
For families in our service areas
For families in our service areas, this guide explains dementia care and how non-medical in-home caregiving can support care planning in East Idaho, Treasure Valley & Magic Valley, Northern Wasatch, North Central West Virginia, and Northeast Ohio.
What You Need to Know About The Difference Between Delirium and
Understanding the nuances between delirium and dementia is vital for caregivers navigating the complexities of cognitive health. Caregivers often face the problem of confusing these two conditions, which present distinct challenges that require tailored approaches to care. This confusion can lead to inadequate support for those affected, making it crucial for caregivers to differentiate between the sudden, fluctuating confusion of delirium and the gradual cognitive decline of dementia.
To address this issue, caregivers must recognize the key characteristics and symptoms of each condition. Delirium typically manifests as rapid changes in attention and awareness, while dementia involves a slow, progressive decline in cognitive function. By understanding these differences, caregivers can respond appropriately and enhance the well-being of those they care for.
This article delves into effective caregiving strategies that empower caregivers to navigate these challenges. By equipping themselves with knowledge and practical tips, caregivers can provide the best support possible, ensuring that they meet the unique needs of individuals experiencing cognitive health issues.
Define Delirium and Dementia: Key Characteristics
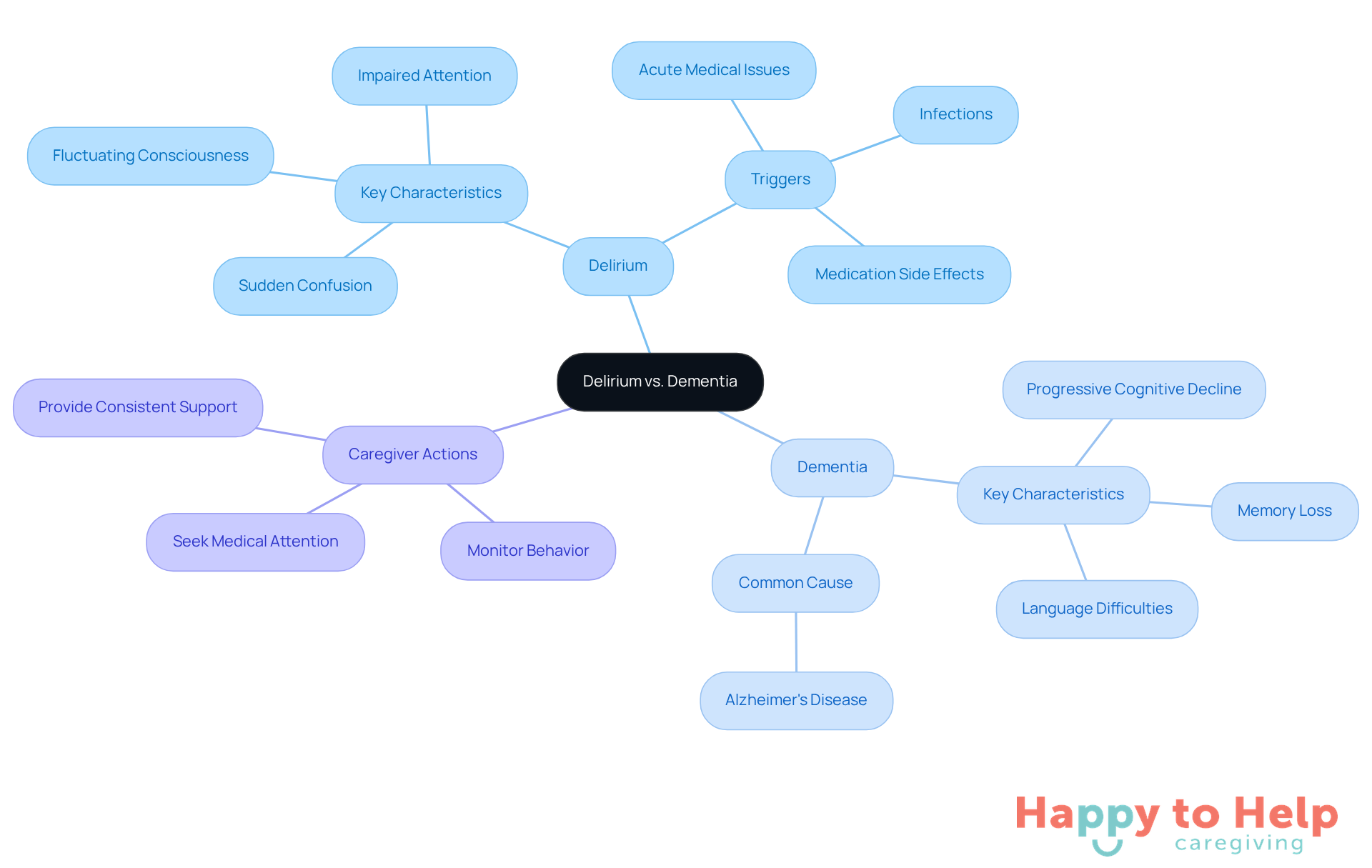
Delirium presents a significant challenge for caregivers, marked by sudden confusion, fluctuating consciousness, and impaired attention. Often triggered by acute medical issues like infections or medication side effects, this condition can evolve rapidly, sometimes within hours or days. In contrast, cognitive decline is a progressive deterioration in cognitive function, characterized by memory loss, language difficulties, and impaired reasoning. Unlike acute confusion, cognitive decline unfolds slowly over months or years and is typically permanent, with Alzheimer's disease accounting for about 70% of cognitive impairment cases.
It is crucial for caregivers to understand the difference between delirium and dementia. Confusion can affect up to 50% of elderly individuals in acute care settings, leading to longer hospital stays and increased mortality rates. Neurologists emphasize that while confusion can be reversible with appropriate care, cognitive decline requires ongoing support. For instance, caregivers may notice a family member exhibiting sudden confusion and disorientation, which could indicate an altered mental state, especially if linked to recent medical changes. Conversely, a gradual decline in memory and reasoning skills over time signals cognitive impairment.
By identifying the difference between delirium and dementia, caregivers can respond effectively, ensuring timely interventions for delirium and providing appropriate support for those experiencing cognitive decline. Here are some actionable steps:
- Monitor changes in behavior and mental state closely.
- Seek immediate medical attention for sudden confusion.
- Provide consistent support and routines for individuals with cognitive decline.
Recognizing these signs and acting promptly can make a significant difference in the care provided.
Compare Symptoms and Stages of Delirium and Dementia
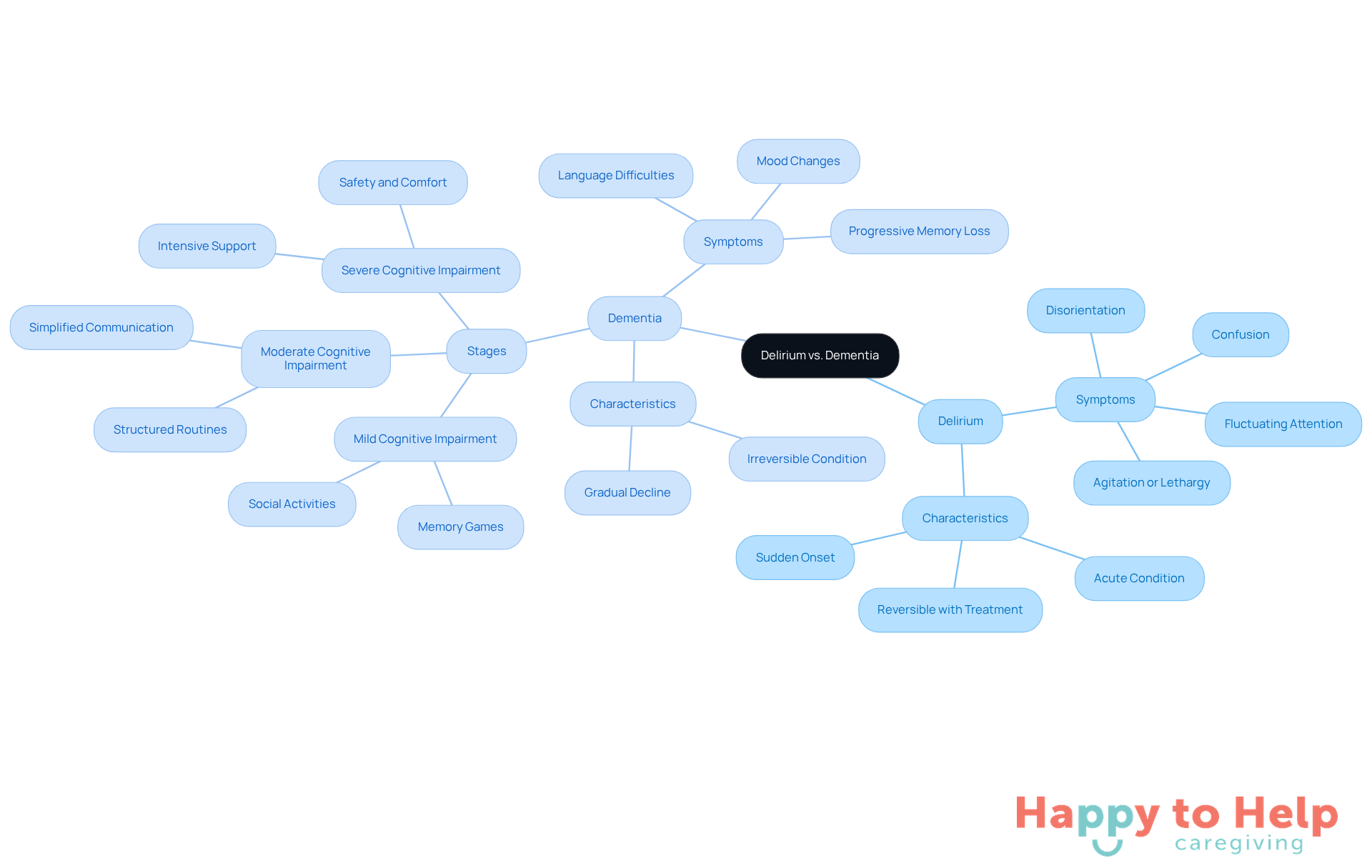
Understanding the difference between delirium and dementia presents a significant challenge for caregivers, characterized by sudden onset symptoms like confusion, disorientation, and fluctuating attention. These symptoms can manifest as either agitation or lethargy, making timely intervention crucial. This acute condition often improves with treatment of its underlying causes. In contrast, the cognitive decline associated with dementia unfolds gradually, highlighting the difference between delirium and dementia, with symptoms such as progressive memory loss, language difficulties, and notable changes in mood or behavior.
Cognitive decline typically progresses through three distinct stages:
- Mild cognitive impairment
- Moderate cognitive impairment
- Severe cognitive impairment
Each stage requires different levels of care and support, highlighting the importance of understanding the difference between delirium and dementia for effective caregiving. For instance, caregivers can apply specific methods tailored to each phase of cognitive decline. In the mild stage, engaging individuals in memory games and social activities can help maintain cognitive function. As the condition advances to moderate, caregivers might focus on creating structured routines and simplifying communication to reduce frustration. In advanced cognitive decline, ensuring safety and comfort becomes paramount, often necessitating more intensive support.
Statistics reveal that up to 75% of older adults may experience some form of confusion during hospitalization, underscoring the need for attentiveness in identifying symptoms. Furthermore, research indicates that 27% of individuals identified with confusion later receive a diagnosis of cognitive decline, emphasizing the difference between delirium and dementia. Non-drug approaches for managing confusion-such as promoting mobility, ensuring adequate nutrition and hydration, and offering reassurance-can also be beneficial. By recognizing the symptoms and stages of both confusion and dementia, caregivers can better tailor their strategies to meet the unique needs of those they care for, while remaining mindful of the potential risks associated with long-term use of psychotropic medications.
Identify Risk Factors and Causes of Delirium and Dementia
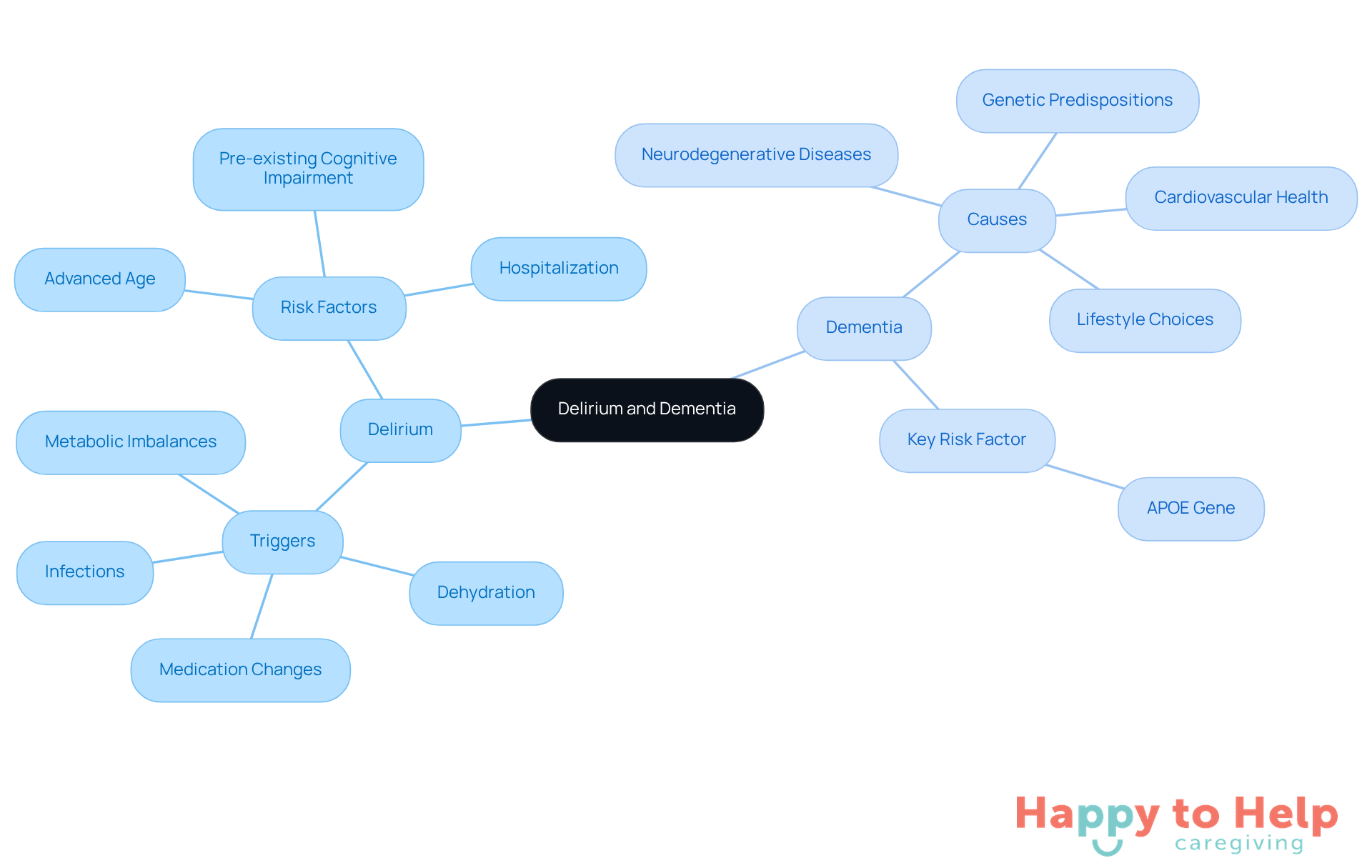
Understanding the difference between delirium and dementia is crucial, as delirium presents a significant challenge for caregivers, arising from various triggers such as infections, dehydration, medication changes, and metabolic imbalances. Alarmingly, about 25% of hospitalized older adults experience confusion, leading to prolonged hospital stays and increased mortality rates. Key risk factors include advanced age, pre-existing cognitive impairment, and hospitalization, making it crucial for caregivers to be aware of these issues.
In contrast, understanding the difference between delirium and dementia is important, as cognitive decline is primarily driven by neurodegenerative diseases, with Alzheimer's disease being the most prevalent. Factors such as genetic predispositions, cardiovascular health, and lifestyle choices significantly contribute to cognitive decline. Recent studies highlight the APOE gene as a notable genetic risk factor for confusion, increasing vulnerability even in individuals without dementia.
Understanding these causes is essential for caregivers. It enables them to recognize when to seek medical intervention and fosters a supportive environment for those affected. Healthcare experts emphasize that individuals with underlying brain vulnerabilities are particularly susceptible to confusion when faced with stressors. Therefore, careful observation and preventive care are vital.
Key Takeaways for Caregivers:
- Be aware of the signs of delirium and confusion.
- Understand the risk factors associated with cognitive decline.
- Foster a supportive environment to help mitigate stressors.
By implementing these strategies, caregivers can better support their loved ones and enhance their overall well-being.
Explore Caregiving Strategies for Delirium and Dementia
Challenges in Caregiving for Delirium and Dementia
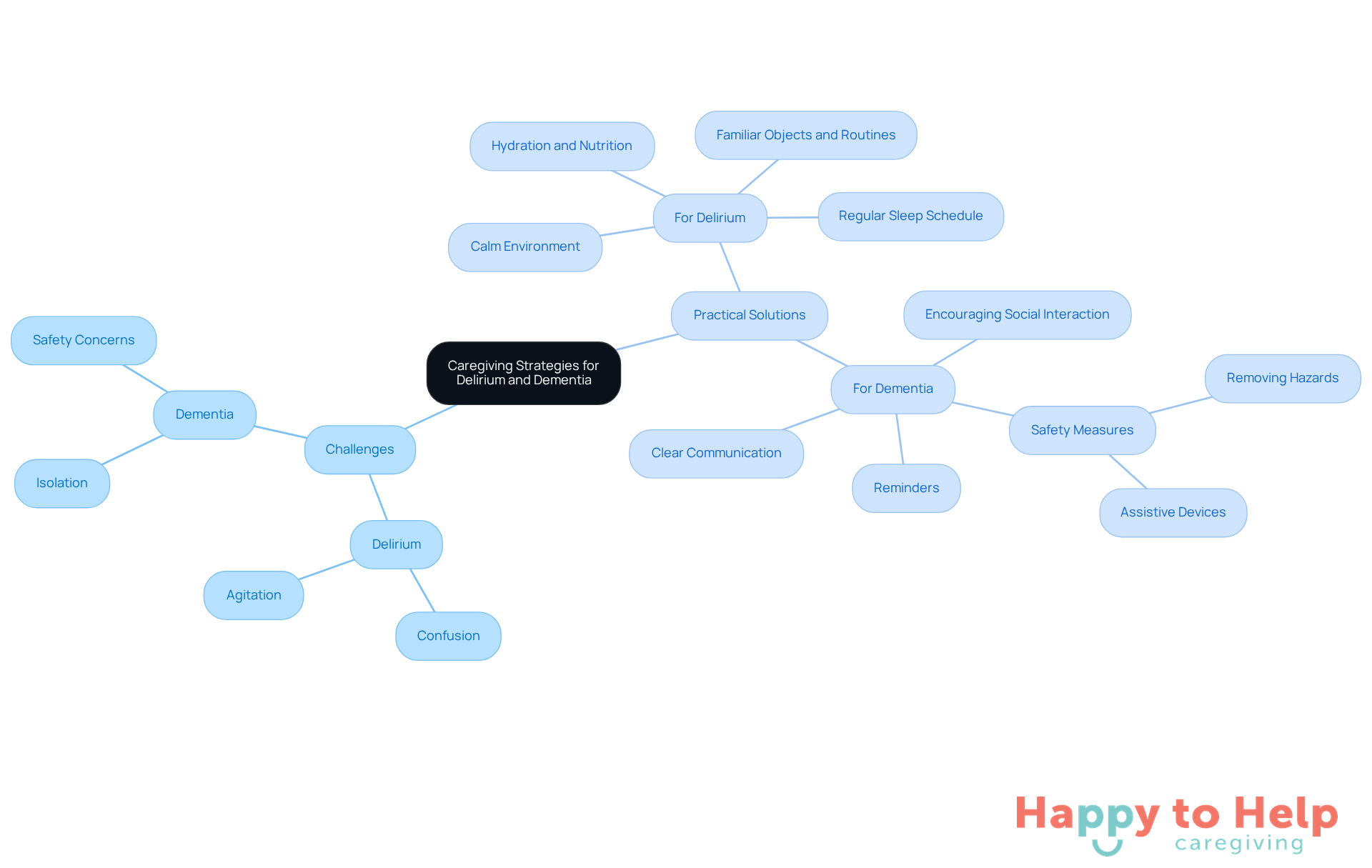
Caregivers often face significant challenges when caring for individuals with delirium and dementia. The difference between delirium and dementia is that delirium can lead to confusion and agitation, while dementia may result in isolation and safety concerns. These issues not only affect the individuals but also place a heavy emotional and physical burden on caregivers.
Practical Solutions for Caregivers
To address these challenges, caregivers can implement several effective strategies:
-
For delirium, creating a calm environment is crucial.
-
This includes ensuring proper hydration and nutrition, as well as maintaining a regular sleep schedule.
-
Engaging the person with familiar objects and routines can also help reduce confusion.
-
For dementia, clear communication is key.
-
Caregivers should provide reminders and encourage social interaction to combat feelings of isolation.
-
Additionally, prioritizing safety by removing hazards and considering assistive devices can significantly enhance the well-being of those in their care.
Tailoring Care to Individual Needs
Ultimately, tailoring these strategies to the individual's preferences and needs can greatly improve their quality of life. By focusing on these actionable solutions, caregivers can create a supportive environment that fosters comfort and safety.
Making the Right Choice
Understanding the nuances between delirium and dementia is essential for caregivers, as it directly influences the quality of care provided to individuals experiencing these conditions. Delirium is characterized by sudden confusion and fluctuating consciousness, often linked to acute medical issues. In contrast, dementia signifies a gradual decline in cognitive function, typically irreversible and progressive. Recognizing these distinctions empowers caregivers to respond appropriately, ensuring timely interventions for delirium and ongoing support for those facing cognitive decline.
Key points highlighted throughout the article include the symptoms and stages of both conditions, risk factors, and effective caregiving strategies. Caregivers are encouraged to:
- Monitor changes in behavior.
- Seek immediate medical attention for sudden confusion.
- Implement tailored support strategies for individuals with dementia.
Understanding the critical differences between these two conditions not only aids in effective caregiving but also fosters a supportive environment that addresses the unique needs of each individual.
Ultimately, the insights shared in this guide underscore the importance of vigilance and informed action in caregiving. By actively engaging in the recognition of symptoms and understanding the underlying causes of delirium and dementia, caregivers can significantly enhance the well-being of those they support. Embracing these practices improves care outcomes and fosters a compassionate approach that honors the dignity of individuals facing these challenging conditions.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5NDBhMjM5NGFiMmI4OGM4M2NiZjVjMSIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What is delirium?
Delirium is a condition characterized by sudden confusion, fluctuating consciousness, and impaired attention, often triggered by acute medical issues like infections or medication side effects.
How quickly can delirium develop?
Delirium can evolve rapidly, sometimes within hours or days.
What are the key characteristics of dementia?
Dementia is marked by a progressive deterioration in cognitive function, including memory loss, language difficulties, and impaired reasoning.
How does the progression of dementia differ from delirium?
Unlike delirium, which is acute and can resolve, dementia unfolds slowly over months or years and is typically permanent.
What percentage of cognitive impairment cases are attributed to Alzheimer's disease?
Alzheimer's disease accounts for about 70% of cognitive impairment cases.
Why is it important for caregivers to understand the difference between delirium and dementia?
Understanding the difference helps caregivers respond effectively, ensuring timely interventions for delirium and providing appropriate support for those experiencing cognitive decline.
What percentage of elderly individuals in acute care settings may experience confusion?
Confusion can affect up to 50% of elderly individuals in acute care settings.
What are some signs that may indicate delirium?
Signs of delirium include sudden confusion and disorientation, especially if linked to recent medical changes.
What should caregivers do if they notice sudden confusion in a family member?
Caregivers should seek immediate medical attention for sudden confusion.
How can caregivers support individuals experiencing cognitive decline?
Caregivers can provide consistent support and routines for individuals with cognitive decline.
List of Sources
- Define Delirium and Dementia: Key Characteristics
- Hospitals Must Better Identify And Manage Delirium In Seniors (https://forbes.com/sites/howardgleckman/2025/08/06/hospitals-must-better-identify-and-manage-delirium-in-seniors)
- Delirium, Dementia, and the Brain (https://hms.harvard.edu/news-events/publications-archive/brain/delirium-dementia-brain)
- Exploring Delirium, Dementia, and Frailty in Elderly Care (https://bioengineer.org/exploring-delirium-dementia-and-frailty-in-elderly-care)
- Your Genes May Predict Delirium Years Before It Happens (https://technologynetworks.com/genomics/news/your-genes-may-predict-delirium-years-before-it-happens-407395)
- Delirium vs. Dementia (https://health.usnews.com/senior-care/articles/delirium-vs-dementia)
- Compare Symptoms and Stages of Delirium and Dementia
- Delirium, Dementia, and the Brain (https://hms.harvard.edu/news-events/publications-archive/brain/delirium-dementia-brain)
- Delirium and dementia: Overlapping symptoms, but distinct syndromes - Norton Healthcare Provider (https://nortonhealthcareprovider.com/news/delirium-vs-dementia)
- Geriatrics Update Session Examines Lewy Body Dementia, Parkinson's Disease, Alzheimer's - UAMS News (https://news.uams.edu/2025/10/27/geriatrics-update-session-examines-lewy-body-dementia-parkinsons-disease-alzheimers)
- Delirium in the United States: Results From the 2023 Cross-Sectional World Delirium Awareness Day Prevalence Study (https://sciencedirect.com/science/article/pii/S2667296024000673)
- Delirium and the risk of developing dementia: a cohort study of 12 949 patients (https://jnnp.bmj.com/content/93/8/822)
- Identify Risk Factors and Causes of Delirium and Dementia
- APOE gene raises delirium risk even without dementia, global analysis reveals (https://medicalxpress.com/news/2025-11-apoe-gene-delirium-dementia-global.html)
- Study finds gene linked with risk of delirium | News | The University of Edinburgh (https://ed.ac.uk/news/study-finds-gene-linked-with-risk-of-delirium)
- Gene Discovery Reveals Hidden Risk Pathway for Delirium - Neuroscience News (https://neurosciencenews.com/genetics-delerium-29975)
- The Delirium Connection (https://alz.org/news/2023/the-delirium-connection)
- Study details independent role of Alzheimer's gene in causing delirium (https://thehindu.com/sci-tech/health/study-details-independent-role-of-alzheimers-gene-in-causing-delirium/article70341643.ece)
- Explore Caregiving Strategies for Delirium and Dementia
- Bridging the gap: Dementia communication strategies - Harvard Health (https://health.harvard.edu/mind-and-mood/bridging-the-gap-dementia-communication-strategies)
- Comparing Two Programs To Prevent Delirium in Hospitalized Older Adults (https://pcori.org/research-results/2022/comparing-two-programs-prevent-delirium-hospitalized-older-adults)
- Hospitals Must Better Identify And Manage Delirium In Seniors (https://forbes.com/sites/howardgleckman/2025/08/06/hospitals-must-better-identify-and-manage-delirium-in-seniors)
- New Study Finds Family and Caregivers Can Help Spot Post-Surgery Delirium Early (https://hebrewseniorlife.org/news/new-study-finds-family-and-caregivers-can-help-spot-post-surgery-delirium-early)
- Dementia and delirium in the ER: Providing better care for older patients | West Health (https://westhealth.org/news/dementia-and-delirium-in-the-er-providing-better-care-for-older-patients)