
What You Need to Know About Dementia and Eating: Strategies
Dementia significantly changes how individuals experience food, impacting their taste, appetite, and engagement with meals. This presents a challenge for caregivers, who must navigate these complexities to ensure their loved ones receive proper nutrition. Understanding the neurological basis of these changes is essential for fostering better eating habits and nutritional health.
Caregivers often struggle with dementia-related eating behaviors, which can lead to inadequate nourishment and diminished quality of life. The implications of these challenges are profound, as proper nutrition is vital for maintaining health and well-being in those affected by cognitive decline. So, how can caregivers effectively address these issues?
This article explores practical strategies that empower caregivers to create a supportive dining environment. By enhancing meal appeal and implementing effective techniques, caregivers can significantly improve the quality of life for individuals with dementia. With the right approach, it is possible to ensure that loved ones receive the nourishment they need.
Explore the Connection Between Dementia and Eating Behaviors
The challenges associated with dementia and eating significantly affect how individuals perceive and engage with food, resulting in notable changes in taste and smell. This cognitive decline can diminish the enjoyment of previously favored foods, making them less appealing. As cognitive impairments progress, issues related to dementia and eating may cause individuals to forget to eat or lose track of mealtimes, resulting in irregular nutritional intake. Neurologists emphasize that these changes stem from fundamental neurological alterations, not just behavioral issues. For instance, research shows that those with dementia and eating difficulties often struggle to recognize hunger and thirst signals, complicating their relationship with nourishment.
Caregivers face the critical task of addressing these challenges. Recognizing these issues as integral to dementia and eating allows caregivers to adapt their strategies effectively. Establishing a structured mealtime routine can help individuals maintain a consistent eating schedule. Additionally, experimenting with flavors and textures can make meals more appealing, encouraging better consumption. Understanding the neurological basis of these changes enables caregivers to provide empathetic and effective support, ensuring that the nutritional needs of individuals with cognitive decline are met compassionately.
Identify Common Eating Challenges in Dementia Care
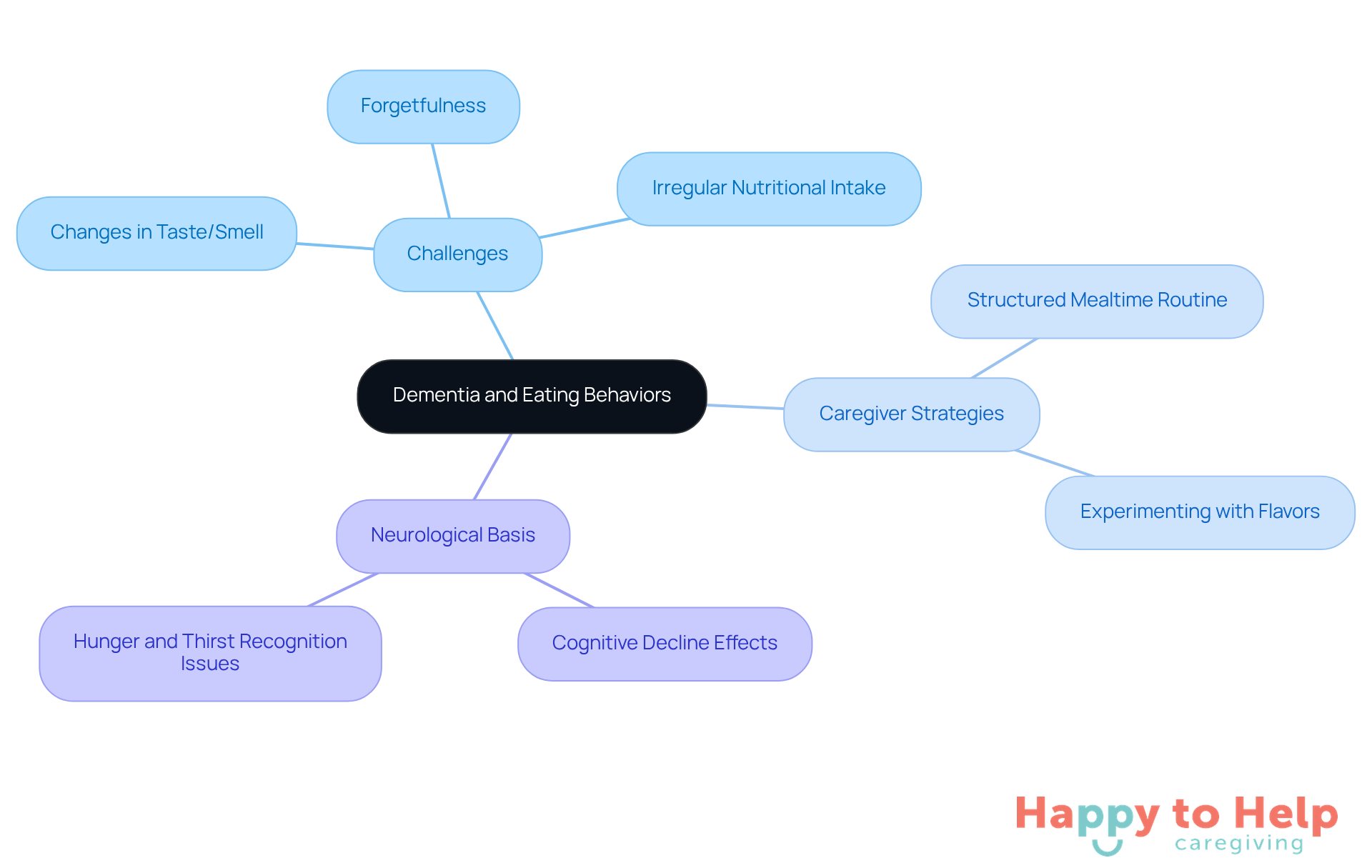
Common eating challenges in dementia care encompass several critical issues:
Problem: Loss of Appetite
A significant number of individuals with dementia experience a marked decrease in interest in food, leading to inadequate nutritional intake. This phenomenon is particularly pronounced in Alzheimer's patients, who are more susceptible to unintentional weight loss compared to their peers. Many individuals with Alzheimer's may experience appetite loss, which affects their dementia and eating habits, without understanding why, complicating their nutritional needs.
Agitate: Difficulty Recognizing Meals
Cognitive decline often results in confusion regarding meal items and utensils, complicating mealtime. As cognitive decline progresses, patients experiencing dementia and eating challenges may struggle to recognize familiar foods, which can further reduce their desire to eat.
Agitate: Swallowing Difficulties
Advanced stages of cognitive decline frequently lead to dysphagia, or difficulty swallowing, heightening the risk of choking and aspiration. Patients with advanced dementia and eating issues commonly experience problems with chewing and swallowing, which can lead to aspiration, weight loss, and malnutrition. This condition necessitates careful monitoring and may require the adjustment of textures to ensure safety during meals.
Agitate: Behavioral Changes
Individuals may display a variety of consumption behaviors, from compulsive overeating to outright refusal of nourishment. These changes can stem from cognitive impairments or emotional factors related to dementia and eating, complicating the caregiving process. For instance, boredom or loneliness may result in comfort consumption, while fatigue can reduce appetite.
Solution: Customized Strategies
Acknowledging these challenges is crucial for caregivers, as it allows them to apply customized strategies that meet the specific needs of each person. Here are some actionable tips:
- Involve patients in meal preparation.
- Present food options with images to help in choosing preferred items.
- Offer smaller, more frequent meals.
- Establish a tranquil dining atmosphere.
Implementing these strategies can greatly improve the dining experience and encourage better nutritional results.
Create a Dementia-Friendly Mealtime Environment
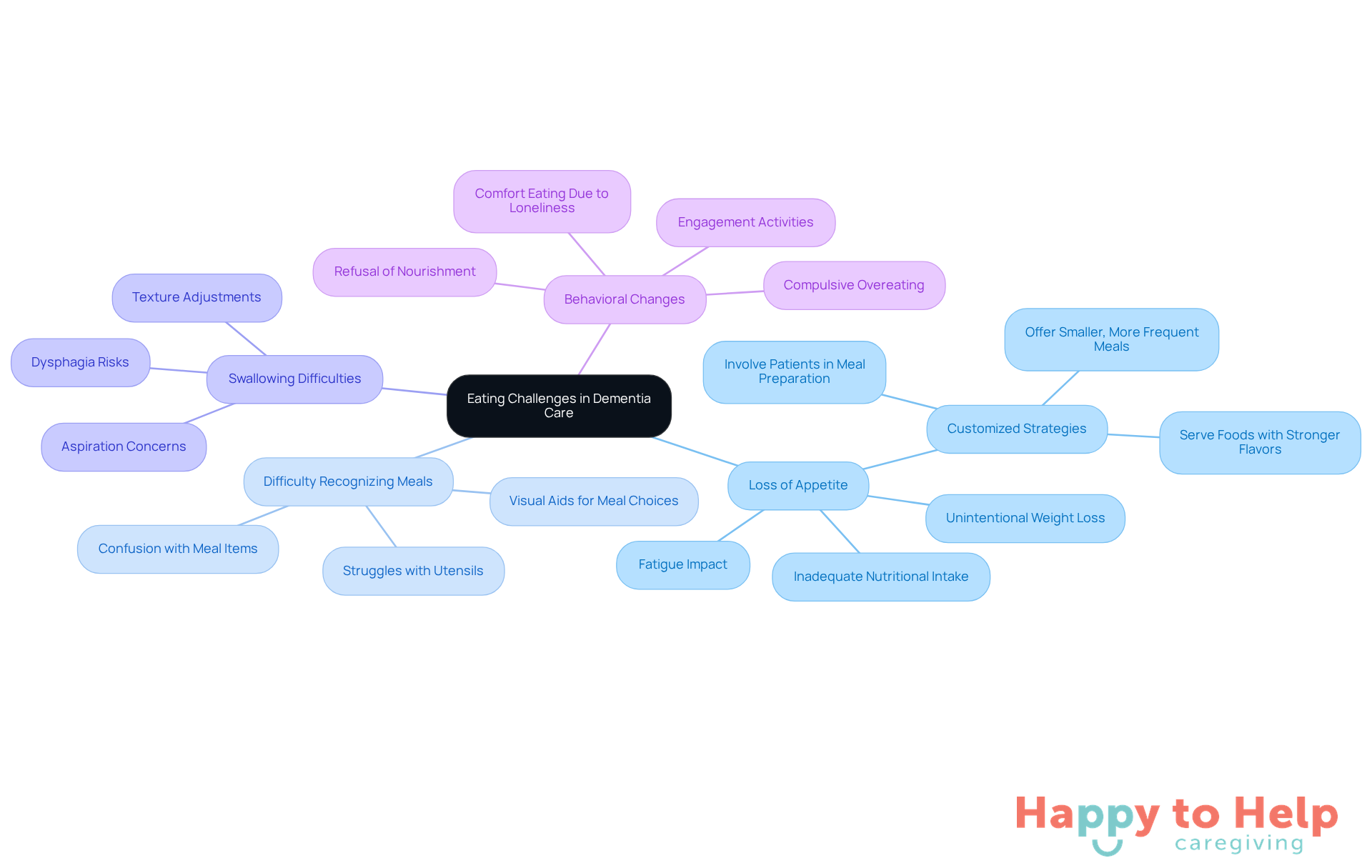
Creating an environment that accommodates dementia and eating presents unique challenges for caregivers. Distractions, such as background noise and visual clutter, can significantly hinder an individual's ability to focus on their meals. This confusion related to dementia and eating can lead to disengagement during mealtimes, making it essential to establish a tranquil atmosphere.
To address this issue, consider the following strategies:
- Minimize Distractions: Reducing background noise and visual clutter is crucial. Occupational therapists emphasize that a calm environment can greatly enhance meal performance for individuals, especially those facing challenges related to dementia and eating, allowing them to concentrate better on their food.
- Use Contrasting Colors: Serving food on plates that contrast with the table setting can improve visibility and appeal. This simple adjustment helps those with cognitive impairments recognize and enjoy their meals more easily.
- Maintain Consistency: Establishing a routine by serving meals at the same time and in the same location fosters comfort and predictability. This consistency can alleviate anxiety and promote healthier eating habits.
- Engage the Senses: Incorporating familiar smells and flavors can stimulate appetite and evoke positive memories, making mealtimes more enjoyable. Research indicates that sensory involvement is vital for individuals with cognitive decline, particularly in the context of dementia and eating, enhancing their overall dining experience.
These adjustments not only improve mealtimes but also promote dignity and independence for those facing challenges related to dementia and eating due to cognitive decline. For instance, case studies like the dementia-friendly dining initiative at Hyllden Heights illustrate the positive effects of tailored dining environments on social interaction and overall well-being. By implementing these strategies, caregivers can create a supportive atmosphere that encourages better dietary habits and enhances the quality of life for those they care for.
Implement Strategies to Enhance Appetite and Nutrition
To enhance appetite and nutrition for individuals, caregivers face a significant challenge related to dementia and eating: ensuring that their loved ones receive adequate nourishment. Dementia and eating can be challenging due to cognitive decline, which may result in poor nutritional health and weight loss.
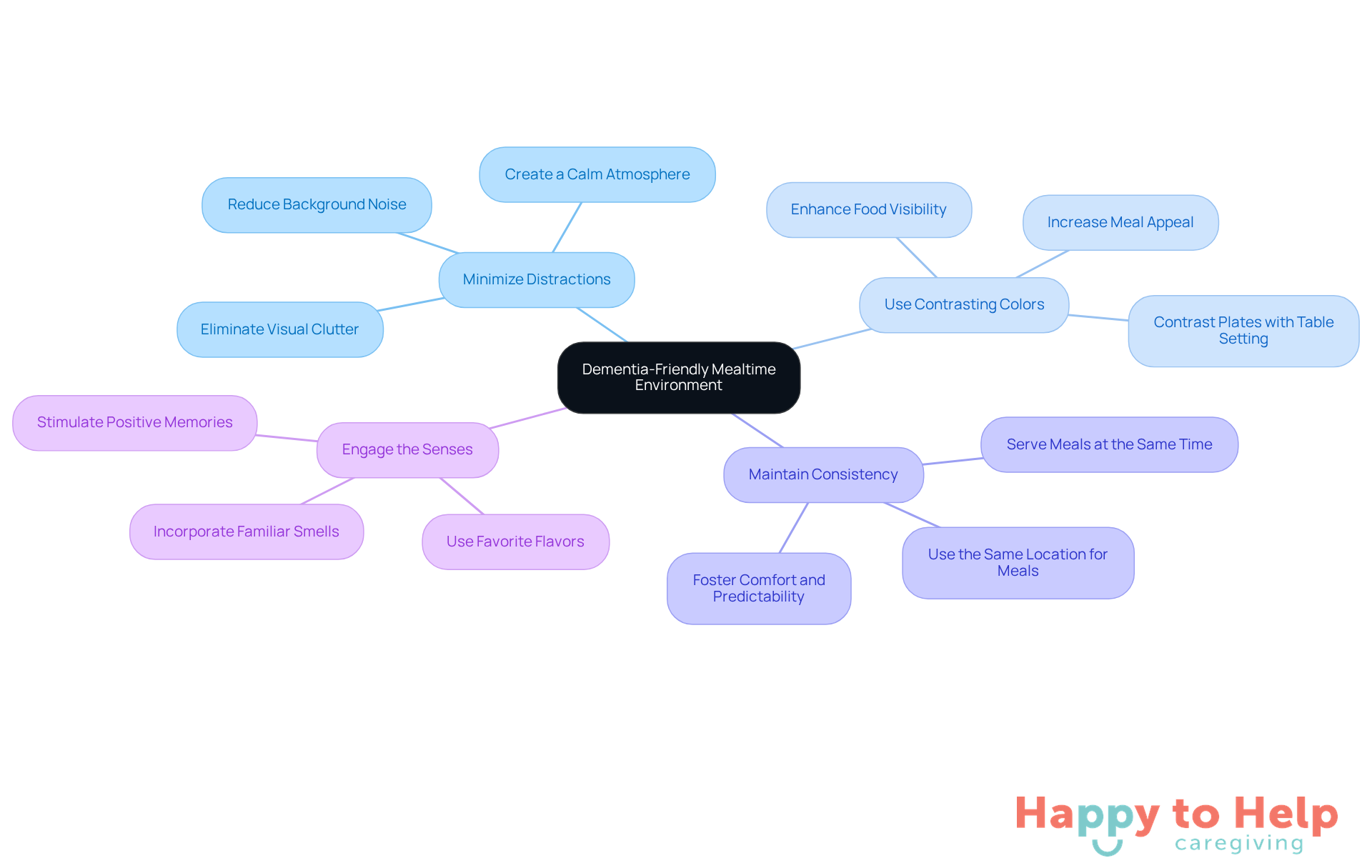
To address this issue, caregivers can implement several effective strategies:
- Offer Smaller, Frequent Meals: Instead of three large meals, provide five to six smaller meals throughout the day. This approach can ease feelings of being overwhelmed and make meals more manageable, as individuals with cognitive decline may struggle with larger portions.
- Incorporate Favorite Foods: Including familiar and enjoyable foods can significantly encourage eating. As preferences may change with the progression of cognitive decline, being flexible and attentive to these changes is crucial.
- Use Flavor Enhancements: Experimenting with herbs and spices can make meals more appealing without relying on salt or sugar. This not only enhances flavor but also supports overall health by reducing sodium intake.
- Encourage Independence: Allowing individuals to participate in meal preparation or choose their meals fosters a sense of control and engagement. This involvement can improve their overall dining experience and encourage better nutritional habits.
- Create a Home-like Dining Atmosphere: Establishing a comfortable and familiar dining environment can enhance the eating experience for people with dementia, making mealtimes more enjoyable.
- Promote Hydration: Encourage caregivers to provide small cups of water or high-water-content items to ensure sufficient hydration, which is crucial for overall well-being.
- Utilize Effective Communication: Caregivers should engage in discussions about food preferences and needs to better support individuals during mealtimes.
- Consider Tiredness: Be mindful of how fatigue can affect a person's ability to eat, and plan mealtimes accordingly to ensure they are alert and engaged.
These strategies are essential for ensuring that individuals facing dementia and eating challenges maintain their nutritional health. Regular, smaller meals can help manage appetite and prevent weight loss. Case studies have shown that tailored approaches, such as these, can lead to improved experiences in dementia and eating, as well as better nutritional outcomes for patients.
Making the Right Choice
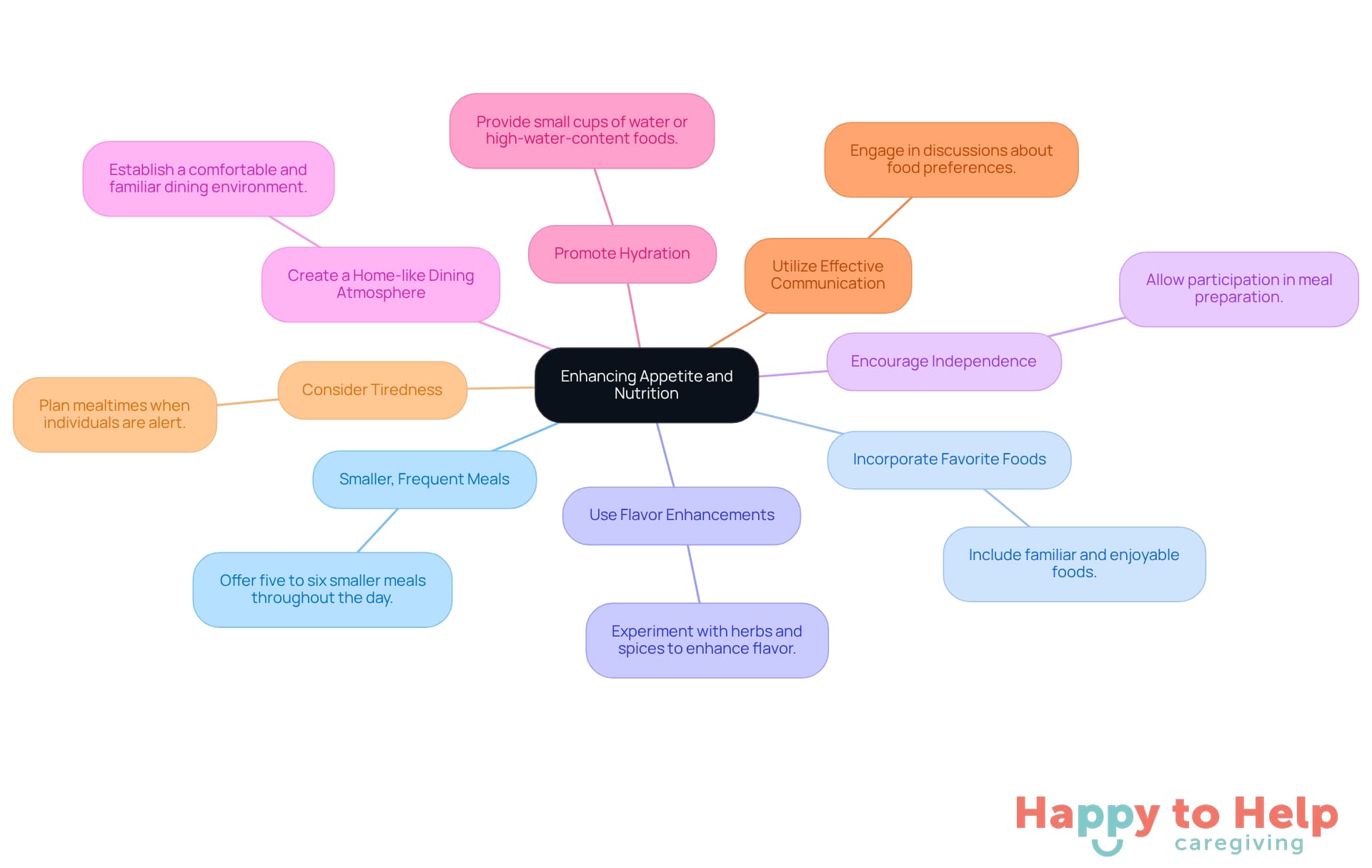
Understanding the relationship between dementia and eating behaviors is essential for caregivers aiming to provide effective support. The cognitive decline associated with dementia significantly affects individuals' perceptions of food, leading to challenges such as loss of appetite, difficulty recognizing meals, and swallowing issues. These challenges can be distressing for both caregivers and those they care for, highlighting the need for a compassionate approach that acknowledges the neurological basis of these changes.
To address these issues, caregivers can implement several practical strategies:
- Creating a structured mealtime routine
- Minimizing distractions
- Engaging the senses
These strategies can improve appetite and nutrition. For instance, offering smaller, more frequent meals and involving individuals in meal preparation can enhance the overall dining experience. By fostering a supportive and dementia-friendly environment, caregivers can help mitigate the negative impacts of cognitive decline on nutritional health.
The importance of understanding dementia and eating behaviors cannot be overstated. Caregivers play a crucial role in ensuring that individuals with cognitive decline receive the nourishment they need while maintaining their dignity and independence. Implementing these strategies not only improves nutritional outcomes but also enhances the quality of life for those affected by dementia. By prioritizing these approaches, caregivers can create a more compassionate and effective care experience for individuals facing the challenges of dementia and eating.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5MjI0ZjU4NGZjYWRhOTUwOGRlNDNjMSIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
How does dementia affect eating behaviors?
Dementia can significantly alter how individuals perceive and engage with food, leading to changes in taste and smell, diminished enjoyment of previously favored foods, and difficulties in recognizing hunger and thirst signals.
What are the consequences of cognitive decline on nutrition?
As cognitive impairments progress, individuals with dementia may forget to eat or lose track of mealtimes, resulting in irregular nutritional intake and potential malnutrition.
What is the neurological basis for eating difficulties in dementia patients?
The changes in eating behaviors associated with dementia stem from fundamental neurological alterations rather than just behavioral issues, affecting the individual's ability to recognize hunger and thirst.
What role do caregivers play in addressing eating challenges for individuals with dementia?
Caregivers need to recognize the eating challenges as integral to dementia and adapt their strategies, which may include establishing a structured mealtime routine and experimenting with flavors and textures to encourage better consumption.
How can caregivers support the nutritional needs of individuals with cognitive decline?
By understanding the neurological basis of eating changes, caregivers can provide empathetic and effective support, ensuring that the nutritional needs of individuals with dementia are met compassionately.
List of Sources
- Explore the Connection Between Dementia and Eating Behaviors
- Patient Information: Eating and Swallowing Problems in People With Advanced Dementia (https://jamanetwork.com/journals/jama/fullarticle/2835480)
- ADI - Nutrition and dementia (https://alzint.org/resource/nutrition-and-dementia)
- Changes in eating habits and food preference (https://alzheimers.org.uk/get-support/living-with-dementia/changes-eating-habits-food-preference)
- Prevalence of Malnutrition in People with Dementia in Long-Term Care: A Systematic Review and Meta-Analysis - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10343750)
- Caregiver Experiences with Dementia-Related Feeding/Eating Difficulties | MDPI (https://mdpi.com/2227-9032/12/2/133)
- Identify Common Eating Challenges in Dementia Care
- Six Nutrition Challenges Facing Alzheimer’s Patients (https://houston-homecare.com/alzheimers-care-six-nutrition-challenges-facing-alzheimers-patients)
- Patient Information: Eating and Swallowing Problems in People With Advanced Dementia (https://jamanetwork.com/journals/jama/fullarticle/2835480)
- Restoring Functional Eating in Late Stage Dementia – Massachusetts AI & Technology Center (https://massaitc.org/2025/04/02/restoring-functional-eating-in-late-stage-dementia)
- Dementia and appetite loss: Causes and management (https://medicalnewstoday.com/articles/dementia-patient-not-eating)
- Appetite and dementia (https://alzheimers.org.uk/get-support/living-with-dementia/poor-appetite-dementia)
- Create a Dementia-Friendly Mealtime Environment
- Hyllden Heights Launches Dementia-Friendly Dining Community Restaurant | Oakland Care Homes (https://oaklandcare.com/latest-news/hyllden-heights-launches-dementia-friendly-dining-community-restaurant)
- Hildenborough care home launches dementia-friendly restaurant (https://bbc.com/news/articles/cp8j023er11o)
- The Association of Eating Performance and Environmental Stimulation among Older Adults with Dementia in Nursing Homes: A Secondary Analysis - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC5495475)
- Dementia-friendly dining: This Brevard eatery staff trained to offer it. How does it work? (https://floridatoday.com/story/news/2025/07/06/viera-eatery-is-now-a-dementia-friendly-dining-spot-what-is-that/84453610007)
- Hollerbach’s German Restaurant joins Central Florida Dementia-Friendly Dining (https://orlandoweekly.com/food-drink/hollerbachs-german-restaurant-joins-central-florida-dementia-friendly-dining-37383118)
- Implement Strategies to Enhance Appetite and Nutrition
- Interventions to improve food intake for persons with dementia in nursing homes. A systematic review (https://sciencedirect.com/science/article/abs/pii/S0197457225005609)
- How to eat more in older age (https://medicalnewstoday.com/articles/treatment-for-loss-of-appetite-in-elderly)
- Appetite and dementia (https://alzheimers.org.uk/get-support/living-with-dementia/poor-appetite-dementia)
- Five strategies to add to your daily routine to fight dementia (https://news.fiu.edu/2025/five-strategies-to-incorporate-into-your-daily-routine-to-fight-dementia)
- Food & Eating | Alzheimer's Association (https://alz.org/help-support/caregiving/daily-care/food-eating)

