
For families in our service areas
For families in our service areas, this guide explains alzheimer's care and how non-medical in-home caregiving can support care planning in East Idaho, Treasure Valley & Magic Valley, Northern Wasatch, North Central West Virginia, and Northeast Ohio.
What You Need to Know About When Alzheimer
Appetite loss in Alzheimer's patients presents a significant challenge for caregivers. This issue intertwines cognitive, emotional, and physical factors, which can severely impact nutritional health. Understanding the reasons behind this decline is crucial, as it paves the way for effective strategies that can enhance the eating experience and improve overall well-being.
However, caregivers often grapple with the delicate balance of encouraging nourishment while addressing the unique needs of those living with Alzheimer's. This complexity not only affects the patients but also places a considerable burden on caregivers, who must navigate these challenges daily.
To tackle this issue, caregivers can implement several practical solutions:
- Creating a structured meal environment can help reduce distractions and promote focus during mealtime.
- Offering smaller, more frequent meals may encourage better intake without overwhelming the patient.
- Engaging patients in meal preparation can also foster a sense of involvement and enjoyment, making the eating experience more appealing.
By understanding the intricacies of appetite loss and employing these strategies, caregivers can significantly enhance the nutritional health and overall quality of life for those they care for.
Understand the Reasons Behind Appetite Loss in Alzheimer's Patients
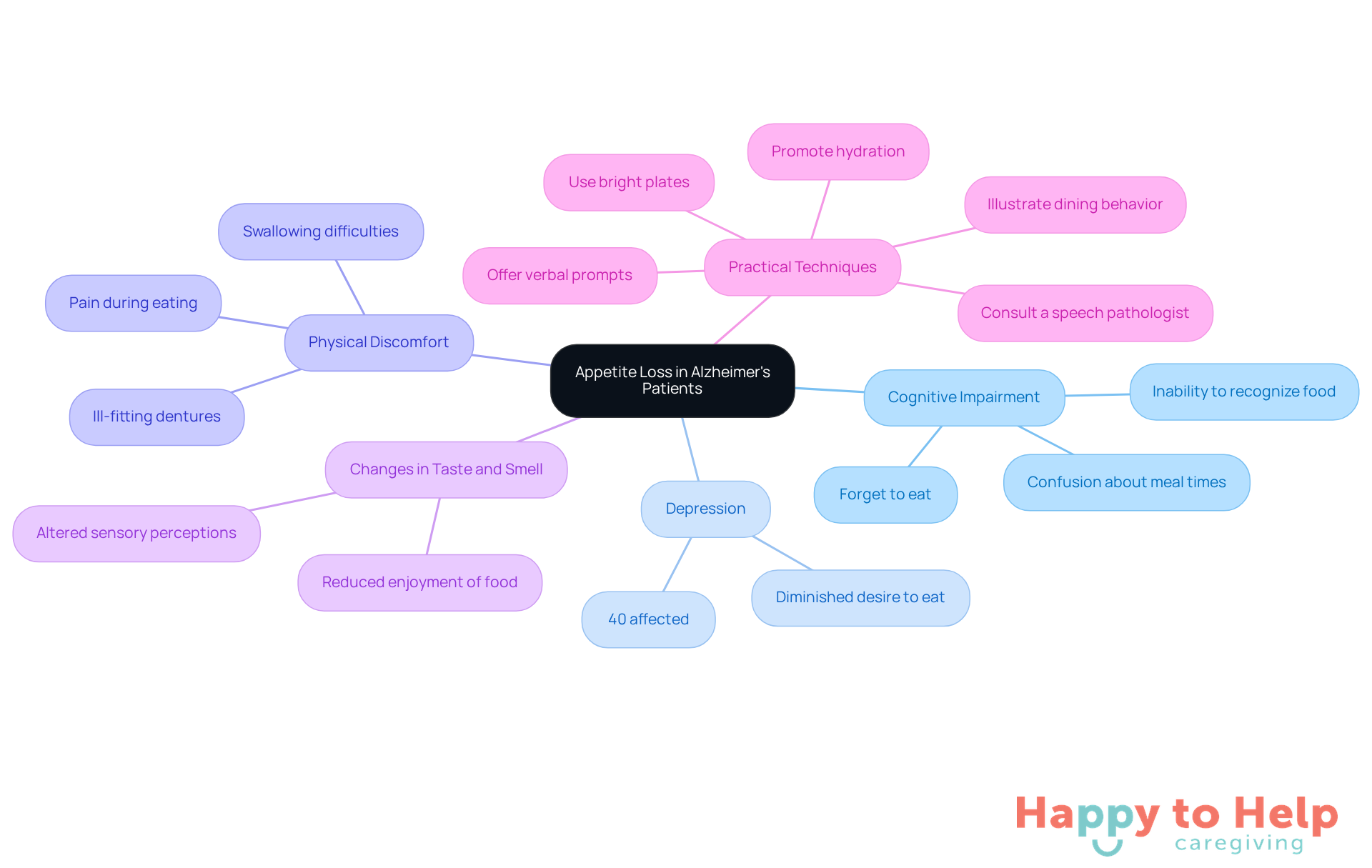
Appetite loss in Alzheimer's patients presents a significant challenge for caregivers, stemming from several interconnected factors:
-
Cognitive Impairment: Many patients may forget to eat or struggle to recognize food. This confusion can be compounded by uncertainty about meal times or the inability to recall whether they have already eaten, leading to missed meals.
-
Depression: Depression affects up to 40% of individuals with Alzheimer's, significantly diminishing their desire to eat. Caregivers must recognize and address signs of depression to support their loved ones effectively.
-
Physical Discomfort: Issues like ill-fitting dentures, swallowing difficulties, or other health-related problems can make eating painful or uncomfortable. Caregivers should monitor these conditions to ensure a more pleasant dining experience.
-
Changes in Taste and Smell: Alzheimer's can alter sensory perceptions, reducing the enjoyment of food. As taste and smell diminish, caregivers should modify food choices to include more appealing alternatives, potentially enhancing the dining experience.
Moreover, it's crucial to note that 54% of early-stage Alzheimer's individuals are at risk of malnutrition, especially when Alzheimer's patients stop eating, which highlights the severity of appetite loss in this population.
To combat these challenges, caregivers can implement practical techniques:
- Use simple, bright plates to boost food intake by 25%.
- Offer verbal prompts during meals, such as 'Pick up your spoon.'
- Illustrate dining behavior to support clients.
- Consult a speech pathologist for dietary modifications if swallowing issues arise.
- Promote hydration throughout the day and remain vigilant for signs of dehydration.
By acknowledging these factors and employing these strategies, caregivers can create customized approaches to encourage food consumption, ultimately supporting the nutritional well-being of their loved ones.
Implement Strategies to Encourage Eating
Significant challenges for caregivers can arise when Alzheimer's patients stop eating due to eating difficulties. These individuals often struggle with appetite and nutrition, which can lead to further health complications. Understanding how to encourage eating is crucial for promoting better nutrition and overall well-being, particularly when Alzheimer's patients stop eating.
To tackle this issue, caregivers can implement several effective strategies:
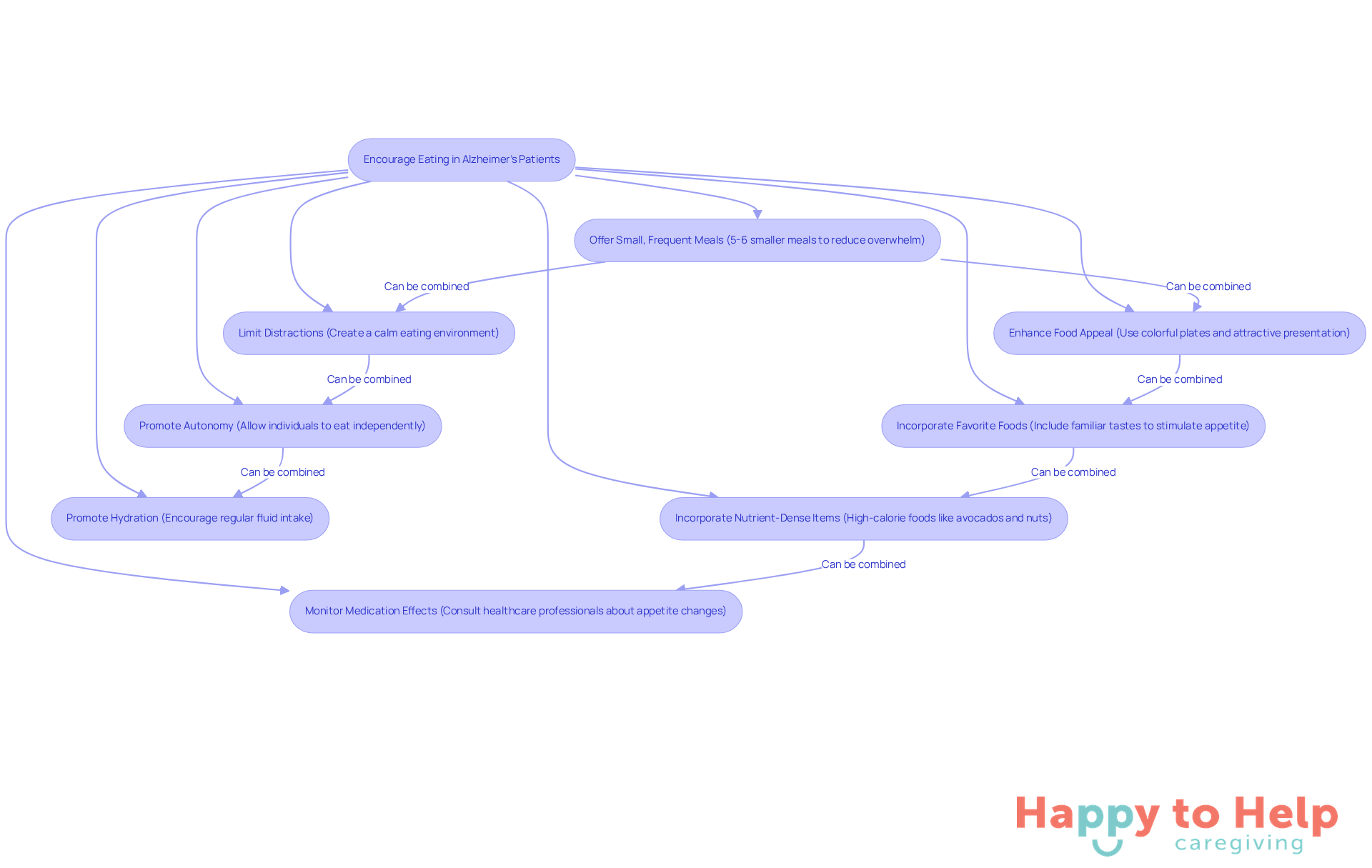
- Offer Small, Frequent Meals: Instead of three large meals, provide five to six smaller meals throughout the day. This approach can make eating less overwhelming and more manageable for individuals with dementia. Remember, it can take an hour or more for a person with dementia to complete a dining experience, so patience is essential.
- Enhance Food Appeal: Use colorful plates and present food attractively. Research indicates that visually appealing dishes can stimulate appetite, so trying out various textures and flavors is crucial to discover what the patient prefers.
- Limit Distractions: Create a calm eating environment by minimizing noise and visual distractions. Turning off the TV and keeping the table setting simple can help individuals focus on their meals.
- Incorporate Favorite Foods: Including foods that the individual has enjoyed in the past can stimulate appetite. Familiar tastes often evoke positive memories and encourage eating.
- Promote Autonomy: Allow individuals to eat on their own when feasible. This can enhance their sense of control and willingness to eat, making mealtimes more enjoyable.
- Incorporate Nutrient-Dense Items: Concentrate on items that are high in calories and nutrients, such as avocados, nuts, and smoothies. This ensures that patients obtain sufficient nutrition even if their overall consumption is lower.
- Promote Hydration: Encourage fluid intake throughout the day by offering small cups of water or other liquids regularly. Staying hydrated is crucial for preventing dehydration, which is a common challenge for individuals with dementia.
- Monitor Medication Effects: Be aware that changes to medication or dosage can significantly affect a person's appetite. Consulting with healthcare professionals about any concerns can help manage these issues.
- Utilize Visual Aids: Consider using visual aids to help bridge communication gaps, as individuals with dementia may struggle to express hunger or food preferences. This can make mealtimes more manageable and enjoyable.
By implementing these strategies, caregivers can significantly improve the eating experience for individuals with Alzheimer's, particularly when Alzheimer's patients stop eating, promoting better nutrition and overall well-being.
Create a Supportive Mealtime Environment
Creating a supportive mealtime environment for individuals with Alzheimer's can be challenging. Caregivers often face difficulties in ensuring that meals are not only nutritious but also enjoyable and stress-free. This is crucial, as mealtime can significantly impact both physical health and emotional well-being.
To address these challenges, here are some actionable solutions:
-
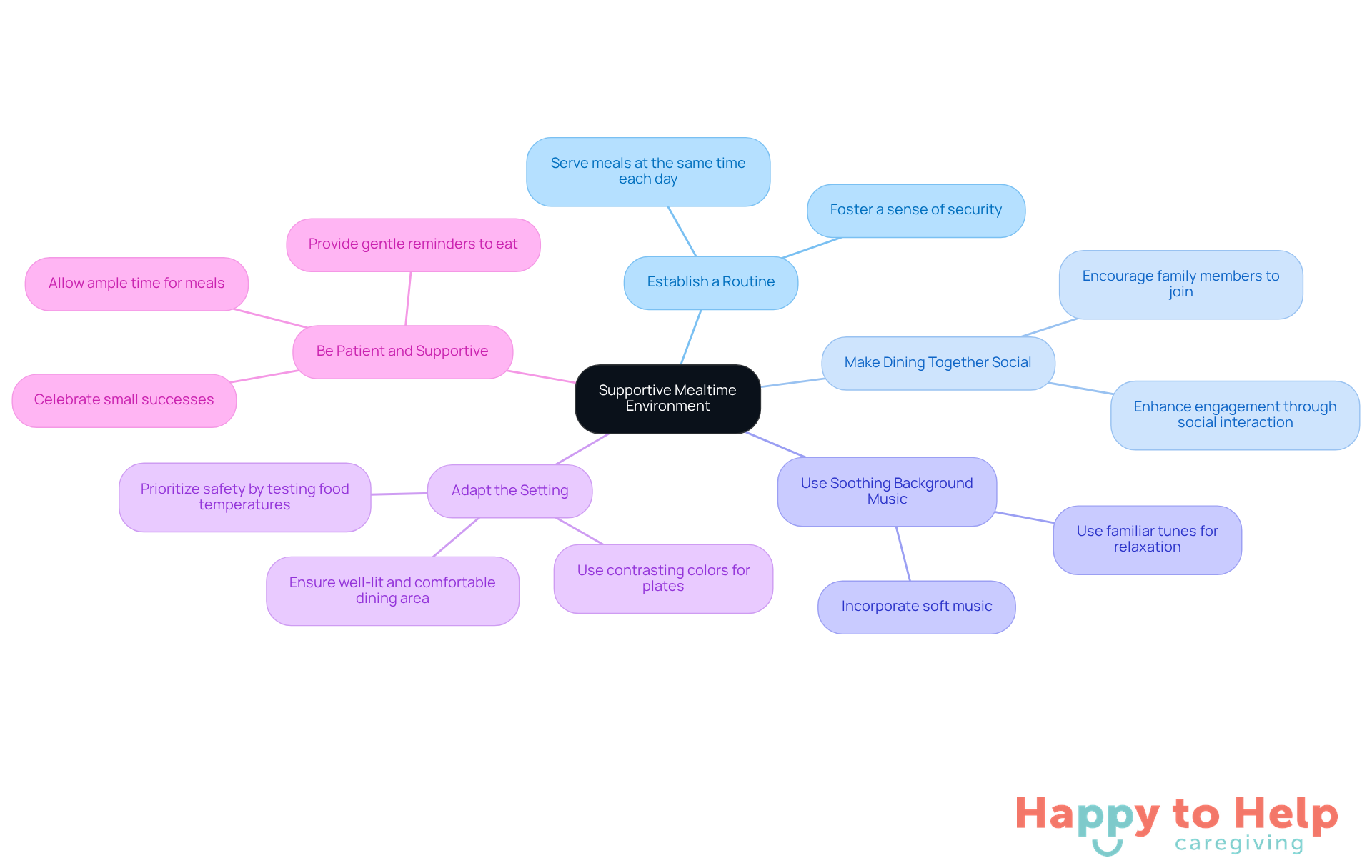
Establish a Routine: Consistency is key. Aim to serve food at the same time each day to foster a sense of security. As noted by The Bristal, maintaining consistent dining times supports physical health and emotional well-being through social connections during shared meals.
-
Make Dining Together Social: Encourage family members to join at the table. Social interaction enhances the dining experience and promotes engagement, positively influencing eating habits. The Alzheimer's Association highlights that social mealtimes can encourage individuals to eat more.
-
Use Soothing Background Music: Incorporating soft music can create a calming atmosphere, helping individuals relax and enjoy their meals. Familiar tunes can be particularly effective as part of a gentle routine.
-
Adapt the Setting: Ensure the dining area is well-lit and comfortable. Using contrasting colors for plates and table settings can help individuals differentiate meals from the background, making mealtime less overwhelming. Caregivers should also prioritize safety by testing food temperatures and monitoring for choking risks.
-
Be Patient and Supportive: Allow ample time for meals and provide gentle reminders to eat. Celebrating small successes can boost confidence and encourage further eating, reinforcing positive mealtime experiences.
Recognize When to Seek Professional Assistance
Caregivers often encounter significant challenges when it comes to ensuring proper nutrition for their patients. Here are some critical issues to watch for:
-
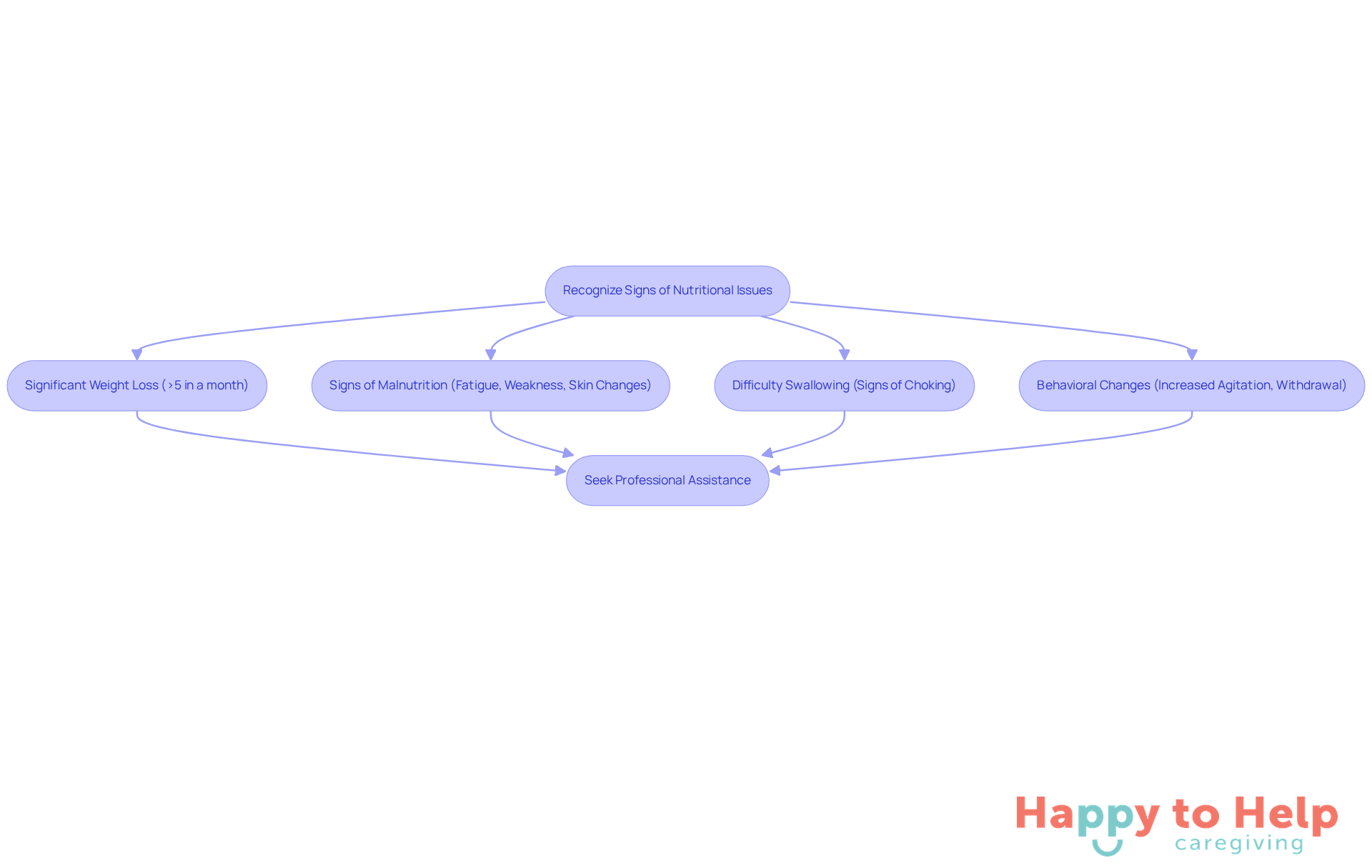
Significant Weight Loss: If a patient loses more than 5% of their body weight in a month, this could signal a serious health concern that warrants immediate medical evaluation.
When Alzheimer's patients stop eating consistently for several days, it’s crucial to consult a healthcare provider to address potential underlying issues. -
Signs of Malnutrition: Symptoms like fatigue, weakness, or changes in skin condition may indicate nutritional deficiencies. Recognizing these signs early can lead to timely intervention.
-
Difficulty Swallowing: If a patient shows signs of choking or struggles to swallow, seeking immediate medical advice is essential to prevent complications.
-
Behavioral Changes: Sudden shifts in behavior, such as increased agitation or withdrawal during mealtimes, may require professional assessment when Alzheimer's patients stop eating to uncover and address underlying problems.
By being vigilant about these signs, caregivers can take proactive steps to ensure their patients receive the necessary support and care.
Making the Right Choice
Addressing appetite loss in Alzheimer's patients presents a significant challenge for caregivers, impacting their nutritional health and overall well-being. This issue arises from various underlying factors, including cognitive impairment, depression, physical discomfort, and sensory changes. Understanding these reasons is crucial for caregivers to develop effective strategies that encourage eating and ensure patients receive necessary nourishment.
To combat appetite loss effectively, caregivers can implement several practical solutions:
- Create a supportive mealtime environment that fosters comfort and reduces distractions.
- Offer smaller, more frequent meals to make eating less overwhelming.
- Enhance food appeal by presenting meals attractively and incorporating favorite foods.
- Promote hydration to ensure patients remain well-hydrated, which is essential for overall health.
Additionally, caregivers should be vigilant about signs of malnutrition and know when to seek professional help. Recognizing these signs early can prevent further health complications and ensure timely intervention.
Ultimately, caregivers play a vital role in fostering a positive eating experience for those affected by Alzheimer's. By implementing these strategies and remaining attentive to their loved ones' needs, caregivers can significantly improve nutritional intake and enhance the quality of life for Alzheimer's patients. Recognizing the importance of mealtime and taking proactive steps can lead to better health outcomes and a more enjoyable dining experience, reinforcing the significance of compassionate care in this challenging journey.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5MjI2NTBmNGUzNmZmNzE5NDQ4Mjc3MSIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What are the main reasons for appetite loss in Alzheimer's patients?
Appetite loss in Alzheimer's patients can be attributed to cognitive impairment, depression, physical discomfort, and changes in taste and smell.
How does cognitive impairment affect eating in Alzheimer's patients?
Cognitive impairment may lead patients to forget to eat, struggle to recognize food, or be uncertain about meal times, resulting in missed meals.
What role does depression play in appetite loss for individuals with Alzheimer's?
Depression affects up to 40% of individuals with Alzheimer's, significantly reducing their desire to eat, which caregivers need to address to support their loved ones.
What physical issues might contribute to appetite loss in Alzheimer's patients?
Physical discomfort from problems like ill-fitting dentures, swallowing difficulties, or other health-related issues can make eating painful or uncomfortable.
How do changes in taste and smell impact food consumption in Alzheimer's patients?
Alzheimer's can alter sensory perceptions, diminishing the enjoyment of food, which may lead caregivers to modify food choices to include more appealing alternatives.
What is the risk of malnutrition in early-stage Alzheimer's patients?
Approximately 54% of early-stage Alzheimer's individuals are at risk of malnutrition, particularly when they stop eating.
What strategies can caregivers use to encourage eating in Alzheimer's patients?
Caregivers can use simple, bright plates to boost food intake, offer verbal prompts during meals, illustrate dining behavior, consult a speech pathologist for dietary modifications, and promote hydration throughout the day.
List of Sources
- Understand the Reasons Behind Appetite Loss in Alzheimer's Patients
- Food & Eating | Alzheimer's Association (https://alz.org/help-support/caregiving/daily-care/food-eating)
- Alzheimer’s Patient Won’t Eat: Why It Happens and What to Do (https://healthline.com/health/alzheimers/alzheimers-patient-not-eating)
- Dementia and appetite loss: Causes and management (https://medicalnewstoday.com/articles/dementia-patient-not-eating)
- Appetite and dementia (https://alzheimers.org.uk/get-support/living-with-dementia/poor-appetite-dementia)
- Poor Appetite in Your Alzheimer’s Patients? (https://guidestareldercare.com/blog/poor-appetite-in-your-alzheimers-patients)
- Implement Strategies to Encourage Eating
- Food & Eating | Alzheimer's Association (https://alz.org/help-support/caregiving/daily-care/food-eating)
- Meal time (https://alzheimer.ca/en/help-information/im-caring-person-living-dementia/providing-day-day-care/meal-time)
- Appetite and dementia (https://alzheimers.org.uk/get-support/living-with-dementia/poor-appetite-dementia)
- Changes in eating habits and food preference (https://alzheimers.org.uk/get-support/living-with-dementia/changes-eating-habits-food-preference)
- Create a Supportive Mealtime Environment
- Food & Eating | Alzheimer's Association (https://alz.org/help-support/caregiving/daily-care/food-eating)
- Supporting someone with dementia to eat and drink (https://alzheimers.org.uk/get-support/living-with-dementia/improving-eating-experience-dementia)
- (https://belleviecare.co.uk/support-advice/dementia-quotes-to-lift-your-spirits)
- The Importance of Routine for Seniors with Alzheimer’s and Dementia (https://blog.thebristal.com/importance-routine-seniors-alzheimers-dementia)
- Optimizing mealtime care and outcomes for people with dementia and their caregivers: A systematic review and meta‐analysis of intervention studies - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC11922811)
- Recognize When to Seek Professional Assistance
- ADI - Nutrition and dementia (https://alzint.org/resource/nutrition-and-dementia)
- Weight Loss in Patients with Dementia: Considering the Potential Impact of Pharmacotherapy - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC6779159)
- Meta-analysis and moderator analysis of the prevalence of malnutrition and malnutrition risk among older adults with dementia (https://sciencedirect.com/science/article/abs/pii/S0020748923002134)
- When Is It Time To Hire Dementia Care Help? (https://ilcorp.org/time-hire-dementia-care-help)
- Prevalence of Malnutrition in People with Dementia in Long-Term Care: A Systematic Review and Meta-Analysis - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10343750)