
What You Need to Know About Why Dementia Patients Eat Less and How
Dementia poses a significant challenge for caregivers, especially when it comes to managing the eating habits of those affected. As cognitive decline progresses, many individuals face a notable decrease in appetite. This often results in alarming weight loss and nutritional deficiencies, which can severely impact their overall health and well-being.
Understanding the reasons behind these changes is essential for caregivers who want to enhance the quality of life for their loved ones. By recognizing the complexities of appetite reduction in dementia patients, caregivers can better address these issues.
So, what strategies can be effectively implemented to create a supportive mealtime environment that encourages better eating habits in dementia patients?
Explore the Impact of Dementia on Appetite
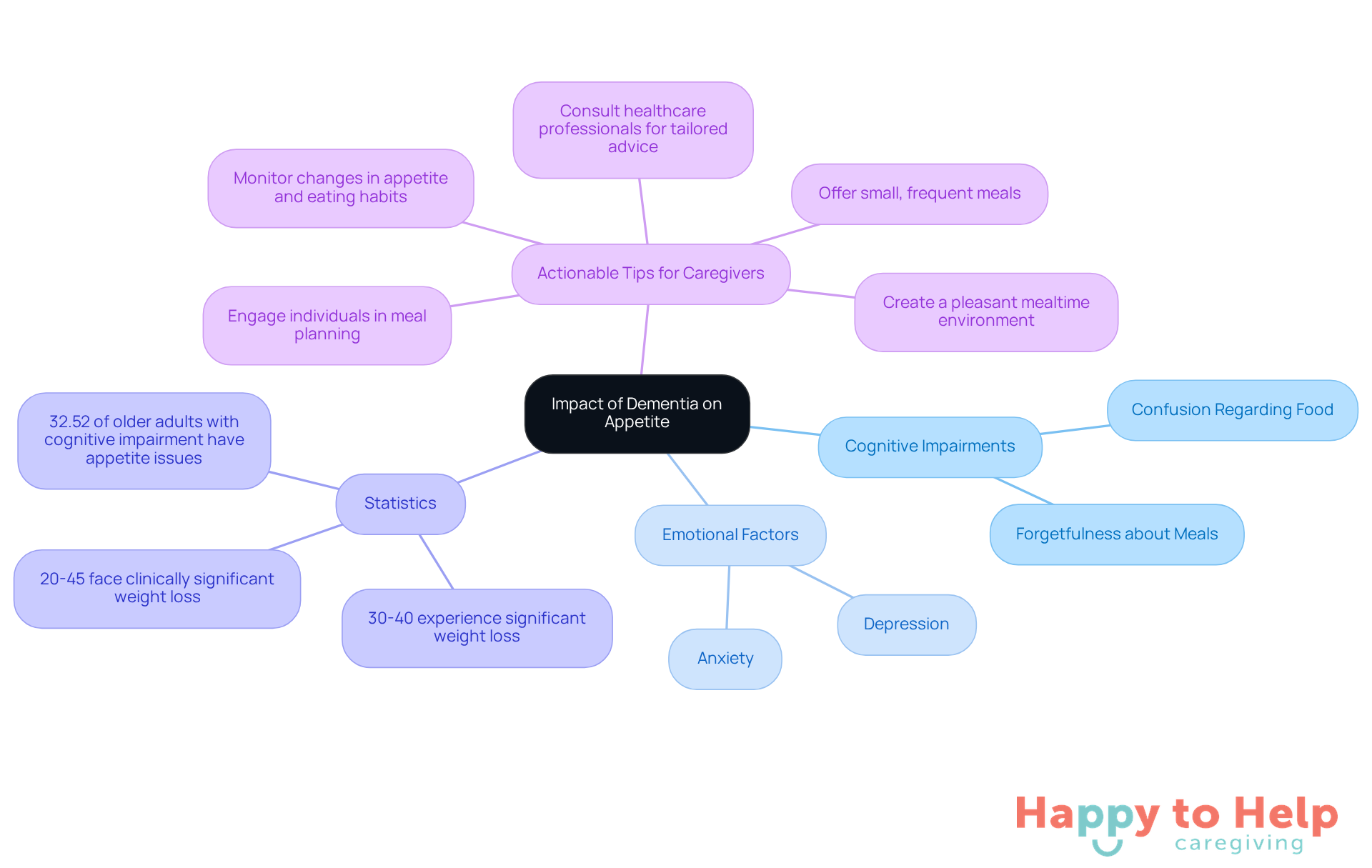
A significant challenge for caregivers in dementia is managing the issue of dementia eating less, particularly when it comes to appetite. As the condition progresses, dementia eating less often leads individuals to experience a decreased sense of taste and smell, diminishing the appeal of meals. Cognitive impairments can lead to forgetfulness about meals or confusion regarding food, which is often a factor in dementia eating less, as a person may not recognize food as something to eat or may forget they have already had a meal.
These issues are compounded by emotional factors such as depression and anxiety, which can contribute to dementia eating less by further suppressing appetite. This suppression can result in unintentional weight loss and nutritional deficiencies, particularly in individuals with dementia eating less. Alarmingly, statistics indicate that around 30-40% of individuals with cognitive impairment, particularly those with dementia eating less, experience considerable weight loss within a year, while 20-45% of those in the community face clinically significant weight loss over the same period. Additionally, 32.52% of older adults with cognitive impairment experience issues like dementia eating less, underscoring the urgency of addressing these challenges.
Loss of appetite, often seen as dementia eating less, can also signal depression, a common occurrence in individuals facing cognitive decline. Understanding these effects is crucial for caregivers. By recognizing the signs and implications of appetite loss, caregivers can implement suitable support methods and interventions to enhance the eating experience for those affected by cognitive impairment, particularly in cases of dementia eating less.
Actionable Tips for Caregivers:
- Monitor changes in appetite and eating habits.
- Create a pleasant mealtime environment to stimulate interest in food.
- Offer small, frequent meals that are easy to consume.
- Engage individuals in meal planning to encourage participation.
- Consult with healthcare professionals for tailored nutritional advice.
Identify Causes of Appetite Loss in Dementia
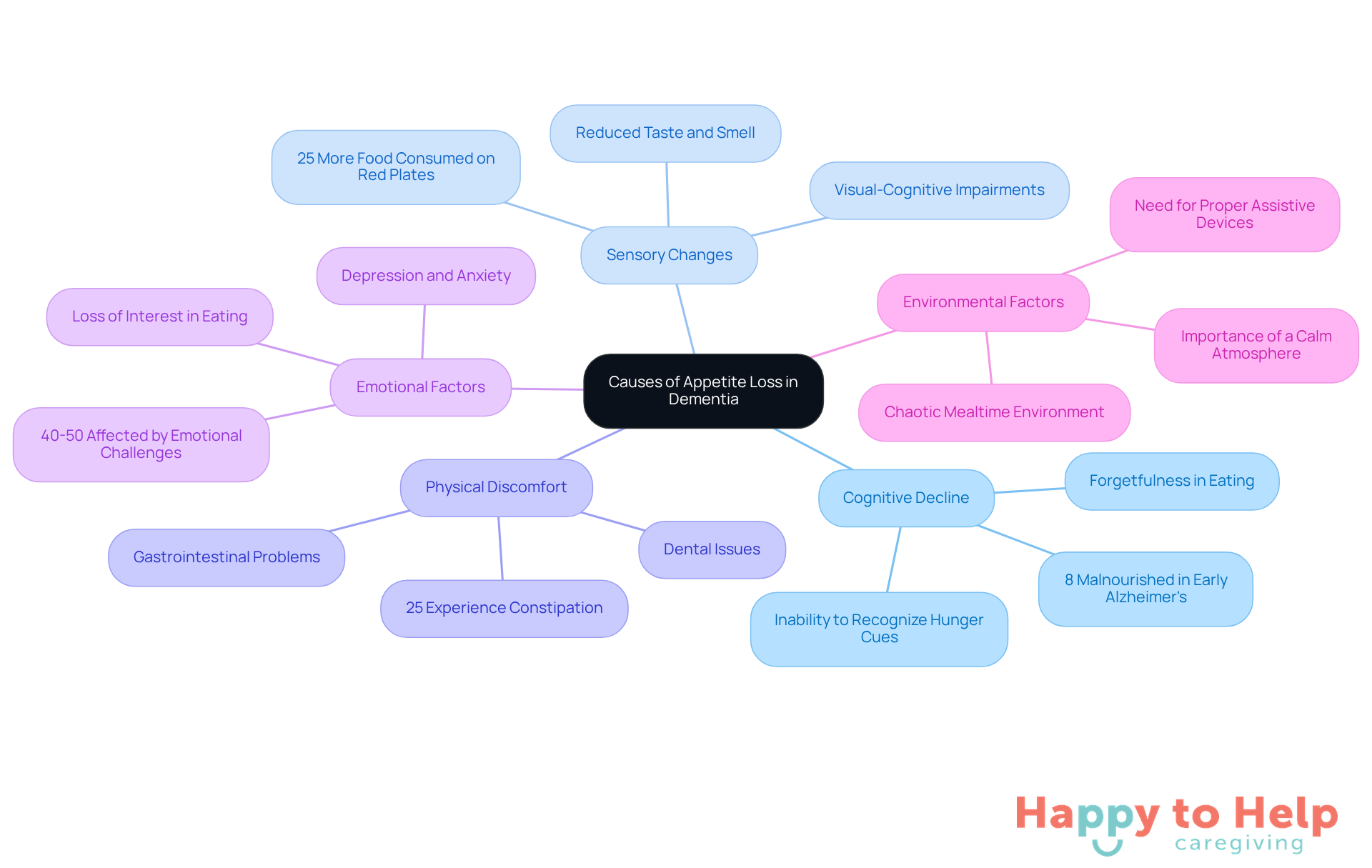
The challenge of dementia eating less poses significant difficulties for caregivers of individuals with dementia. This issue can stem from several interrelated factors that impact nutrition and overall health.
-
Cognitive Decline: As dementia progresses, individuals may forget to eat or struggle to recognize food, leading to missed meals and inadequate nutrition. Research shows that cognitive impairments can lead to dementia eating less, significantly influencing eating habits, with many patients unable to identify hunger cues or the need to eat. Alarmingly, 8% of patients in the early stages of Alzheimer's are already malnourished, underscoring the severity of this issue.
-
Sensory Changes: Reduced taste and smell are common in dementia patients, diminishing the pleasure of meals. These sensory impairments can lead to a decreased interest in eating, as individuals may not find food appealing. For example, patients often consume 25% more when meals are served on red plates, illustrating how visual stimuli can enhance appetite.
-
Physical Discomfort: Dental issues, such as ill-fitting dentures or oral pain, can make eating uncomfortable. Regular mouth checks and maintaining oral hygiene are essential to address pain-related eating issues. Additionally, gastrointestinal problems like constipation-which affects about 25% of individuals with cognitive impairment-can cause nausea and further deter nutritional intake. Encouraging fiber-rich foods and hydration can alleviate constipation and improve appetite.
-
Emotional Factors: Depression and anxiety are prevalent among those with dementia, impacting approximately 40-50% of patients. These emotional challenges can result in dementia eating less, as individuals may lose interest in activities they once enjoyed, including eating. Caregivers should consult a doctor to rule out medical reasons for refusal to eat, as this can provide critical insights into a person's health.
-
Environmental Factors: The mealtime environment plays a crucial role in encouraging or discouraging eating. A chaotic or uncomfortable setting can distract individuals, making them less inclined to engage with their food. Creating a calm and inviting atmosphere can help improve focus and reduce anxiety during meals. Ensuring that dentures, hearing aids, and glasses are in place before dining can also enhance the eating experience.
By understanding these causes, caregivers can implement targeted strategies to encourage better eating habits. Consider using colorful plates, ensuring a pleasant dining environment, serving small, frequent snacks, and addressing any physical discomfort that may hinder appetite.
Implement Strategies to Encourage Eating and Nutrition
To encourage eating and improve nutrition in dementia patients, caregivers face a significant challenge. Many individuals with dementia eating less struggle with mealtime routines, which leads to anxiety. This can have serious implications for their overall health and well-being.
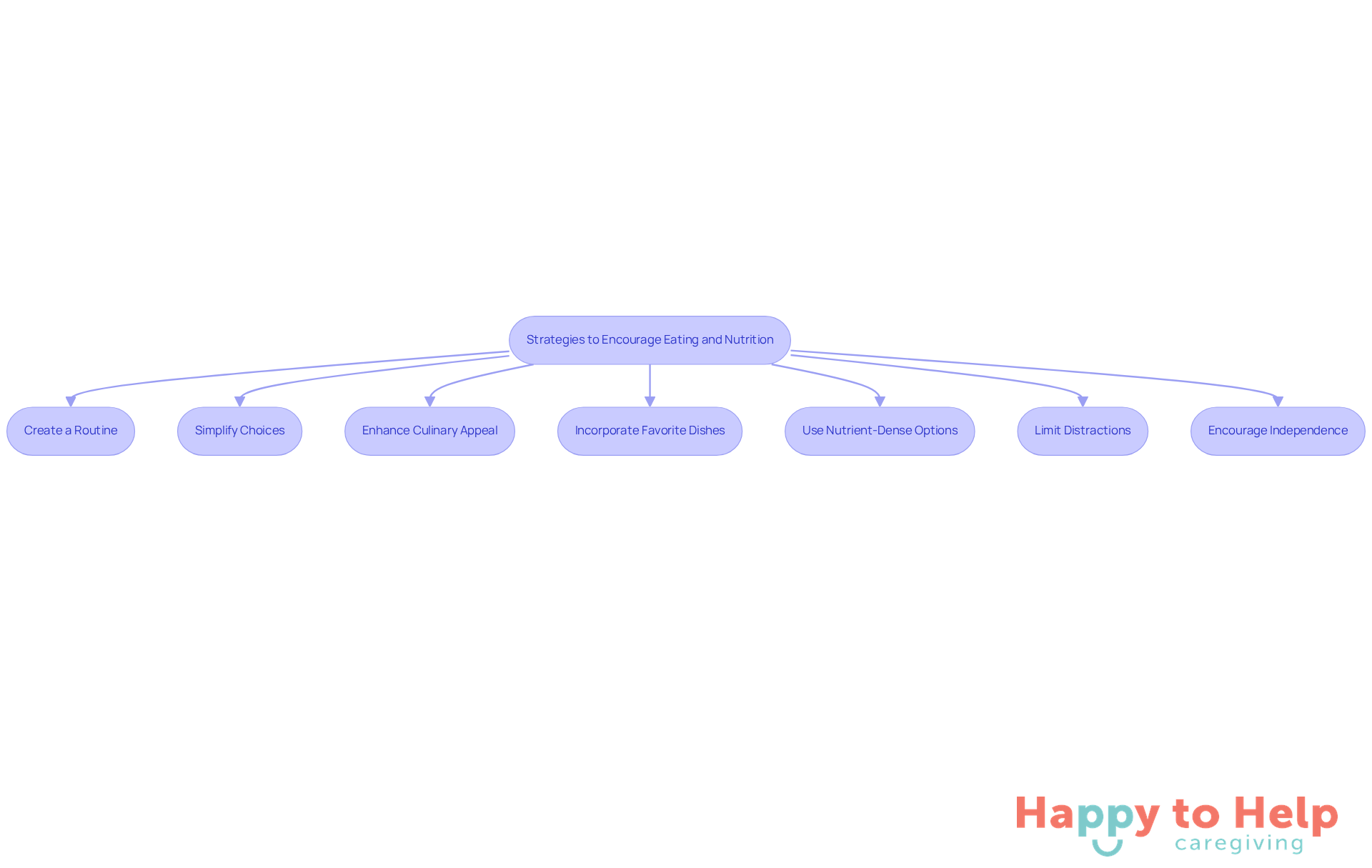
To address these issues, caregivers can implement several effective strategies:
- Create a Routine: Establishing regular meal times fosters structure and predictability, significantly reducing anxiety for individuals with dementia. Consistency in mealtime routines enhances willingness to eat, creating a comforting environment.
- Simplify Choices: Providing a limited variety of options can prevent overwhelming the individual, making decision-making easier. This approach often leads to more successful food participation.
- Enhance Culinary Appeal: Utilizing colorful plates and visually attractive presentations can stimulate interest in dishes. Studies show that appealing culinary presentations motivate people to engage more with their meals.
- Incorporate Favorite Dishes: Including familiar and enjoyable meals can encourage consumption. Celebrating small successes, such as finishing a meal, builds confidence and promotes future eating.
- Use Nutrient-Dense Options: Focusing on high-calorie, nutrient-rich items like smoothies, yogurt, and soups ensures adequate nutrition, even in smaller quantities. These options help preserve strength and health without burdening individuals, especially those with dementia eating less.
- Limit Distractions: Creating a serene mealtime atmosphere reduces noise and interruptions, allowing individuals to focus on their meals. This can significantly enhance their eating experience.
- Encourage Independence: Allowing individuals to eat at their own pace and using adaptive utensils promotes self-feeding. Finger foods and easy-to-handle options enhance their sense of autonomy during meals.
Implementing these strategies not only meets the nutritional needs of individuals with cognitive decline but also transforms mealtimes into opportunities for connection and enjoyment. As noted by Jenan Mohammad Jiménez, "Our aim was to develop a resource that is simple, practical, and accessible-something that caregivers can use in daily life." With over 80% of people with dementia in the U.S. living at home, these strategies are crucial for family caregivers. The toolkit developed by Macarena Espina Díaz and Jenan Mohammad Jiménez provides further assistance during mealtimes, emphasizing the importance of patience and understanding that eating can vary in difficulty from day to day.
Create a Comfortable and Supportive Mealtime Environment
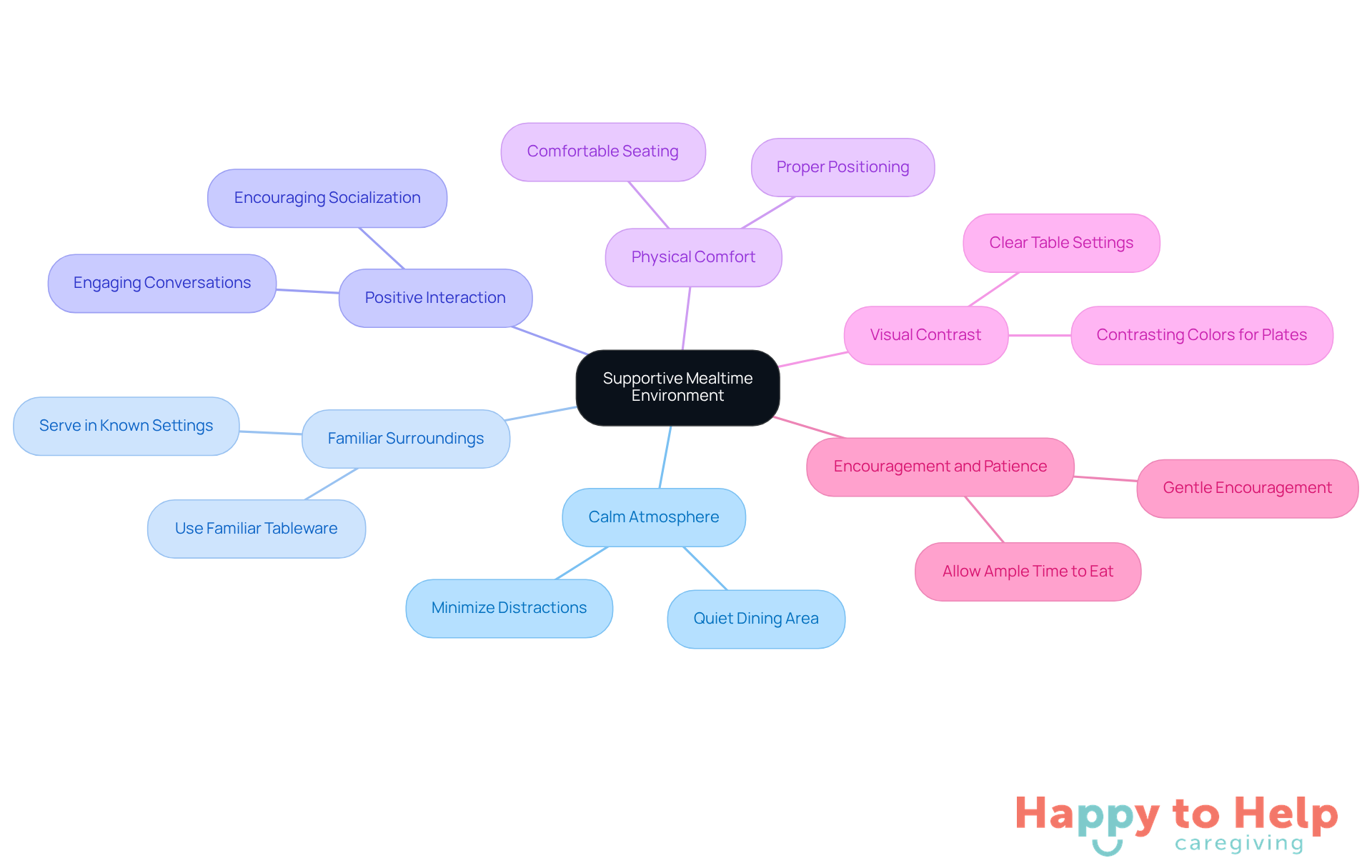
Creating a comfortable and supportive mealtime environment is essential for individuals, especially those with dementia eating less. A chaotic or distracting atmosphere can lead to anxiety and reluctance to eat, which is especially problematic for those with dementia eating less, making it crucial for caregivers to establish a calming setting.
-
Calm Atmosphere: Ensure the dining area is quiet and free from distractions, such as loud music or television. This helps create a peaceful environment that supports dementia eating less.
-
Familiar Surroundings: Serve food in a familiar setting to provide comfort and reduce anxiety. Familiarity can significantly enhance the mealtime experience, especially for individuals with dementia eating less.
-
Positive Interaction: Engage in pleasant conversation during meals. This not only creates a relaxed atmosphere but also encourages those with dementia eating less, making the experience more enjoyable.
-
Physical Comfort: Ensure that the seating is comfortable and that the person is positioned properly to eat. Physical comfort is key to enhancing the mealtime experience for those experiencing dementia eating less.
-
Visual Contrast: Use contrasting colors for plates and table settings. This helps the individual distinguish food from the background, making it easier to focus on eating.
-
Encouragement and Patience: Offer gentle encouragement and be patient. Allow the individual ample time to eat without feeling rushed, as dementia eating less can be a significant issue. Celebrate small successes to boost their confidence and willingness to eat.
Moving Forward with Why Dementia Patients Eat Less and How
Understanding the complexities surrounding why individuals with dementia eat less is crucial for caregivers striving to enhance the quality of life for their loved ones. Diminished appetite in dementia patients arises from various factors, including cognitive decline, sensory changes, emotional challenges, and environmental influences. Recognizing these elements empowers caregivers to take informed actions that can significantly improve mealtime experiences.
Key strategies to address this issue include:
- Creating a structured mealtime routine: Consistency can help patients feel more secure and engaged during meals.
- Simplifying food choices: Offering fewer options can reduce overwhelm and encourage eating.
- Enhancing the appeal of meals: Attractive presentation and familiar flavors can stimulate appetite.
- Fostering a calm and supportive dining environment: A peaceful setting can make mealtimes more enjoyable.
By implementing these approaches, caregivers can help mitigate the negative effects of appetite loss, ensuring that individuals with dementia receive the nutrition they need while also enjoying their meals.
Ultimately, addressing the issue of dementia eating less is not just about nutrition; it is about nurturing connections and creating meaningful moments during mealtimes. Caregivers are encouraged to embrace patience and understanding, recognizing that each day presents unique challenges. By fostering a supportive environment and utilizing effective strategies, caregivers can make a significant difference in the lives of those affected by dementia, reinforcing the importance of compassionate care in navigating this complex journey.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5MjEwYWJlY2E3OGI5ZDliYTJkYTUyYiIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What is a significant challenge for caregivers of individuals with dementia regarding appetite?
A significant challenge is managing the issue of dementia eating less, which often occurs as the condition progresses and leads to a decreased sense of taste and smell.
How do cognitive impairments affect eating habits in individuals with dementia?
Cognitive impairments can lead to forgetfulness about meals or confusion regarding food, causing individuals to not recognize food as something to eat or to forget that they have already had a meal.
What emotional factors can contribute to decreased appetite in individuals with dementia?
Emotional factors such as depression and anxiety can suppress appetite, leading to dementia eating less.
What are the potential consequences of decreased appetite in individuals with dementia?
The suppression of appetite can result in unintentional weight loss and nutritional deficiencies, with statistics showing that 30-40% of individuals with cognitive impairment may experience considerable weight loss within a year.
How prevalent is the issue of decreased appetite among older adults with cognitive impairment?
Approximately 32.52% of older adults with cognitive impairment experience issues related to dementia eating less.
What might loss of appetite indicate in individuals facing cognitive decline?
Loss of appetite can signal depression, which is common in individuals experiencing cognitive decline.
What can caregivers do to support individuals with dementia who are eating less?
Caregivers can monitor changes in appetite, create a pleasant mealtime environment, offer small and frequent meals, engage individuals in meal planning, and consult with healthcare professionals for tailored nutritional advice.
List of Sources
- Explore the Impact of Dementia on Appetite
- Can Dementia Cause Weight Loss? | Sewell, NJ (https://junipercommunities.com/can-dementia-cause-weight-loss)
- ADI - Nutrition and dementia (https://alzint.org/resource/nutrition-and-dementia)
- Meta-analysis and moderator analysis of the prevalence of malnutrition and malnutrition risk among older adults with dementia (https://sciencedirect.com/science/article/abs/pii/S0020748923002134)
- Appetite and dementia (https://alzheimers.org.uk/get-support/living-with-dementia/poor-appetite-dementia)
- Eating and dementia (https://dementia.org.au/living-dementia/home-life/eating-and-dementia)
- Identify Causes of Appetite Loss in Dementia
- Poor Appetite in Your Alzheimer’s Patients? (https://guidestareldercare.com/blog/poor-appetite-in-your-alzheimers-patients)
- Dementia and Appetite: Is Your Loved One with Dementia Not Eating? (https://lidementia.org/dementia-and-appetite)
- Dementia and appetite loss: Causes and management (https://medicalnewstoday.com/articles/dementia-patient-not-eating)
- Why do Dementia Patients Not Want to Eat? - Helpful Tips (https://wehelpcaregivers.com/news/dementia-refuses-to-eat)
- Appetite Loss in Memory Care: Warning Signs & Solutions (https://irisseniorliving.com/senior-living/tx/dallas/dickason-ave/blog/appetite-loss-in-memory-care-warning-signs-solutions)
- Implement Strategies to Encourage Eating and Nutrition
- Tips for Caregivers: Helping People With Alzheimer’s Disease Eat Well (https://nia.nih.gov/health/alzheimers-caregiving/tips-caregivers-helping-people-alzheimers-disease-eat-well)
- Fostering the Enjoyment of Eating through Inclusive Strategies for People Living with Dementia | Global Brain Health Institute (https://gbhi.org/news-publications/fostering-enjoyment-eating-through-inclusive-strategies-people-living-dementia)
- Helping caregivers help people with dementia eat at home (https://news.osu.edu/helping-caregivers-help-people-with-dementia-eat-at-home)
- Dementia And Eating Issues: How To Help Your Loved One Eat More - NCCDP (https://nccdp.org/dementia-and-eating-issues-how-to-help-your-loved-one-eat-more)
- 7 Caretaker Tips for Getting Dementia Patients to Eat (https://verywellhealth.com/how-to-get-dementia-patients-to-eat-11711215)
- Create a Comfortable and Supportive Mealtime Environment
- Supporting someone with dementia to eat and drink (https://alzheimers.org.uk/get-support/living-with-dementia/improving-eating-experience-dementia)
- Food & Eating | Alzheimer's Association (https://alz.org/help-support/caregiving/daily-care/food-eating)
- Supporting Nutrition and Hydration | Dementia Adventure (https://dementiaadventure.org/news/supporting-nutrution-and-hydration)
- The Benefits of Specialized Dining for Seniors with Dementia (https://blog.thebristal.com/specialized-dining-for-seniors-with-dementia)
- Fostering the Enjoyment of Eating through Inclusive Strategies for People Living with Dementia | Global Brain Health Institute (https://gbhi.org/news-publications/fostering-enjoyment-eating-through-inclusive-strategies-people-living-dementia)

