
What You Need to Know About When Should Dementia Patients Go Into
Deciding when to transition a loved one with dementia into care can be an incredibly emotional journey for families. With over 6 million Americans facing cognitive impairment, the need to evaluate care requirements and living situations has never felt more pressing.
This article serves as a heartfelt guide for caregivers, delving into the essential factors to consider, the emotional weight of caregiving, and the various support options available. As families navigate this challenging terrain, they often wonder: how can they find the right moment to seek professional care while ensuring the well-being of both their loved one and themselves?
It's important to recognize the stress and burnout that can accompany this decision. Many caregivers experience feelings of guilt and uncertainty, making it vital to explore the emotional and practical support that exists. Remember, you are not alone in this journey.
As we explore the options available, let’s take a moment to reflect on the compassionate care that can make a difference. Stories from caregivers who have walked this path can offer insight and comfort, reminding us that seeking help is a sign of strength, not weakness.
Ultimately, the goal is to foster a nurturing environment for both the individual and their family. Together, we can navigate this complex landscape with empathy and understanding.
Assess Care Needs and Living Conditions
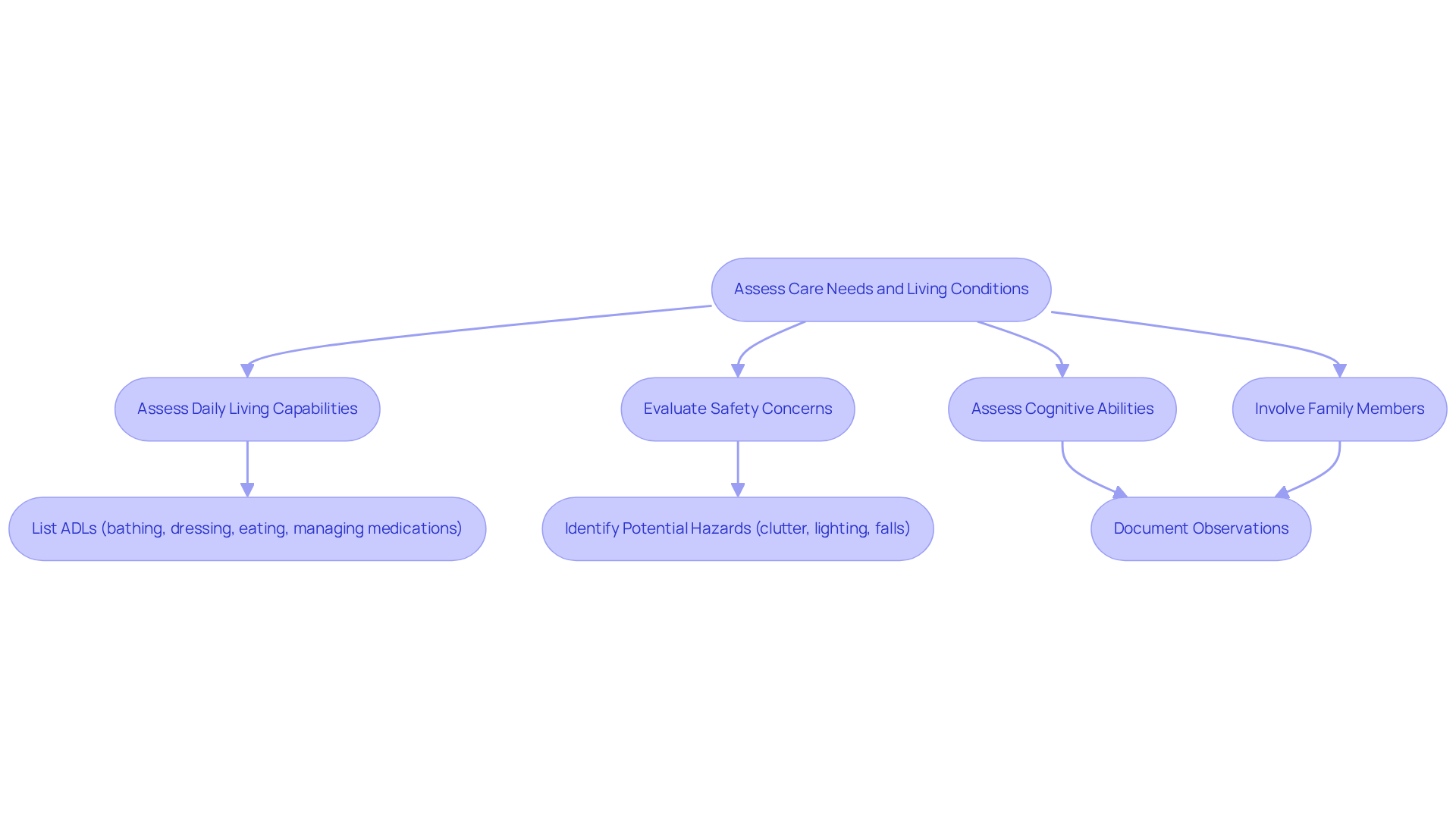
Start by gently assessing the individual's daily living capabilities, focusing on their ability to perform activities of daily living (ADLs) like bathing, dressing, eating, and managing medications. It's crucial to pay close attention to safety concerns in their living environment - think clutter, inadequate lighting, and potential hazards that could lead to falls. With over 6 million Americans currently living with cognitive impairment and projections of 14 million cases by 2060, addressing these safety concerns in their homes becomes even more urgent. Also, take a moment to assess their cognitive abilities: Can they remember important information, follow conversations, or recognize familiar faces? Documenting these observations helps create a clearer picture of their current situation.
Involving family members or support persons in this evaluation is essential, as their insights into the individual's behavior and needs are invaluable. Using specific checklists or assessment tools, like the Brain Health Toolkit available in both English and Spanish, can ensure a thorough evaluation. This step is vital; it will guide the following decisions regarding support options and resources, ultimately enhancing the quality of life for those affected by dementia, including when should dementia patients go into care. Remember, you’re not alone in this journey - there are compassionate resources available to help you every step of the way.
Evaluate Caregiver Capacity and Emotional Readiness
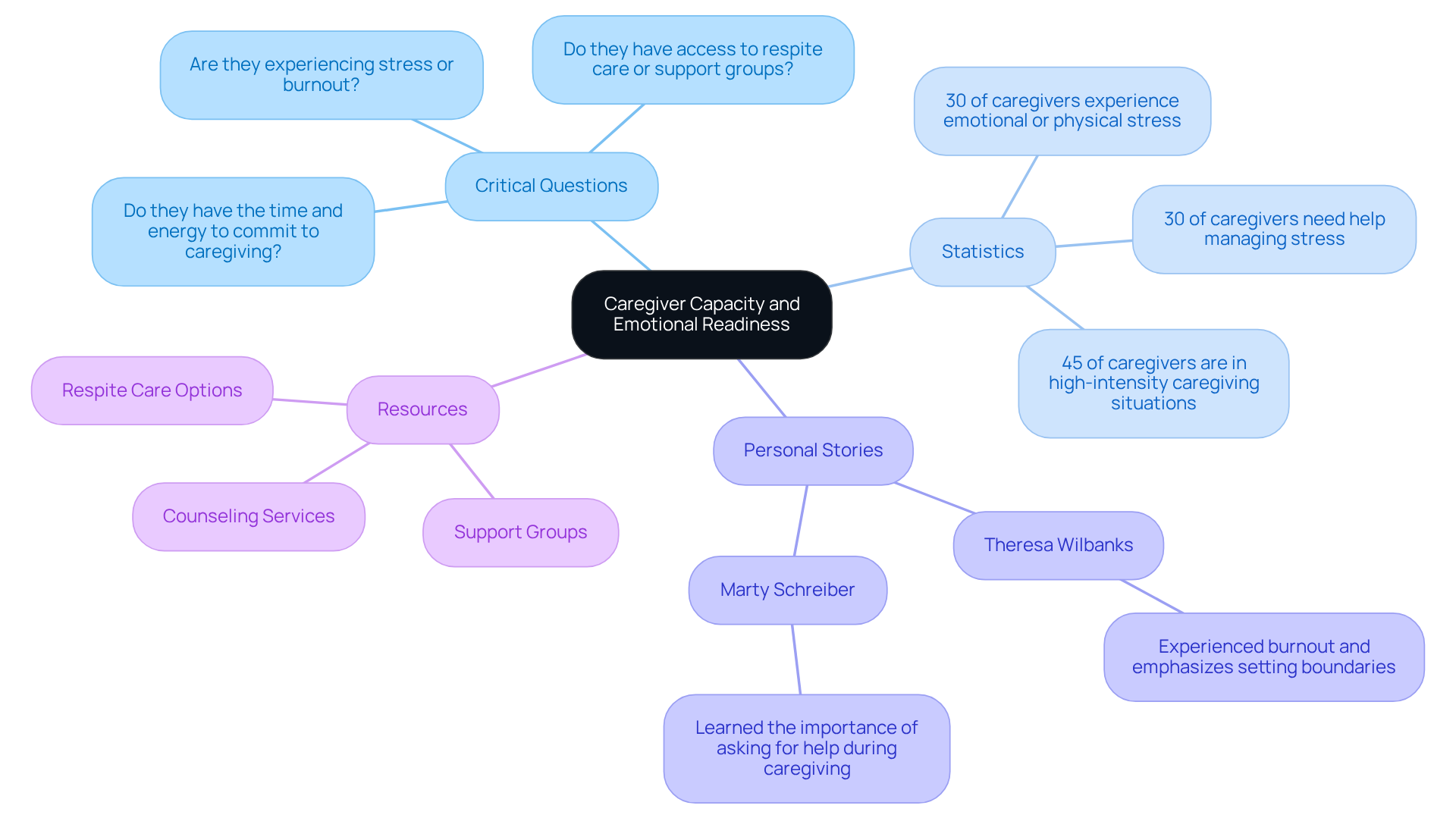
Evaluating a provider's physical and emotional capabilities is essential for understanding their ability to deliver effective support. It's important to consider their overall health, availability, and existing support systems. Caregivers should reflect on some critical questions:
- Do they have the time and energy to commit to caregiving?
- Are they experiencing stress or burnout?
- Do they have access to respite care or support groups?
Recognizing emotions like stress, frustration, or fear is crucial for those providing care. These feelings are completely normal and signal the need for self-care and support. Research shows that nearly 30% of caregivers experience emotional or physical stress, underscoring the importance of acknowledging one's boundaries. Additionally, 30% of caregivers need help managing their emotional or physical stress, highlighting the challenges they face. Resources such as counseling services and support groups can offer vital assistance, helping caregivers navigate their responsibilities more effectively.
Take, for example, Theresa Wilbanks, a support worker who faced burnout. She emphasizes the importance of setting boundaries and seeking help. Similarly, former Wisconsin Governor Marty Schreiber learned the hard way about the significance of asking for help during his caregiving journey. Mental health experts stress that caregivers must prioritize their well-being to sustain their support efforts. Signs of provider exhaustion include emotional numbness, fatigue, and social withdrawal, which can significantly impact their ability to provide support.
Utilizing available resources, like support groups and respite care, can ease some of the challenges caregivers encounter. These networks not only offer practical support but also foster a sense of community, reminding individuals that they are not alone in their journey. Support groups are often seen as a lifeline for caregivers, providing vital connections and shared experiences that can help alleviate feelings of isolation.
Explore Available Care Options and Resources
When it comes to supporting individuals with cognitive impairment, the choices available can truly make a difference in their quality of life. It’s essential to recognize the emotional challenges caregivers face, as they often experience stress and burnout while trying to provide the best care possible. Thankfully, there are several options that not only offer practical assistance but also nurture the well-being of both the individual and their caregiver.
-
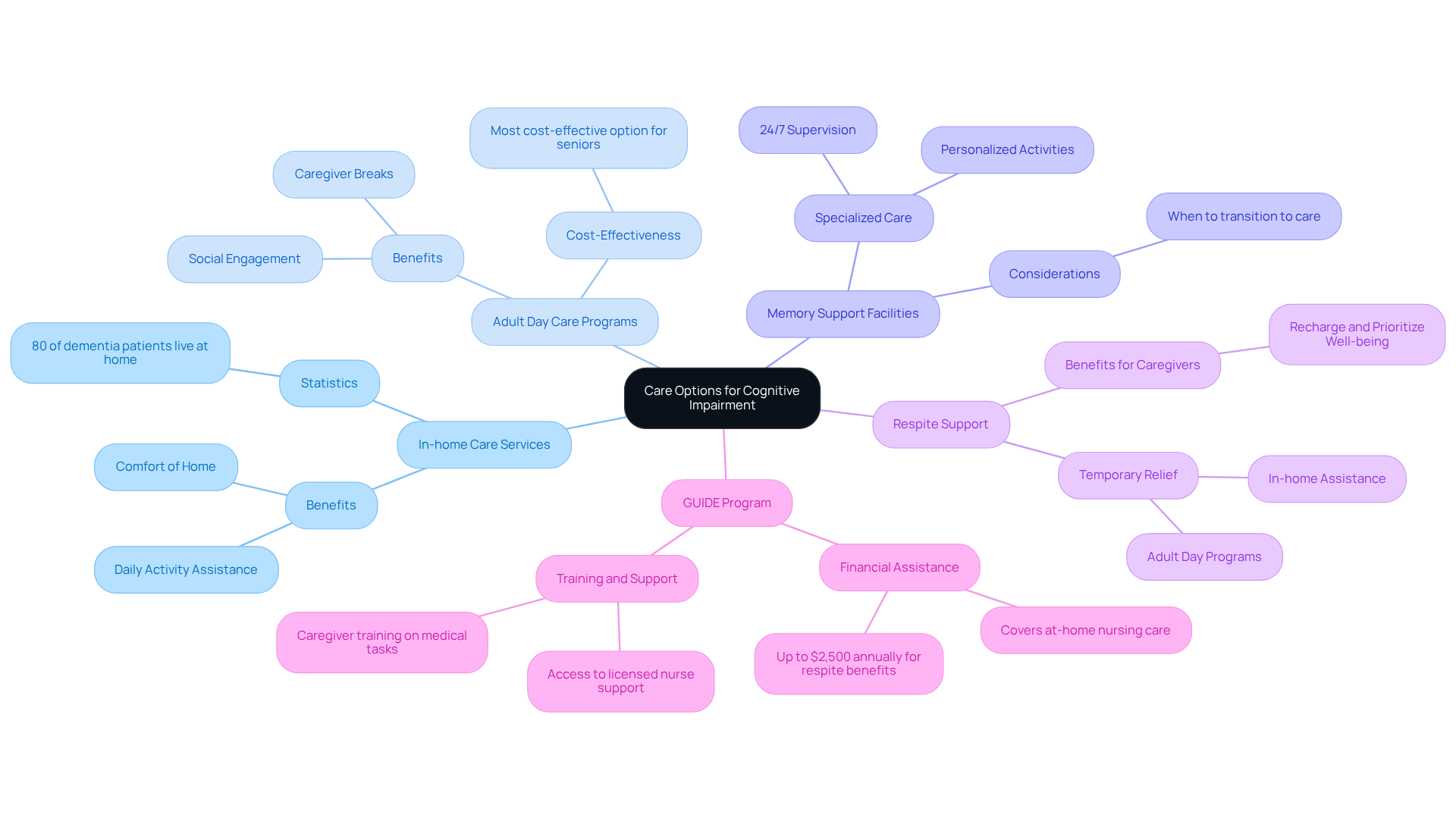
In-home care services stand out as a compassionate choice. Professional caregivers can help with daily activities, allowing individuals to stay in the comfort of their own homes. This familiarity promotes a sense of safety, which is crucial for those with cognitive impairment. In fact, studies show that nearly 80% of dementia patients live at home with family members, underscoring the importance of maintaining this environment for as long as possible.
-
Adult day care programs provide organized activities and social engagement throughout the day. This gives caregivers the necessary breaks they need. According to the 2024 Genworth and CareScout Cost of Care Survey, adult day services are recognized as the most cost-effective option for seniors and adults with developmental disabilities. These programs not only alleviate caregiver stress but also enhance participants' well-being through engaging activities tailored to their needs. As Mary Michlovich, the executive director of OPICA, poignantly states, "Everyone is living longer and they’re being diagnosed (with dementia-related issues) so much younger. The need has exploded but the funding support is just not there." This highlights the growing demand for such vital services.
-
For those needing more specialized care, it is important to consider when should dementia patients go into care at memory support facilities that offer a safe haven. These living options are designed specifically for individuals with cognitive impairment, providing 24/7 supervision and personalized activities. They focus on creating a supportive environment that addresses the unique challenges faced by dementia patients, particularly in determining when should dementia patients go into care.
-
Respite support is another invaluable service. It offers temporary relief for primary caregivers, ensuring that their loved ones receive assistance while they take a much-needed break. Respite services can be arranged through in-home assistance or adult day programs, allowing caregivers to recharge and prioritize their own well-being.
-
Additionally, the recently introduced GUIDE program provides financial assistance and support for caregivers, enabling them to access necessary services without incurring extra costs. This initiative aims to enhance the quality of life for individuals with cognitive impairment while reducing the strain on unpaid caregivers.
To make informed decisions, it’s advisable to utilize online resources, local agencies, and community support groups to gather information about these options. Visiting facilities in person can also provide valuable insights into their suitability, including staff training, safety measures, and the types of activities offered. Engaging with these resources can help families navigate the complexities of cognitive decline support and discover the best solutions for their loved ones.
Consult Healthcare Professionals for Guidance
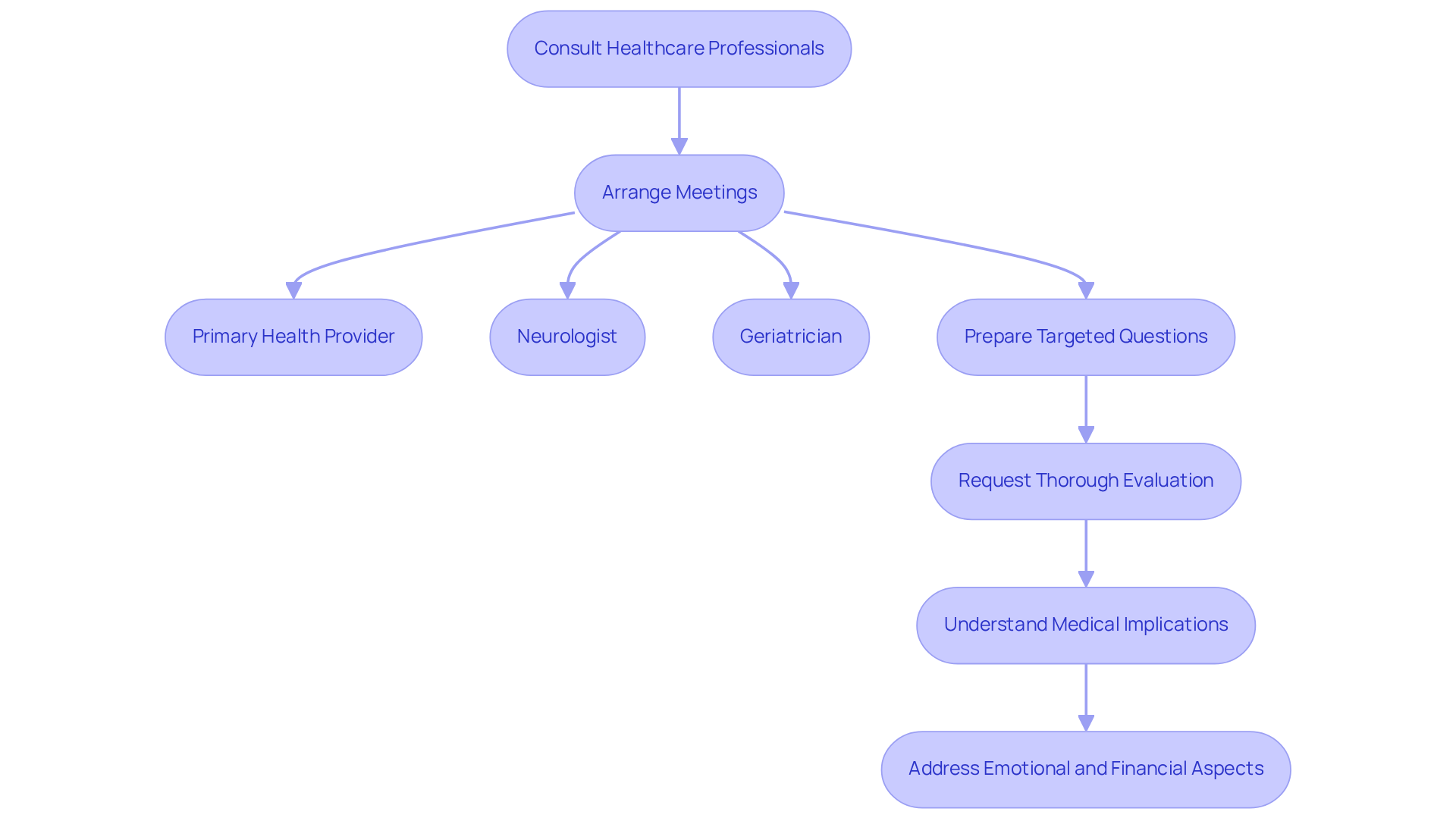
Interacting with healthcare experts is so important for families dealing with cognitive decline. It’s a good idea to arrange meetings with the person’s primary health provider, neurologist, or geriatrician to gain valuable insights. To make the most of these appointments, prepare a list of targeted questions, such as:
- What stage of dementia is my loved one currently experiencing?
- What changes can we expect in their condition over time?
- What support options do you suggest based on their current needs?
Request a thorough evaluation that includes cognitive assessments and tailored treatment recommendations. This expert advice is essential for understanding the medical implications of your loved one’s situation and will significantly influence decisions regarding when should dementia patients go into care. Neurologists emphasize that early and ongoing consultations can lead to better outcomes, as they equip families with the knowledge needed to make informed choices that align with the patient’s evolving needs.
Moreover, studies like the D-CARE trial, which evaluated various dementia treatment methods with 2,176 participants, highlight the importance of specialized program offerings. Engaging with healthcare experts can also enhance the self-efficacy of those providing support, which has been shown to improve within six months of service delivery. Additionally, being aware of the latest FDA-approved medications, such as donanemab and lecanemab, that target amyloid in the brain can offer families insights into treatment options.
Ultimately, addressing the emotional and financial aspects of dementia care is crucial for family caregivers when should dementia patients go into care as they navigate these challenging decisions. Remember, you’re not alone in this journey; there’s support available to help you every step of the way.
Key Takeaways for Caregivers
Determining when dementia patients should transition into care can be a deeply emotional journey. It’s a multifaceted process that requires careful consideration of various factors. It’s essential to assess both the individual’s needs and the caregiver’s capacity, ensuring that both parties receive the support necessary for their well-being. By understanding the complexities of cognitive impairment and the resources available, families can make informed decisions that truly enhance the quality of life for their loved ones.
Key insights from this guide highlight the critical steps involved in this decision-making process:
- Evaluating daily living capabilities
- Ensuring safety in the home
- Recognizing the emotional readiness of caregivers
Exploring available care options - from in-home services to specialized memory support facilities - can provide the necessary assistance while promoting a nurturing environment for those affected by dementia. Consulting healthcare professionals can further enrich this process, offering expert guidance tailored to the unique circumstances of each individual.
Ultimately, navigating the challenges of dementia care requires a heartfelt commitment to seeking help and utilizing available resources. Families are encouraged to engage with support networks, healthcare providers, and community services to foster a collaborative approach to caregiving. By prioritizing both the needs of the dementia patient and the well-being of the caregiver, a more compassionate and effective care journey can be achieved. Remember, you’re not alone in this; there’s a community ready to support you every step of the way.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5MWZhYzVhMDFkMDk4M2JlYjM1N2I1ZiIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What should I assess when evaluating an individual's care needs?
You should assess the individual's daily living capabilities, focusing on their ability to perform activities of daily living (ADLs) such as bathing, dressing, eating, and managing medications. Additionally, it's important to evaluate safety concerns in their living environment, including clutter, inadequate lighting, and potential hazards that could lead to falls.
Why is it important to focus on safety concerns in the living environment?
Safety concerns are critical because they can significantly impact the individual's well-being. With over 6 million Americans currently living with cognitive impairment and projections of 14 million cases by 2060, addressing these safety issues becomes increasingly urgent to prevent accidents and ensure a safe living space.
How can I assess an individual's cognitive abilities?
You can assess cognitive abilities by observing if the individual can remember important information, follow conversations, or recognize familiar faces. Documenting these observations will help create a clearer picture of their current cognitive situation.
Why is involving family members important in the evaluation process?
Involving family members or support persons is essential because their insights into the individual's behavior and needs can provide valuable information that aids in the assessment and understanding of the individual's situation.
Are there tools available to assist in the assessment process?
Yes, specific checklists or assessment tools, such as the Brain Health Toolkit available in both English and Spanish, can help ensure a thorough evaluation of the individual's care needs and living conditions.
What is the ultimate goal of assessing care needs and living conditions?
The ultimate goal is to guide decisions regarding support options and resources, ultimately enhancing the quality of life for those affected by dementia and determining when dementia patients may need to go into care.

