
The Importance of Get a Dementia Patient to Eat
Dementia significantly alters the eating habits of those affected, creating unique challenges for caregivers striving to ensure proper nutrition. This problem is not just about food; it impacts the overall well-being of patients and complicates mealtime dynamics. Caregivers often find themselves navigating a complex landscape where maintaining a patient’s dignity and independence during meals is crucial.
Understanding these complexities is essential. It opens the door to effective strategies that can transform mealtime into a more comfortable and enjoyable experience. Caregivers must balance supporting a dementia patient’s nutritional needs with fostering a sense of autonomy. How can they achieve this? By implementing practical solutions that address both nutritional requirements and emotional well-being.
Understand Dementia's Impact on Eating Habits
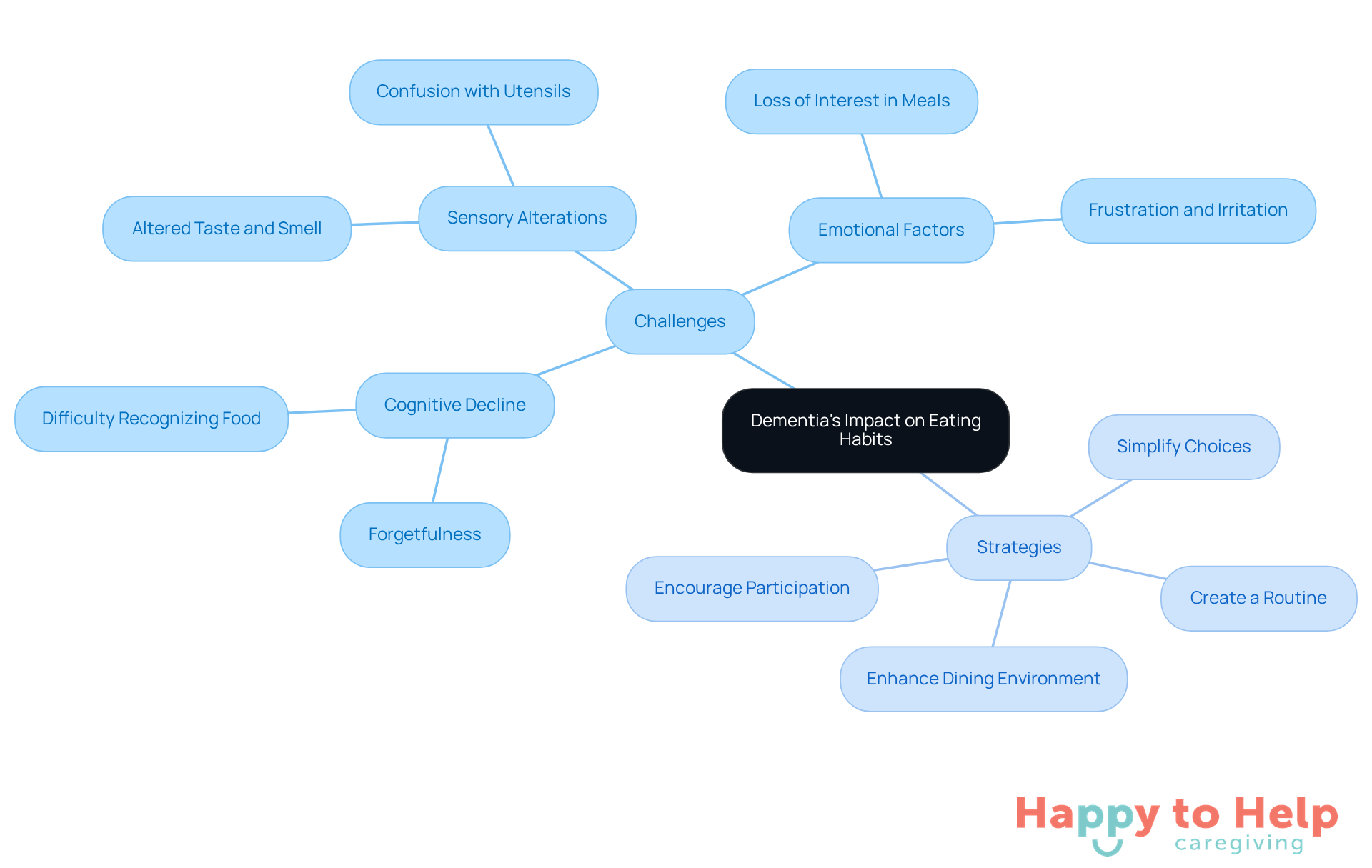
Dementia presents significant challenges for caregivers, especially in learning how to get a dementia patient to eat. Cognitive decline, sensory alterations, and emotional factors can complicate how to get a dementia patient to eat, as they may forget to eat, lose interest in meals, or struggle with the mechanics of eating.
These changes can be frustrating for both patients and caregivers. For instance, an individual with dementia may not recognize familiar food items or utensils, which can result in irritation and a refusal to eat, emphasizing the importance of knowing how to get a dementia patient to eat. Additionally, alterations in taste and smell can further complicate food preferences, making it essential for caregivers to observe and adapt to these shifts.
To effectively support individuals with dementia, caregivers can implement several strategies:
- Create a routine: Establish regular meal times to provide structure.
- Simplify choices: Offer a limited selection of foods to reduce overwhelm.
- Enhance the dining environment: Make mealtimes pleasant by minimizing distractions and creating a calm atmosphere.
- Encourage participation: Involve patients in meal preparation to stimulate interest.
Recognizing these challenges allows caregivers to approach mealtime with empathy and patience, ensuring they provide the necessary support for those in their care.
Create a Comfortable Eating Environment
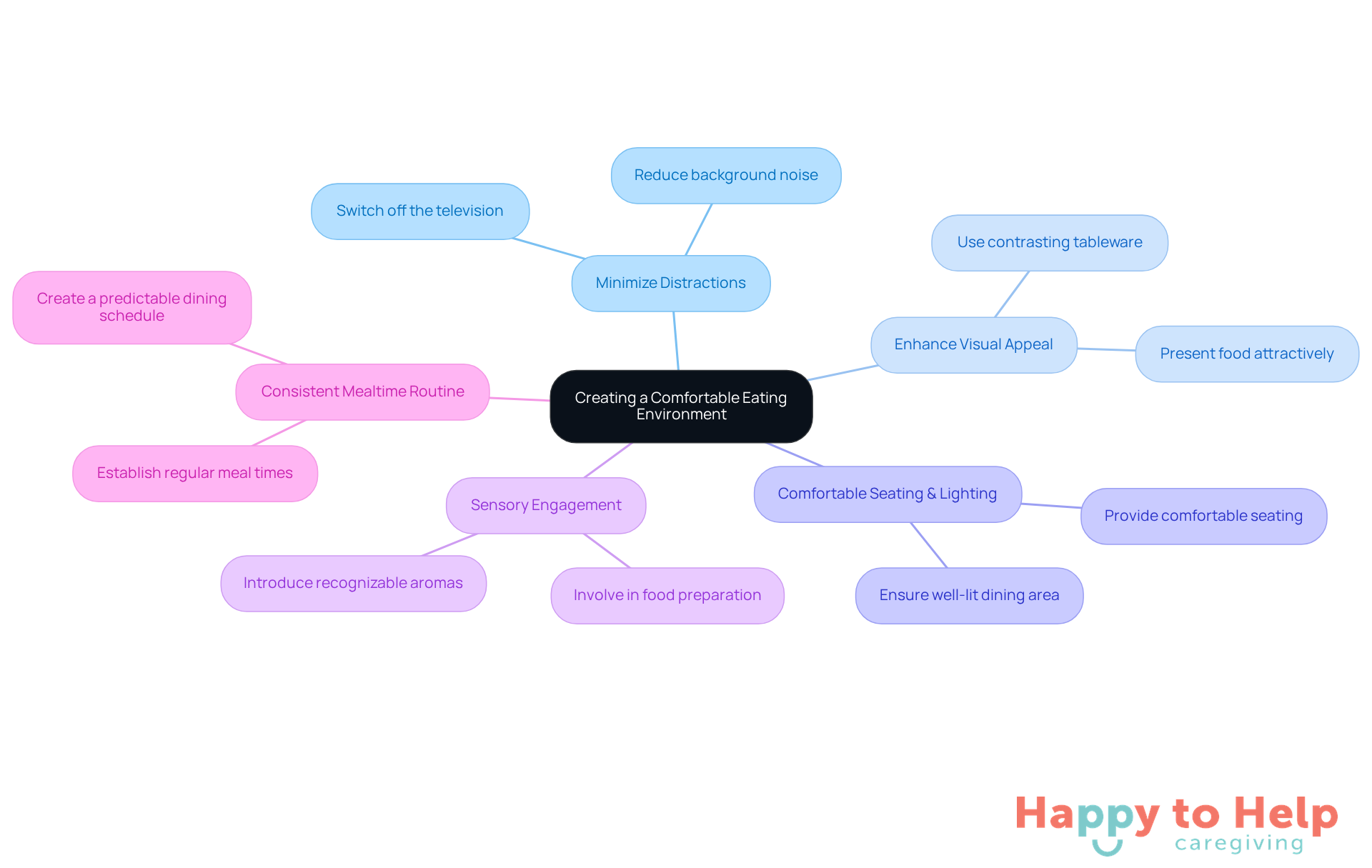
To learn how to get a dementia patient to eat, it is essential to create a comfortable dining environment by addressing a significant problem: distractions. Excessive noise can disrupt eating patterns, leading to reduced appetite and involvement during meals. Individuals with dementia may forget to eat or lose track of mealtimes, which raises the question of how to get a dementia patient to eat and ensure they have a regular nutritional intake.
To tackle this issue, caregivers should minimize distractions by:
- Switching off the television
- Reducing background noise
Research indicates that a serene environment significantly enhances dining performance, allowing individuals to focus on their nourishment. Additionally, using simple, contrasting tableware-like white plates on a dark tablecloth-can improve the visual appeal of food, making it easier for individuals to identify and enjoy their meals.
Comfortable seating and appropriate lighting are also essential. Ensure the dining area is well-lit but not harsh. Recognizable aromas can enhance appetite, so consider inviting the individual into the kitchen during food preparation to engage their senses. Occupational therapists emphasize that sensory engagement is crucial for those experiencing cognitive decline, particularly regarding dementia and nutrition.
Establishing a consistent mealtime routine is vital for learning how to get a dementia patient to eat. It provides structure and predictability, which can be particularly comforting for individuals with dementia. By implementing these strategies, caregivers can create a more enjoyable and effective dining experience for those they care for.
Implement Techniques to Enhance the Eating Experience
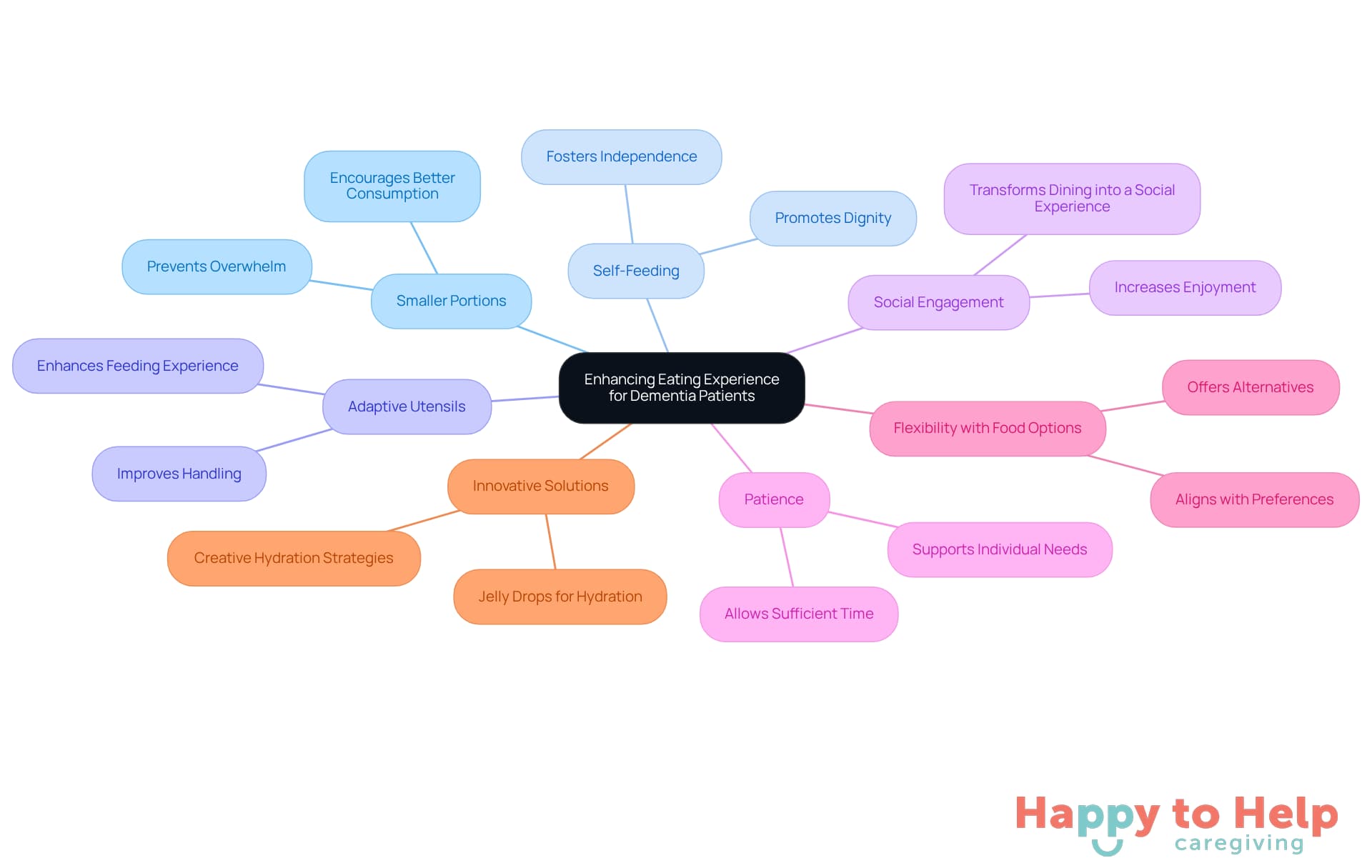
Caregivers face a significant challenge in how to get a dementia patient to eat, as large portions can often feel overwhelming, which impacts the dining experience for individuals with dementia. This can lead to decreased food consumption and negatively impact how to get a dementia patient to eat. Research shows that smaller, more frequent servings can help prevent these feelings and encourage better eating habits, which is crucial when considering how to get a dementia patient to eat.
Allowing patients to feed themselves is crucial for fostering independence and dignity. Adaptive utensils can significantly assist this process; studies indicate that their use improves the feeding experience for elderly individuals, making it easier for them to handle their food. Finger snacks are particularly advantageous, as they require less coordination and are simpler to manage, promoting a sense of independence during meals.
Engaging individuals in conversation can transform dining into a social experience, which is a useful strategy for understanding how to get a dementia patient to eat, as it increases enjoyment and improves food consumption. As noted by Iris Senior Living, "The caregiver should sit face-to-face with the senior, close enough to support their hand without pulling," emphasizing the importance of caregiver involvement during meals. Patience is essential when learning how to get a dementia patient to eat, as individuals with dementia may need more time to finish their food, so allowing sufficient time is vital.
It is also important to consider how to get a dementia patient to eat by providing flexibility with food options. If an individual declines a specific dish, offering alternatives that align with their preferences is an important aspect of learning how to get a dementia patient to eat more successfully. Caregivers have observed that using adaptive utensils not only facilitates feeding but also helps maintain a connection during meals, reinforcing the need for compassion and understanding in caregiving.
With a reported 79.66% prevalence of malnutrition among individuals experiencing cognitive decline, implementing these strategies is crucial. Innovative solutions like Jelly Drops can also enhance hydration and nutrition for individuals with dementia, further supporting their overall well-being.
Plan Nutrient-Dense Meals for Optimal Health
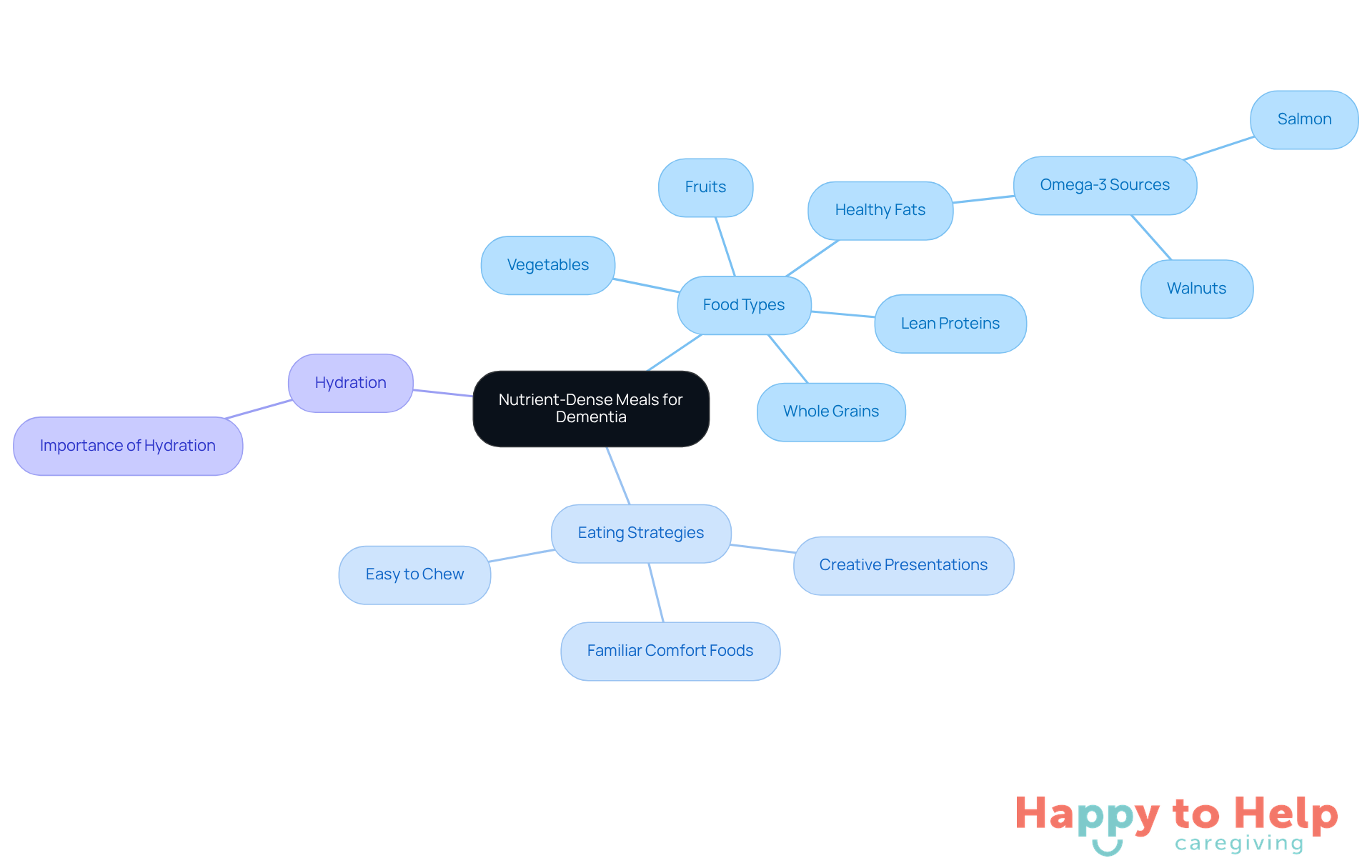
When caring for individuals with dementia, one significant challenge is knowing how to get a dementia patient to eat properly. Poor dietary choices can negatively impact brain health, leading to further cognitive decline. Therefore, it’s crucial to focus on nutrient-rich options that support brain function.
To address this issue, caregivers should incorporate a variety of fruits, vegetables, whole grains, lean proteins, and healthy fats into the diet. Foods rich in omega-3 fatty acids, such as salmon and walnuts, are particularly beneficial for brain health. Additionally, understanding how to get a dementia patient to eat by considering their preferences and past favorites can encourage them to eat more willingly.
If individuals resist conventional dishes, caregivers can consider how to get a dementia patient to eat by trying creative presentations or offering familiar comfort foods. It’s also essential to ensure that food is easy to chew and swallow, which is a crucial aspect of how to get a dementia patient to eat, as this can significantly affect their willingness to eat. Providing plenty of hydration throughout the day is equally important to maintain overall health.
Regularly assessing dietary intake and adjusting meal plans as needed will help ensure that individuals with dementia receive adequate nutrition. By implementing these strategies, caregivers can effectively support how to get a dementia patient to eat.
Your Path Forward
Supporting individuals with dementia during mealtimes presents significant challenges that can impact their nutritional health and overall well-being. Cognitive decline often alters eating habits, making it essential for caregivers to adapt meal environments and choices to meet these unique needs.
To address this issue, caregivers should:
- Establish routines
- Simplify food options
- Enhance the dining atmosphere
Minimizing distractions, promoting sensory engagement, and offering smaller, manageable portions can foster a sense of independence and dignity. Additionally, focusing on nutrient-dense meals that align with individual preferences can significantly improve willingness to eat.
Caring for someone with dementia requires patience and understanding. By implementing these strategies, caregivers can enhance not only the eating habits of dementia patients but also their quality of life. It’s crucial to remain adaptable and attentive, ensuring that mealtimes become a source of comfort and connection rather than a struggle.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5MjRmMWRmZWM0Y2FiOGU3NGVjMDBkYyIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What challenges do caregivers face when helping dementia patients eat?
Caregivers face challenges such as cognitive decline, sensory alterations, and emotional factors that can lead to patients forgetting to eat, losing interest in meals, or struggling with the mechanics of eating.
How can dementia affect a patient's eating habits?
Dementia can cause patients to forget familiar food items or utensils, lose interest in meals, and experience changes in taste and smell, complicating their food preferences.
What strategies can caregivers use to help dementia patients eat?
Caregivers can create a routine with regular meal times, simplify food choices, enhance the dining environment to minimize distractions, and encourage patient participation in meal preparation.
Why is it important for caregivers to recognize the challenges of feeding dementia patients?
Recognizing these challenges allows caregivers to approach mealtime with empathy and patience, ensuring they provide the necessary support for the individuals in their care.
List of Sources
- Understand Dementia's Impact on Eating Habits
- Prevalence of Malnutrition in People with Dementia in Long-Term Care: A Systematic Review and Meta-Analysis - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10343750)
- ADI - Nutrition and dementia (https://alzint.org/resource/nutrition-and-dementia)
- Caregiver Dementia Quotes (Encouragement For Dementia Caregivers) (https://optoceutics.com/caregiver-dementia-quotes-encouragement-dementia-caregivers?srsltid=AfmBOopJr33GFPo5y\_FEvx3kdoPC4q4zpDIf7CK5j6255V7\_3LXWugZh)
- Appetite and dementia (https://alzheimers.org.uk/get-support/living-with-dementia/poor-appetite-dementia)
- Eating Behaviors and Dietary Changes in Patients With Dementia - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10852764)
- Create a Comfortable Eating Environment
- Supporting someone with dementia to eat and drink (https://alzheimers.org.uk/get-support/living-with-dementia/improving-eating-experience-dementia)
- Understanding Dementia and Eating: Strategies for Caregivers - Happy To Help (https://happytohelpcaregiving.com/understanding-dementia-and-eating-strategies-for-caregivers)
- Fostering the Enjoyment of Eating through Inclusive Strategies for People Living with Dementia | Global Brain Health Institute (https://gbhi.org/news-publications/fostering-enjoyment-eating-through-inclusive-strategies-people-living-dementia)
- Food & Eating | Alzheimer's Association (https://alz.org/help-support/caregiving/daily-care/food-eating)
- Tips for Caregivers: Helping People With Alzheimer’s Disease Eat Well (https://nia.nih.gov/health/alzheimers-caregiving/tips-caregivers-helping-people-alzheimers-disease-eat-well)
- Implement Techniques to Enhance the Eating Experience
- Supporting someone with dementia to eat and drink (https://alzheimers.org.uk/get-support/living-with-dementia/improving-eating-experience-dementia)
- Natural Touch Therapy for Senior Comfort (https://irisseniorliving.com/senior-living/ok/oklahoma-city/n-macarthur-blvd/blog/natural-touch-therapy-for-senior-comfort?article=6-ways-to-improve-a-dementia-patient-s-eating-habits)
- Dining Well With Dementia: This Is A Lot To Swallow! -Article 5772 (https://occupationaltherapy.com/articles/dining-well-with-dementia-this-5772)
- Why Do People with Dementia Stop Eating? Understanding the Causes - Happy To Help (https://happytohelpcaregiving.com/why-do-people-with-dementia-stop-eating-understanding-the-causes)
- (https://belleviecare.co.uk/support-advice/dementia-quotes-to-lift-your-spirits)
- Plan Nutrient-Dense Meals for Optimal Health
- A well-balanced diet boosts your brain health | HonorHealth (https://honorhealth.com/healthy-living/a-well-balanced-diet-boosts-your-brain-health)
- New UH study: It’s never too late to eat smarter to help your brain avoid dementia (https://uhcancercenter.org/about-us/newsroom/1123-new-uh-study-it-s-never-too-late-to-eat-smarter-to-help-your-brain-avoid-dementia)
- Foods linked to better brainpower - Harvard Health (https://health.harvard.edu/healthbeat/foods-linked-to-better-brainpower)
- Dietary Patterns and Brain Health in Middle-Aged and Older Adults: A Narrative Review (https://mdpi.com/2072-6643/17/9/1436)
- If you want to protect your brain, this diet beats the Mediterranean diet, new study suggests (https://nbcnews.com/health/aging/mind-diet-mediterranean-dash-dementia-study-rcna209573)

