
For families in our service areas
For families in our service areas, this guide explains dementia care and how non-medical in-home caregiving can support care planning in East Idaho, Treasure Valley & Magic Valley, Northern Wasatch, North Central West Virginia, and Northeast Ohio.
Understanding When Should a Dementia Patient Go into
Deciding when a dementia patient should move into a care home is a significant challenge that many families encounter as cognitive decline progresses. This transition can be fraught with emotional turmoil and practical concerns, making it essential for caregivers to recognize the signs that indicate a need for more structured support.
The implications of delaying this decision can be profound, affecting not only the patient’s quality of life but also the well-being of their families. Caregivers often grapple with feelings of guilt and uncertainty, questioning whether they are making the right choice for their loved ones. This emotional burden can complicate an already difficult situation.
To navigate this complex landscape, caregivers need clear, actionable solutions. Recognizing specific signs - such as increased confusion, difficulty with daily activities, or safety concerns - can help determine when it’s time to seek additional support. Engaging with healthcare professionals and exploring care options early can also ease the transition, ensuring that loved ones receive the best possible care.
Understand Dementia Progression and Stages
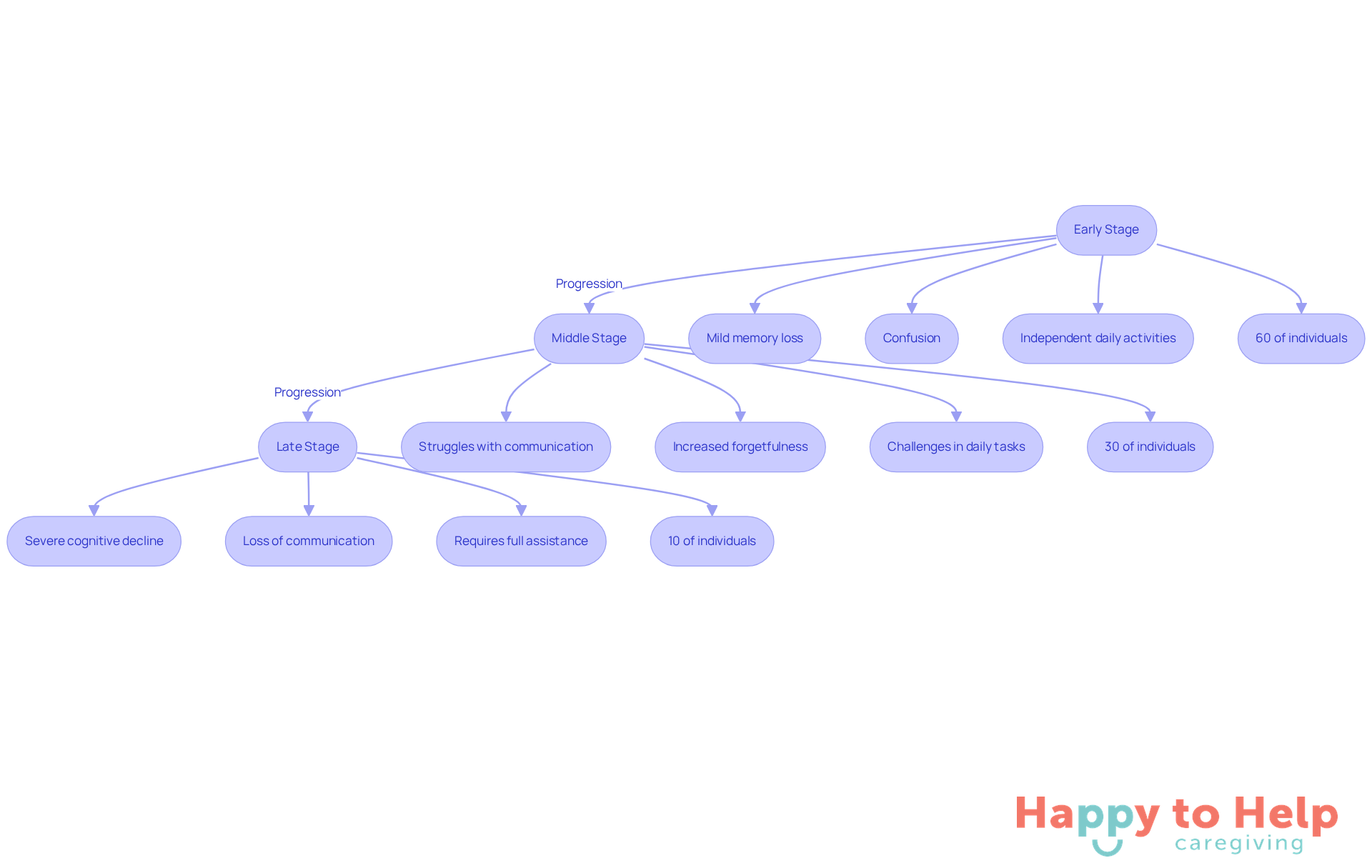
Dementia progresses through distinct stages: early, middle, and late, each marked by specific cognitive and functional changes.
Problem: In the early stage, individuals may experience mild memory loss, confusion, and occasional disorientation. They can often manage daily activities independently, but approximately 60% of individuals with cognitive decline are in this stage. This highlights the need for early intervention and support to enhance quality of life.
Agitate: As cognitive decline advances to the middle stage, symptoms become more pronounced. Patients may struggle with communication, exhibit increased forgetfulness, and face challenges in performing daily tasks. This phase represents about 30% of memory loss instances, emphasizing the necessity for caregivers to provide more organized assistance and oversight.
Solution: In the late stage, individuals experience severe cognitive decline, losing the ability to communicate effectively and requiring assistance with all aspects of daily living. This phase accounts for approximately 10% of dementia patients, necessitating thorough support strategies to ensure safety and comfort.
Understanding these phases is essential for caregivers. It helps evaluate when should a dementia patient go into a care home, indicating when a family member may need more organized support. Geriatric specialists stress the importance of identifying these changes early to enable prompt interventions and improve overall health outcomes. By grasping the progression of cognitive decline, caregivers can manage the intricacies of support more effectively and make informed decisions about their loved ones' needs.
Identify Key Signs for Transitioning to a Care Home
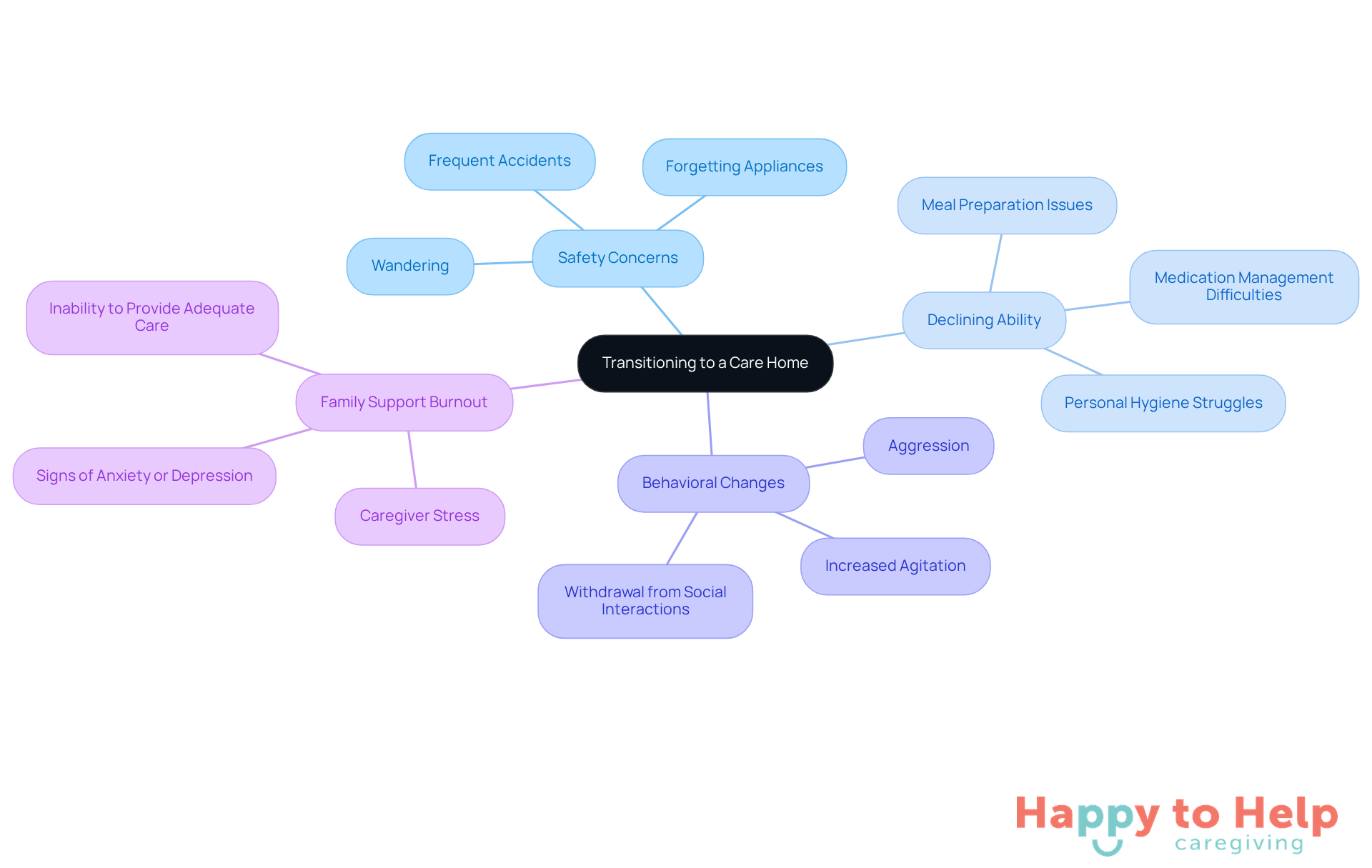
Several key signs may indicate that a dementia patient should transition to a care home:
Problem: Increased Safety Concerns
Wandering behavior, forgetting to turn off appliances, or frequent accidents can signal that the individual is no longer safe at home. Caregivers often express concerns about the risks associated with these behaviors, emphasizing the need for a secure environment.
Agitate: Declining Ability to Perform Daily Activities
Struggles with personal hygiene, meal preparation, and medication management are significant indicators that more structured care is necessary. As dementia progresses, the ability to manage these tasks diminishes, leading to potential health risks.
Agitate: Behavioral Changes
Increased agitation, aggression, or withdrawal from social interactions may suggest that the individual is having difficulty coping at home. These changes can create a challenging environment for both the patient and the health provider, often leading to heightened stress levels.
Agitate: Family Support Burnout
Relatives who provide care often encounter significant stress, with studies showing that 60% report signs of anxiety or depression. If those providing support feel incapable of delivering the essential standard of assistance, it may raise the question of when should a dementia patient go into a care home. Real-world examples highlight how caregiver burnout can lead to neglect of both the caregiver's and the patient's well-being.
Solution: Action Steps
- Monitor daily activities and behaviors closely.
- Keep a journal of any concerning incidents to discuss with healthcare professionals.
Engage Family and Professionals in the Decision-Making Process
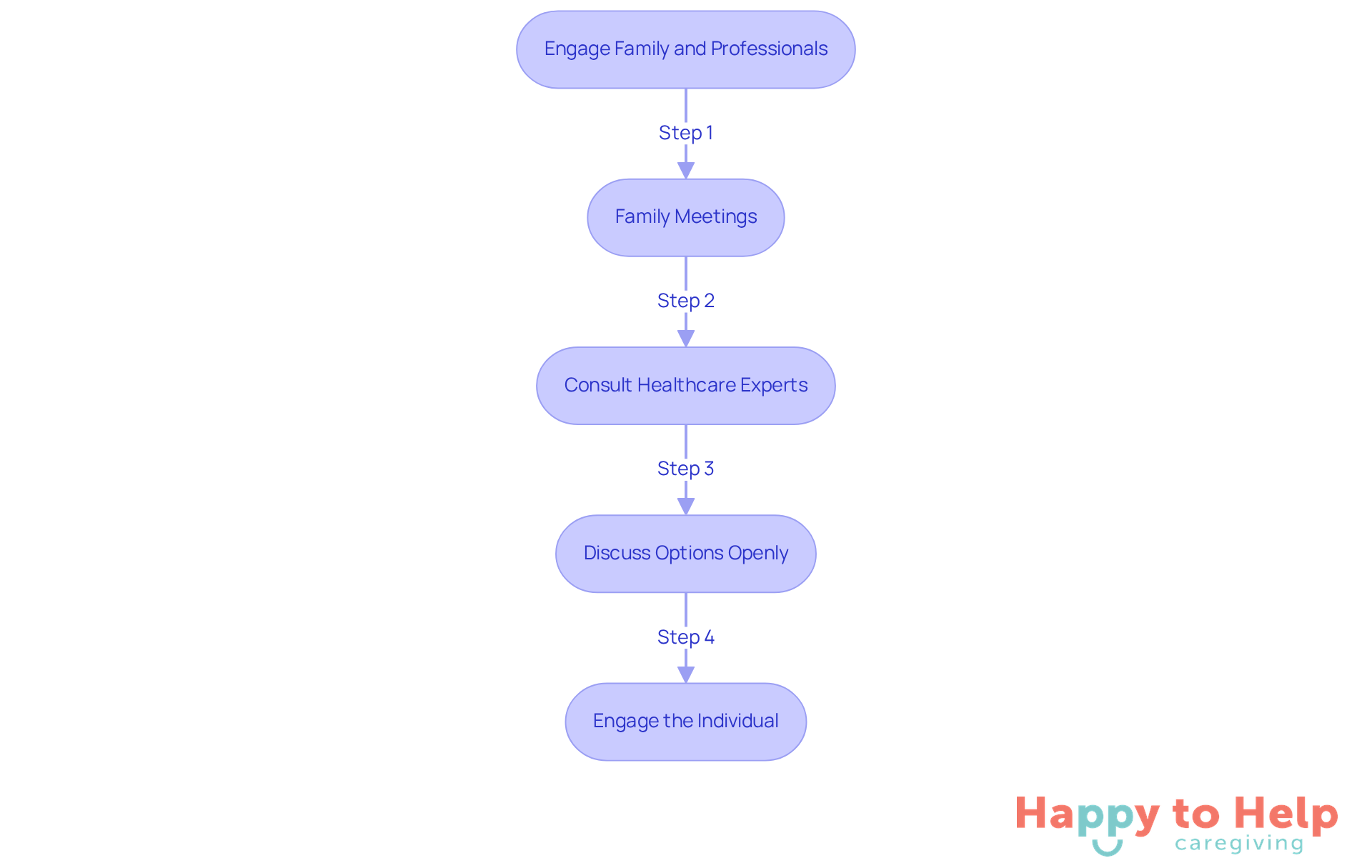
Transitioning to a residential facility can be a daunting process for families, particularly when they are faced with the question of when should a dementia patient go into a care home. Involving family members and experts in decision-making is crucial to ensure a smooth transition. Here are key steps to facilitate this engagement:
-
Family Meetings: Regular gatherings with family members are essential to discuss the loved one's support needs and any changes in behavior or health. Research indicates that these meetings significantly improve coordination of assistance and emotional support for caregivers. With approximately 7.2 million people in the U.S. experiencing Alzheimer's and other forms of cognitive decline, these discussions are vital for effective support planning.
-
Consult Healthcare Experts: Engaging with physicians, social workers, or geriatric support managers can provide valuable insights and recommendations tailored to the individual's health status. Many caregivers feel unprepared to navigate the complexities of cognitive impairment support. As Laura Gitlin, Dean of the College of Nursing and Health Professions at Drexel University, states, "We need a much more comprehensive approach that recognizes the prolonged, degenerative nature of this illness and the fact that dementia is a family affair."
-
Discuss options openly by encouraging conversations about when should a dementia patient go into a care home, considering the potential benefits and drawbacks of moving to a residential facility. Addressing family members' concerns can alleviate anxiety and foster a collaborative planning approach. Notably, 48% of recipients live in their own homes, making this transition a significant consideration for families.
-
Engage the Individual: Whenever possible, involve the person with cognitive impairment in discussions about their support preferences. Honoring their autonomy not only respects their wishes but can also enhance their dignity during this challenging transition.
Tips for Effective Communication:
- Use clear and compassionate language to convey information.
- Be patient and allow time for questions and concerns to be voiced, ensuring that all family members feel heard and valued.
Select the Right Care Home for Your Loved One
Choosing the right residence for support can be a daunting task for caregivers. The challenge lies in ensuring that the selected facility meets the unique needs of your loved one, particularly when it comes to memory loss support. This decision can significantly impact their well-being and quality of life.
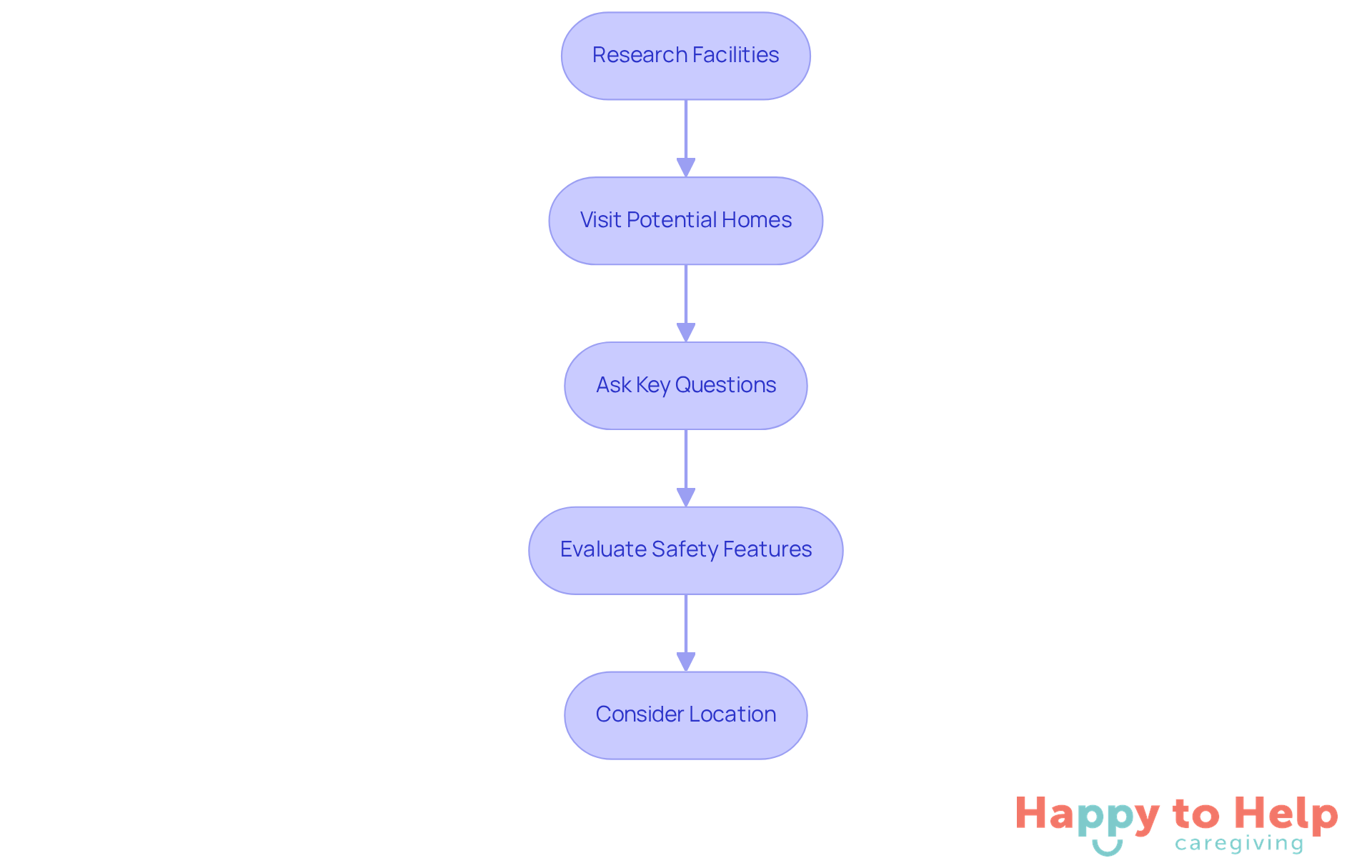
To navigate this process effectively, consider the following steps:
- Research Facilities: Start by investigating nearby residential homes that specialize in memory loss support. Look for reviews and ratings from other families to gauge their experiences.
- Visit Potential Homes: Schedule tours of the facilities to assess the environment, cleanliness, and overall atmosphere. Observe how staff interact with residents, as this can provide insight into the quality of care.
- Ask Key Questions: Inquire about staff qualifications, resident-to-staff ratios, and the types of activities offered. It's crucial to ensure that the facility has a structured program designed for individuals with cognitive impairments.
- Evaluate Safety Features: Check for safety measures such as secure entrances, non-slip flooring, and emergency response systems to protect your loved one.
- Consider Location: Choose a facility that is conveniently located for family visits. Regular visits can help ease the transition for your loved one, making them feel more at home.
Checklist for Evaluating Care Homes:
- Cleanliness and safety of the environment.
- Staff qualifications and training in dementia support.
- Availability of personalized care plans and activities.
Key Takeaways for Caregivers
Understanding when a dementia patient should transition to a care home presents a significant challenge for caregivers. This decision is not just about logistics; it involves the safety and well-being of loved ones. The complexity of dementia, with its progressive stages and varying symptoms, underscores the need for a proactive approach. Recognizing the signs that indicate a need for more structured care is essential for ensuring a smooth transition.
Caregivers face several critical issues, including safety concerns, the ability to perform daily tasks, and the emotional toll on both the patient and themselves. Engaging family members and professionals in the decision-making process is vital. This collaboration fosters respect for the individual’s preferences and enhances the overall care experience. Additionally, selecting the right care home requires thorough research, facility visits, and careful consideration of safety features.
To navigate this transition effectively, caregivers can take several actionable steps:
- Recognize the signs: Be vigilant about changes in behavior or ability that may indicate a need for more support.
- Involve others: Engage family members and professionals to ensure a well-rounded decision-making process.
- Research options: Visit potential care homes and assess their safety features and services.
Ultimately, transitioning a dementia patient to a care home can enhance the quality of life for both the patient and the caregiver. By staying informed and proactive, caregivers can approach this difficult process with compassion and confidence. Prioritizing the well-being of loved ones and seeking support will lead to more positive outcomes during this challenging time.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5MjY0Mzg5ZDdhYTIxYWI5OTE3NmUxOSIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What are the stages of dementia progression?
Dementia progresses through three distinct stages: early, middle, and late, each characterized by specific cognitive and functional changes.
What symptoms are associated with the early stage of dementia?
In the early stage, individuals may experience mild memory loss, confusion, and occasional disorientation. They can often manage daily activities independently.
What percentage of individuals with cognitive decline are in the early stage of dementia?
Approximately 60% of individuals with cognitive decline are in the early stage.
What challenges do individuals face during the middle stage of dementia?
In the middle stage, symptoms become more pronounced, including struggles with communication, increased forgetfulness, and difficulties in performing daily tasks.
What percentage of memory loss instances does the middle stage of dementia represent?
The middle stage accounts for about 30% of memory loss instances.
What happens in the late stage of dementia?
In the late stage, individuals experience severe cognitive decline, losing the ability to communicate effectively and requiring assistance with all aspects of daily living.
What percentage of dementia patients are in the late stage?
This phase accounts for approximately 10% of dementia patients.
Why is understanding the stages of dementia important for caregivers?
Understanding these phases helps caregivers evaluate when a dementia patient may need to go into a care home and indicates when more organized support is necessary.
What do geriatric specialists emphasize regarding dementia progression?
Geriatric specialists stress the importance of identifying changes early to enable prompt interventions and improve overall health outcomes for dementia patients.
How can caregivers benefit from understanding dementia progression?
By grasping the progression of cognitive decline, caregivers can manage support intricacies more effectively and make informed decisions about their loved ones' needs.
List of Sources
- Understand Dementia Progression and Stages
- ADI - Dementia statistics (https://alzint.org/about/dementia-facts-figures/dementia-statistics)
- Alzheimer's Disease Facts and Figures (https://alz.org/alzheimers-dementia/facts-figures)
- Fact Sheet: U.S. Dementia Trends (https://prb.org/resources/fact-sheet-u-s-dementia-trends)
- Risk and future burden of dementia in the United States (https://nih.gov/news-events/nih-research-matters/risk-future-burden-dementia-united-states)
- United States Dementia Cases Estimated to Double by 2060 (https://nyulangone.org/news/united-states-dementia-cases-estimated-double-2060)
- Identify Key Signs for Transitioning to a Care Home
- New Alzheimer’s Association Report Reveals Top Stressors for Caregivers and Lack of Care Navigation Support and Resources (https://alz.org/news/2024/new-alzheimers-association-report-reveals-top-stressors-caregivers)
- 11 Signs It's Time for Memory Care | Home of the Good Shepherd (https://homeofthegoodshepherd.com/news/when-is-it-time-for-memory-care)
- Caregiver Stress in Dementia (https://braincheck.com/articles/caregiver-stress-dementia)
- When should someone with dementia go into a care home? (https://medicalnewstoday.com/articles/when-should-someone-with-dementia-go-into-a-care-home)
- Alzheimer's Disease Facts and Figures (https://alz.org/alzheimers-dementia/facts-figures)
- Engage Family and Professionals in the Decision-Making Process
- Dementia care programs help, if caregivers can find them (https://cbsnews.com/news/alzheimers-dementia-care-programs-help-if-caregivers-can-find-them)
- Alzheimer's Disease Facts and Figures (https://alz.org/alzheimers-dementia/facts-figures)
- Caregiver Statistics: Demographics (https://caregiver.org/resource/caregiver-statistics-demographics)
- The Importance of Family Involvement in Long Term Care - (https://shakerplace.org/news/the-importance-of-family-involvement-in-long-term-care)
- Select the Right Care Home for Your Loved One
- 65 Inspirational Quotes About Caring For Elderly Parents - Home Care Agency | Global One Home Care Boston (https://globalonehomecare.com/65-inspirational-quotes-about-caring-for-elderly-parents)
- Taking Care of Elderly Parents Quotes - Freedom Care (https://freedomcare.com/taking-care-of-elderly-parents-quotes)
- 40 Inspirational Quotes for Caregivers - Care Options for Kids (https://careoptionsforkids.com/blog/inspirational-quotes-for-caregivers)
- CaringBridge (https://caringbridge.org/resources/inspirational-quotes-on-caregiving)
- Taking Care of Elderly Parents Quotes (https://ultimatecareny.com/resources/taking-care-of-elderly-parents-quotes)