
Understanding When Should Someone with Alzheimer
Understanding the complexities of Alzheimer's disease is crucial. It affects millions and brings unique challenges for families. As the disease progresses through its distinct stages, recognizing when to transition a loved one to care becomes vital for ensuring their safety and well-being.
What signs should families look for? How can they navigate the emotional landscape of care options? These are critical questions that many face. Exploring them can empower families to make informed decisions during this challenging journey.
It's important to acknowledge the emotional weight of these decisions. Caregivers often experience stress and burnout, feeling overwhelmed by the responsibilities they carry. But there is support available. By sharing personal stories and testimonials, we can highlight the compassionate care that makes a difference.
As families navigate this path, they can find reassurance in knowing they are not alone. Together, we can explore the options and find the best solutions for their loved ones.
Understand Alzheimer's Disease and Its Stages
Alzheimer's disease is a progressive neurological disorder that deeply affects memory, thinking, and behavior. It typically unfolds in three distinct stages, each presenting unique challenges for individuals and their loved ones.
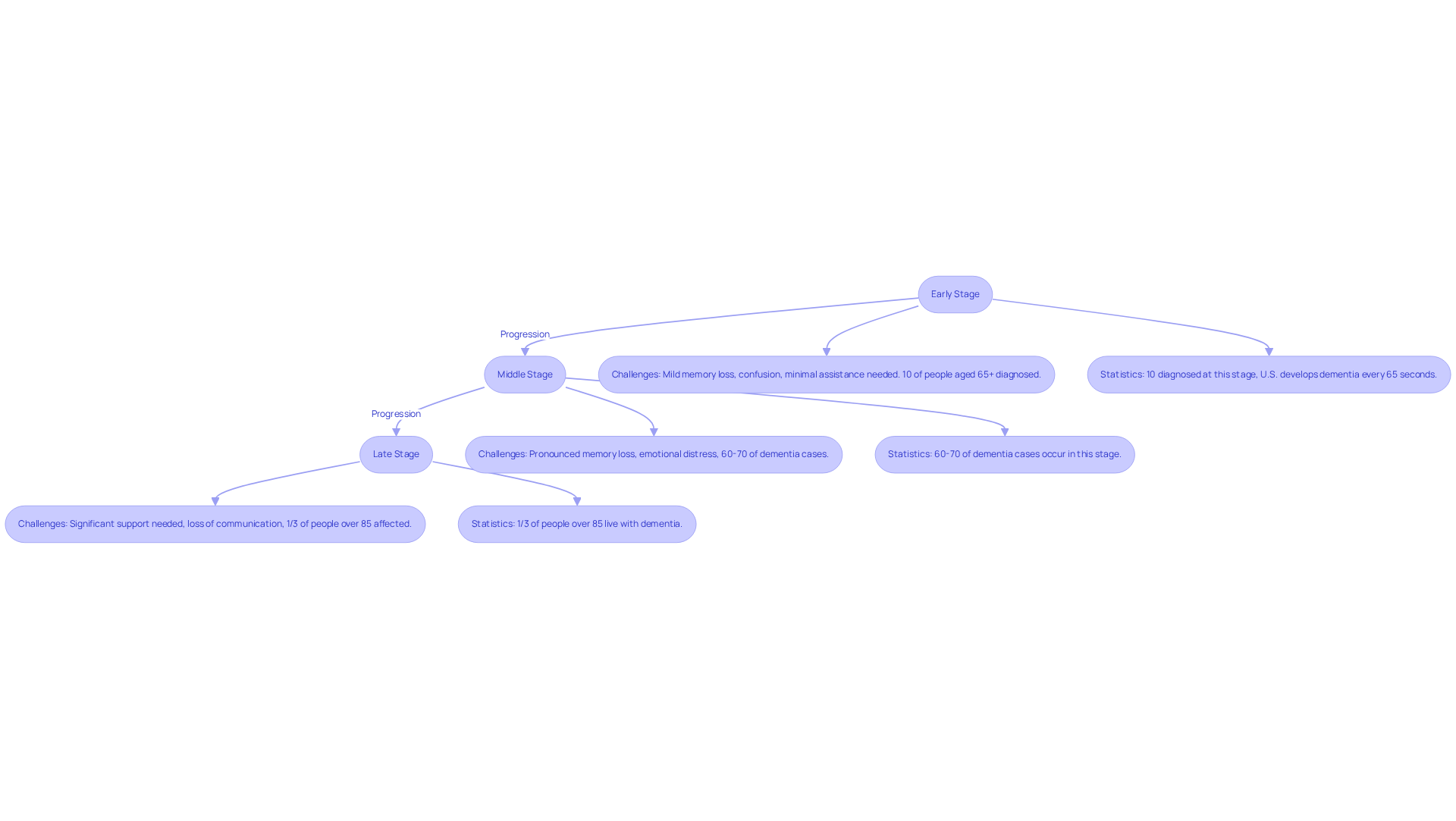
Early Stage: In this initial phase, individuals may face mild memory loss and confusion. They often manage daily activities with minimal assistance, but the strain can be felt by those around them. About 10% of people aged 65 and older are diagnosed at this stage. In the U.S., someone develops dementia every 65 seconds, a rate that’s expected to double by mid-century. This statistic can be overwhelming, but understanding it is the first step toward providing support.
Middle Stage: As the disease progresses, memory loss becomes more pronounced. Individuals may struggle to recognize their loved ones or perform familiar tasks, leading to emotional distress for both them and their caregivers. This phase accounts for approximately 60-70% of dementia cases, and caregivers often report increased difficulties in providing assistance. It’s a time when compassion and understanding are crucial.
Late Stage: In this final phase, individuals require significant support with daily activities. They may lose the ability to communicate and often need constant supervision. It’s estimated that one-third of people over 85 years old live with dementia, highlighting the urgent need for comprehensive support solutions. Projections suggest that by 2060, more than 13.9 million Americans will be living with this disease, underscoring the importance of community and care.
Understanding these phases is vital for families. It allows them to anticipate the changing support needs of their loved ones. Neurologists stress that recognizing the signs of progression can lead to timely interventions and support. Recent research emphasizes the importance of early diagnosis and intervention. Studies show that new treatments can slow disease progression when administered early. A groundbreaking blood biomarker has even been discovered, capable of identifying early tau pathology-a crucial sign of dementia-before it becomes detectable through imaging.
As the field of memory loss research evolves, families are encouraged to stay informed about developments that may impact their support strategies. Amy Arnsten highlights the need for effective drugs with fewer side effects, reinforcing the significance of ongoing research in dementia treatment. Together, we can navigate this journey with compassion and understanding.
Recognize Signs That Indicate a Need for Care
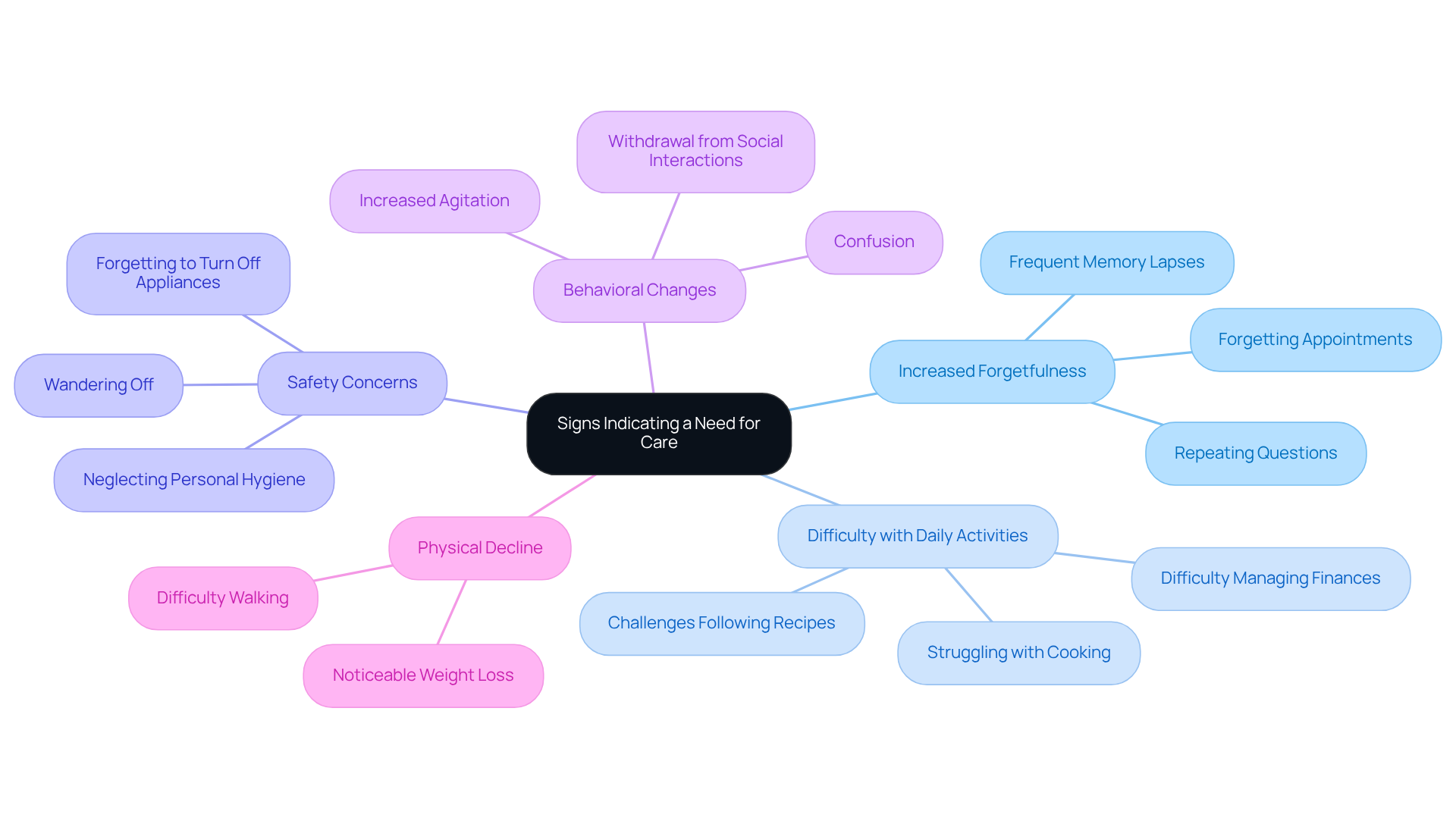
Recognizing when a loved one with Alzheimer's needs extra care can be challenging, but several signs can help guide you:
-
Increased Forgetfulness: If you notice frequent memory lapses-like forgetting appointments or repeating questions-this could be a sign. With nearly 7 million Americans living with Alzheimer's, persistent memory loss can significantly disrupt daily life. It's important to remember that 79% of Americans wish to know if they have dementia before symptoms arise, underscoring the need for early detection.
-
Difficulty with Daily Activities: Struggling with everyday tasks, such as cooking, cleaning, or managing finances, can indicate a decline in cognitive function. Your loved one may find it harder to follow recipes or keep track of medications, highlighting the importance of support during these times.
-
Safety Concerns: Increased risks, like wandering off, forgetting to turn off appliances, or neglecting personal hygiene, can pose serious dangers. It's crucial for families to stay alert to these behaviors, as they can lead to hazardous situations.
-
Behavioral Changes: If you notice significant shifts in mood or behavior-like increased agitation, confusion, or withdrawal from social interactions-this may signal that your loved one is struggling. These mood and personality changes can be distressing for both the individual and their family.
-
Physical Decline: Keep an eye out for observable changes in physical health, such as noticeable weight loss or difficulty walking. These issues can complicate the support your loved one needs, making monitoring essential for timely intervention.
Identifying these signs early can prompt important conversations about care options, such as when should someone with Alzheimer's go into care, ensuring your loved one receives the support they need before things become critical. With the number of people living with dementia expected to nearly double by 2050, taking proactive steps is vital for effective management. For more insights on distinguishing between normal aging and dementia signs, families can visit 10signs.org.
Explore Care Options: In-Home vs. Residential Care
When families consider care options for someone with Alzheimer's, they often find themselves facing two primary choices that can feel overwhelming:
-
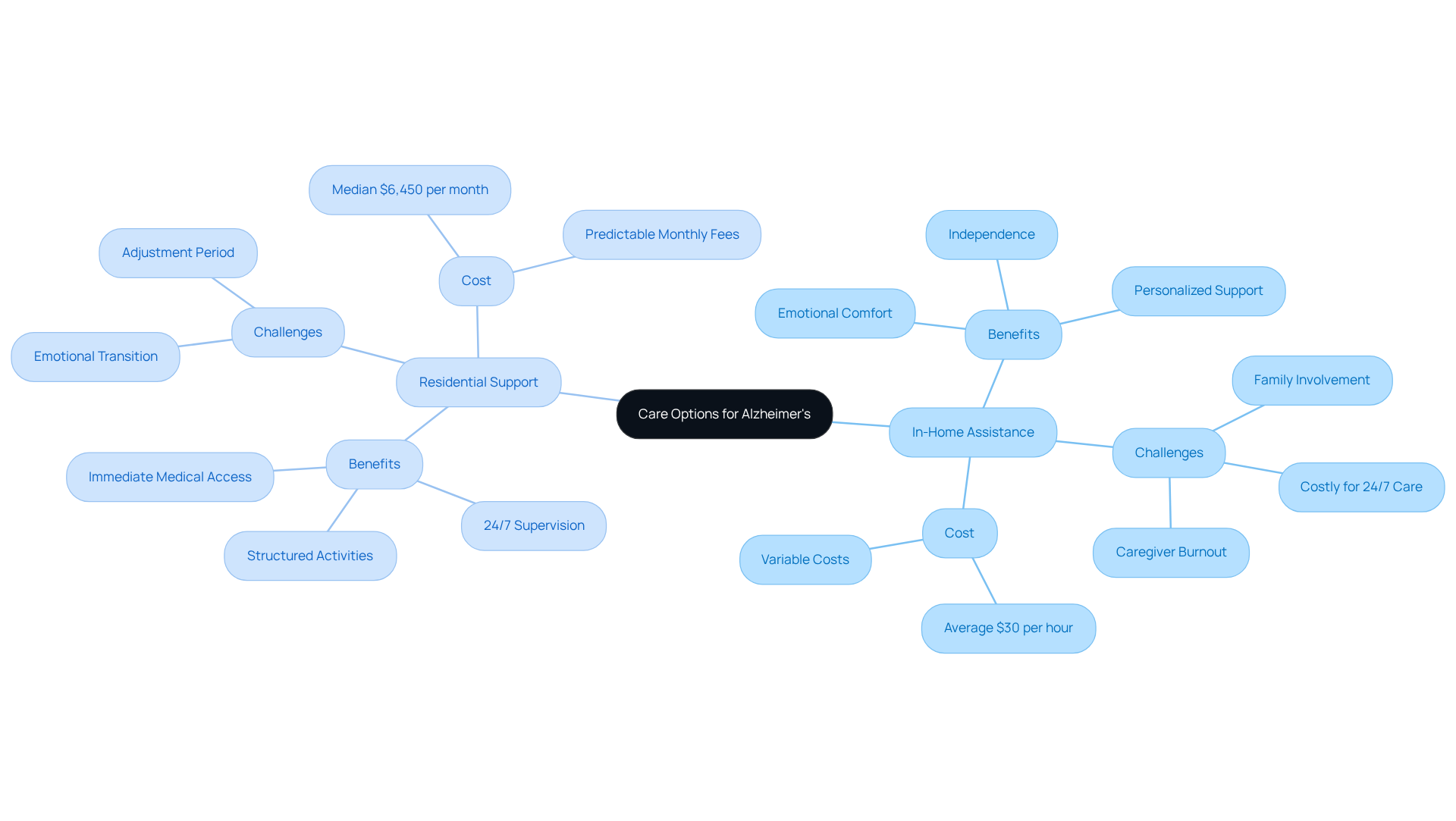
In-Home Assistance: This option allows individuals to remain in the comfort of their own homes while receiving personalized support. Services can include companionship, help with daily activities, and medical assistance. The emotional comfort of familiar surroundings can help slow cognitive decline and improve overall quality of life. In-home assistance promotes independence and offers customized support, but it may require significant family involvement and can become costly, especially if 24/7 supervision is needed. Typically, in-home support costs around $30 per hour, which can rise considerably based on the level of assistance required, particularly if continuous help is essential.
-
Residential Support: Memory support facilities provide specialized assistance in a structured environment designed specifically for individuals with Alzheimer's. These facilities offer 24/7 supervision, immediate access to medical care, and activities tailored to cognitive abilities, enhancing safety and quality of life. While this option can relieve family caregivers from daily pressures, the transition can be emotionally challenging for both the individual and their family. The national median cost for memory support is about $6,450 monthly, which may be more predictable compared to the variable costs of in-home services.
Families should carefully assess their loved one's needs, preferences, and the level of assistance required to understand when should someone with Alzheimer's go into care. It's crucial to consider safety concerns and oversight needs, as these factors can significantly impact the suitability of each support option. Engaging with facility directors can provide valuable insights into the benefits of memory support, while exploring successful in-home assistance examples can illustrate how tailored care can effectively meet the needs of Alzheimer's patients. Additionally, families should be mindful of the risk of caregiver burnout, which can arise from the demands of providing in-home assistance.
Communicate with Family and Plan for Care Transitions
Transitioning to a new support arrangement can be quite challenging for families. It’s important to acknowledge the emotional weight this process carries. Here are some steps to help facilitate communication and planning:
-
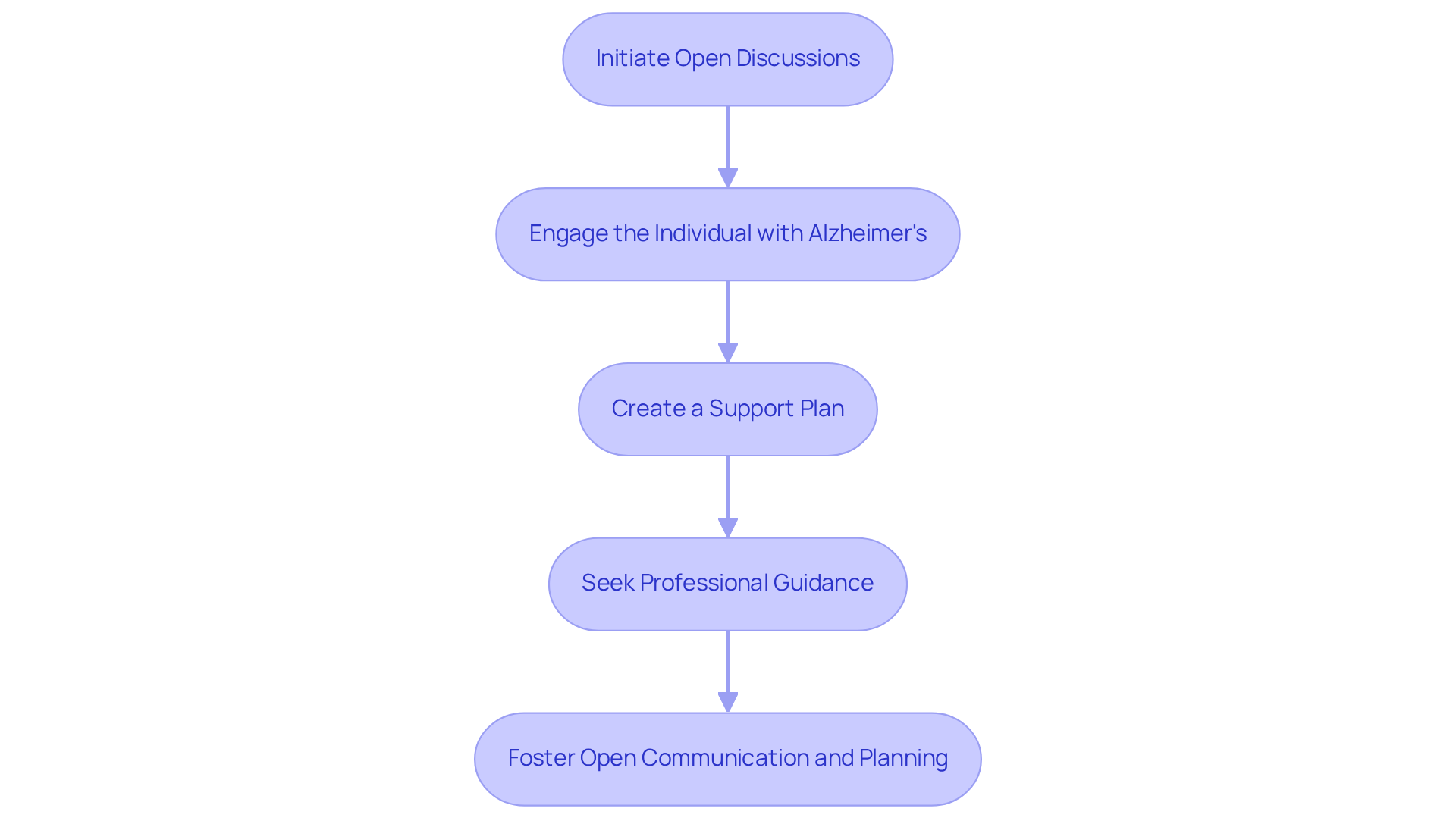
Initiate Open Discussions: Encourage family members to share their observations and concerns about their loved one’s condition. Specific examples can help illustrate any changes in behavior or health, making it easier to understand the situation.
-
Engage the Individual with Alzheimer's: Whenever possible, involve the person in conversations about their preferences and needs. This involvement can empower them, helping them feel more in control and respected during this transition.
-
Create a Support Plan: Collaboratively develop a support plan that outlines the type of assistance needed, preferred providers, and any financial considerations. It’s essential to revisit this plan regularly, as the individual’s needs may change over time.
-
Seek Professional Guidance: Don’t hesitate to consult with a senior support advisor or healthcare expert. Their insights can be invaluable in identifying the best assistance options and resources available.
By fostering open communication and planning together, families can navigate the complexities of care transitions more effectively. Remember, you’re not alone in this journey; support is available, and together, you can create a nurturing environment for your loved one.
Key Takeaways for Caregivers
Deciding when to transition a loved one with Alzheimer's to care is a deeply emotional and complex journey that many families face. As the disease progresses, it can profoundly affect an individual's ability to live independently, making it essential to approach care decisions with thoughtfulness and compassion. By recognizing the signs of cognitive decline and understanding the various stages of Alzheimer's, families can make informed choices about when to seek additional support.
Key indicators like increased forgetfulness, challenges with daily activities, safety concerns, behavioral changes, and physical decline are vital signals that a loved one may need more extensive care. Families often find themselves weighing the benefits and challenges of in-home assistance versus residential support, all while considering their loved one's unique needs and the emotional impact of these transitions. Open communication among family members, along with involving the individual with Alzheimer's in discussions about their care, can create a supportive environment that eases the transition process.
Ultimately, navigating the journey of Alzheimer's care requires compassion, understanding, and proactive planning. By staying informed about the stages of the disease and recognizing the signs that indicate a need for care, families can better prepare for the future. Embracing available resources and seeking professional guidance empowers families to make decisions that prioritize their loved one's well-being, ensuring they receive the necessary support to maintain a quality of life throughout the progression of the disease. Remember, you are not alone in this journey; there are compassionate services available to help you every step of the way.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5MWU1YWMwMDAzNjA5ODRkZWZlZjlhYiIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What is Alzheimer's disease?
Alzheimer's disease is a progressive neurological disorder that significantly affects memory, thinking, and behavior.
What are the stages of Alzheimer's disease?
Alzheimer's disease typically unfolds in three distinct stages: Early Stage, Middle Stage, and Late Stage, each presenting unique challenges for individuals and their loved ones.
What are the characteristics of the Early Stage of Alzheimer's?
In the Early Stage, individuals may experience mild memory loss and confusion but can manage daily activities with minimal assistance. About 10% of people aged 65 and older are diagnosed at this stage.
How frequently does someone develop dementia in the U.S.?
In the U.S., someone develops dementia every 65 seconds, and this rate is expected to double by mid-century.
What happens during the Middle Stage of Alzheimer's?
During the Middle Stage, memory loss becomes more pronounced, and individuals may struggle to recognize loved ones or perform familiar tasks, leading to emotional distress for both them and their caregivers.
What percentage of dementia cases does the Middle Stage account for?
The Middle Stage accounts for approximately 60-70% of dementia cases.
What are the challenges faced in the Late Stage of Alzheimer's?
In the Late Stage, individuals require significant support with daily activities, may lose the ability to communicate, and often need constant supervision.
What is the estimated prevalence of dementia in individuals over 85 years old?
It's estimated that one-third of people over 85 years old live with dementia.
Why is understanding the phases of Alzheimer's important for families?
Understanding these phases helps families anticipate the changing support needs of their loved ones, allowing for timely interventions and support.
How can early diagnosis and intervention impact Alzheimer's disease progression?
Early diagnosis and intervention can lead to timely support and may slow disease progression, as new treatments can be more effective when administered early.
What recent advancements have been made in Alzheimer's research?
A groundbreaking blood biomarker has been discovered that can identify early tau pathology, a crucial sign of dementia, before it becomes detectable through imaging.
What is the significance of ongoing research in dementia treatment?
Ongoing research aims to develop effective drugs with fewer side effects, which is essential for improving care and support for individuals with dementia.

