
For families in our service areas
For families in our service areas, this guide explains dementia care and how non-medical in-home caregiving can support care planning in East Idaho, Treasure Valley & Magic Valley, Northern Wasatch, North Central West Virginia, and Northeast Ohio.
Understanding What Happens When a Dementia Patient Can
Swallowing difficulties, known as dysphagia, pose a significant challenge for individuals with dementia, impacting their health and quality of life. As cognitive decline progresses, the ability to swallow often deteriorates, leading to serious complications like malnutrition and aspiration pneumonia. Caregivers are left to navigate these complexities, frequently questioning how to ensure safe and enjoyable mealtimes for their loved ones.
The implications of dysphagia are profound. Caregivers may feel overwhelmed by the responsibility of managing these issues, which can lead to increased stress and anxiety. The risk of malnutrition and aspiration pneumonia not only affects the patient's health but also diminishes their overall quality of life. So, what can caregivers do to effectively manage these swallowing difficulties?
Implementing practical strategies can significantly improve the well-being of dementia patients. Caregivers can focus on:
- Creating a safe mealtime environment
- Offering modified food textures
- Using adaptive utensils
Additionally, consulting with healthcare professionals for personalized guidance can provide valuable support. By taking these steps, caregivers can enhance mealtime experiences and promote better health outcomes for their loved ones.
Defining Swallowing Difficulties in Dementia Patients
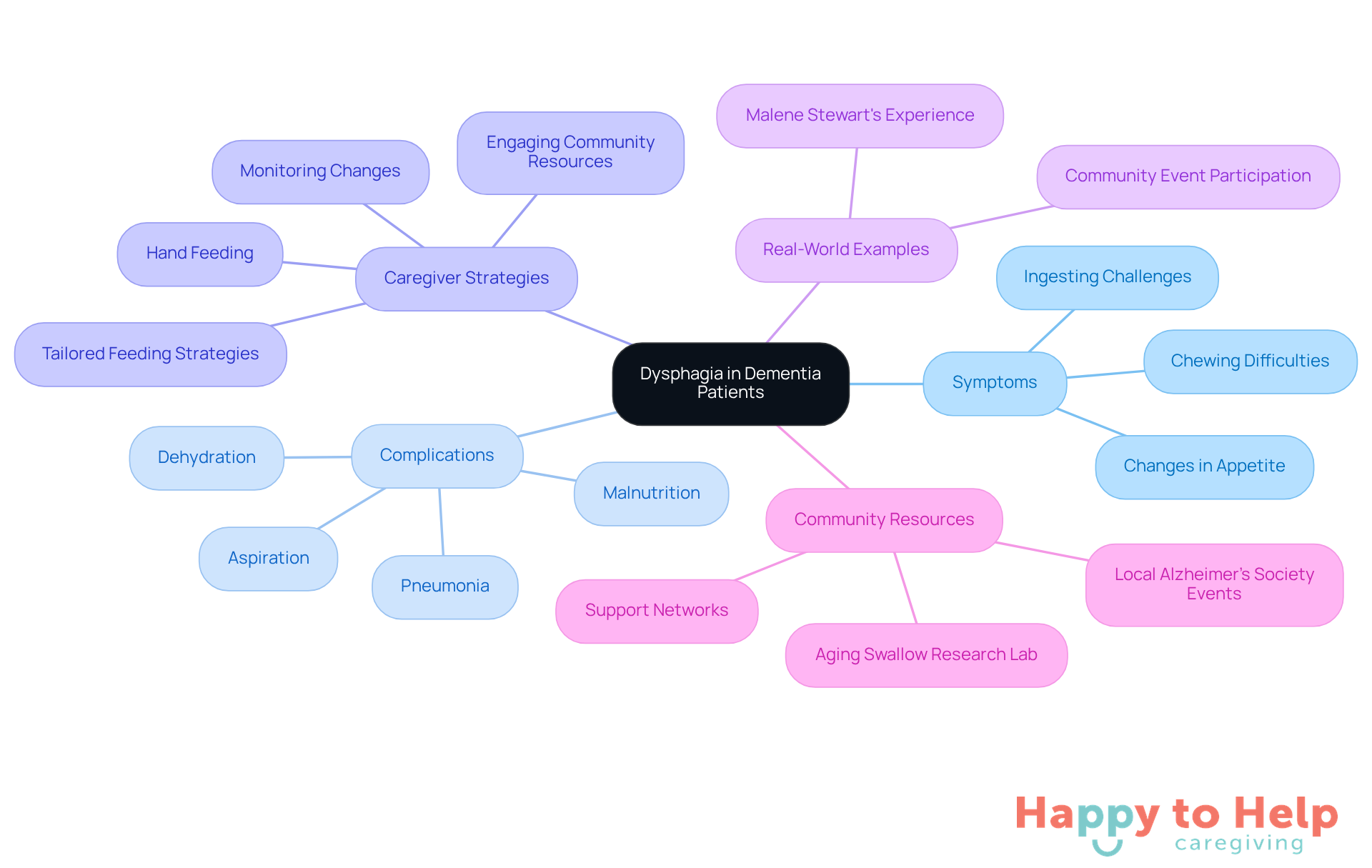
Swallowing difficulties, clinically known as dysphagia, pose a significant problem for individuals with dementia, raising questions about what happens when a dementia patient can't swallow, which impacts their health and well-being. This condition can manifest as challenges in chewing or ingesting food, leading to severe complications such as aspiration, where food or liquid mistakenly enters the airway. Such incidents can result in pneumonia, malnutrition, and dehydration, making it crucial for caregivers to recognize and address these issues promptly.
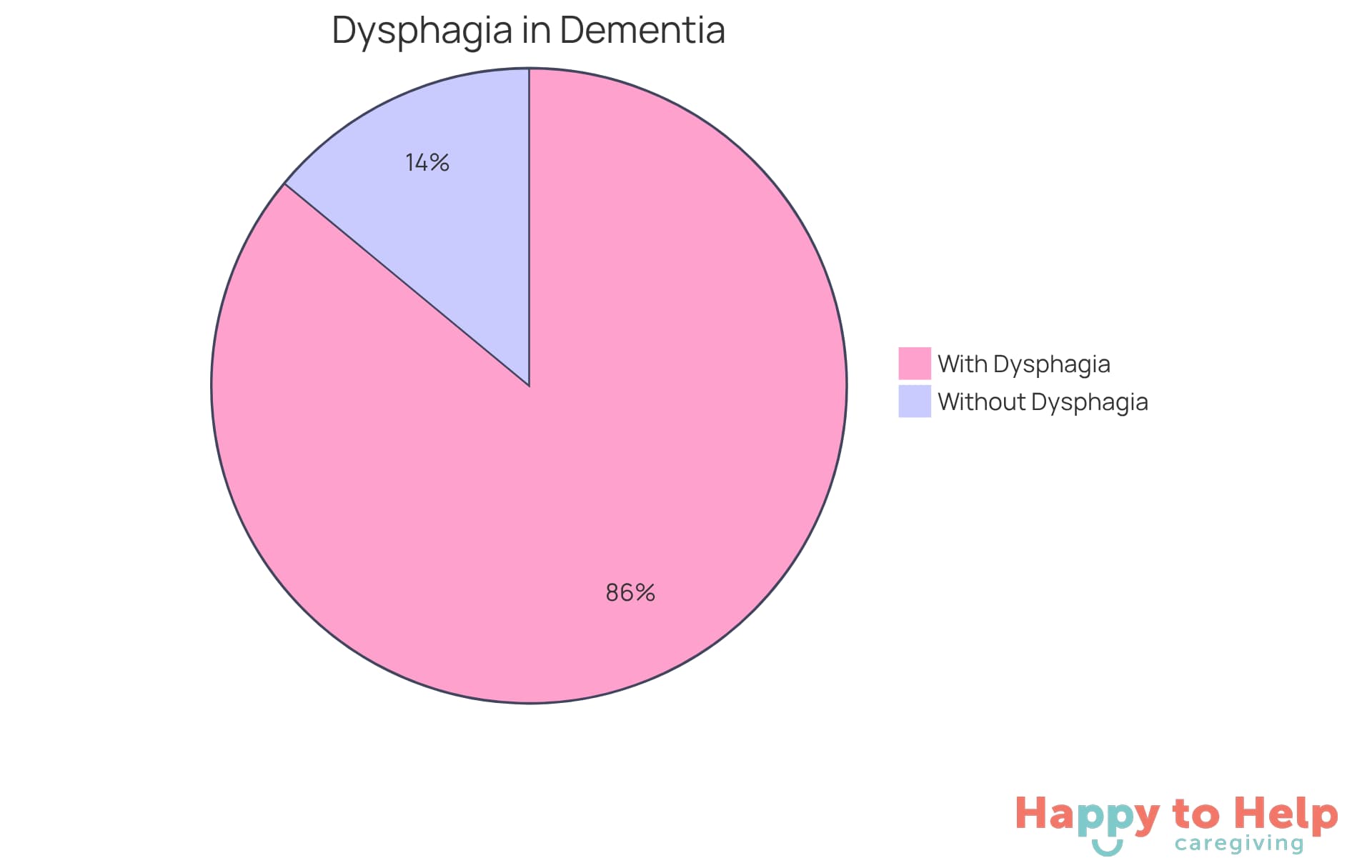
As cognitive decline progresses, it becomes crucial to understand what happens when a dementia patient can't swallow, as the coordination of muscles involved in swallowing deteriorates, complicating mealtime experiences. Research shows that up to 86 percent of hospitalized individuals with Alzheimer's disease and related dementias experience oropharyngeal dysphagia. This statistic underscores the urgent need for effective management strategies. Caregivers should be vigilant about changes in appetite, difficulties in recognizing hunger, and challenges in meal preparation, as these factors can worsen nutritional intake.
To tackle these challenges, assessing swallowing function and developing tailored feeding strategies is essential. Speech-language pathologists can offer valuable insights into safe feeding practices, ensuring patients receive adequate nutrition while minimizing aspiration risks. Additionally, caregivers are encouraged to engage in hand feeding, which can help alleviate hunger and strengthen emotional connections during meals.
Real-world examples illustrate the difficulties faced by caregivers. Malene Stewart, who supports her mother with Alzheimer's, participated in a swallowing study that assessed her mother's abilities and provided essential education and support. This experience not only expanded her support network but also highlighted the importance of community resources in managing dysphagia within cognitive impairment care.
It is vital for caregivers to understand dysphagia and what happens when a dementia patient can't swallow, as it directly impacts the nutritional intake and overall well-being of individuals with cognitive impairments. By recognizing the signs of eating challenges and seeking appropriate interventions, caregivers can significantly improve their loved ones' quality of life. With the number of people living with Alzheimer's projected to triple to 14 million by 2060, awareness and management of dysphagia will become increasingly critical. Caregivers are also encouraged to attend community events, such as the one scheduled for June 27, 2024, focusing on mealtime changes and nutrition, which will provide valuable insights and support.
Causes of Swallowing Problems in Dementia
The challenges with ingesting food in individuals with cognitive decline relate to what happens when a dementia patient can't swallow, stemming from neurological deterioration that disrupts the brain's ability to manage the ingesting process. As cognitive decline advances, it impacts critical brain areas responsible for this function, leading to weakened oral and pharyngeal muscles, mental deterioration, and sensory deficits that affect what happens when a dementia patient can't swallow.
Research shows that up to 86 percent of hospitalized patients with Alzheimer's disease and related dementias experience oropharyngeal dysphagia, highlighting the importance of understanding what happens when a dementia patient can't swallow. This statistic highlights the widespread nature of this issue. Environmental factors, such as interruptions during meals, can exacerbate these difficulties. Therefore, it is essential for caregivers to create a calm and attentive mealtime atmosphere.
It is crucial for caregivers to understand what happens when a dementia patient can't swallow. By doing so, they can implement effective feeding strategies that prioritize safety and comfort during mealtimes. Here are some actionable tips for caregivers:
- Establish a quiet environment free from distractions.
- Encourage slow eating to facilitate swallowing.
- Offer small, manageable bites to reduce the risk of choking.
By focusing on these strategies, caregivers can significantly improve the mealtime experience for individuals facing cognitive decline.
Implications of Inability to Swallow: Health Risks and Caregiver Challenges
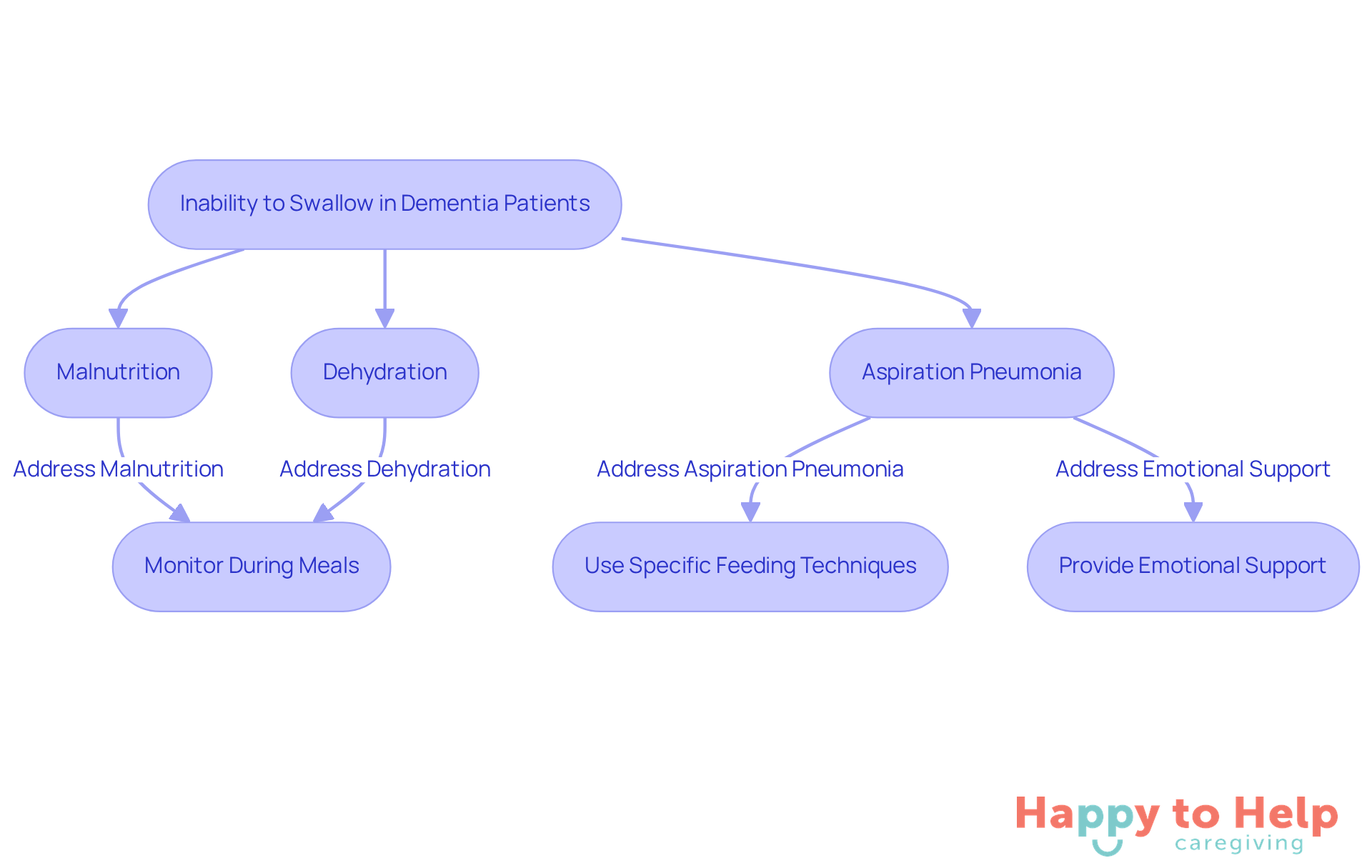
The inability to swallow effectively raises concerns about what happens when a dementia patient can't swallow, posing significant health risks for individuals with dementia. What happens when a dementia patient can't swallow can lead to malnutrition, dehydration, and aspiration pneumonia, ultimately resulting in a decline in overall health and quality of life.
Agitate: For caregivers, managing an individual with dysphagia is particularly challenging. It requires constant vigilance during meals and the implementation of specific feeding techniques to minimize risks. Additionally, caregivers must navigate the emotional aspects of feeding, as individuals may become frustrated or resistant to eating, complicating the caregiving process.
Solution: To address these challenges, caregivers can implement the following strategies:
- Monitor closely during meals: Stay attentive to the individual's swallowing abilities and adjust food textures accordingly.
- Use specific feeding techniques: Techniques such as offering small bites and encouraging slow eating can help reduce the risk of choking.
- Provide emotional support: Understanding and patience can ease frustration during mealtimes, making the experience more positive for both the caregiver and the individual.
Support Strategies for Caregivers Managing Swallowing Difficulties
Eating challenges in individuals with cognitive impairments pose significant risks, particularly regarding safety and comfort during meals. Dysphagia, or difficulty swallowing, is common in advanced stages of cognitive decline, highlighting what happens when a dementia patient can't swallow, which increases the risk of choking and aspiration. Caregivers face the daunting task of ensuring that mealtimes are both safe and enjoyable for their patients.
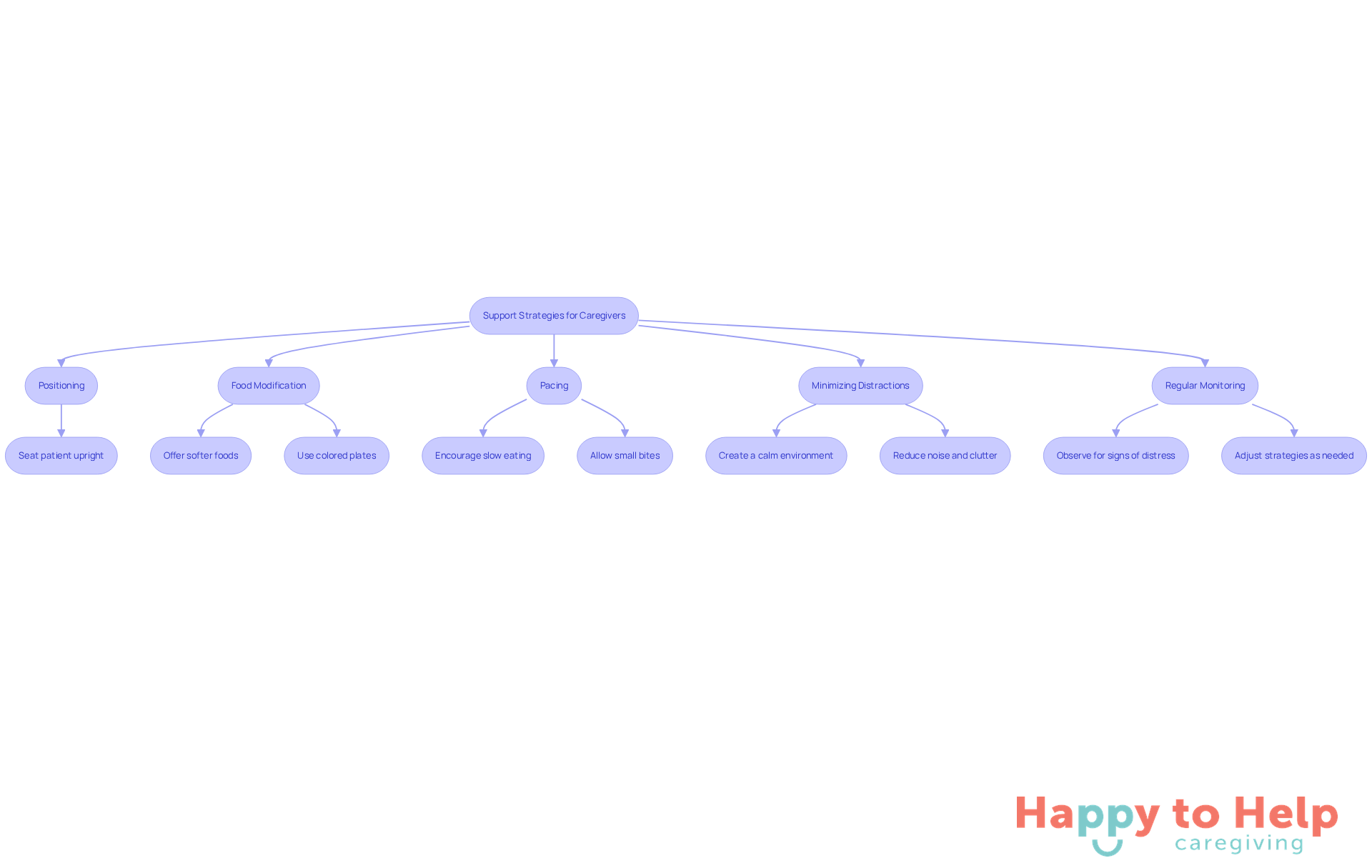
To address these challenges, caregivers can implement several effective strategies:
- Positioning: Ensure the patient is seated upright during meals. This positioning facilitates swallowing and reduces the risk of aspiration.
- Food Modification: Offer softer foods and thickened liquids that are easier to swallow, such as pureed fruits, yogurt, and smoothies. Using colored plates that contrast with the food can also help individuals with dementia see their meals more clearly, enhancing their mealtime experience.
- Pacing: Encourage slow eating and drinking. Allowing the patient to take small bites and sips helps prevent overwhelming them and promotes better control over swallowing. As caregivers note, "When eating is a pleasurable experience, they may be more open to eating."
- Minimizing Distractions: Create a calm eating environment by reducing noise and clutter. A tranquil setting can help the individual focus on eating, making mealtimes more enjoyable.
- Regular Monitoring: Observe for signs of aspiration or distress during meals, such as coughing or changes in breathing. Caregivers should be ready to adjust strategies as needed to ensure safety. Additionally, adaptive utensils with larger handles can assist individuals with dementia in gripping their cutlery, promoting independence during meals.
By employing these techniques, caregivers can significantly enhance the quality of life for patients with dysphagia, particularly in addressing what happens when a dementia patient can't swallow, making mealtimes safer and more comfortable.
Taking the Next Steps
Understanding the complexities of swallowing difficulties in dementia patients is essential for caregivers who strive to enhance their loved ones' quality of life. These challenges, often rooted in neurological decline, can lead to serious health risks such as malnutrition and aspiration pneumonia. Recognizing the signs of dysphagia and implementing effective feeding strategies can significantly improve mealtime experiences and overall well-being.
The problem is clear: swallowing difficulties can severely impact the health and comfort of dementia patients. Caregivers face the daunting task of managing these challenges, which can lead to frustration and concern. As the prevalence of Alzheimer's and related dementias continues to rise, the urgency to address these issues becomes even more critical.
To tackle this problem, caregivers can create a calm mealtime environment and utilize specific feeding techniques. Here are some actionable tips:
- Recognize the signs of dysphagia: Look for coughing, choking, or difficulty swallowing.
- Modify food textures: Offer softer foods that are easier to swallow.
- Encourage slow eating: Allow ample time for meals to reduce stress.
Real-world examples illustrate the importance of community resources and support networks in navigating these difficulties. Engaging with healthcare professionals and attending community events can provide valuable insights and foster a more compassionate caregiving approach.
By prioritizing awareness and proactive measures, caregivers can make a meaningful difference in the lives of those they care for. Addressing swallowing difficulties not only enhances the quality of life for dementia patients but also empowers caregivers with the knowledge and tools they need to provide effective support.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5MmY5MTlkY2E4MDg5MWIwMmZiMDBmOCIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What are swallowing difficulties in dementia patients?
Swallowing difficulties, clinically known as dysphagia, refer to challenges in chewing or ingesting food experienced by individuals with dementia, which can lead to severe complications like aspiration, pneumonia, malnutrition, and dehydration.
How common are swallowing difficulties in dementia patients?
Research indicates that up to 86 percent of hospitalized individuals with Alzheimer's disease and related dementias experience oropharyngeal dysphagia.
What factors should caregivers be aware of regarding swallowing difficulties?
Caregivers should monitor changes in appetite, difficulties in recognizing hunger, and challenges in meal preparation, as these can worsen nutritional intake for dementia patients.
What strategies can help manage swallowing difficulties in dementia patients?
Assessing swallowing function and developing tailored feeding strategies are essential. Speech-language pathologists can provide insights into safe feeding practices, and hand feeding can help alleviate hunger and strengthen emotional connections during meals.
Can you provide an example of caregiver experiences with swallowing difficulties?
Malene Stewart, who supports her mother with Alzheimer's, participated in a swallowing study that assessed her mother's abilities and provided essential education and support, highlighting the importance of community resources in managing dysphagia.
Why is it important for caregivers to understand dysphagia in dementia patients?
Understanding dysphagia is vital as it directly impacts the nutritional intake and overall well-being of individuals with cognitive impairments. Recognizing signs of eating challenges and seeking appropriate interventions can significantly improve quality of life.
What is the projected future of Alzheimer's disease and its relation to dysphagia?
The number of people living with Alzheimer's is projected to triple to 14 million by 2060, making awareness and management of dysphagia increasingly critical for caregivers.
Are there community resources available for caregivers dealing with dysphagia?
Yes, caregivers are encouraged to attend community events, such as the one scheduled for June 27, 2024, focusing on mealtime changes and nutrition, which will provide valuable insights and support.
List of Sources
- Defining Swallowing Difficulties in Dementia Patients
- Feinstein Institutes study challenges use of thick liquid diets in hospital patients with dementia and dysphagia (https://feinstein.northwell.edu/feinstein-institutes-study-challenges-use-of-thick-liquid-diets-in-dementia-dysphagia-patients)
- Researchers aim to ease mealtime challenges for dementia patients and caregivers (https://srs.healthsci.mcmaster.ca/researchers-aim-to-ease-mealtime-challenges-for-dementia-patients-and-caregivers)
- Patient Information: Eating and Swallowing Problems in People With Advanced Dementia (https://jamanetwork.com/journals/jama/fullarticle/2835480)
- 80 Quotes About Loving Someone With Alzheimer's (https://parade.com/1178790/kaitlin-vogel/alzheimers-quotes)
- Causes of Swallowing Problems in Dementia
- June is #DysphagiaAwareness Month - Dysphagia Expert Witness Services | Swallow Disorder Expert (https://swallowstudy.com/june-is-dysphagiaawareness-month)
- Feinstein Institutes study challenges use of thick liquid diets in hospital patients with dementia and dysphagia (https://feinstein.northwell.edu/feinstein-institutes-study-challenges-use-of-thick-liquid-diets-in-dementia-dysphagia-patients)
- Patient Information: Eating and Swallowing Problems in People With Advanced Dementia (https://jamanetwork.com/journals/jama/fullarticle/2835480)
- Dysphagia in Dementia: Causes & Symptoms | Stellar Care (https://stellarcaresd.com/about-us/blog/dysphagia-and-dementia)
- Three Common Medical Issues With Advanced Dementia - Compassion & Choices (https://compassionandchoices.org/news/three-common-medical-issues-with-advanced-dementia)
- Support Strategies for Caregivers Managing Swallowing Difficulties
- Simple Mealtime Strategies for Dementia Caregivers (https://physioinq.com.au/blog/simple-mealtime-strategies-for-dementia-caregivers)
- 7 Caretaker Tips for Getting Dementia Patients to Eat (https://verywellhealth.com/how-to-get-dementia-patients-to-eat-11711215)
- 5.1: Appendix A - Case Studies (https://med.libretexts.org/Bookshelves/Nutrition/Culinary\_Medicine\_2025e\_(Antonopoulos\_et\_al.)/05:\_Appendices/5.01:_Appendix\_A_\-\_Case\_Studies)
- CaringBridge (https://caringbridge.org/resources/inspirational-quotes-on-caregiving)