
For families in our service areas
For families in our service areas, this guide explains caregiver support and how non-medical in-home caregiving can support care planning in East Idaho, Treasure Valley & Magic Valley, Northern Wasatch, North Central West Virginia, and Northeast Ohio.
Quick Guide to Nighttime Hallucinations in the
Nighttime hallucinations in the elderly can be deeply distressing, often stemming from cognitive decline, medication side effects, sensory loss, sleep disorders, and various medical conditions. These factors can lead to unsettling sensory perceptions that occur without any external stimuli.
For caregivers, understanding these causes is crucial. It not only helps in recognizing the challenges faced by their loved ones but also allows them to provide compassionate care. By being aware of these underlying issues, caregivers can implement effective coping strategies that significantly enhance the quality of life for those affected.
Imagine the relief that comes from knowing how to respond to these episodes with empathy and understanding. Caregivers often experience stress and burnout, but they are not alone. There are resources and support systems available that can help lighten this emotional load.
By sharing personal stories and testimonials from those who have navigated similar challenges, we can foster a deeper emotional connection. These narratives highlight the compassionate care that makes a difference, reminding us that every small act of kindness counts.
As we move forward, let’s embrace the journey together, offering reassurance and encouragement to one another. Remember, your efforts matter, and with the right support, you can create a nurturing environment that uplifts both you and your loved ones.
Why Nighttime Hallucinations in the Matters
Understanding the complexities of nighttime hallucinations in the elderly is vital for caregivers facing this often distressing experience. It’s heart-wrenching to know that about one-third of seniors with dementia encounter these unsettling sensory perceptions. The implications for both the individuals affected and their caregivers are significant.
As caregivers strive to provide compassionate support, they may find themselves grappling with questions:
- What underlying factors contribute to these hallucinations?
- How can they effectively manage them?
This guide aims to shed light on the causes of nighttime hallucinations while offering practical strategies to enhance the quality of care for those impacted.
Navigating this journey can be overwhelming, but remember, you’re not alone. Many caregivers share similar experiences, and together, we can find ways to cope and provide the best care possible.
Define Hallucinations in the Elderly
Hallucinations in the elderly at night can be deeply unsettling. These sensory perceptions occur without any external stimulus, affecting sight, sound, touch, taste, and smell. Many elderly individuals experience hallucinations in the elderly at night, such as visual distortions where they see things that aren’t there or auditory experiences like hearing voices or sounds that don’t exist. This can be distressing not just for those experiencing hallucinations in the elderly at night but also for their caregivers, emphasizing the need to understand these phenomena and their implications.
Research indicates that about 33% of elderly individuals with dementia encounter illusions, based on a study of 2,337 seniors. However, many cases go unreported due to stigma and shame. Patients and caregivers often hesitate to share their experiences with healthcare providers, creating a significant gap in understanding the true prevalence of these sensory experiences. Geriatric specialists point out that hallucinations in the elderly at night can stem from various underlying conditions, including dementia, delirium, and sensory impairments. For instance, visual impairments can exacerbate hallucinations, making it crucial for caregivers to ensure that individuals are using their glasses or hearing aids as needed.
Real-life situations shed light on the impact of these sensory experiences in elderly care. Caregivers frequently find themselves in scenarios where individuals misidentify familiar people or objects, leading to confusion and distress. In these moments, employing validation methods—acknowledging the emotions behind these experiences and providing calm reassurance—can be a powerful way to offer comfort and support. Understanding sensory experiences, particularly hallucinations in the elderly at night, is essential for caregivers to provide appropriate assistance and enhance the quality of life for those affected.
As caregivers, it’s important to remember that you’re not alone in this journey. Many have walked this path and found ways to cope and provide compassionate care. By sharing experiences and seeking support, you can navigate these challenges together, fostering a nurturing environment for both you and your loved ones.

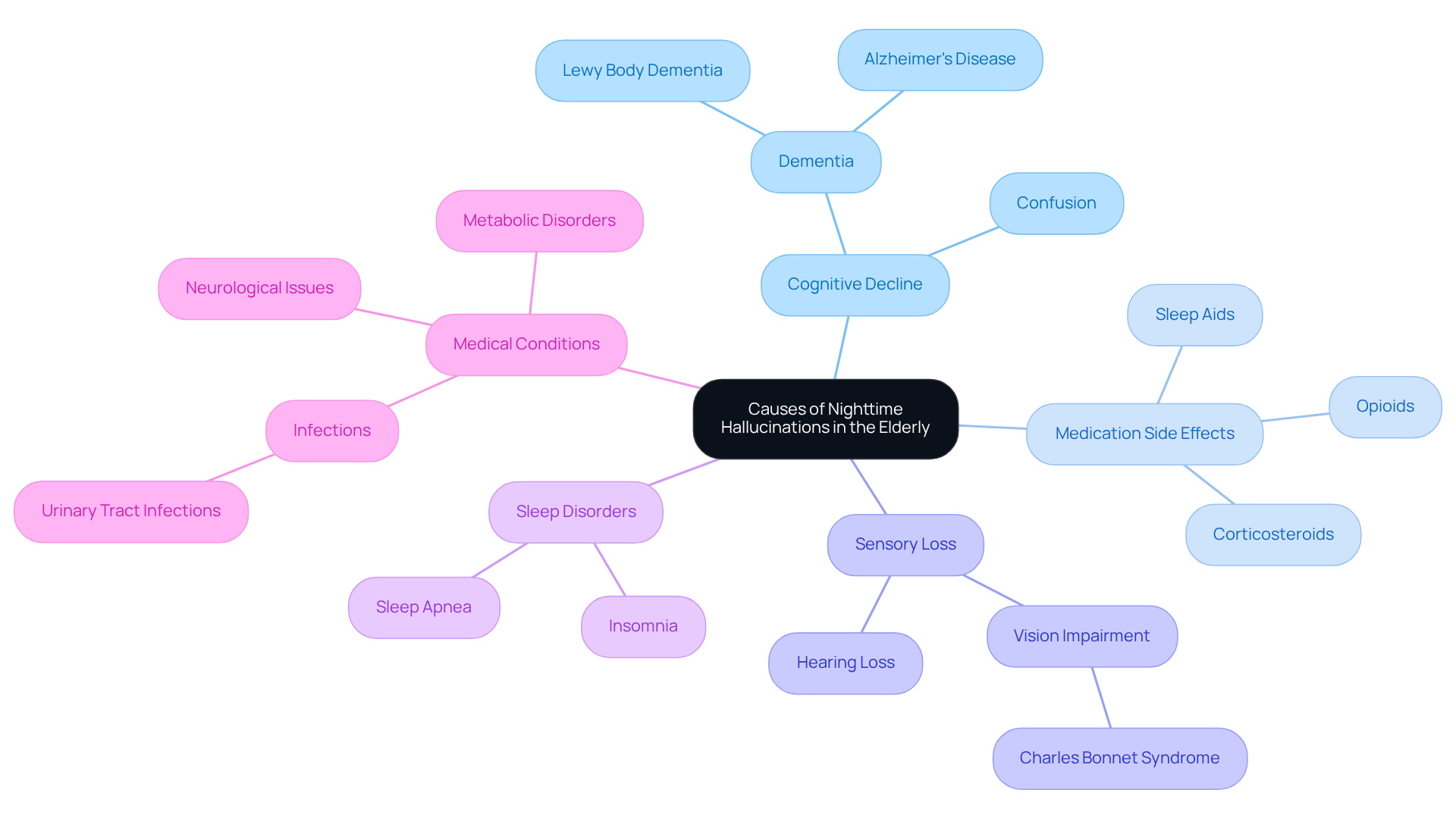
Identify Causes of Nighttime Hallucinations
Hallucinations in the elderly at night can be distressing for both them and their caregivers. Understanding the factors that contribute to hallucinations in the elderly at night is crucial for providing compassionate care.
-
Cognitive Decline is one significant factor. Conditions like dementia can lead to confusion and hallucinations in the elderly at night, especially when cognitive function tends to wane. Caregivers should be particularly attentive during these times, as research indicates that hallucinations in the elderly at night are common in individuals with Lewy body dementia.
-
Medication Side Effects also play a role. Some medications, particularly those affecting the central nervous system, can cause visual or auditory distortions. Opioids, corticosteroids, and certain sleep aids are known to have these side effects. It’s essential for caregivers to monitor medication regimens closely to ensure the well-being of older adults and reduce the risk of hallucinations in the elderly at night.
-
Sensory Loss can further complicate matters. Impairments in vision or hearing may lead to misinterpretations of stimuli, which can result in false perceptions and potentially cause hallucinations in the elderly at night. For instance, seniors experiencing vision loss might encounter Charles Bonnet syndrome, where they see vivid images that aren’t actually there.
-
Sleep Disorders like sleep apnea or insomnia can exacerbate these perceptions, particularly during the transition between wakefulness and sleep. A lack of sleep increases the likelihood of hallucinations in the elderly at night, making it vital to address any sleep-related issues promptly.
-
Medical Conditions such as infections, metabolic disorders, or neurological issues can also trigger visual disturbances. For example, urinary tract infections (UTIs) often present with altered mental states in older adults, leading to confusion and distorted perceptions. It is essential to consult healthcare professionals for proper diagnosis and treatment to effectively manage symptoms such as hallucinations in the elderly at night.
Navigating these challenges can be overwhelming, but caregivers are not alone. Seeking support and understanding can make a significant difference in managing the emotional and practical aspects of care.
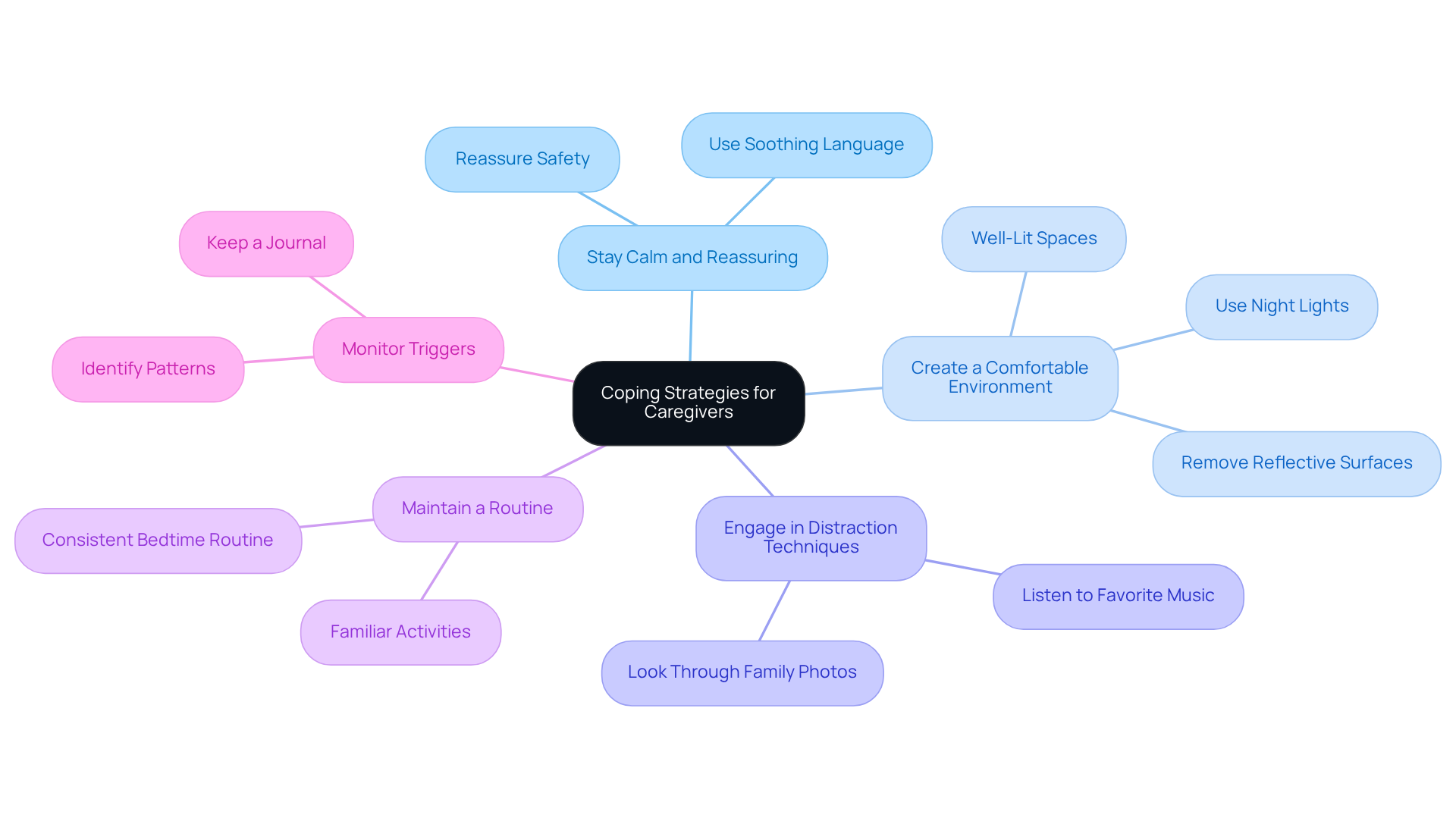
Implement Coping Strategies for Caregivers
Caring for a loved one who is experiencing hallucinations in the elderly at night can be incredibly challenging. It’s important to recognize the emotional toll this can take on caregivers. You’re not alone in feeling overwhelmed; many caregivers share similar feelings of stress and burnout. However, there are effective strategies you can implement to help manage situations involving hallucinations in the elderly at night with compassion and care.
-
Stay Calm and Reassuring: When your loved one experiences a hallucination, responding with calmness is crucial. Reassure them that they are safe and that you’re right there to help. This simple act can significantly alleviate their anxiety and provide comfort during distressing moments caused by hallucinations in the elderly at night.
-
Create a Comfortable Environment: A soothing atmosphere can make a world of difference. Ensure the room is well-lit and free from shadows that might provoke visual distortions. Consider using night lights and removing potential triggers, like reflective surfaces, to create a space that feels safe and calming.
-
Engage in Distraction Techniques: Sometimes, redirecting attention can be beneficial. Engaging your loved one in enjoyable activities, such as listening to their favorite music or looking through family photos, can be beneficial, particularly for those experiencing hallucinations in the elderly at night. These moments can help shift their focus away from distressing experiences and foster a sense of connection.
-
Maintain a Routine: Establishing a consistent bedtime routine can ease anxiety and confusion. Familiarity provides a sense of security, making it easier for your loved one to transition to sleep. This small change can have a big impact on their overall well-being.
-
Monitor Triggers: Keeping a journal to record when episodes occur can help identify potential triggers, such as fatigue or increased stress. Understanding these patterns allows you to make adjustments that can minimize future occurrences, providing both you and your loved one with a greater sense of control.
Remember, you’re doing an incredible job. It’s okay to seek support and take care of yourself, too. Your well-being is just as important as that of your loved one.
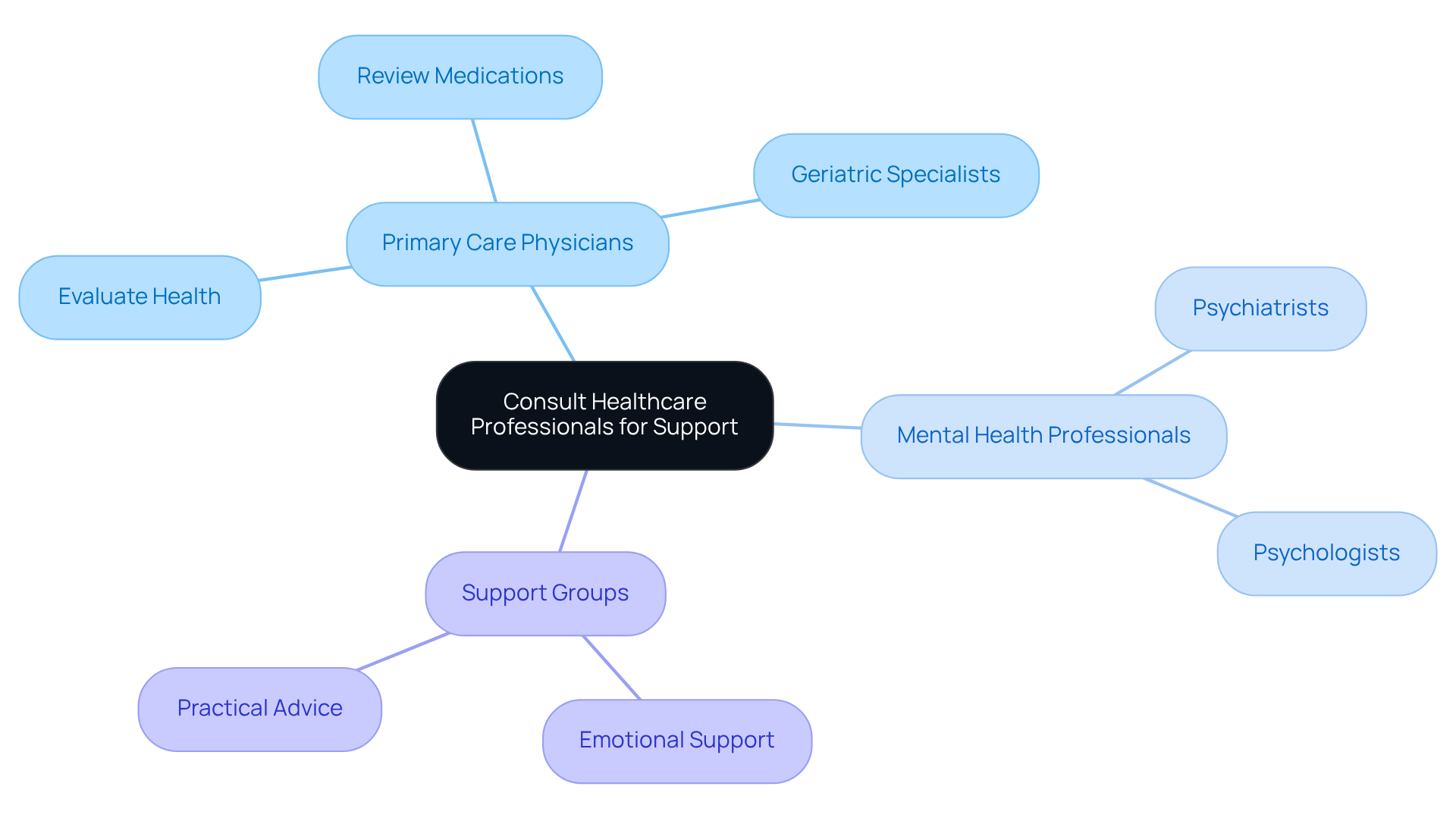
Consult Healthcare Professionals for Support
Caring for someone experiencing hallucinations in the elderly at night can be overwhelming, and it’s important for caregivers to know they’re not alone. Consulting healthcare professionals can be a vital step in ensuring the well-being of your loved one. Here are some options to consider:
- Primary Care Physicians: They play a crucial role in evaluating overall health, reviewing medications, and ruling out any underlying medical conditions that might be contributing to these experiences. Geriatric specialists focus on the unique needs of older adults, including addressing hallucinations in the elderly at night, and offer tailored advice and treatment options that can make a significant difference.
- Mental Health Professionals: Psychiatrists or psychologists can help address any psychological factors that may be at play, providing therapies that can ease distressing symptoms.
- Support Groups: Connecting with other caregivers can be incredibly beneficial. Sharing experiences can provide not only emotional support but also practical advice on managing similar situations.
Regular check-ins with healthcare providers are essential. They can help monitor any changes in your loved one’s condition, ensuring that any concerns are addressed promptly. Remember, seeking help is a sign of strength, and you’re taking an important step in providing the best care possible.
Key Takeaways for Caregivers
Understanding nighttime hallucinations in the elderly is vital for nurturing compassionate care and support. These sensory experiences can be distressing, not just for those experiencing them but also for their caregivers. By recognizing the complexities surrounding hallucinations, caregivers can navigate the emotional and practical challenges that arise, ultimately enhancing the quality of life for their loved ones.
Hallucinations in the elderly can arise from various causes, including:
- Cognitive decline
- Medication side effects
- Sensory loss
- Sleep disorders
- Underlying medical conditions
Caregivers play a crucial role in identifying these factors and implementing effective coping strategies. Maintaining a calm environment, engaging in distraction techniques, and establishing a consistent routine can make a significant difference. Additionally, consulting healthcare professionals can provide invaluable support and guidance, ensuring that both caregivers and their loved ones receive the care they need.
The journey of caring for someone experiencing nighttime hallucinations can feel overwhelming. However, it’s essential to remember that support and understanding are available. By fostering open communication, seeking help when necessary, and sharing experiences with fellow caregivers, a nurturing environment can be created. This collaborative approach not only eases the burden of caregiving but also reinforces the dignity and well-being of those affected by hallucinations.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5MDQwNjM4MmU5MmEzYjRjYWFmYzM1MyIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What are hallucinations in the elderly?
Hallucinations in the elderly are sensory perceptions that occur without any external stimulus, affecting sight, sound, touch, taste, and smell. They can include visual distortions or auditory experiences, such as seeing things that aren’t there or hearing voices or sounds that don’t exist.
How common are hallucinations in the elderly, particularly at night?
Research indicates that about 33% of elderly individuals with dementia experience hallucinations. However, many cases go unreported due to stigma and shame, which creates a significant gap in understanding their true prevalence.
What underlying conditions can cause hallucinations in the elderly?
Hallucinations in the elderly can stem from various underlying conditions, including dementia, delirium, and sensory impairments. For example, visual impairments can exacerbate hallucinations.
How can caregivers support elderly individuals experiencing hallucinations?
Caregivers can support elderly individuals by using validation methods, which involve acknowledging the emotions behind the hallucinations and providing calm reassurance to offer comfort and support.
What should caregivers keep in mind when dealing with hallucinations in the elderly?
Caregivers should ensure that individuals are using their glasses or hearing aids as needed, as sensory impairments can contribute to hallucinations. It is also important for caregivers to seek support and share experiences with others facing similar challenges.