
For families in our service areas
For families in our service areas, this guide explains dementia care and how non-medical in-home caregiving can support care planning in East Idaho, Treasure Valley & Magic Valley, Northern Wasatch, North Central West Virginia, and Northeast Ohio.
The Importance of Why Do Dementia Patients Not Want to
Dementia profoundly alters not just cognitive abilities but also essential aspects of daily life, like appetite and eating habits. It’s heartbreaking to see how this condition can affect something as fundamental as nourishment. Understanding why dementia patients often refuse to eat reveals a complex interplay of psychological and physical factors that can significantly impact their well-being.
What drives this aversion to food? Caregivers often feel overwhelmed by the emotional weight of these challenges. It’s important to recognize that this struggle is not just about food; it’s about the deep connection we have with nourishment and care. By addressing these issues with compassion, caregivers can help ensure that their loved ones receive the nutrition they need.
In this journey, caregivers can find support and solutions that not only enhance the quality of life for those they care for but also alleviate their own feelings of stress and burnout. Together, we can navigate these challenges, fostering a nurturing environment that prioritizes both emotional and physical well-being.
Explore Psychological Factors Affecting Appetite in Dementia
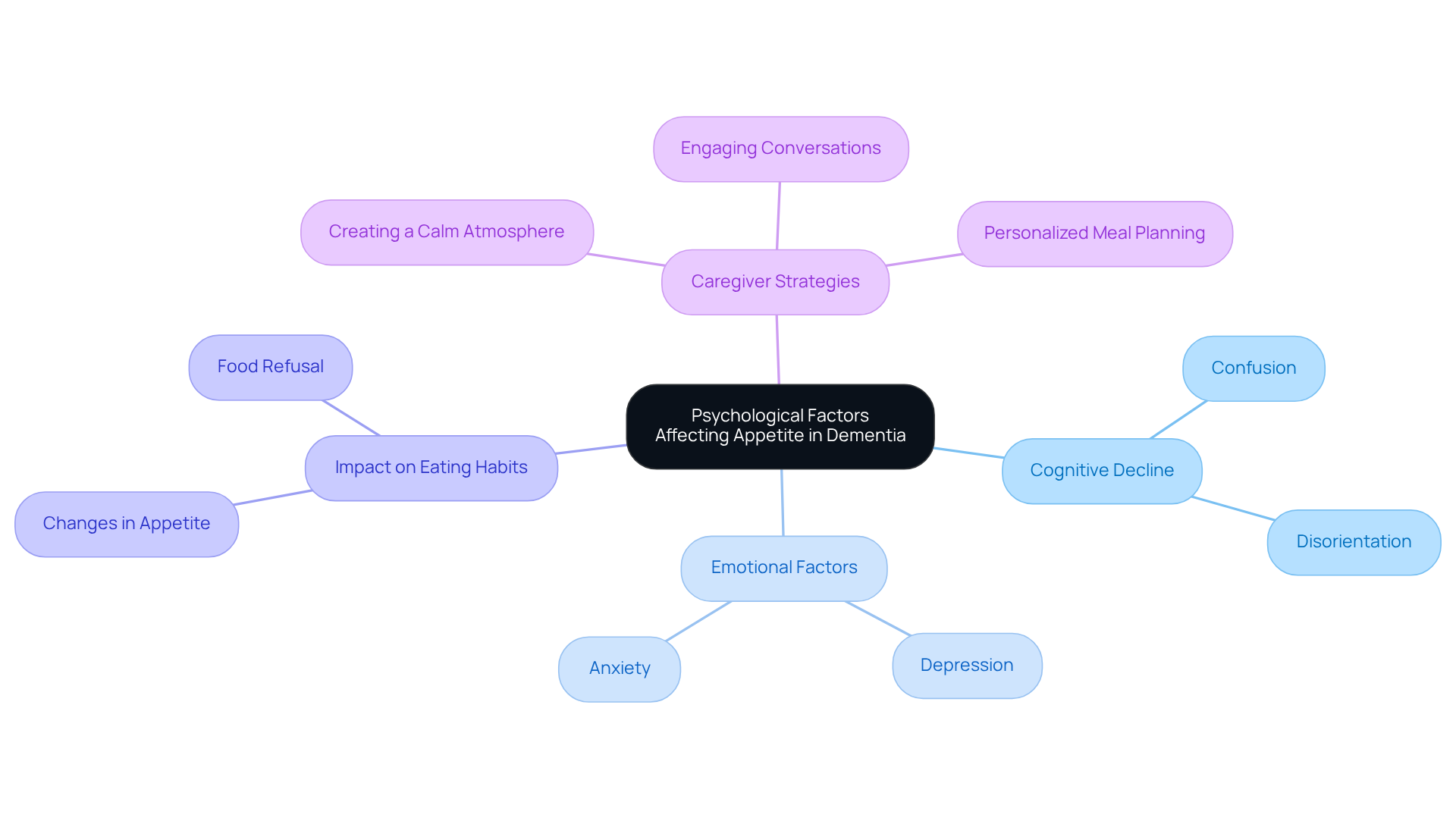
Dementia can deeply affect a person's psychological state, prompting us to consider why do dementia patients not want to eat, which leads to significant changes in appetite and eating habits. It’s not uncommon for cognitive decline to cause confusion and disorientation, making it tough for individuals to recognize meals or grasp mealtime routines. Emotional factors, such as depression and anxiety, are reasons for why do dementia patients not want to eat. For instance, someone might feel overwhelmed by the act of eating or connect mealtime with negative experiences, which raises the question of why do dementia patients not want to eat.
Research shows that about 33% to 60% of individuals with cognitive impairment experience depression, which plays a crucial role in appetite loss. As caregivers, it’s vital to recognize these psychological influences and take steps to promote emotional well-being. Creating a calm mealtime atmosphere and engaging individuals in pleasant conversations can help rekindle their interest in food.
Moreover, understanding how mental health and nutrition intersect is essential. Poor dietary habits can worsen mental health issues, creating a cycle that further affects appetite and overall health. By addressing these concerns with compassion and care, we can make a meaningful difference in the lives of those we support.
Examine Physical Challenges Impacting Eating Habits
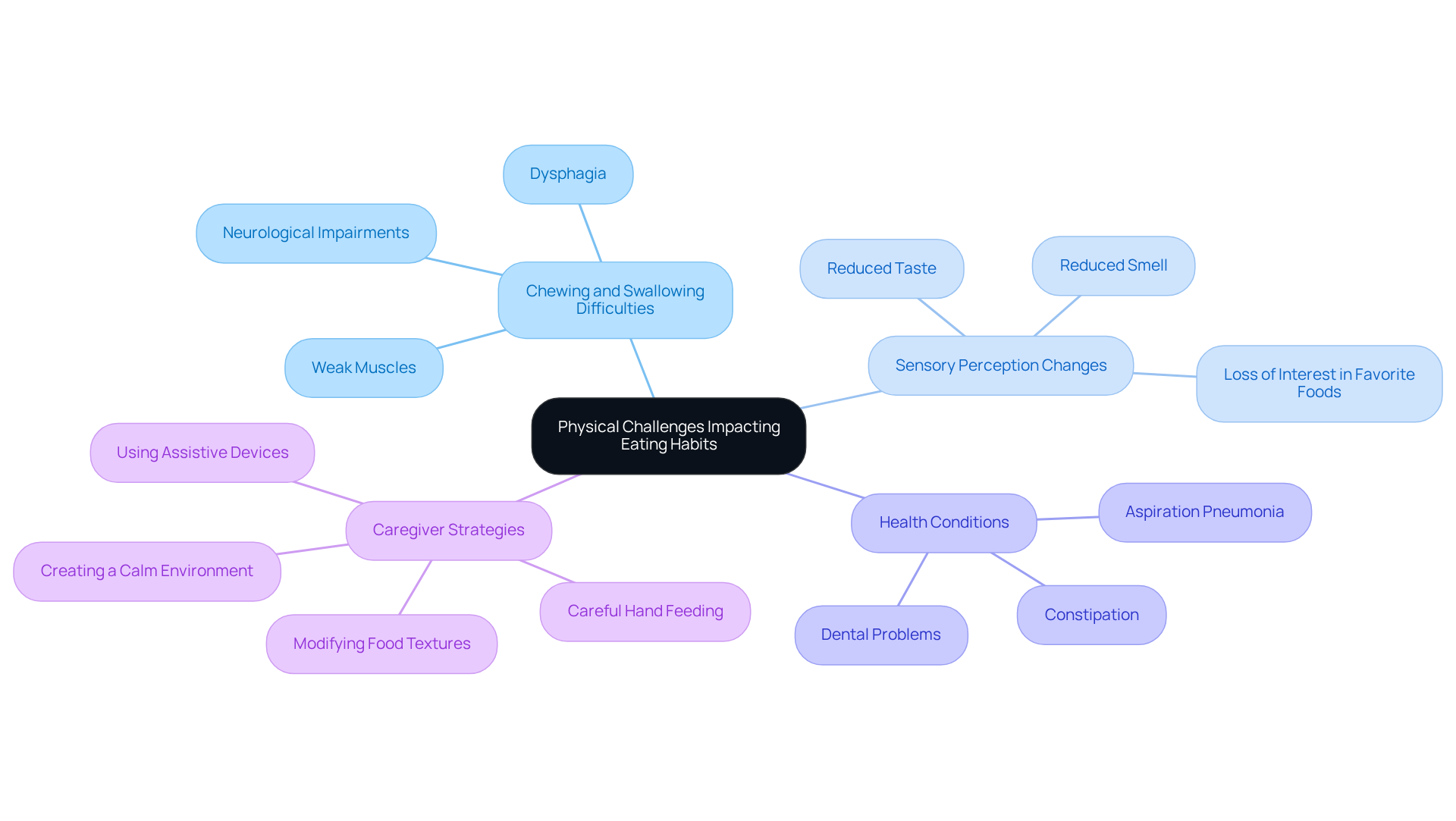
As cognitive decline progresses, patients encounter various physical challenges that can significantly impact why do dementia patients not want to eat. Chewing and swallowing difficulties, affecting 13-57% of individuals with dementia, contribute to understanding why do dementia patients not want to eat, often arising from weakened muscles and neurological impairments. These issues can lead to dysphagia, complicating the eating process and increasing the risk of aspiration pneumonia, a leading cause of hospitalization and death in this population, raising questions about why do dementia patients not want to eat. Early identification and treatment with oral antibiotics are vital in managing this risk.
Moreover, changes in sensory perception, such as reduced taste and smell, can raise the question of why do dementia patients not want to eat. Imagine a patient losing interest in their favorite dishes due to these sensory shifts, raising the question of why do dementia patients not want to eat, which can lead to a decreased appetite. Conditions like constipation and dental problems can also cause discomfort during meals, which is a factor in understanding why do dementia patients not want to eat.
Caregivers play an essential role in navigating these challenges. By working closely with healthcare professionals, they can implement effective strategies to support their loved ones. Modifying food textures, such as offering softer or pureed options, can make eating easier. Using assistive devices, like specialized utensils or plates with contrasting colors, can enhance the dining experience. Additionally, careful hand feeding has been recognized as one of the most effective interventions for dysphagia.
By acknowledging and addressing these physical barriers, caregivers can help ensure that individuals with cognitive impairments understand why do dementia patients not want to eat, allowing them to receive the nutrition they need to maintain their health and wellness. Hydration is equally important, as individuals may confuse thirst with hunger, complicating their eating habits. Together, with compassion and understanding, we can make a difference in the lives of those we care for.
Implement Strategies to Encourage Eating in Dementia Care
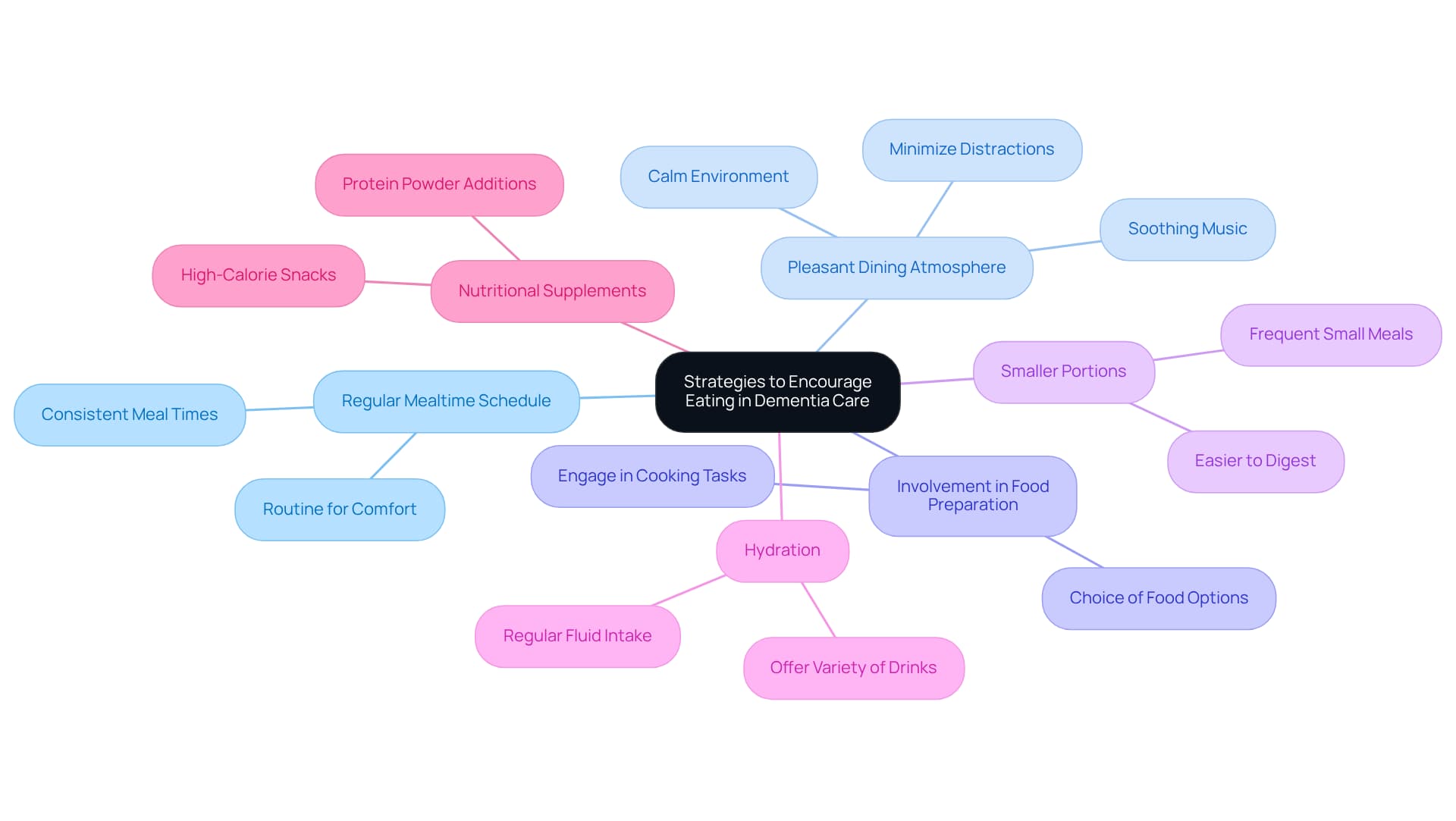
Caring for individuals with cognitive decline can be a challenging journey for caregivers. It’s essential to recognize the emotional weight that comes with this responsibility. Establishing a regular mealtime schedule can provide much-needed structure and familiarity, offering reassurance to those in your care. Research shows that 74%-78% of individuals with dementia face mealtime challenges, raising the question of why do dementia patients not want to eat, which makes routine vital for enhancing their appetite.
Creating a pleasant dining atmosphere is another important step. A calm environment, free from distractions and noise, helps individuals focus on their food. Involving them in the food preparation process can also spark interest in meals. Allowing them to choose from various food options or participate in simple cooking tasks can significantly boost their appetite.
Additionally, serving smaller, more frequent portions can ease the stress of large servings and aid digestion. It’s important for caregivers to remain calm and flexible, adjusting meals to suit the preferences and needs of those they care for. Don’t forget about hydration; offering water, milk, or juice throughout the day is crucial, as many individuals may forget to drink.
In some cases, nutritional supplements might be necessary to ensure adequate caloric intake, particularly when considering why do dementia patients not want to eat, as 68%-70% of them experience low food intake. By implementing these compassionate strategies, caregivers can create a supportive mealtime experience that not only promotes better nutrition but also enhances overall well-being.
Moving Forward with Why Do Dementia Patients Not Want to
Understanding why dementia patients may refuse to eat involves exploring a complex mix of psychological and physical factors. It's crucial to recognize that appetite loss isn't just a behavioral issue; it often reflects deeper emotional and cognitive challenges faced by individuals with dementia.
Psychological factors like depression and anxiety can significantly impact appetite. On top of that, physical challenges such as chewing difficulties and altered sensory perceptions complicate eating habits even further. Caregivers play a vital role in addressing these issues. By creating a supportive mealtime environment, they can promote better nutritional intake.
Fostering an atmosphere of compassion and understanding is essential. Implementing structured routines, engaging individuals in meal preparation, and adapting food textures can greatly enhance the eating experience for dementia patients. This thoughtful approach not only improves their nutritional health but also contributes to their overall well-being. It highlights the profound impact that compassionate care can have on the lives of those affected by dementia.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5MWZkYzVmYTdkMmM5NDAwMmQ5OTU4YyIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
How does dementia affect appetite in patients?
Dementia can lead to confusion and disorientation, making it difficult for individuals to recognize meals or understand mealtime routines, which significantly changes their appetite and eating habits.
What emotional factors contribute to appetite loss in dementia patients?
Emotional factors such as depression and anxiety can cause individuals to feel overwhelmed by eating or associate mealtime with negative experiences, leading to decreased appetite.
What percentage of individuals with cognitive impairment experience depression?
Research indicates that about 33% to 60% of individuals with cognitive impairment experience depression, which is a significant factor in appetite loss.
What can caregivers do to help improve the eating habits of dementia patients?
Caregivers can create a calm mealtime atmosphere and engage individuals in pleasant conversations to help rekindle their interest in food.
How do mental health and nutrition intersect in dementia patients?
Poor dietary habits can exacerbate mental health issues, creating a cycle that further affects appetite and overall health, highlighting the importance of addressing both mental health and nutrition.