chronic condition, which can alter hunger signals and digestive efficiency.
-
Medical Conditions: Chronic illnesses like diabetes, heart disease, and dementia greatly impact hunger. Medications for these conditions can complicate matters, leading to side effects such as nausea or altered taste perception. Studies reveal that hunger loss occurs in 38% to 63% of inpatient environments, highlighting the need for careful monitoring in these groups.
-
Psychological Factors: Mental health issues, including depression and anxiety, are common among older adults and can significantly reduce interest in food. Social isolation can worsen these feelings, leading to irregular eating patterns. Approximately 45% of seniors with depression experience appetite disruptions, creating a cycle of malnutrition and declining mental health.
-
Environmental Factors: Living situations, whether alone or in care facilities, can greatly influence dining experiences and accessibility. A lack of social interaction during meals can decrease motivation to eat, further increasing the risk of malnutrition.
To effectively tackle appetite loss in older adults, caregivers must identify these interconnected factors that influence elderly stop eating and drinking life expectancy. Implementing targeted interventions can improve nutritional intake and enhance overall well-being.
Analyze the Effects of Reduced Food and Fluid Intake on Life Expectancy
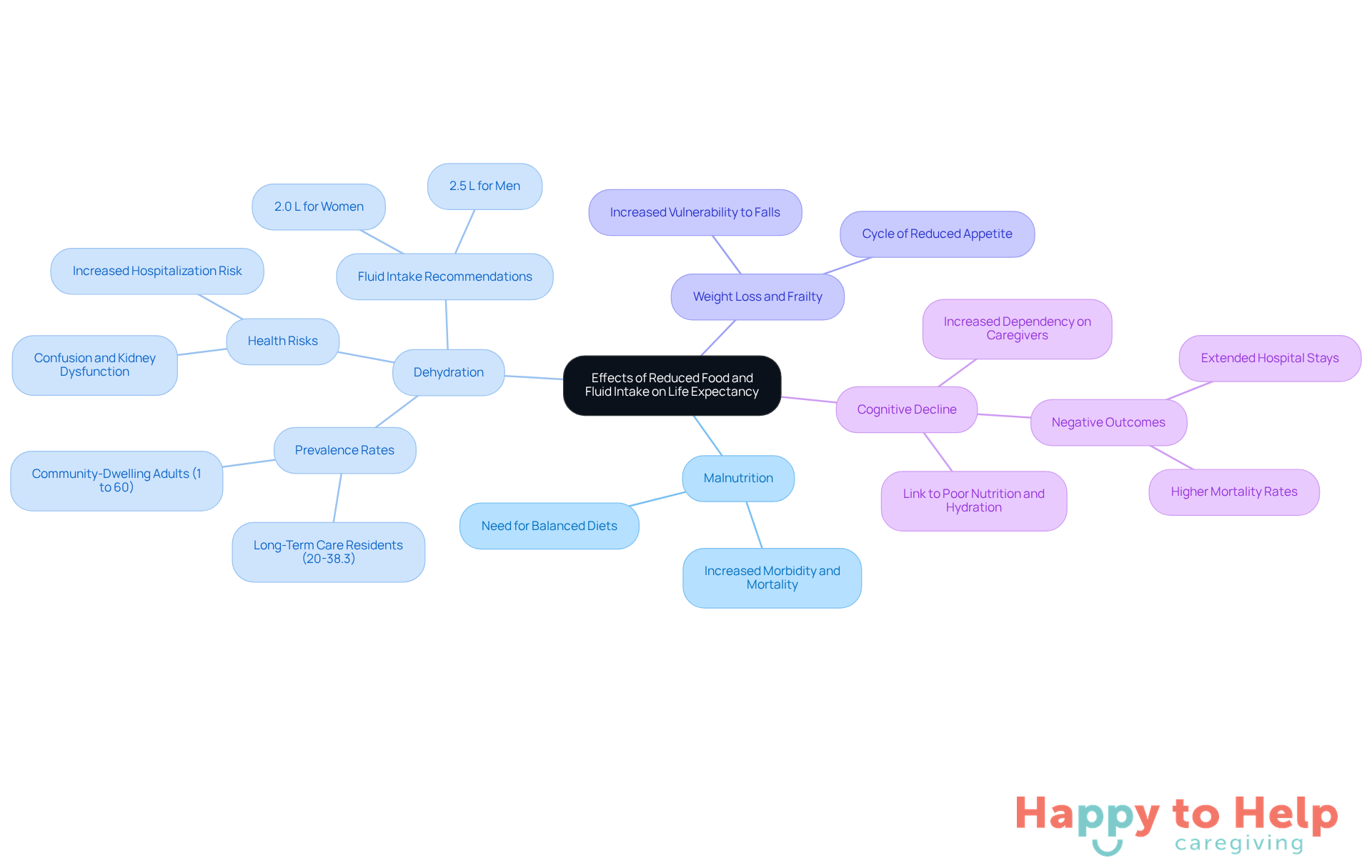
When the elderly stop eating and drinking, it poses significant challenges that impact their life expectancy in several critical ways.
-
Malnutrition is a major concern. Inadequate nutrient intake often leads to malnutrition, which is linked to increased morbidity and mortality rates in seniors. Research indicates that malnutrition can lead to the elderly stop eating and drinking, which significantly shortens life expectancy, underscoring the necessity for balanced diets.
-
Dehydration is another serious risk. Insufficient fluid consumption can lead to dehydration, resulting in confusion, kidney dysfunction, and a heightened risk of hospitalization. Studies show that dehydration prevalence among community-dwelling older adults ranges from 1% to 60%, with long-term care residents facing even higher rates of 20-38.3%. The European Food Safety Authority recommends a daily fluid intake of 2.0 L for women and 2.5 L for men to maintain proper hydration.
-
Weight loss and frailty are also critical issues. Unintentional weight loss frequently leads to frailty, increasing vulnerability to falls and other medical complications. This weakness can create a damaging cycle, further reducing appetite and nutritional intake, which intensifies risks to well-being.
-
Cognitive decline is accelerated by poor nutrition and hydration. This decline diminishes quality of life and increases dependency on caregivers. Research links dehydration to cognitive decline, resulting in negative outcomes such as extended hospital stays and higher mortality rates. A Cochrane systematic review highlights that traditional clinical symptoms may not reliably indicate dehydration in older adults, emphasizing the need for careful assessment.
Understanding these effects is crucial. Caregivers must take proactive measures to ensure adequate nutrition and hydration, as these are vital for maintaining health and preventing the elderly from stopping eating and drinking, which impacts life expectancy.
Implement Strategies for Supporting Elderly Individuals Who Stop Eating and Drinking
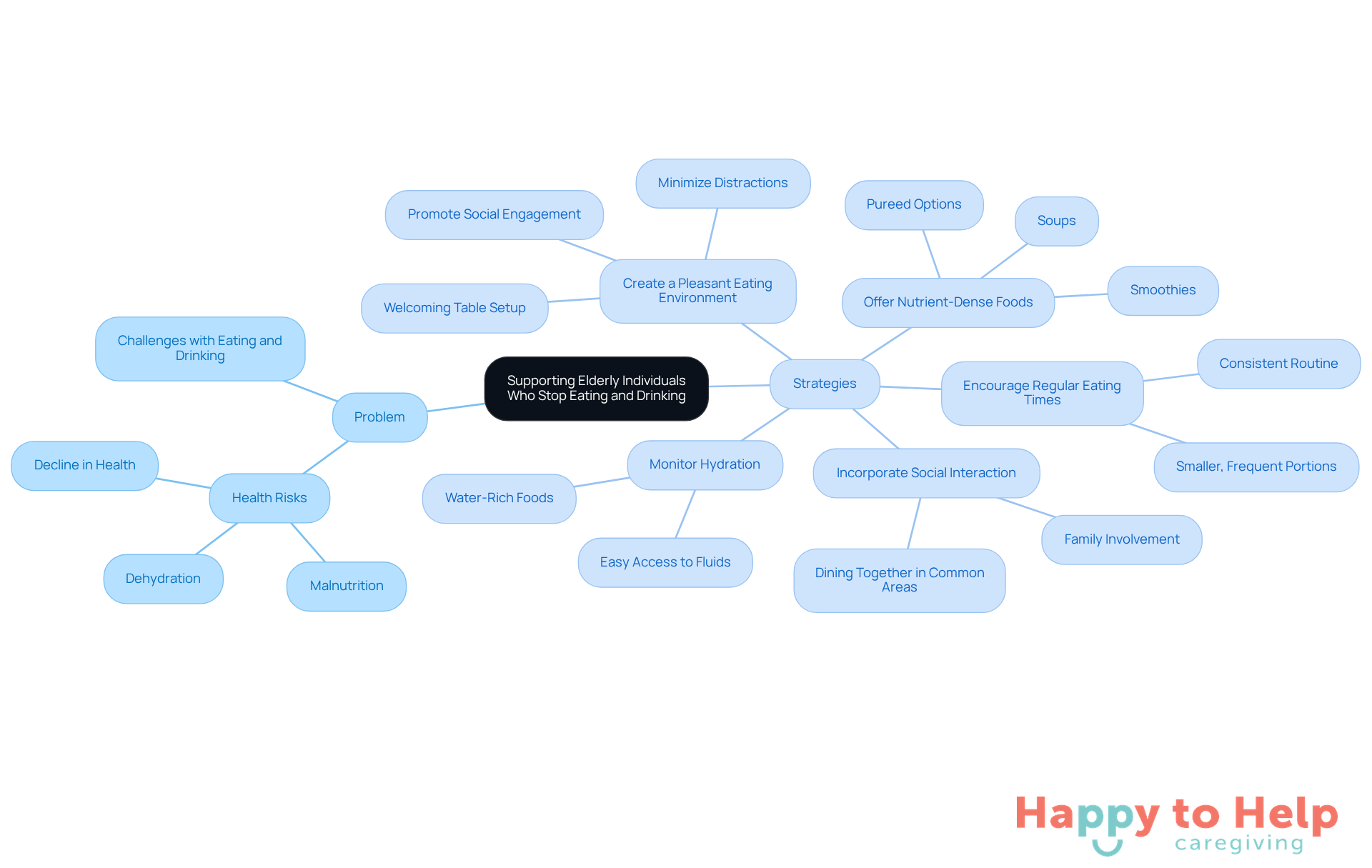
Problem: Many elderly individuals face challenges with eating and drinking, which can lead to serious health issues. This situation not only affects their nutritional intake but also impacts their overall well-being.
Agitate: When the elderly stop eating and drinking, it can lead to malnutrition, dehydration, and a decline in health, ultimately affecting their life expectancy. Caregivers often struggle to find effective ways to encourage proper nutrition and hydration, which can be frustrating and concerning.
Solution: To effectively support elderly individuals who have stopped eating and drinking, consider implementing the following strategies:
- Create a Pleasant Eating Environment: Transform mealtimes into enjoyable experiences by setting a welcoming table, utilizing colorful plates, and minimizing distractions. As Scaringella, a licensed nutritionist, observes, "Establishing a welcoming dining environment and promoting social engagement during dining can also boost hunger." A pleasant atmosphere can significantly enhance the overall dining experience, making dishes more appealing.
- Offer Nutrient-Dense Foods: Prioritize foods that are rich in nutrients yet low in volume, such as smoothies, soups, and pureed options. These choices provide essential vitamins and minerals without overwhelming the individual, making it easier for them to consume adequate nutrition.
- Encourage Regular Eating Times: Establishing a consistent routine for food and snacks can help stimulate appetite. Smaller, more frequent portions are often easier for seniors than conventional three large servings a day, encouraging better intake.
- Incorporate Social Interaction: Encourage family members or friends to join for dining. Socializing during meals not only enhances the enjoyment of food but also stimulates appetite, creating a more engaging mealtime experience. Scaringella emphasizes that "encouraging residents to dine together in common areas fosters socialization and improves meal enjoyment."
- Monitor Hydration: Ensure that fluids are easily accessible and promote regular consumption. Individuals over 60 should consume 25-30 ml of fluids per kg of body weight daily, as highlighted by Scaringella. Offering water-rich foods like fruits and vegetables can help maintain hydration levels, which is crucial for overall health.
By implementing these strategies, caregivers can significantly improve the nutritional intake and overall well-being of elderly individuals, which can help address issues related to the elderly stop eating and drinking life expectancy, fostering a healthier and more enjoyable dining experience.
Address Emotional Challenges for Caregivers and Families
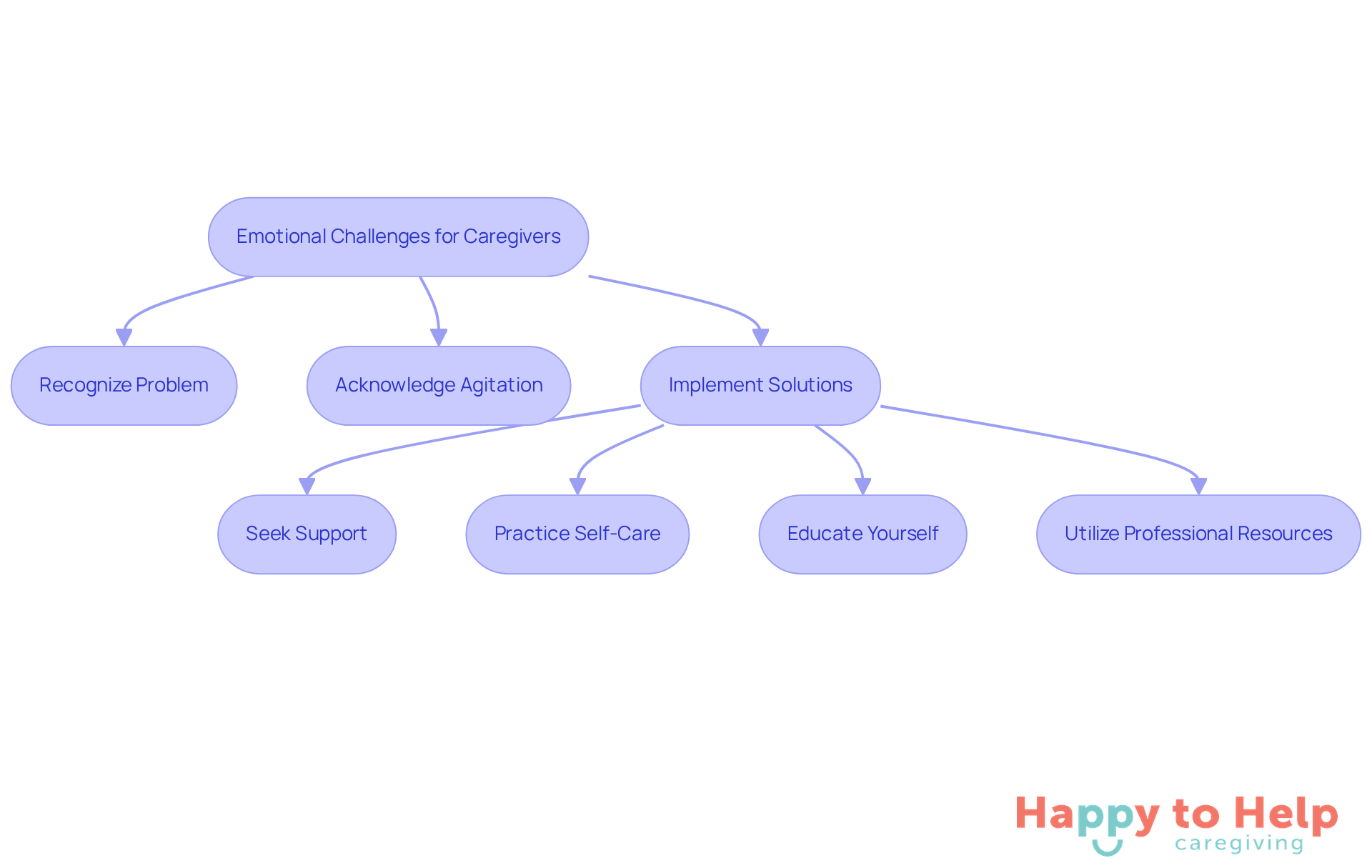
Caregivers often face significant emotional challenges when managing appetite loss in elderly individuals. Recognizing these challenges is crucial for effective support.
Problem: Caregiver stress can manifest as fatigue, irritability, and feelings of being overwhelmed. Research shows that 40 to 70 percent of caregivers exhibit symptoms of depression compared to noncaregivers. Acknowledging these emotions is the first step toward effective management.
Agitate: The emotional toll on caregivers can lead to burnout, impacting their ability to provide care. Financial strain is also prevalent, with 71% of caregivers reporting financial struggles, making self-care even more critical.
Solution: Here are effective strategies to address these challenges:
- Seek Support: Connecting with family, friends, or support groups can be invaluable. Sharing experiences not only provides relief but also offers new perspectives on coping strategies. Case studies show that caregivers in support groups report enhanced mental well-being, highlighting the importance of community.
- Practice Self-Care: Prioritizing wellness is essential. Regular breaks, engaging in hobbies, and maintaining social connections are vital for emotional resilience.
- Educate Yourself: Understanding the causes and effects of appetite loss can empower caregivers to take proactive measures that prevent the elderly from stop eating and drinking, which can negatively impact their life expectancy. Knowledge reduces feelings of helplessness and enhances management capabilities.
- Utilize Professional Resources: Consulting healthcare professionals or nutritionists specializing in geriatric care can provide tailored support. As Debra Barrett from Otsuka emphasizes, addressing the mental health of caregivers is essential for whole-person care.
By addressing these emotional challenges, caregivers can enhance their own well-being while providing more effective support for their loved ones.
Making the Right Choice
Understanding the factors contributing to appetite loss in the elderly is crucial, as this issue has significant implications for their life expectancy. When older adults stop eating and drinking, it can lead to a cascade of health challenges, including malnutrition, dehydration, and cognitive decline. These challenges can severely impact their quality of life and longevity.
Several key reasons for appetite loss include:
- Physiological changes
- Medical conditions
- Psychological factors
- Environmental influences
Each of these elements diminishes the desire to eat, ultimately leading to serious health risks. Caregivers can address these challenges by:
- Creating a pleasant dining atmosphere
- Offering nutrient-dense foods
- Promoting social interaction during meals
Recognizing the emotional toll on caregivers is also essential for fostering a supportive environment for both the elderly and their families.
The health and well-being of elderly individuals depend on proactive measures to ensure proper nutrition and hydration. Caregivers and families must remain vigilant in identifying signs of appetite loss and implementing strategies to encourage healthy eating habits. By prioritizing nutrition and emotional support, the elderly can lead healthier, more fulfilling lives, thereby enhancing their overall life expectancy.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5MjY0MzlmMTRjODUwNzI1NGI4N2FjMiIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What is the significance of appetite loss in the elderly?
Appetite loss in the elderly can significantly impact life expectancy, as it often leads to a reduction in food and fluid intake.
What physiological changes contribute to appetite loss in older adults?
Aging typically brings a decline in taste and smell, which diminishes the appeal of food. Additionally, many older adults have chronic conditions that can alter hunger signals and digestive efficiency.
How do medical conditions affect appetite in the elderly?
Chronic illnesses such as diabetes, heart disease, and dementia can greatly impact hunger. Medications for these conditions may lead to side effects like nausea or altered taste perception, contributing to appetite loss.
What percentage of older adults experience hunger loss in inpatient environments?
Studies indicate that hunger loss occurs in 38% to 63% of inpatient environments among older adults, highlighting the need for careful monitoring.
What psychological factors influence appetite in older adults?
Mental health issues, particularly depression and anxiety, are common in older adults and can significantly reduce interest in food. Social isolation may exacerbate these feelings, leading to irregular eating patterns.
How prevalent is appetite disruption among seniors with depression?
Approximately 45% of seniors with depression experience disruptions in appetite, which can create a cycle of malnutrition and declining mental health.
What environmental factors affect dining experiences for the elderly?
Living situations, whether alone or in care facilities, can greatly influence dining experiences and accessibility. A lack of social interaction during meals can decrease motivation to eat, increasing the risk of malnutrition.
What is essential for caregivers to address appetite loss in older adults?
Caregivers must identify the interconnected factors influencing appetite loss and implement targeted interventions to improve nutritional intake and enhance overall well-being.
List of Sources
- Explore Reasons for Appetite Loss in the Elderly
- How Behavioral Health Affects Nutrition and Appetite in Older Adults - Supportive Care (https://thesupportivecare.com/blog/how-behavioral-health-affects-nutrition-and-appetite-in-older-adults)
- Study: Appetite loss strikes 1 in 4 older adults before malnutrition develops (https://mcknights.com/news/study-appetite-loss-strikes-1-in-4-older-adults-before-malnutrition-develops)
- Appetite loss in older adults without undernutrition: associated factors and clinical implications - BMC Geriatrics (https://bmcgeriatr.biomedcentral.com/articles/10.1186/s12877-025-06336-3)
- What Causes Loss of Appetite in Older Adults? (https://ncoa.org/article/4-common-nutrition-challenges-of-older-adults-and-what-to-do-about-them)
- Poor Appetite in Frail Older Persons—A Systematic Review - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10346828)
- Analyze the Effects of Reduced Food and Fluid Intake on Life Expectancy
- Hydration and older adults: Why water matters more as you age (https://uclahealth.org/news/article/hydration-and-older-adults-why-water-matters-more-you-age)
- Link between hydration and aging (https://nih.gov/news-events/nih-research-matters/link-between-hydration-aging)
- Hydration Status in Older Adults: Current Knowledge and Future Challenges - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10255140)
- Implement Strategies for Supporting Elderly Individuals Who Stop Eating and Drinking
- Proper Nutrition Crucial for Seniors in Assisted Living Facilities, Says Dietitian (https://ltcnews.com/articles/proper-nutrition-seniors-assisted-living-facilities-dietitian)
- Frontiers | A study on the reasonable dietary trajectory of elderly people in the community and its correlation with body mass index (https://frontiersin.org/journals/nutrition/articles/10.3389/fnut.2024.1429627/full)
- The changing nutritional needs of older adults and how to meet them (https://heart.org/en/news/2024/12/18/the-changing-nutritional-needs-of-older-adults-and-how-to-meet-them)
- How Dining Together Builds Community in Senior Living (https://somerbypeachtreecity.com/how-dining-together-builds-community-in-senior-living)
- Famous Quotes on Nutrition and Well-Being - Center for the Advancement of Well-Being (https://wellbeing.gmu.edu/famous-quotes-on-nutrition-and-well-being)
- Address Emotional Challenges for Caregivers and Families
- New Report Reveals Crisis Point for America’s 63 million Family Caregivers (https://press.aarp.org/2025-07-24-New-Report-Reveals-Crisis-Point-for-Americas-63-million-Family-Caregivers)
- Caregiving’s Mental Health Crisis (https://forbes.com/sites/otsuka/2025/10/02/caregivings-mental-health-crisis)
- The Caregiving Landscape: Data & Insights on the Caregiver Experience in the U.S. (https://caregiveraction.org/caregiver-statistics)
- Opinion | America’s Caregivers Are in Crisis (https://nytimes.com/2025/11/24/opinion/caregiving-crisis.html)
- Caregiving is taking a toll on the mental health of millions of Americans (https://npr.org/2025/01/26/nx-s1-5271537/caregiving-is-taking-a-toll-on-the-mental-health-of-millions-of-americans)