
Understanding What Happens When Dementia Patients
When dementia patients refuse food, the ramifications can be profound, presenting a daunting challenge for caregivers. This problem leads to significant nutritional decline, resulting in malnutrition and dehydration, which can accelerate cognitive deterioration and increase the risk of serious health complications.
Understanding the reasons behind appetite loss is essential for caregivers. The emotional and psychological factors at play can complicate the situation further. Caregivers must recognize these challenges to enhance the quality of life for their loved ones.
So, how can caregivers effectively navigate this complex landscape? Here are some actionable strategies:
- Engage in open communication: Talk to the patient about their preferences and feelings regarding food.
- Create a pleasant eating environment: Make mealtimes enjoyable and stress-free.
- Offer small, frequent meals: This can help manage appetite and make eating less overwhelming.
By implementing these strategies, caregivers can encourage eating while addressing the emotional aspects of food refusal.
Define the Consequences of Stopping Eating in Dementia Patients
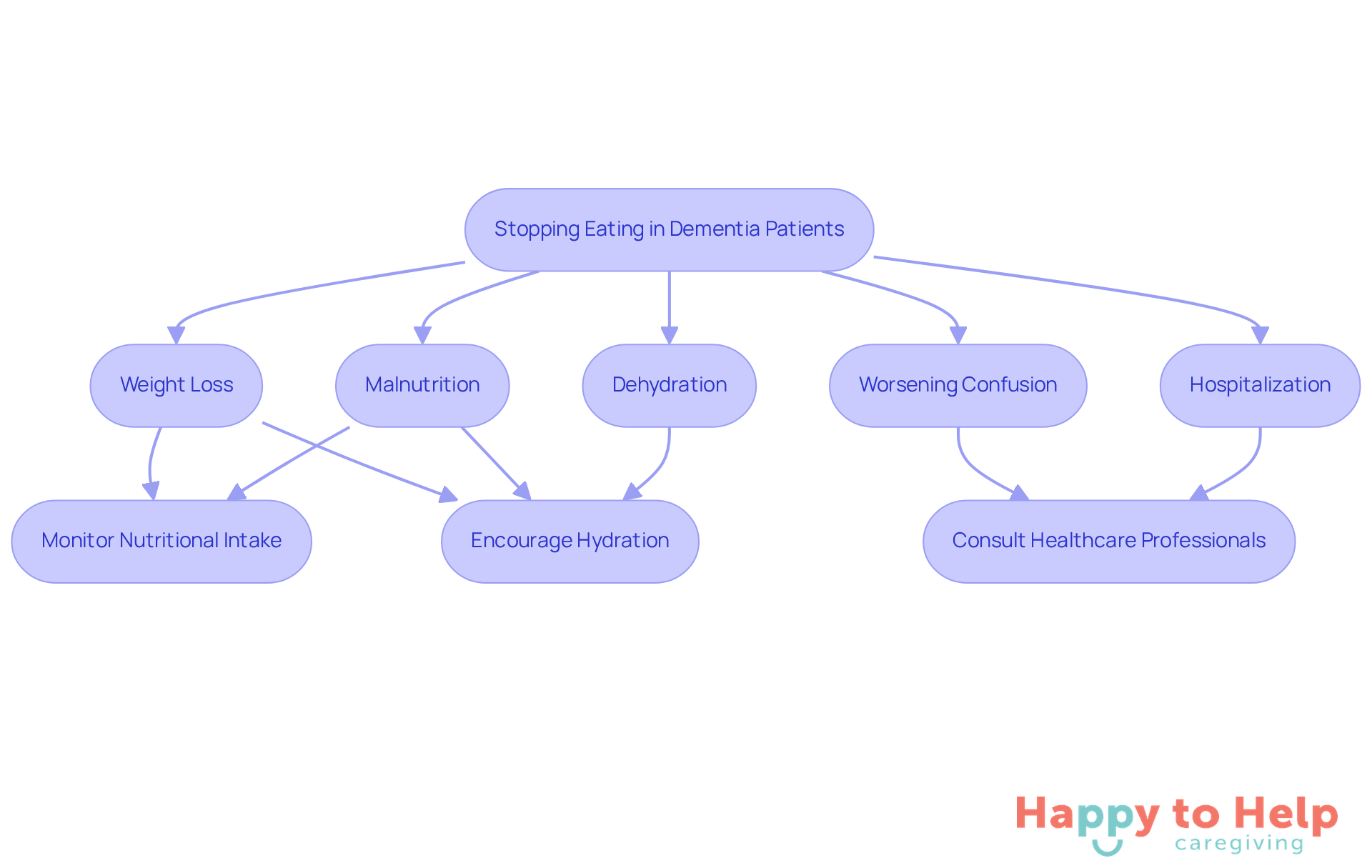
When individuals with cognitive decline stop eating, it creates serious challenges for caregivers, highlighting what happens when dementia patients stop eating. The most immediate problem is weight loss, which can lead to malnutrition and a decline in overall health. Without essential nutrients, patients may face weakened immune systems, increased susceptibility to infections, and further cognitive decline.
Moreover, what happens when dementia patients stop eating can include dehydration, worsening confusion, and potentially leading to hospitalization. In advanced stages, it is crucial to understand what happens when dementia patients stop eating, as this often signals the body shutting down and marks a critical phase in cognitive decline.
Understanding these consequences is crucial for caregivers. Here are some practical solutions:
- Monitor Nutritional Intake: Regularly assess the patient’s diet to ensure they receive necessary nutrients.
- Encourage Hydration: Offer fluids frequently to prevent dehydration and confusion.
- Consult Healthcare Professionals: Work with doctors or nutritionists to create tailored meal plans.
By recognizing these challenges and implementing supportive strategies, caregivers can significantly improve the quality of life for those experiencing cognitive decline.
Examine Reasons Behind Appetite Loss in Dementia Patients
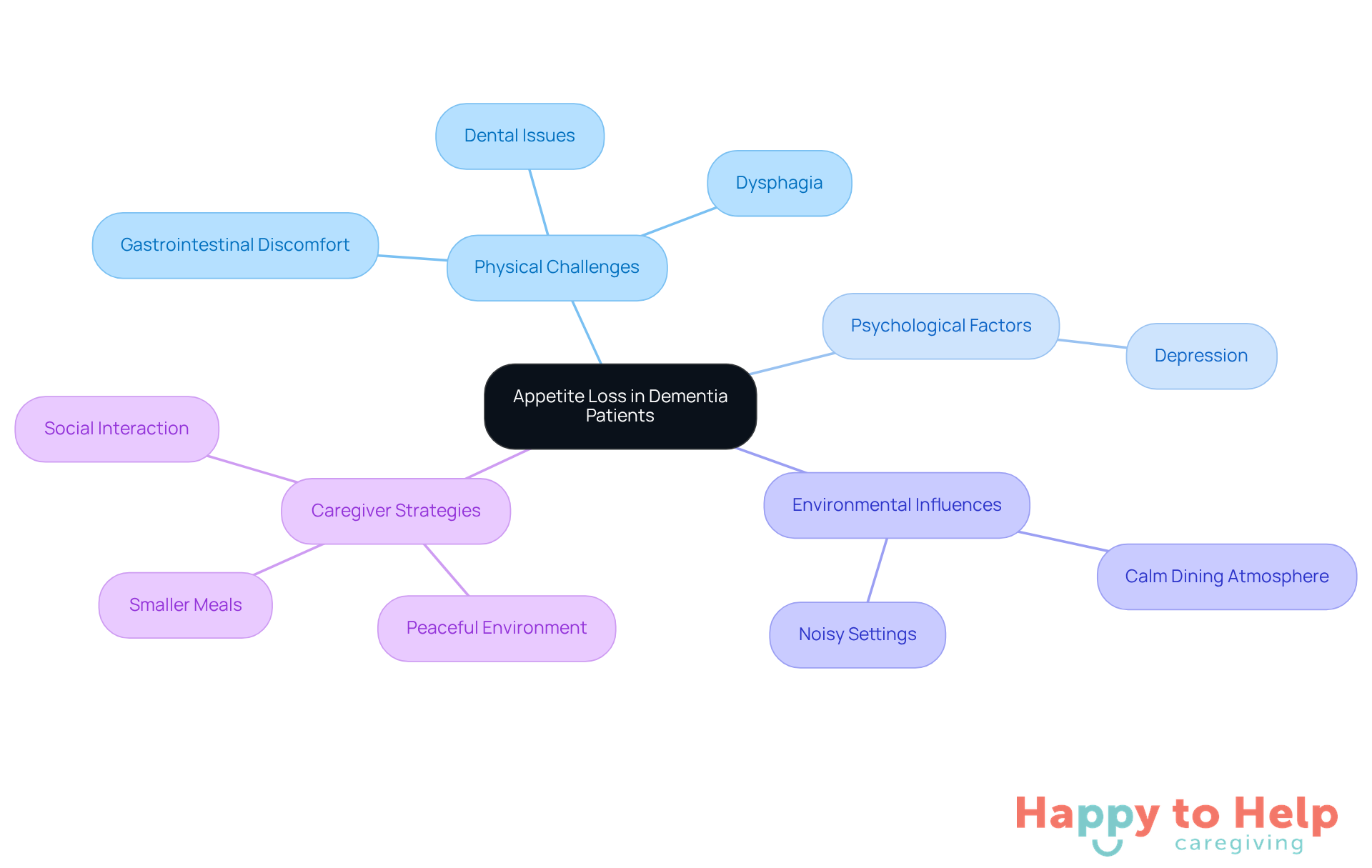
Appetite loss in individuals with cognitive decline presents a significant challenge for caregivers, especially considering what happens when dementia patients stop eating. This issue arises from a complex interplay of factors that hinder the ability to recognize meals and understand mealtime signals, often leading to what happens when dementia patients stop eating. Research indicates that many individuals experience reduced food and drink intake after transitioning to memory care settings, highlighting what happens when dementia patients stop eating, which can be concerning for families.
Several physical challenges exacerbate this problem. Dysphagia, or difficulty swallowing, affects a considerable number of individuals with cognitive decline, alongside dental issues and gastrointestinal discomfort. These factors can severely limit their ability to obtain adequate nutrition. Additionally, psychological aspects, such as depression-which impacts around 40% of those living with Alzheimer's disease-can significantly reduce the desire to eat, highlighting the importance of understanding what happens when dementia patients stop eating.
Environmental influences also play a crucial role in this scenario. Creating a calm dining atmosphere can enhance nutritional intake for memory care residents, while noisy or chaotic settings may turn mealtimes into stressful experiences rather than enjoyable ones.
To address these challenges, caregivers can implement several strategies:
- Create a peaceful dining environment: Minimize distractions to help residents focus on their meals.
- Encourage social interaction: Mealtime can be more enjoyable when shared with others, fostering a sense of community.
- Offer smaller, more frequent meals: This can make eating less overwhelming and more manageable.
Identifying and understanding these factors is essential for caregivers. By customizing their strategies, they can encourage improved eating habits and promote the overall well-being of their loved ones.
Analyze Health Risks Associated with Reduced Food Intake
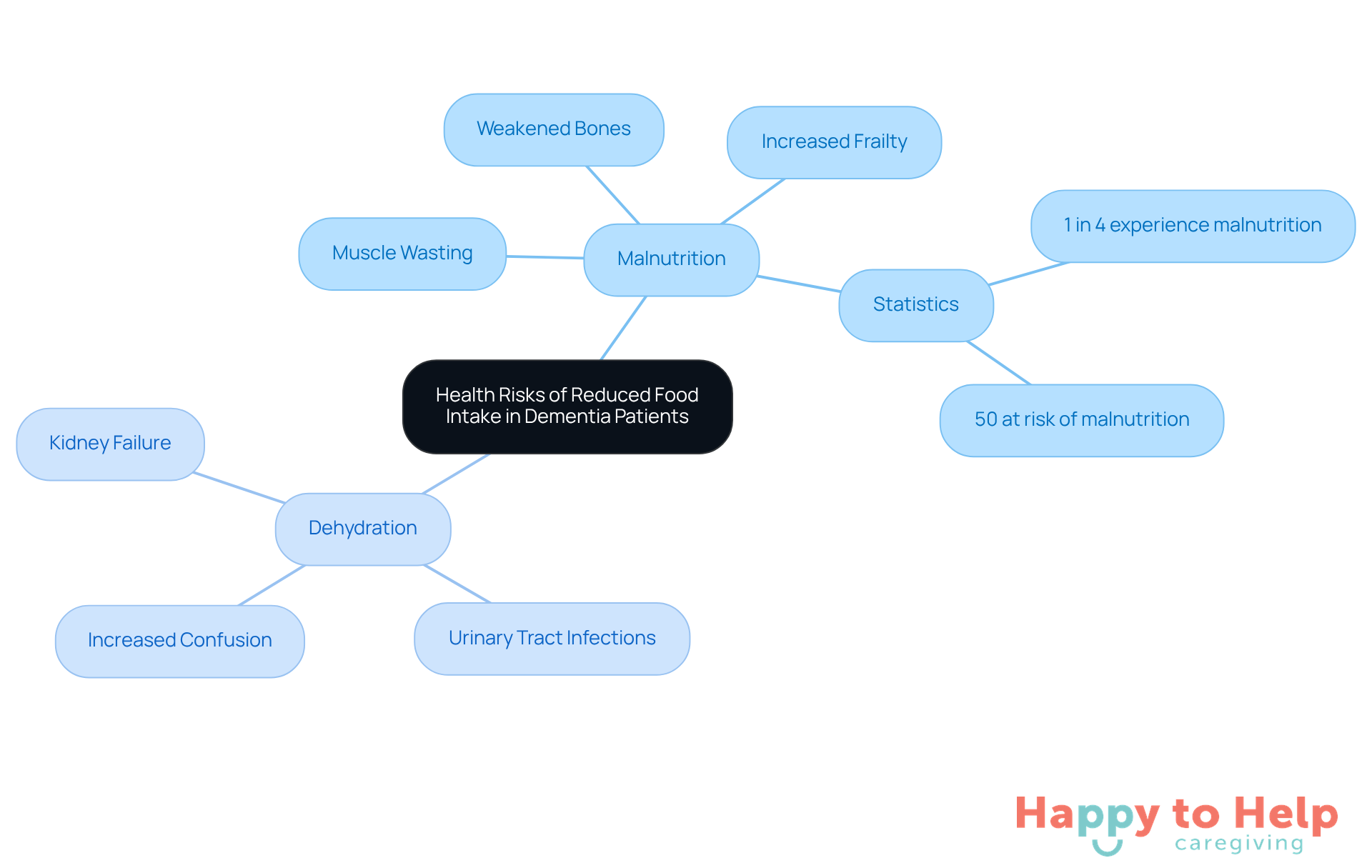
The health hazards linked to what happens when dementia patients stop eating are significant and can lead to serious outcomes.
-
Malnutrition is a primary concern, often resulting in muscle wasting, weakened bones, and increased frailty. This heightens the risk of falls and fractures. Statistics show that nearly one in four individuals with cognitive decline in long-term care facilities experience malnutrition, while almost 50% are at risk. This highlights the urgent need for caregivers to closely monitor nutrition intake.
-
Dehydration compounds these issues, potentially leading to kidney failure, urinary tract infections, and increased confusion, which further complicates the individual's overall condition. Nutrient deficiencies, especially in essential vitamins and minerals, can accelerate cognitive decline, underscoring the critical role of nutrition in brain health. In extreme cases, what happens when dementia patients stop eating can lead to life-threatening conditions, necessitating urgent medical intervention.
Caregivers must stay vigilant in recognizing the signs of malnutrition and dehydration. Early intervention can significantly reduce these risks and enhance the quality of life for their loved ones. Consulting a registered dietitian to create suitable dietary plans can also provide valuable support in addressing these challenges.
Explore Strategies for Supporting Dementia Patients Who Refuse Food
Assisting individuals with dementia presents a significant challenge for caregivers, particularly when considering what happens when dementia patients stop eating. This issue can lead to increased anxiety and a decline in the quality of life for those affected.
Agitate: Establishing a calming and familiar mealtime environment is crucial. A chaotic dining space can heighten anxiety and distract individuals from their meals. For instance, reducing background noise and visual distractions can help individuals focus better on eating. Additionally, large portions may overwhelm them, making the eating experience daunting.
Solution: To address these challenges, caregivers can implement several strategies:
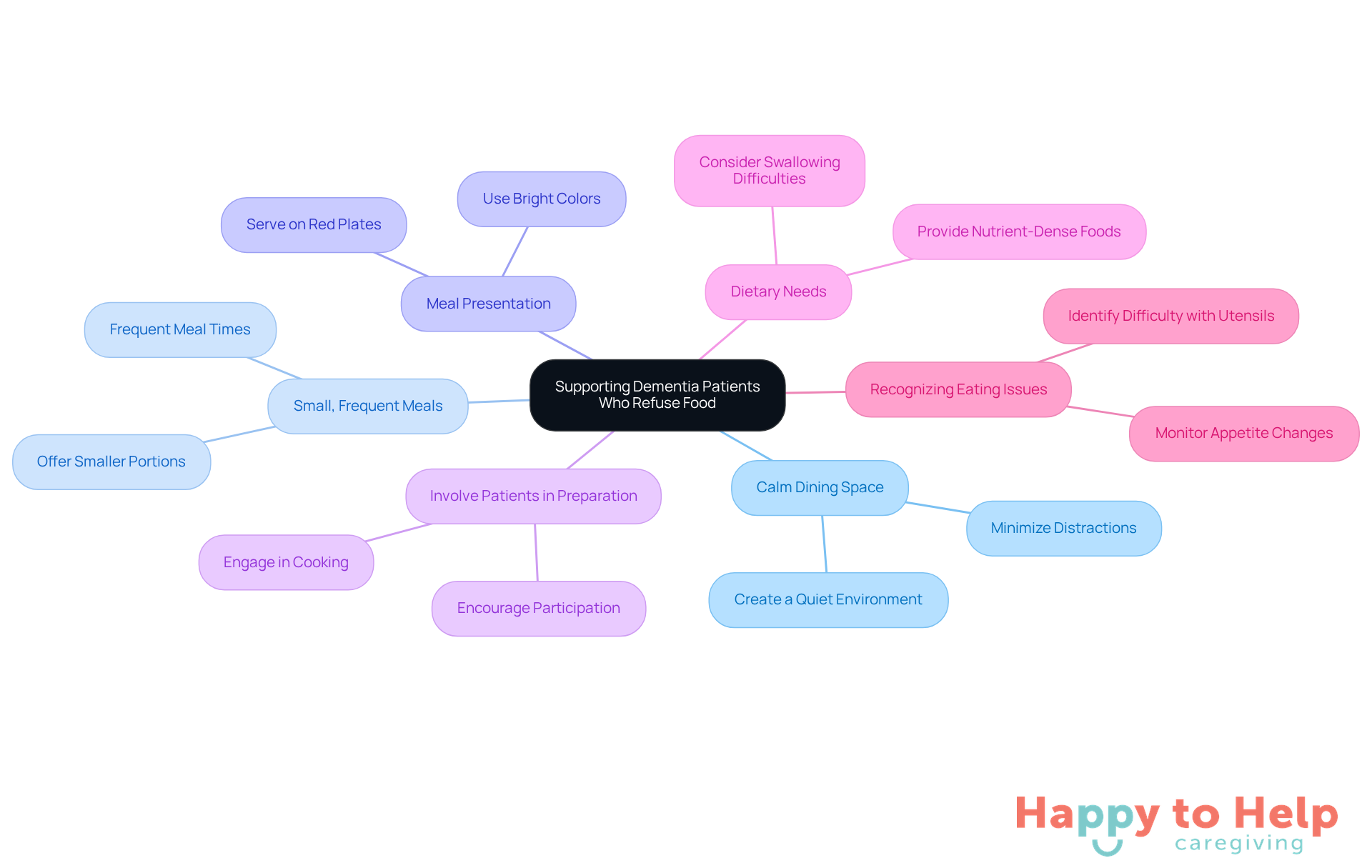
- Create a Calm Dining Space: Establish a serene environment that minimizes distractions.
- Offer Small, Frequent Meals: Instead of large portions, provide smaller meals throughout the day to make eating more manageable.
- Enhance Meal Presentation: Use lively colors and familiar tastes to stimulate interest. Research shows that serving meals on a red plate can increase consumption for individuals with Alzheimer's, making it a beneficial approach.
- Involve Patients in Meal Preparation: Engaging individuals in preparing their meals can strengthen their connection to food and motivate them to eat.
- Consider Dietary Needs: For those facing swallowing challenges, pureed foods or thickened liquids can ensure safety during meals.
Recognizing signs of eating issues, such as reduced appetite and difficulty using utensils, is essential for effective support. Maintaining a regular meal schedule offers organization and reliability, which is particularly beneficial for individuals with cognitive impairments. Community-focused nutrition initiatives, like Meals-on-Wheels, can provide additional resources for caregivers. By implementing these strategies, caregivers can foster a nurturing atmosphere that encourages dementia patients to eat, which is crucial to understanding what happens when dementia patients stop eating, ultimately enhancing their quality of life.
Key Takeaways for Caregivers
Understanding the implications of reduced food intake in dementia patients is vital for caregivers striving to maintain the health and well-being of their loved ones. The cessation of eating can lead to severe health consequences, including malnutrition and dehydration, which significantly impact overall health and cognitive function. Recognizing these challenges is crucial for caregivers as they navigate the complexities of supporting individuals with dementia.
Key insights reveal that appetite loss stems from various factors, including physical difficulties and psychological influences. Caregivers must be aware of these underlying issues to effectively address and mitigate them. Strategies such as:
- Creating a calm dining environment
- Offering smaller meals
- Involving patients in meal preparation
can foster a more positive eating experience. These approaches not only enhance nutritional intake but also improve the quality of life for individuals facing cognitive decline.
The significance of this topic cannot be overstated. By prioritizing nutrition and understanding the barriers to eating, caregivers can make a profound difference in the lives of dementia patients. Implementing thoughtful strategies and remaining vigilant about nutritional needs can lead to better health outcomes and a more fulfilling life for those affected by this challenging condition.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5NDBhMjNjOTc5ZjhiMGM0MmQzYjU4OSIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What are the immediate consequences of dementia patients stopping eating?
The immediate consequences include weight loss, malnutrition, and a decline in overall health, which can lead to a weakened immune system and increased susceptibility to infections.
How does stopping eating affect the cognitive health of dementia patients?
Stopping eating can lead to further cognitive decline due to a lack of essential nutrients.
What are some other serious effects of stopping eating in dementia patients?
Other serious effects include dehydration, worsening confusion, and potentially hospitalization.
What does it signify when dementia patients stop eating in advanced stages?
In advanced stages, stopping eating often signals the body shutting down and marks a critical phase in cognitive decline.
What strategies can caregivers implement to address the challenges of dementia patients who stop eating?
Caregivers can monitor nutritional intake, encourage hydration, and consult healthcare professionals to create tailored meal plans.
List of Sources
- Define the Consequences of Stopping Eating in Dementia Patients
- Meta-analysis and moderator analysis of the prevalence of malnutrition and malnutrition risk among older adults with dementia (https://sciencedirect.com/science/article/abs/pii/S0020748923002134)
- 'Aggressive' Advance Directive Permits Halting Food And Water In Severe Dementia (https://npr.org/sections/health-shots/2018/03/27/597499464/-aggressive-advance-directive-authorizes-stopping-food-in-cases-of-dementia)
- Malnutrition and Dementia: What Clinical Trials Are Revealing (https://researchforyou.co.uk/mac-news/malnutrition-and-dementia-what-clinical-trials-are-revealing)
- Prevalence of Malnutrition in People with Dementia in Long-Term Care: A Systematic Review and Meta-Analysis - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10343750)
- 2023: New research reveals high rates of malnutrition in people living with dementia in long-term care - University of Wollongong – UOW (https://uow.edu.au/media/2023/new-research-reveals-high-rates-of-malnutrition-in-people-living-with-dementia-in-long-term-care.php)
- Examine Reasons Behind Appetite Loss in Dementia Patients
- Appetite Loss in Memory Care: Warning Signs & Solutions (https://irisseniorliving.com/senior-living/tx/dallas/dickason-ave/blog/appetite-loss-in-memory-care-warning-signs-solutions)
- Dementia and appetite loss: Causes and management (https://medicalnewstoday.com/articles/dementia-patient-not-eating)
- Why do Dementia Patients Not Want to Eat? - Helpful Tips (https://wehelpcaregivers.com/news/dementia-refuses-to-eat)
- Dementia severity and weight loss: A comparison across eight cohorts. The 10/66 study - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC3898277)
- Analyze Health Risks Associated with Reduced Food Intake
- Alzheimer's: Malnutrition may drive onset of disease (https://medicalnewstoday.com/articles/does-nutrition-affect-alzheimers-disease-progression)
- Risk of malnutrition on the rise among older adults in Singapore, hospitals warn (https://channelnewsasia.com/singapore/malnutrition-risk-rise-older-adults-seniors-elderly-5387721)
- Is food insecurity among older adults associated with higher subsequent dementia risk and memory decline? (https://news-medical.net/news/20231122/Is-food-insecurity-among-older-adults-associated-with-higher-subsequent-dementia-risk-and-memory-decline.aspx)
- Malnutrition and Dementia: What Clinical Trials Are Revealing (https://researchforyou.co.uk/mac-news/malnutrition-and-dementia-what-clinical-trials-are-revealing)
- New research reveals high rates of malnutrition in people living with dementia in long-term care (https://medicalxpress.com/news/2023-06-reveals-high-malnutrition-people-dementia.html)
- Explore Strategies for Supporting Dementia Patients Who Refuse Food
- Supporting someone with dementia to eat and drink (https://alzheimers.org.uk/get-support/living-with-dementia/improving-eating-experience-dementia)
- Dementia And Eating Issues: How To Help Your Loved One Eat More - NCCDP (https://nccdp.org/dementia-and-eating-issues-how-to-help-your-loved-one-eat-more)
- Nutrition and Dementia: How Caregivers Can Improve Mealtime (https://aarp.org/caregiving/medical/dementia-nutrition-loss-of-appetite)
- Helping caregivers help people with dementia eat at home (https://sciencedaily.com/releases/2024/02/240215113556.htm)
- Tips for Caregivers: Helping People With Alzheimer’s Disease Eat Well (https://nia.nih.gov/health/alzheimers-caregiving/tips-caregivers-helping-people-alzheimers-disease-eat-well)

