
For families in our service areas
For families in our service areas, this guide explains dementia care and how non-medical in-home caregiving can support care planning in East Idaho, Treasure Valley & Magic Valley, Northern Wasatch, North Central West Virginia, and Northeast Ohio.
What You Need to Know About Reasons Dementia Patients Aren
Appetite loss among dementia patients presents a significant challenge for caregivers, intertwined with complex cognitive, physical, and emotional issues. This problem not only affects the nutritional intake of these individuals but also impacts their overall well-being. Caregivers often find themselves navigating a difficult landscape of mealtime struggles, raising the question: how can they ensure their loved ones receive the nourishment they need?
Understanding the underlying causes of appetite loss is crucial. Factors such as cognitive decline, changes in taste and smell, and emotional distress can all contribute to this issue. By recognizing these challenges, caregivers can better address the needs of those they care for.
To tackle this problem effectively, caregivers can implement several actionable strategies. Here are some tips to foster a more supportive and engaging eating experience:
- Create a pleasant mealtime environment: Minimize distractions and enhance comfort to encourage eating.
- Offer smaller, frequent meals: This can make eating less overwhelming and more manageable.
- Incorporate favorite foods: Familiar tastes can stimulate appetite and make meals more enjoyable.
- Engage in social eating: Sharing meals with others can enhance the experience and encourage consumption.
By understanding the reasons behind appetite loss and applying these strategies, caregivers can significantly improve the eating experience for dementia patients, ultimately enhancing their nutritional intake and quality of life.
Explore Causes of Appetite Loss in Dementia Patients
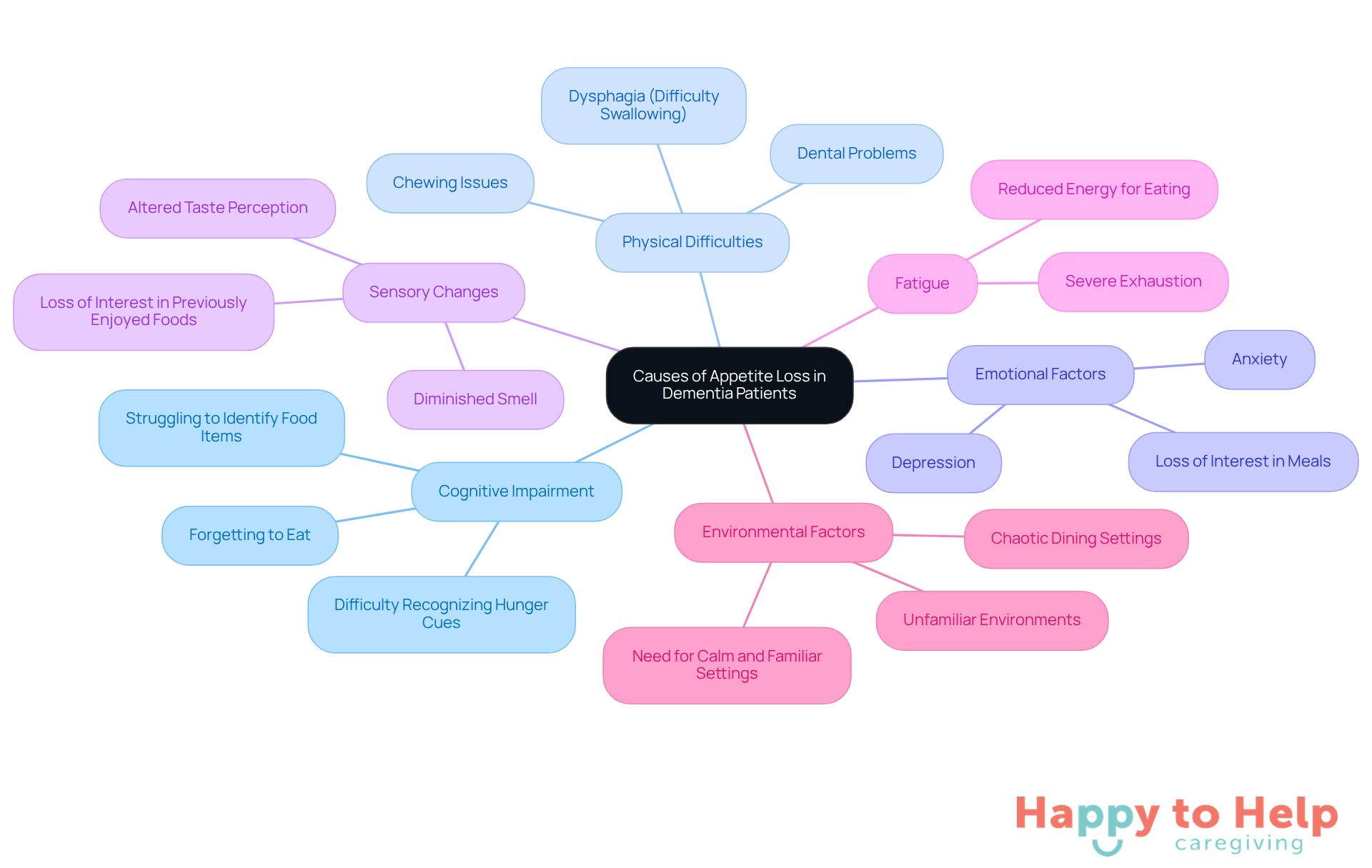
Appetite loss in dementia patients presents a significant challenge for caregivers, stemming from multiple interrelated causes:
-
Cognitive Impairment: Dementia disrupts the brain's ability to recognize hunger cues, leading to decreased interest in food. Patients may forget to eat or struggle to identify food items on their plates, resulting in missed meals. Research shows that up to 50% of individuals experience cognitive decline, leading to dementia patients not eating in care environments, which underscores the prevalence of this issue. As Heidi Moawad, M.D. notes, "Individuals dealing with cognitive decline may exhibit signs of appetite loss."
-
Physical Difficulties: Many individuals encounter challenges like dysphagia (difficulty swallowing) or chewing issues, often worsened by dental problems or ill-fitting dentures. These physical barriers can make eating uncomfortable or painful, discouraging adequate nutrition. Real-world examples illustrate how these difficulties significantly impact eating ability.
-
Emotional Factors: Depression and anxiety are common among dementia patients, affecting their appetite and interest in meals. Approximately 40% of individuals living with Alzheimer's disease may experience depression, which can result in dementia patients not eating and a notable decrease in nourishment consumption as they disengage from activities they once enjoyed, including mealtimes.
-
Sensory Changes: Dementia can alter taste and smell perceptions, diminishing meal appeal. Patients may lose interest in foods they previously loved, complicating their nutritional intake.
-
Fatigue: Severe exhaustion is prevalent among individuals with cognitive decline, reducing the energy available for eating. This fatigue can turn mealtimes from a pleasurable experience into a burdensome task.
-
Environmental Factors: Unfamiliar or chaotic dining settings can induce stress, prompting individuals to avoid meals altogether. A calm and familiar environment is crucial for encouraging eating.
Recognizing and understanding these causes is essential for caregivers aiming to effectively address appetite loss in dementia patients not eating who are experiencing cognitive decline. The occurrence of malnutrition in this group varies from 6.8% to 75.6%, highlighting the nutritional difficulties they face.
To combat these challenges, caregivers can:
- Create a structured meal schedule to help patients remember to eat.
- Offer meals in a calm, familiar environment to reduce stress.
- Adapt food textures to accommodate physical difficulties, ensuring meals are both appealing and manageable.
- Engage patients in meal preparation to rekindle interest in food.
- Monitor emotional well-being and seek professional support when needed.
By implementing these strategies, caregivers can help improve the nutritional intake and overall well-being of individuals with cognitive decline.
Identify Mealtime Challenges for Dementia Patients
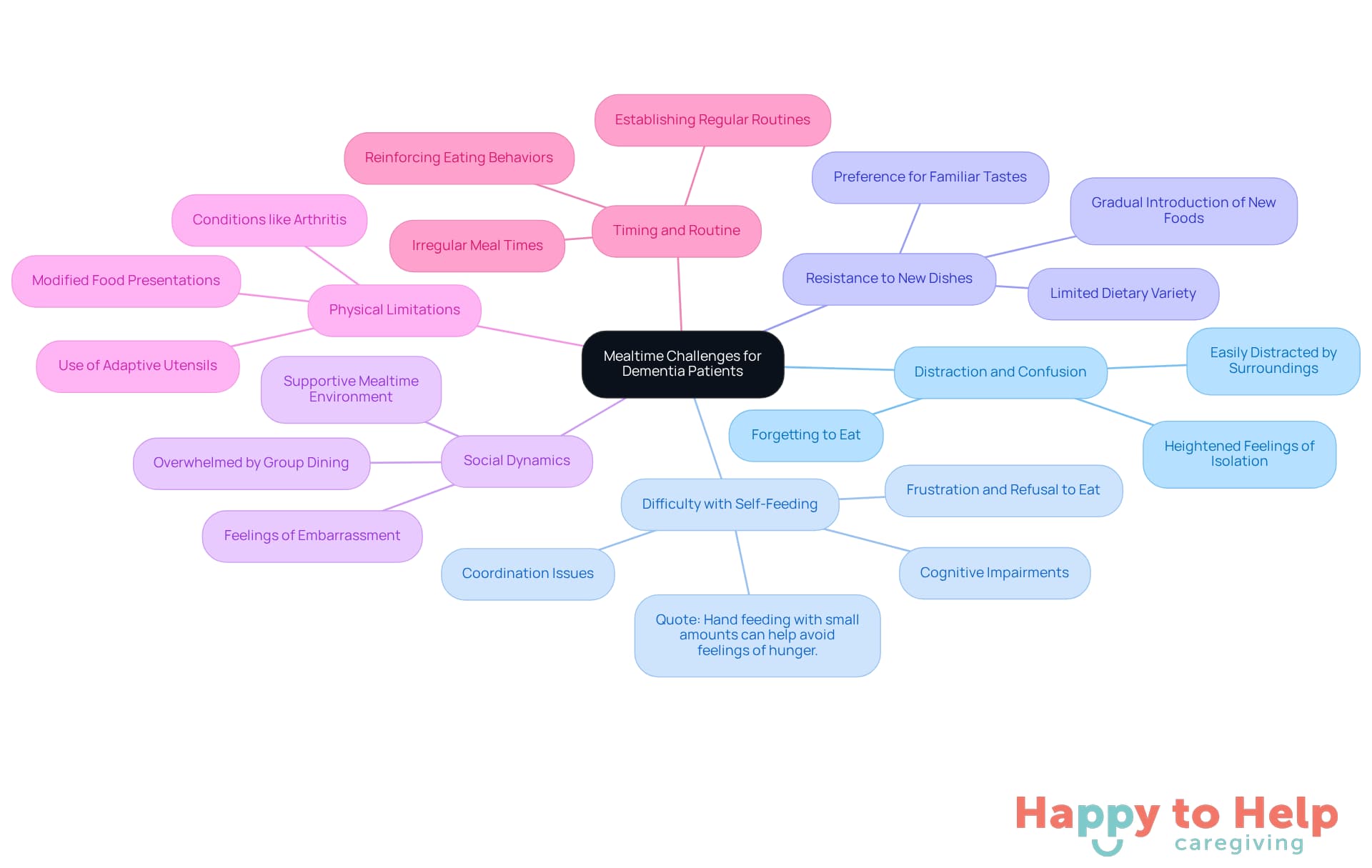
Mealtime can present significant challenges for dementia patients not eating, which impacts their nutritional intake and overall health. Here are some key issues:
- Distraction and Confusion: Patients often find themselves easily distracted by their surroundings, leading to confusion about the eating process. This distraction can result in forgetting to eat or losing interest in their meal, which may heighten feelings of isolation and anxiety during mealtimes.
- Difficulty with Self-Feeding: Many individuals with dementia struggle with the coordination required for self-feeding. This difficulty can lead to frustration and a refusal to eat, particularly in dementia patients not eating, complicating their nutritional needs. Occupational therapists note that these challenges often arise from cognitive impairments that hinder the ability to recognize hunger cues or effectively use utensils. Leah V. Estrada, PhD, RN, states, "hand feeding with small amounts of sustenance and fluids can help avoid feelings of hunger and thirst."
- Resistance to New Dishes: Introducing new foods can be particularly challenging, as patients typically prefer familiar tastes and textures. This resistance limits dietary variety and can lead to nutritional deficiencies. Caregivers should gradually incorporate new foods, perhaps by preparing several small dishes instead of three large ones, which can be beneficial for those with reduced appetites.
- Social Dynamics: Dining in a group can overwhelm some individuals, causing anxiety and food avoidance. Feelings of embarrassment about their eating difficulties can further complicate the situation for dementia patients not eating. It’s crucial for caregivers to foster a supportive and understanding mealtime environment.
- Physical Limitations: Conditions like arthritis can make it hard for individuals to hold utensils or manipulate food, leading to reluctance to eat. Caregivers should consider using adaptive utensils or modifying food presentations to facilitate easier self-feeding.
- Timing and Routine: Irregular meal times can disrupt eating habits, making it difficult for individuals to develop a consistent appetite. Establishing a regular mealtime routine can reinforce eating behaviors and improve overall nutrition.
A recent study revealed that 96.8 percent of caregivers reported feelings of sadness, helplessness, and social isolation related to their caregiving duties, underscoring the emotional toll of these challenges. By recognizing these difficulties, caregivers can implement strategies to better assist individuals with cognitive impairments during mealtimes, ensuring they receive the necessary nutrition while promoting a pleasant dining experience. For those seeking additional resources, a community event titled "Preparing for Mealtime Changes" is scheduled for June 27, 2024, which may offer valuable insights and support.
Implement Strategies to Encourage Eating
Eating difficulties among dementia patients not eating pose a significant challenge for caregivers. These individuals often struggle with appetite and mealtime engagement, which can lead to inadequate nutrition and overall well-being. Understanding the implications of these challenges is crucial for caregivers seeking to improve the eating experience for their loved ones.
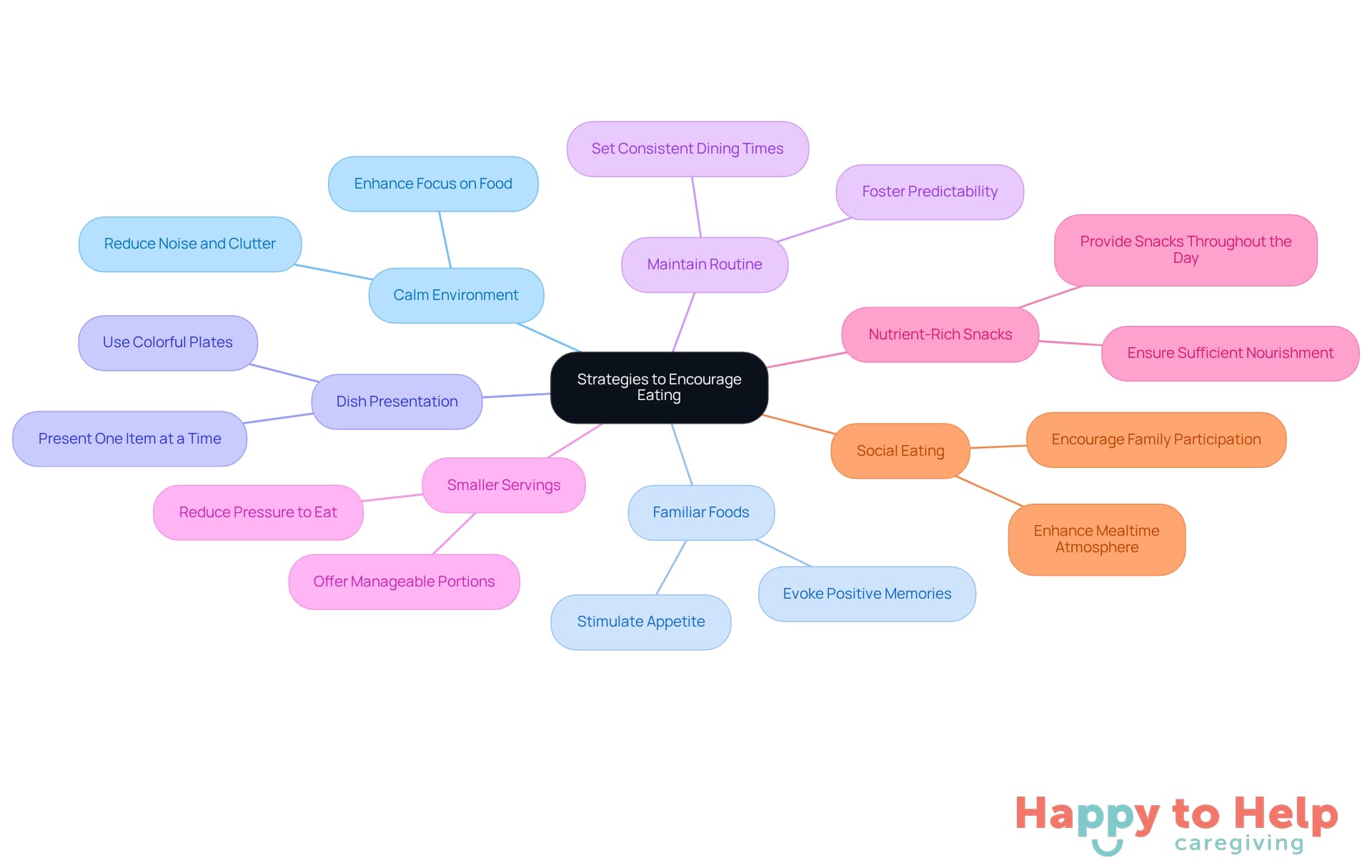
To address these issues, caregivers can implement several effective strategies:
- Create a Calm Environment: Reducing noise and clutter during mealtimes can significantly enhance focus on food. A tranquil environment allows individuals to concentrate better, enriching the pleasure of mealtimes. Research from dementia support forums indicates that minimizing distractions can lead to improved mealtime experiences.
- Use Familiar Foods: Serving meals that individuals recognize and enjoy can stimulate their appetite. Familiarity with cuisine not only promotes eating but also evokes positive memories, enhancing the overall mealtime experience. Diet experts suggest that utilizing well-known items can effectively encourage consumption among individuals with dementia.
- Adjust Dish Presentation: Using colorful plates and arranging items attractively can make dishes visually appealing. Presenting one food item at a time can prevent overwhelming the individual, making it easier for them to engage with their meal.
- Maintain a Routine: Setting consistent dining times fosters predictability, helping individuals anticipate food and form a schedule that encourages eating.
- Provide Smaller Servings: Offering smaller, manageable portions can alleviate the pressure of consuming a full dish, making the task feel less intimidating and motivating individuals to eat more.
- Include Nutrient-Rich Snacks: Providing nutritious snacks throughout the day ensures that individuals receive sufficient nourishment, even if they decline larger portions.
- Engage in Social Eating: Encouraging family members or caregivers to eat with the individual can enhance the mealtime experience. Social interaction during meals can stimulate appetite and create a more enjoyable atmosphere.
By applying these strategies, caregivers can effectively assist dementia patients not eating to overcome barriers, ultimately improving their nutritional intake and overall well-being. Insights from the case study "Strategies to Enhance Mealtime for Dementia Patients" further emphasize the importance of these approaches in creating a supportive mealtime environment.
Taking the Next Steps
Appetite loss in dementia patients presents a significant challenge that affects their nutritional health and overall quality of life. This multifaceted issue arises from various factors, including cognitive impairments, physical difficulties, and emotional influences. For caregivers, understanding these contributing elements is essential for providing effective support.
Cognitive decline can hinder the recognition of hunger cues, complicating mealtimes. Additionally, physical challenges such as dysphagia and fatigue further exacerbate the situation. Emotional factors, including anxiety and depression, also play a crucial role in diminishing appetite. Recognizing these underlying causes allows caregivers to implement targeted strategies that can make a difference.
To address these eating challenges, caregivers can:
- Create a calm dining environment
- Offer familiar foods
- Maintain a consistent meal routine
These practical solutions not only support physical health but also enhance emotional well-being. By adopting a compassionate and proactive approach, caregivers can transform mealtimes into positive experiences that foster connection and nourishment.
Ultimately, implementing these strategies can significantly improve the quality of life for individuals with dementia, making a meaningful impact on their daily experiences.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5MjY0MzVmM2U1ODU0NTE1NmI5MjVlMCIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What are the main causes of appetite loss in dementia patients?
The main causes of appetite loss in dementia patients include cognitive impairment, physical difficulties, emotional factors, sensory changes, fatigue, and environmental factors.
How does cognitive impairment affect appetite in dementia patients?
Cognitive impairment disrupts the brain's ability to recognize hunger cues, leading to decreased interest in food. Patients may forget to eat or struggle to identify food items, resulting in missed meals.
What physical difficulties can contribute to appetite loss in dementia patients?
Physical difficulties such as dysphagia (difficulty swallowing) and chewing issues, often worsened by dental problems or ill-fitting dentures, can make eating uncomfortable or painful, discouraging adequate nutrition.
How do emotional factors impact the appetite of dementia patients?
Depression and anxiety, common among dementia patients, can negatively affect appetite and interest in meals. Approximately 40% of individuals with Alzheimer's disease may experience depression, leading to reduced nourishment consumption.
What sensory changes occur in dementia patients that affect their appetite?
Dementia can alter taste and smell perceptions, diminishing the appeal of meals and causing patients to lose interest in foods they previously enjoyed.
How does fatigue influence eating habits in dementia patients?
Severe exhaustion is prevalent among individuals with cognitive decline, reducing the energy available for eating and making mealtimes feel burdensome rather than pleasurable.
What environmental factors can affect appetite in dementia patients?
Unfamiliar or chaotic dining settings can induce stress, prompting individuals to avoid meals. A calm and familiar environment is important for encouraging eating.
What is the prevalence of malnutrition in dementia patients?
The occurrence of malnutrition in dementia patients varies from 6.8% to 75.6%, highlighting the significant nutritional challenges they face.
What strategies can caregivers implement to help improve appetite in dementia patients?
Caregivers can create a structured meal schedule, offer meals in a calm environment, adapt food textures, engage patients in meal preparation, and monitor emotional well-being to improve nutritional intake.
List of Sources
- Explore Causes of Appetite Loss in Dementia Patients
- Why Do People with Dementia Stop Eating? Understanding the Causes - Happy To Help (https://happytohelpcaregiving.com/why-do-people-with-dementia-stop-eating-understanding-the-causes)
- Dementia and appetite loss: Causes and management (https://medicalnewstoday.com/articles/dementia-patient-not-eating)
- Appetite Loss in Memory Care: Warning Signs & Solutions (https://irisseniorliving.com/senior-living/tx/dallas/dickason-ave/blog/appetite-loss-in-memory-care-warning-signs-solutions)
- Prevalence of Malnutrition in People with Dementia in Long-Term Care: A Systematic Review and Meta-Analysis - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10343750)
- Identify Mealtime Challenges for Dementia Patients
- Researchers aim to ease mealtime challenges for dementia patients and caregivers (https://srs.healthsci.mcmaster.ca/researchers-aim-to-ease-mealtime-challenges-for-dementia-patients-and-caregivers)
- Food & Eating | Alzheimer's Association (https://alz.org/help-support/caregiving/daily-care/food-eating)
- Easing the Burden of Mealtime Caregiving (https://alzinfo.org/articles/caregiving/easing-the-burden-of-mealtime-caregiving)
- Helping caregivers help people with dementia eat at home (https://news.osu.edu/helping-caregivers-help-people-with-dementia-eat-at-home)
- Patient Information: Eating and Swallowing Problems in People With Advanced Dementia (https://jamanetwork.com/journals/jama/fullarticle/2835480)
- Implement Strategies to Encourage Eating
- Fostering the Enjoyment of Eating through Inclusive Strategies for People Living with Dementia | Global Brain Health Institute (https://gbhi.org/news-publications/fostering-enjoyment-eating-through-inclusive-strategies-people-living-dementia)
- Helping caregivers help people with dementia eat at home (https://news.osu.edu/helping-caregivers-help-people-with-dementia-eat-at-home)
- Tips for Caregivers: Helping People With Alzheimer’s Disease Eat Well (https://nia.nih.gov/health/alzheimers-caregiving/tips-caregivers-helping-people-alzheimers-disease-eat-well)
- How to Improve Mealtimes for Someone with Dementia - Whitsyms In-Home Care (https://whitsymsinhomecare.com/our-blog/how-to-improve-mealtimes-for-someone-with-dementia)
- Supporting someone with dementia to eat and drink (https://alzheimers.org.uk/get-support/living-with-dementia/improving-eating-experience-dementia)