
The Importance of Dementia and Not Eating or Drinking:
Dementia profoundly affects cognitive function and the essential act of eating, creating numerous challenges for both patients and caregivers. Over 80% of individuals experiencing cognitive decline face issues such as loss of appetite and swallowing difficulties. This makes it crucial to understand the complex relationship between dementia and eating behaviors.
Caregivers often struggle with mealtime complexities, which can jeopardize the nutritional well-being of their loved ones. How can they effectively navigate these challenges? This article explores key insights and practical strategies that empower caregivers to enhance the dining experience for individuals with dementia, addressing both emotional and practical aspects of nutrition and hydration.
Explore the Connection Between Dementia and Eating Behaviors
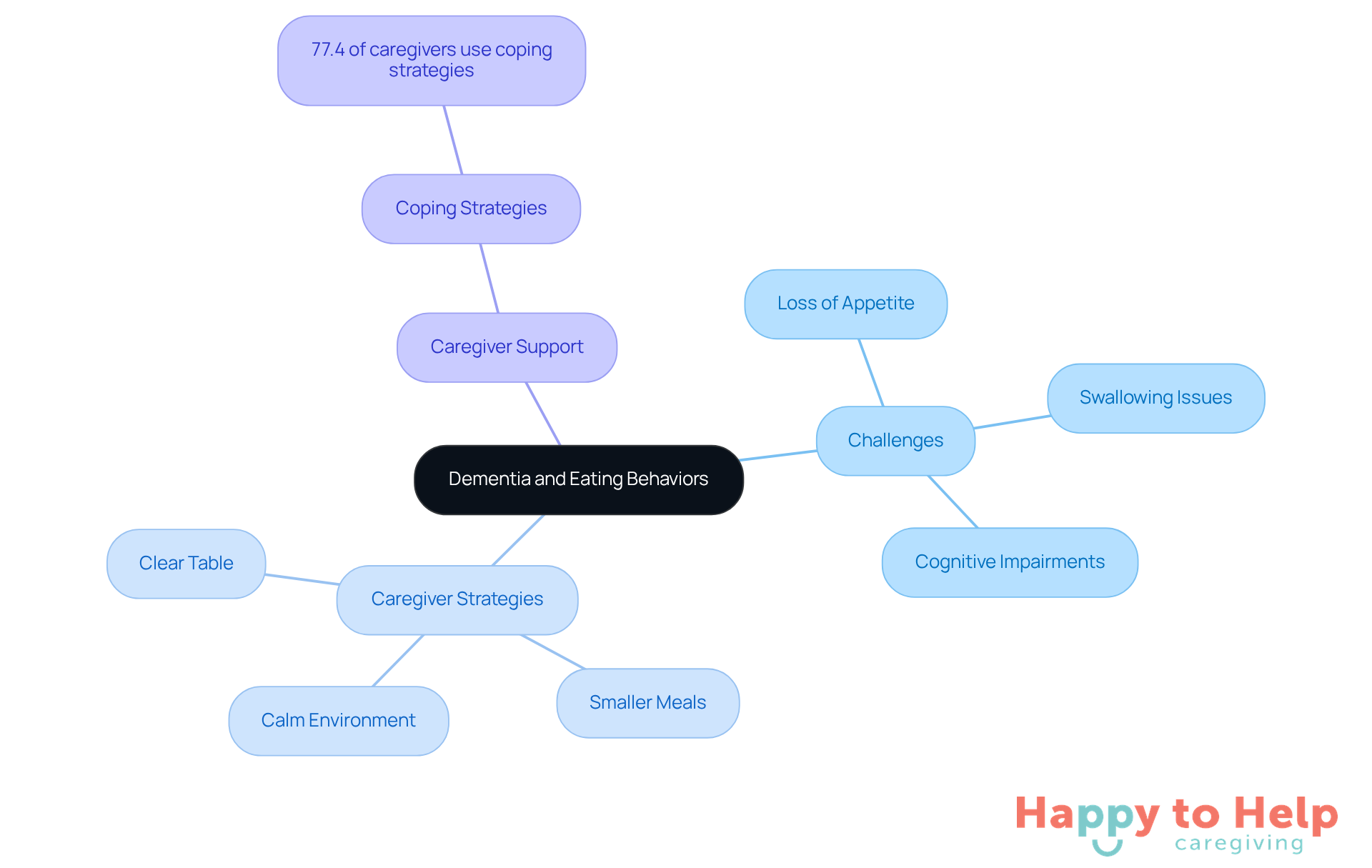
Dementia significantly alters how individuals perceive and interact with meals. Difficulties in recognizing food, understanding mealtime routines, and even remembering to eat can arise from cognitive impairments, particularly in cases of dementia and not eating or drinking. Research indicates that over 80% of individuals with cognitive impairment, particularly those experiencing dementia and not eating or drinking, face various eating challenges, including loss of appetite and swallowing issues.
These changes are not merely behavioral; they stem from the neurological impacts of dementia, which can diminish the senses of taste and smell, complicating the eating experience. Caregivers must recognize this connection to approach mealtimes with empathy and tailored strategies that address the unique needs of their loved ones.
To enhance the mealtime experience, consider:
- Creating a familiar and calm dining environment.
- Offering smaller, more frequent meals to help manage appetite fluctuations.
- Ensuring that non-food items are cleared from the table to avoid confusion, allowing ample time for individuals to eat.
Understanding the complex relationship between cognitive decline, particularly dementia and not eating or drinking, enables caregivers to better assist their loved ones in maintaining nutritional well-being. Notably, 77.4% of caregivers reported using coping strategies to manage the challenges they encounter, underscoring the importance of support in their caregiving journey.
Identify Causes of Appetite Loss in Dementia Patients
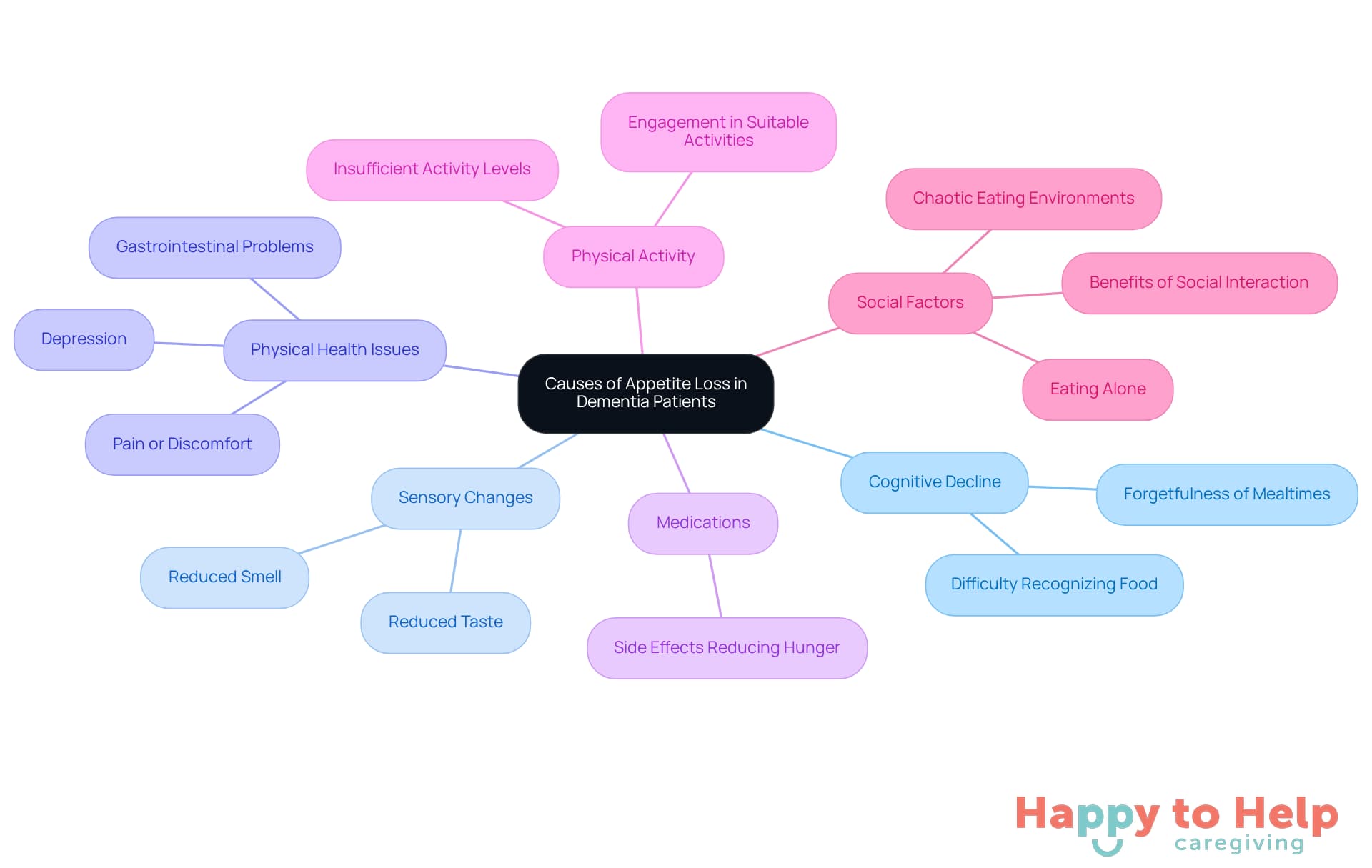
The decline in appetite among individuals with dementia and not eating or drinking presents a significant challenge for caregivers. This decline can stem from various interrelated physical, psychological, and environmental factors, making it crucial for caregivers to understand these causes to improve eating habits.
Cognitive Decline: As dementia progresses, patients may forget mealtimes or struggle to recognize food, leading to missed meals and reduced intake. This cognitive decline associated with dementia and not eating or drinking can severely impact nutritional health.
Sensory Changes: Reduced taste and smell, common in cognitive decline, can significantly decrease the appeal of food, making it less enticing. When food loses its allure, individuals may eat less.
Physical Health Issues: Conditions such as depression, pain, or gastrointestinal problems often accompany cognitive decline and can further suppress appetite. Research indicates that nearly 40-50% of individuals with cognitive decline, particularly those dealing with dementia and not eating or drinking, experience depression, which is closely linked to eating difficulties.
Medications: Certain medications prescribed for cognitive decline or related conditions may have side effects that diminish hunger, complicating nutritional intake. Caregivers should be aware of the potential effects related to dementia and not eating or drinking.
Physical Activity: Insufficient physical activity can lead to reduced appetite. Involving individuals with dementia in suitable physical activities may help enhance their appetite and overall well-being.
Social Factors: Eating alone or in a chaotic environment can discourage individuals from eating. Studies show that residents tend to consume more when sharing meals with companions, highlighting the importance of social interaction during mealtimes.
By acknowledging these factors, caregivers can create customized approaches to promote improved eating habits. Here are some actionable solutions:
- Establish a peaceful dining atmosphere.
- Engage patients in meal preparation.
- Present options that cater to their evolving tastes.
- Make food visually appealing through colors, tastes, and smells to stimulate appetite.
Furthermore, caregivers should consult a doctor for any underlying medical conditions affecting appetite. This proactive approach can help mitigate the impact of cognitive decline on nutrition and overall well-being.
Implement Strategies to Encourage Eating and Hydration
Caregivers face significant challenges in encouraging eating and hydration among patients dealing with dementia and not eating or drinking. Studies indicate that 74%-78% of individuals experiencing dementia and not eating or drinking struggle during mealtime, leading to disorientation and stress. Additionally, 94% of dementia patients face risks related to malnutrition, especially in situations of dementia and not eating or drinking, underscoring the urgency of addressing these issues.
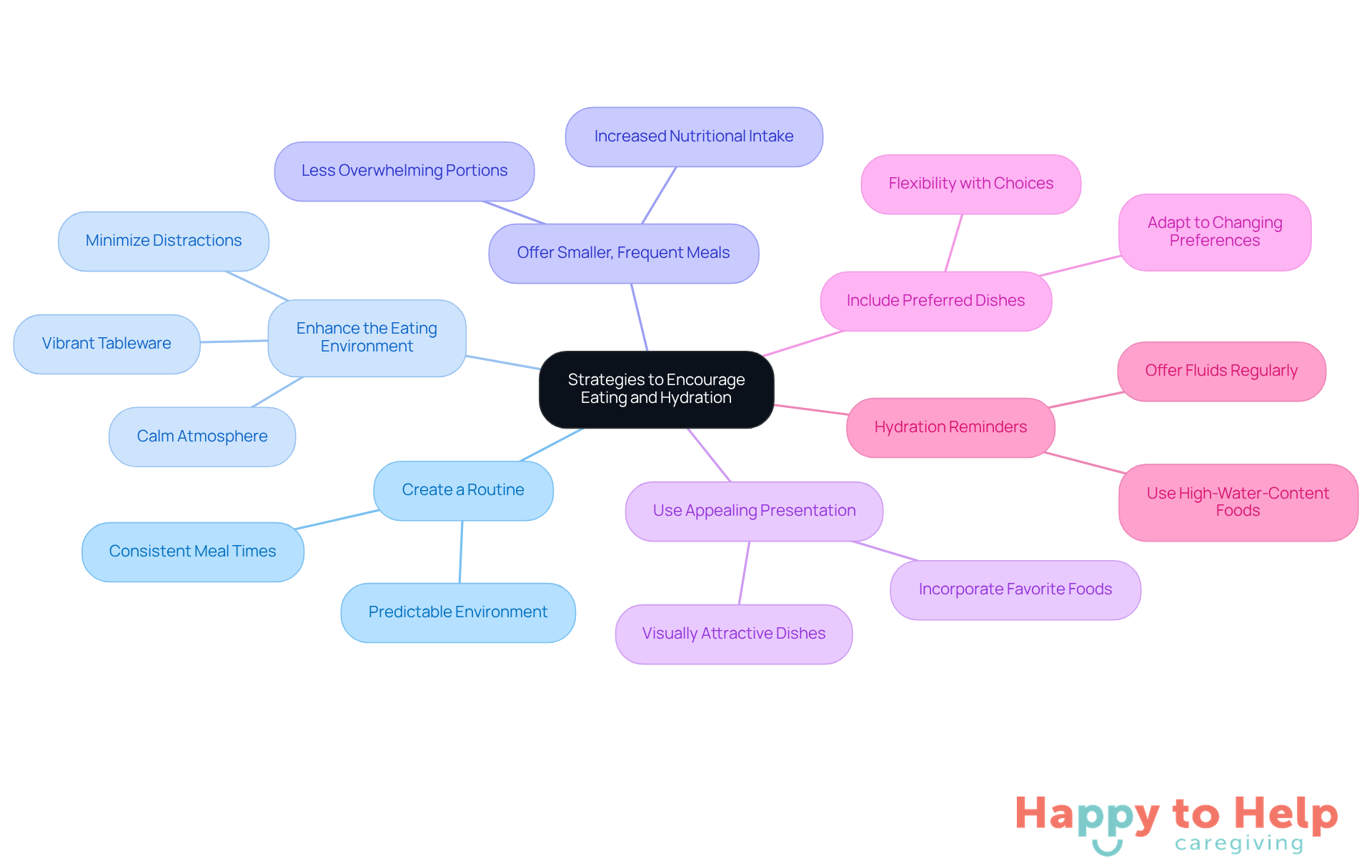
To tackle these problems, caregivers can adopt several effective strategies:
- Create a Routine: Establishing consistent meal and snack times provides the necessary structure for individuals with dementia. A routine can help diminish confusion and promote better focus on meals.
- Enhance the Eating Environment: A calm, inviting atmosphere is essential. High-quality dining settings are linked to increased meal intake. Caregivers should consider using vibrant plates and bowls to help differentiate food items, which can significantly boost intake. As noted by Wen Liu, combining resident training with environmental modifications can further improve mealtime experiences.
- Offer Smaller, Frequent Meals: Smaller portions can be less overwhelming for dementia patients. This approach not only ensures adequate nutrition but also addresses the challenges of dementia and not eating or drinking, thereby reducing mealtime stress.
- Use Appealing Presentation: Visually attractive dishes can stimulate interest. Including favorite dishes that evoke positive memories can enhance both nutritional intake and emotional well-being.
- Include Preferred Dishes: Allowing patients to choose items they enjoy increases their willingness to eat. Caregivers should remain flexible with dietary preferences, as likes and dislikes may change unexpectedly.
- Hydration Reminders: Regularly offering fluids throughout the day is vital. Encouraging hydration can be achieved by providing small cups of water or high-water-content foods like fruits and soups. Flavored options can also enhance appeal and encourage intake.
By implementing these strategies, caregivers can significantly improve the dining experience and nutritional intake for individuals with cognitive impairments, ultimately enhancing their quality of life.
Navigate Ethical Decisions Regarding Nutrition and Hydration
Caregivers often face significant ethical dilemmas concerning nutrition and hydration for individuals with dementia and not eating or drinking, especially in the advanced stages. This situation poses a complex problem that requires careful consideration of various factors.
One major concern is patient autonomy. It's crucial to respect the wishes of the patient, including any advance directives they may have regarding food and hydration. This respect for autonomy can sometimes conflict with the caregiver's instinct to provide care, leading to distressing decisions.
Another important aspect is quality of life. Caregivers must balance the benefits of nutrition and hydration against the potential discomfort or distress that may occur in cases of dementia and not eating or drinking. This balancing act can be emotionally taxing, as caregivers strive to ensure the best possible quality of life for their loved ones.
To navigate these challenges, informed decision-making is essential. Engaging in discussions with healthcare providers and family members can help ensure that decisions align with the patient's values and preferences. This collaborative approach fosters a supportive environment where all voices are heard.
Additionally, caregivers should familiarize themselves with legal and ethical guidelines regarding end-of-life care. Understanding local laws and ethical standards can provide a framework for making compassionate choices that honor the patient's dignity and wishes.
By addressing these key considerations, caregivers can better manage the ethical dilemmas they face, ensuring that their decisions are both compassionate and aligned with the needs of those they care for.
Taking the Next Steps
Understanding the complexities of dementia and its impact on eating and drinking presents a significant challenge for caregivers. Cognitive impairments associated with dementia can severely hinder an individual's ability to recognize food, remember mealtimes, and maintain a healthy appetite. This not only affects nutritional intake but also the overall quality of life for those living with dementia.
Caregivers face the problem of appetite loss, which can stem from various factors, including cognitive decline, sensory changes, and social influences. To address these challenges, it's crucial for caregivers to:
- Create a peaceful dining environment
- Establish consistent routines
- Offer visually appealing and familiar foods to stimulate appetite
Moreover, understanding the ethical considerations surrounding nutrition and hydration is essential. Caregivers must respect patient autonomy while striving to enhance their quality of life. By fostering open communication with healthcare professionals and implementing tailored strategies, caregivers can navigate the complexities of dementia care more effectively.
Ultimately, addressing these challenges is vital. A proactive approach not only enhances nutritional intake but also uplifts the emotional well-being of individuals living with dementia. Compassionate caregiving plays a crucial role in this journey, affirming the importance of support and understanding in the lives of those affected.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5MjRmMWUwZWM0Y2FiOGU3NGVjMDBkZiIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
How does dementia affect eating behaviors?
Dementia significantly alters how individuals perceive and interact with meals, leading to difficulties in recognizing food, understanding mealtime routines, and remembering to eat.
What percentage of individuals with cognitive impairment face eating challenges?
Research indicates that over 80% of individuals with cognitive impairment, particularly those with dementia, experience various eating challenges, including loss of appetite and swallowing issues.
What neurological impacts of dementia affect eating?
Dementia can diminish the senses of taste and smell, complicating the eating experience for affected individuals.
What strategies can caregivers use to improve mealtime experiences for individuals with dementia?
Caregivers can enhance mealtime experiences by creating a familiar and calm dining environment, offering smaller and more frequent meals, and ensuring non-food items are cleared from the table to avoid confusion.
Why is it important for caregivers to understand the relationship between cognitive decline and eating behaviors?
Understanding this relationship enables caregivers to better assist their loved ones in maintaining nutritional well-being and to approach mealtimes with empathy and tailored strategies.
What percentage of caregivers report using coping strategies to manage eating challenges?
Notably, 77.4% of caregivers reported using coping strategies to manage the challenges they encounter in relation to eating behaviors.
List of Sources
- Explore the Connection Between Dementia and Eating Behaviors
- Changes in eating habits and food preference (https://alzheimers.org.uk/get-support/living-with-dementia/changes-eating-habits-food-preference)
- Understanding Dementia and Eating: Strategies for Caregivers - Happy To Help (https://happytohelpcaregiving.com/understanding-dementia-and-eating-strategies-for-caregivers)
- Caregiver Experiences with Dementia-Related Feeding/Eating Difficulties - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10815734)
- Food & Eating | Alzheimer's Association (https://alz.org/help-support/caregiving/daily-care/food-eating)
- Identify Causes of Appetite Loss in Dementia Patients
- Appetite Loss in Memory Care: Warning Signs & Solutions (https://irisseniorliving.com/senior-living/tx/dallas/dickason-ave/blog/appetite-loss-in-memory-care-warning-signs-solutions)
- Dementia and Appetite: Is Your Loved One with Dementia Not Eating? (https://lidementia.org/dementia-and-appetite)
- Dementia and appetite loss: Causes and management (https://medicalnewstoday.com/articles/dementia-patient-not-eating)
- Dementia severity and weight loss: A comparison across eight cohorts. The 10/66 study - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC3898277)
- (https://belleviecare.co.uk/support-advice/dementia-quotes-to-lift-your-spirits)
- Implement Strategies to Encourage Eating and Hydration
- Optimizing mealtime care and outcomes for people with dementia and their caregivers: A systematic review and meta‐analysis of intervention studies - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC11922811)
- Optimizing mealtime care and outcomes for people with dementia and their caregivers: A systematic review and meta‐analysis of intervention studies (https://alz-journals.onlinelibrary.wiley.com/doi/full/10.1002/alz.14522)
- Food & Eating | Alzheimer's Association (https://alz.org/help-support/caregiving/daily-care/food-eating)
- Innovative treats help people living with dementia – DW – 10/05/2024 (https://dw.com/en/jelly-drops-innovative-treats-help-people-living-with-dementia-stay-hydrated/video-70407159)
- 9 Strategies for Helping Dementia Patients Refusing to Eat - Happy To Help (https://happytohelpcaregiving.com/9-strategies-for-helping-dementia-patients-refusing-to-eat)

