
For families in our service areas
For families in our service areas, this guide explains dementia care and how non-medical in-home caregiving can support care planning in East Idaho, Treasure Valley & Magic Valley, Northern Wasatch, North Central West Virginia, and Northeast Ohio.
Understanding Vascular Dementia and Eating Problems:
Understanding the complexities of vascular dementia is essential for caregivers facing significant challenges, especially when it comes to managing eating problems. This condition, marked by cognitive decline due to reduced blood flow to the brain, can severely impact an individual's appetite and nutritional intake. Caregivers often find themselves in a frustrating paradox: they must encourage healthy eating while dealing with their loved ones' diminished interest in food and potential swallowing difficulties.
These eating challenges can lead to serious health implications, including malnutrition and weight loss, which further complicate the caregiving experience. As caregivers strive to ensure the well-being of their loved ones, they may feel overwhelmed and uncertain about how to effectively address these issues. So, how can caregivers tackle these eating challenges while also taking care of their own well-being?
Practical Solutions for Caregivers:
- Create a Routine: Establish regular meal times to help stimulate appetite.
- Enhance Food Appeal: Use colorful plates and present food attractively to make meals more inviting.
- Offer Small, Frequent Meals: Instead of three large meals, provide smaller portions throughout the day to make eating less daunting.
- Focus on Nutrient-Dense Foods: Prioritize foods that are high in nutrients but low in volume, such as smoothies or soups.
- Encourage Hydration: Ensure that your loved one stays hydrated, as dehydration can also affect appetite.
By implementing these strategies, caregivers can better navigate the complexities of eating problems associated with vascular dementia, ultimately supporting both their loved ones and themselves.
Define Vascular Dementia: Causes and Symptoms
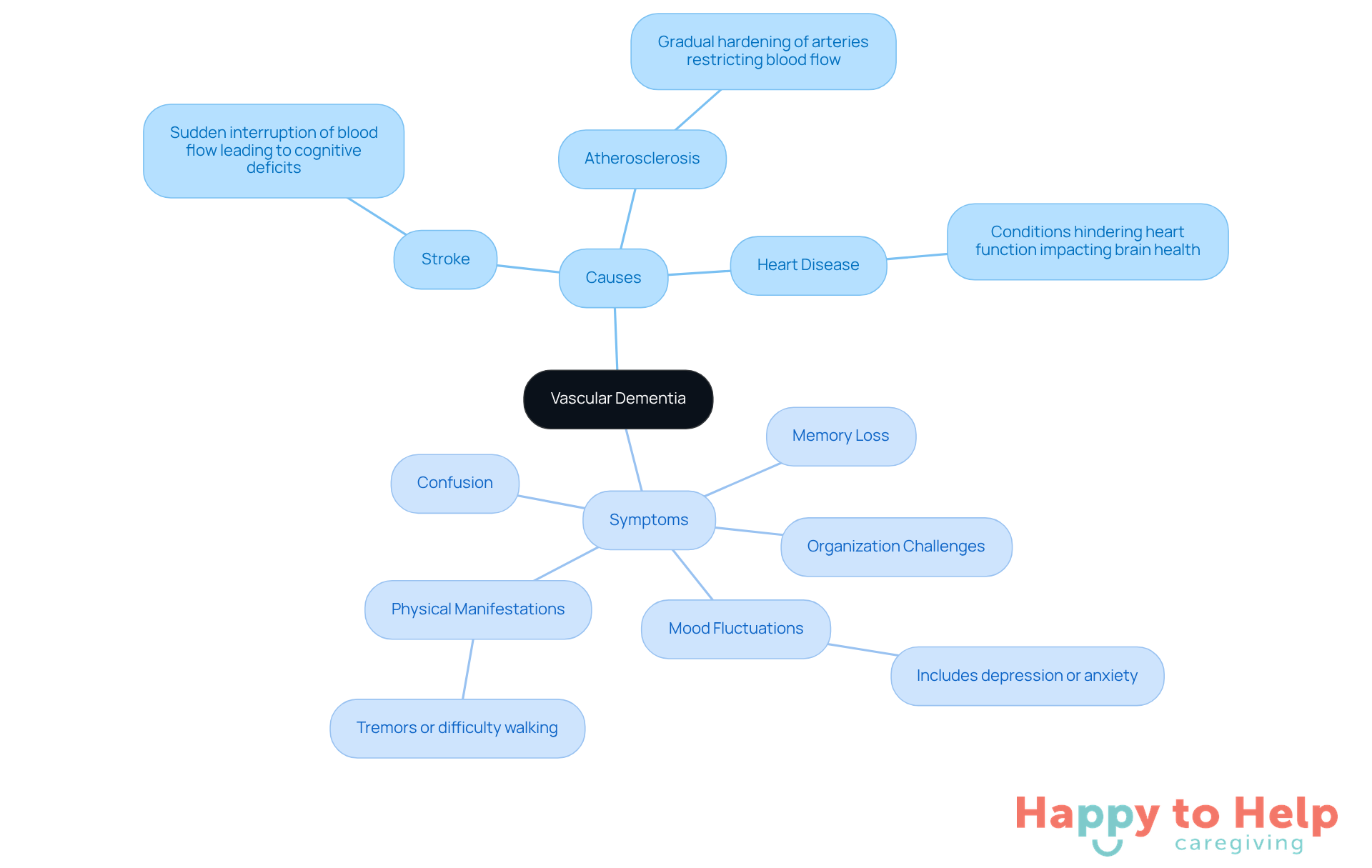
Vascular dementia (VaD) represents a significant challenge, as it involves a decline in mental abilities due to reduced blood flow to the brain, often stemming from strokes or other vascular issues. Caregivers face the daunting task of recognizing and managing this condition, which can severely impact the quality of life for those affected.
Key Causes of Vascular Dementia:
- Stroke: A sudden interruption of blood flow can lead to immediate cognitive deficits, significantly affecting memory and decision-making.
- Atherosclerosis: The gradual hardening of arteries restricts blood flow over time, contributing to mental decline as the brain receives insufficient oxygen and nutrients.
- Heart Disease: Conditions that hinder heart function can negatively impact brain health, increasing the risk of cognitive decline.
Symptoms of Vascular Dementia:
Symptoms can vary widely but typically include:
- Confusion and difficulty concentrating
- Challenges with organization and planning
- Memory loss
- Mood fluctuations, including depression or anxiety
- Physical manifestations such as tremors or difficulty walking
Recognizing these symptoms early is crucial for caregivers. Timely intervention can lead to better management of the condition. Recent studies indicate that factors like heart disease and stroke significantly heighten the risk of developing vascular cognitive impairment. This underscores the importance of monitoring cardiovascular health to protect cognitive function.
Neurologists stress that understanding these symptoms empowers caregivers to seek appropriate support and interventions, ultimately enhancing the quality of life for those affected. Furthermore, a recent study from Finland suggests that low labor market participation for non-retirement related reasons may indicate early signs of cognitive decline, potentially occurring up to 10 years before diagnosis.
Additionally, a global group led by Professor Perminder Sachdev and Dr. Adam Bentvelzen has introduced new diagnostic standards for blood vessel-related mental decline. These standards can aid in identifying and managing the condition more effectively.
Identify Eating Problems in Vascular Dementia
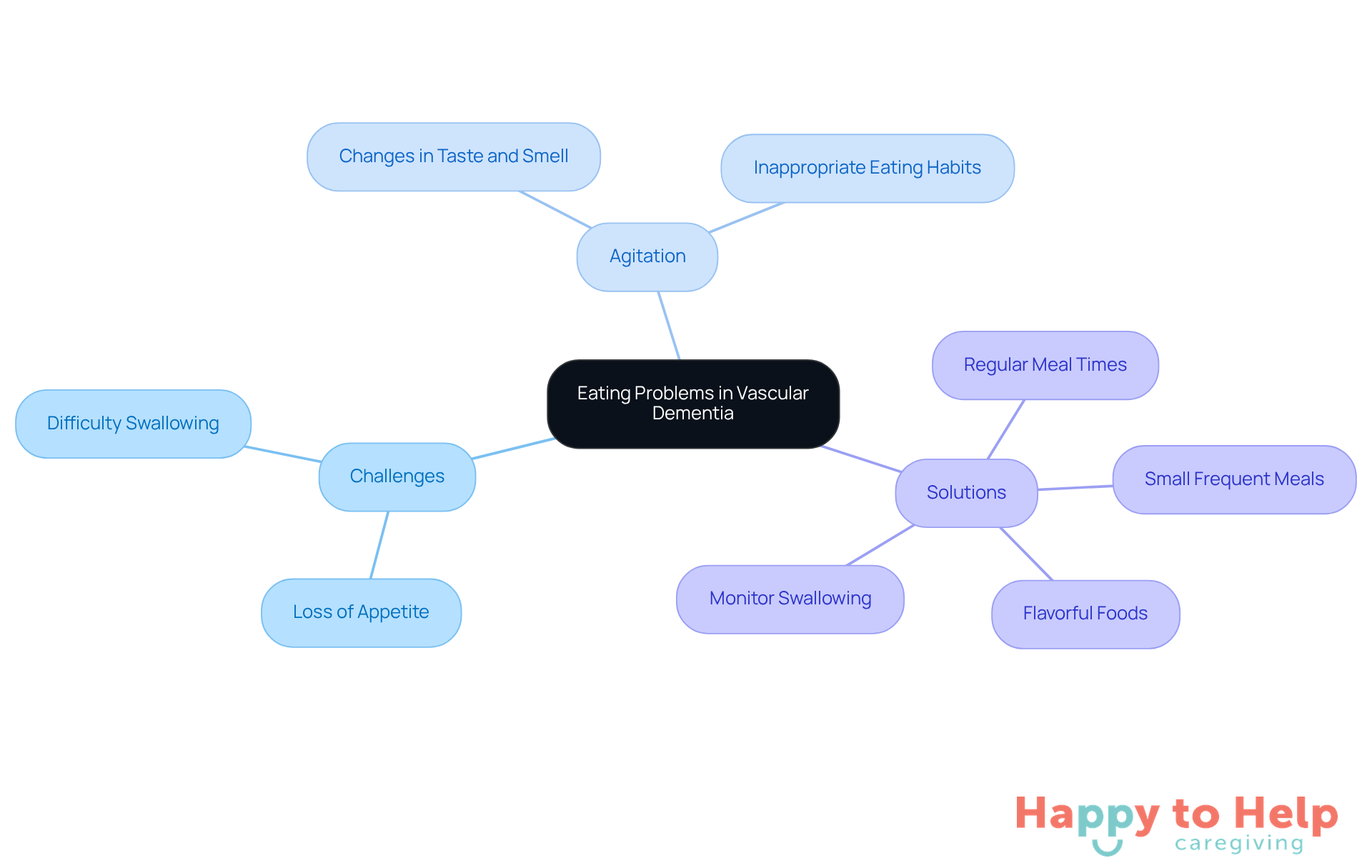
Individuals with vascular dementia and eating problems face several challenges that can significantly impact their health and well-being.
Problem: Many individuals may experience a loss of appetite, forgetting to eat or losing interest in food altogether. This can lead to inadequate nutrition and weight loss. Additionally, difficulty swallowing (dysphagia) poses serious risks, including choking hazards, which require vigilant monitoring.
Agitate: Changes in taste and smell can further complicate matters, making food seem bland and unappealing, which decreases food intake. Moreover, some individuals with vascular dementia and eating problems may develop inappropriate eating habits, such as eating too quickly or taking food from others' plates, which can create social and safety concerns during mealtimes.
Solution: Caregivers should closely observe these behaviors to adapt meal plans effectively. Here are some actionable tips:
- Encourage regular meal times to establish a routine.
- Offer small, frequent meals instead of large ones to make eating less overwhelming.
- Introduce flavorful foods to stimulate appetite and make meals more enjoyable.
- Monitor swallowing closely and consult a healthcare professional for guidance on safe eating practices.
By implementing these strategies, caregivers can help ensure safety and promote better eating habits for individuals dealing with vascular dementia and eating problems.
Implement Strategies to Encourage Healthy Eating
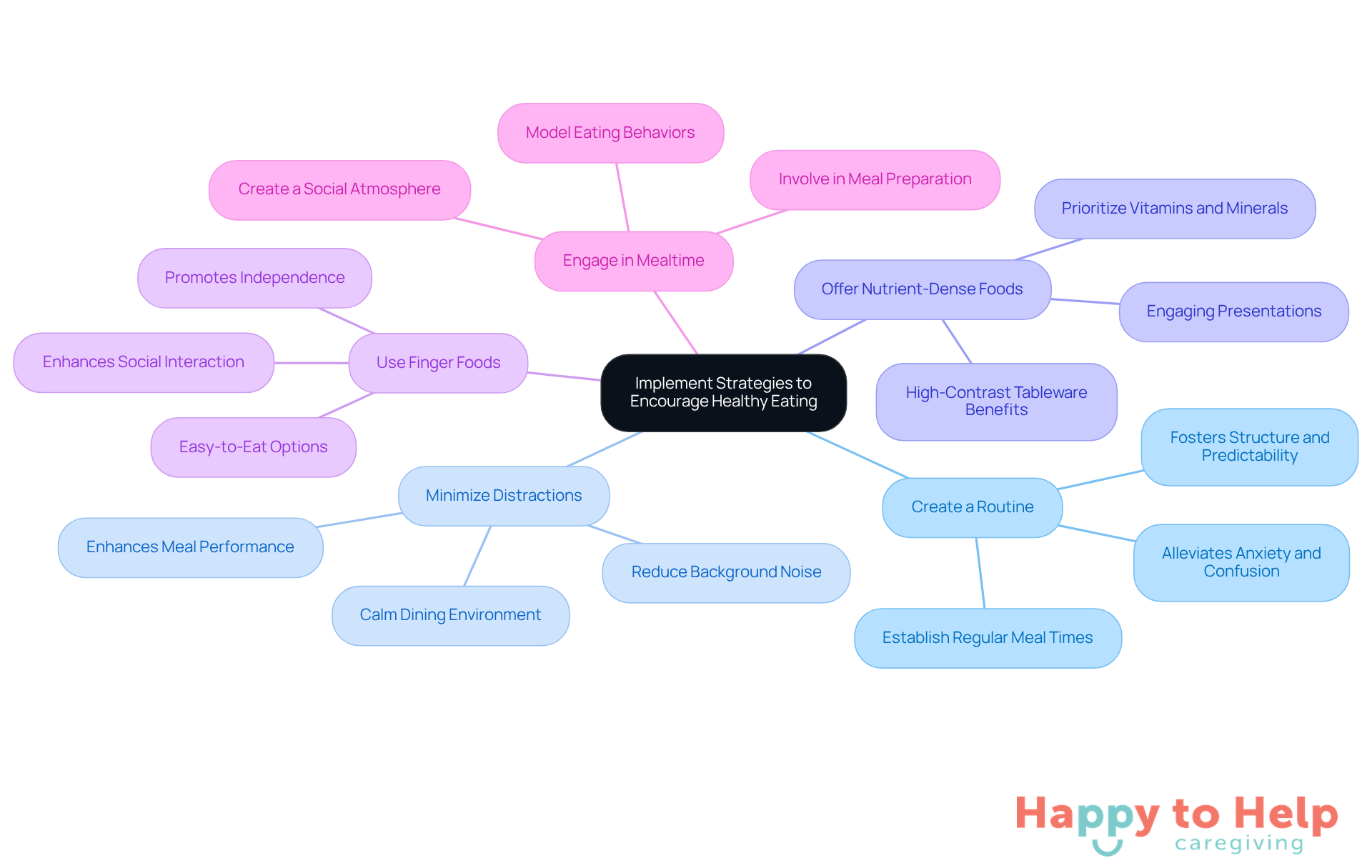
Promoting healthy eating among individuals facing vascular dementia and eating problems presents a significant challenge for caregivers. Cognitive decline can contribute to vascular dementia and eating problems, making mealtimes confusing and stressful, which impacts nutritional intake and overall health. To address this issue, caregivers can implement several effective strategies:
- Create a Routine: Establishing regular meal times fosters structure and predictability. This consistency can alleviate anxiety and confusion, making mealtimes more manageable for individuals experiencing cognitive decline.
- Minimize Distractions: A calm dining environment is essential. Reducing background noise and visual clutter helps individuals focus on their meals, enhancing their ability to enjoy and consume food. Studies show that a calm environment greatly enhances meal performance for individuals with cognitive impairments.
- Offer Nutrient-Dense Foods: Prioritizing foods rich in vitamins and minerals, such as colorful fruits, vegetables, and whole grains, supports overall health. Engaging the senses through appealing presentations can stimulate appetite and encourage better nutritional intake. Notably, utilizing high-contrast tableware can result in a 25% rise in food intake among individuals with cognitive impairment.
- Use Finger Foods: Providing easy-to-eat options that require minimal utensils can empower individuals to feed themselves, promoting independence and reducing frustration during meals. Finger foods can also enhance social interaction during dining.
- Engage in Mealtime: Eating together creates a social atmosphere that can enhance enjoyment and encourage eating. Caregivers should consider participating in meals to model eating behaviors and provide gentle prompts, significantly improving the dining experience. Additionally, involving individuals in meal preparation can foster social interaction and cognitive engagement, further enriching the mealtime experience.
By implementing these strategies, caregivers can not only help maintain nutritional health but also address vascular dementia and eating problems to enrich the overall mealtime experience for individuals.
Address Caregiver Well-Being: Managing Stress and Burnout
Caregivers often face significant challenges, including stress and burnout, which can hinder their ability to provide the best care possible. The implications of neglecting their own well-being can be severe, leading to decreased mental health and feelings of isolation. In fact, 68% of support providers believe they would benefit from direct payment programs to assist with their respite care needs.
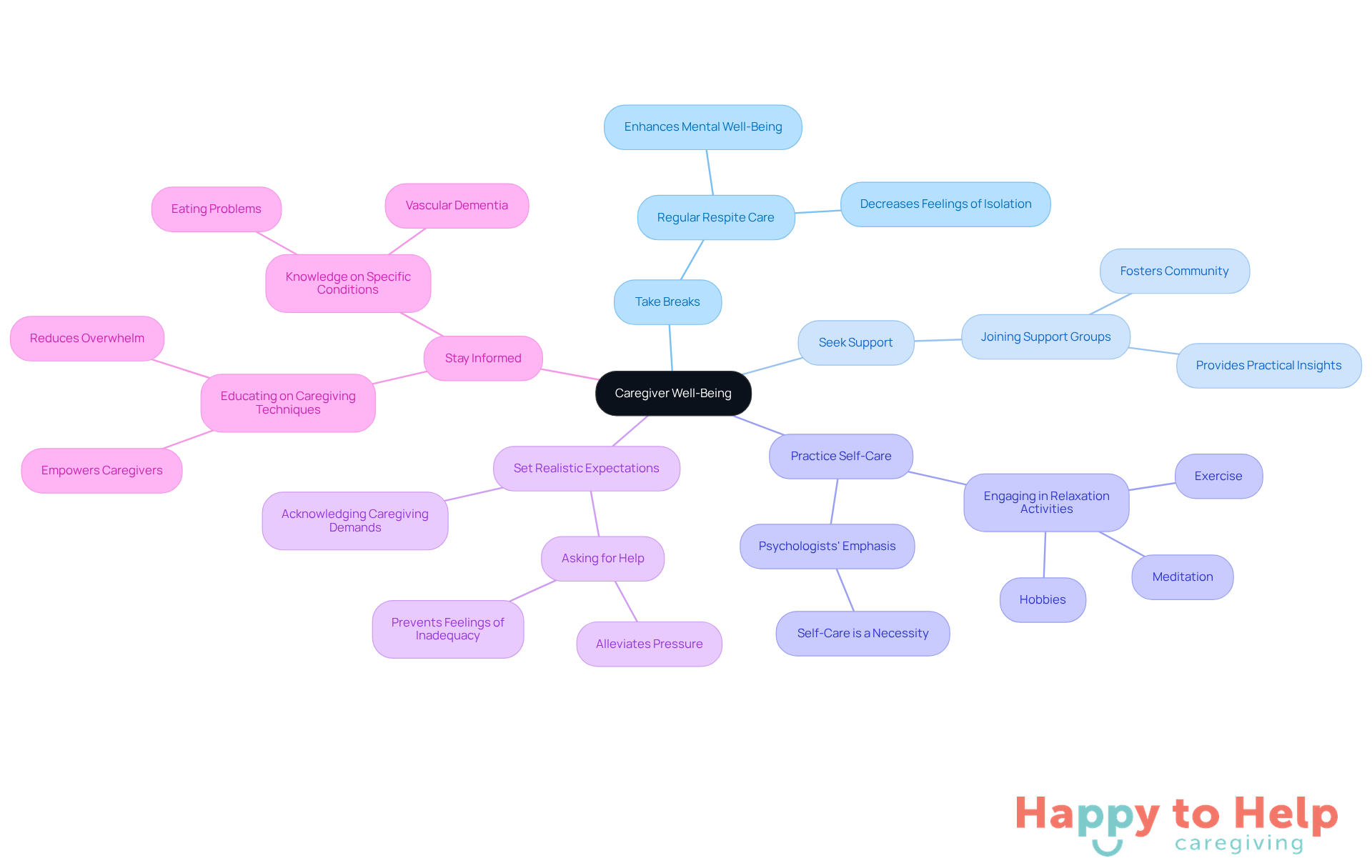
To combat these issues, caregivers can implement several effective strategies:
- Take Breaks: Regular respite care is essential for recharging both physically and emotionally. Studies indicate that those who utilize respite services report enhanced mental well-being and decreased feelings of isolation.
- Seek Support: Joining support groups can be invaluable. Sharing experiences with others facing similar challenges fosters a sense of community and provides practical insights.
- Practice Self-Care: Engaging in activities that promote relaxation-such as exercise, meditation, or hobbies-can significantly enhance emotional resilience. Psychologists emphasize that self-care is not a luxury but a necessity for effective caregiving.
- Set Realistic Expectations: Acknowledge that caregiving can be demanding. It's perfectly acceptable to ask for help when needed, as this can alleviate pressure and prevent feelings of inadequacy. Notably, one in five individuals providing care rate their health as fair or poor, highlighting the importance of maintaining personal well-being.
- Stay Informed: Educating yourself about vascular dementia and eating problems, along with effective caregiving techniques, empowers you and reduces feelings of overwhelm. Knowledge prepares providers to manage challenges more confidently. Additionally, 64% of those providing care experience high emotional stress, underscoring the need for effective stress management strategies.
By prioritizing their own health, caregivers can better support their loved ones, ultimately leading to a more positive caregiving experience.
Moving Forward with Vascular Dementia and Eating Problems:
Vascular dementia poses a significant challenge for caregivers, requiring a thorough understanding of its causes, symptoms, and the specific eating problems that often arise. Reduced blood flow to the brain can lead to various difficulties, making it essential for caregivers to recognize these challenges to improve the quality of life for those affected.
Caregivers face several issues, including the impact of strokes and heart disease, which are common causes of vascular dementia. Symptoms can severely disrupt daily functioning, leading to common eating problems like loss of appetite and swallowing difficulties. To address these issues, caregivers can implement practical strategies to encourage healthier eating habits.
Moreover, caregiver well-being is crucial. Self-care and support not only enhance the caregiving experience but also contribute to better outcomes for those with vascular dementia. By prioritizing their own health, caregivers can provide more effective support.
To effectively manage both cognitive and nutritional needs, caregivers should:
- Implement structured meal routines.
- Foster a calm dining atmosphere.
- Prioritize personal well-being.
These strategies can significantly improve the health of loved ones while reducing the stress and burnout often associated with caregiving. By embracing these approaches, caregivers can create a more fulfilling and supportive environment for themselves and individuals living with vascular dementia.
https://iframe.tely.ai/cta/eyJhcnRpY2xlX2lkIjogIjY5MjY0Mzc0MDBmNGUzMjBmNzc3ZTdkNiIsICJjb21wYW55X2lkIjogIjY4ZWU1ZGNhNzMxNzYyNTU3ZjNjOTVjMSIsICJpbmRleCI6IG51bGwsICJ0eXBlIjogImFydGljbGUifQ==Frequently Asked Questions
What is vascular dementia?
Vascular dementia (VaD) is a decline in mental abilities caused by reduced blood flow to the brain, often resulting from strokes or other vascular issues.
What are the key causes of vascular dementia?
The key causes include stroke, atherosclerosis (hardening of arteries), and heart disease, all of which can lead to insufficient blood flow and oxygen to the brain.
What are the common symptoms of vascular dementia?
Common symptoms include confusion, difficulty concentrating, challenges with organization and planning, memory loss, mood fluctuations (such as depression or anxiety), and physical issues like tremors or difficulty walking.
Why is early recognition of symptoms important for caregivers?
Early recognition of symptoms is crucial as timely intervention can lead to better management of the condition and enhance the quality of life for those affected.
How do cardiovascular health factors relate to vascular dementia?
Factors such as heart disease and stroke significantly increase the risk of developing vascular cognitive impairment, highlighting the need to monitor cardiovascular health to protect cognitive function.
What recent findings suggest early signs of cognitive decline?
A study from Finland indicates that low labor market participation for non-retirement related reasons may signal early signs of cognitive decline, potentially occurring up to 10 years before diagnosis.
What new developments are there in diagnosing vascular dementia?
A global group led by Professor Perminder Sachdev and Dr. Adam Bentvelzen has introduced new diagnostic standards for blood vessel-related mental decline, which can help in identifying and managing the condition more effectively.
List of Sources
- Define Vascular Dementia: Causes and Symptoms
- Medical Xpress - medical research advances and health news (https://medicalxpress.com/tags/vascular+dementia)
- Case Studies (https://physio-pedia.com/Category:Case\_Studies)
- (https://belleviecare.co.uk/support-advice/dementia-quotes-to-lift-your-spirits)
- Identify Eating Problems in Vascular Dementia
- Appetite and dementia (https://alzheimers.org.uk/get-support/living-with-dementia/poor-appetite-dementia)
- How long can a person with dementia live without food or drink? (https://medicalnewstoday.com/articles/dementia-how-long-can-a-person-live-without-eating-or-drinking)
- Caregiver Experiences with Dementia-Related Feeding/Eating Difficulties | MDPI (https://mdpi.com/2227-9032/12/2/133)
- Why Do People with Dementia Stop Eating? Understanding the Causes - Happy To Help (https://happytohelpcaregiving.com/why-do-people-with-dementia-stop-eating-understanding-the-causes)
- Prevalence of Malnutrition in People with Dementia in Long-Term Care: A Systematic Review and Meta-Analysis - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10343750)
- Implement Strategies to Encourage Healthy Eating
- Simple Mealtime Strategies for Dementia Caregivers (https://physioinq.com.au/blog/simple-mealtime-strategies-for-dementia-caregivers)
- Supporting someone with dementia to eat and drink (https://alzheimers.org.uk/get-support/living-with-dementia/improving-eating-experience-dementia)
- 9 Strategies for Helping Dementia Patients Refusing to Eat - Happy To Help (https://happytohelpcaregiving.com/9-strategies-for-helping-dementia-patients-refusing-to-eat)
- Food & Eating | Alzheimer's Association (https://alz.org/help-support/caregiving/daily-care/food-eating)
- Understanding Dementia and Eating: Strategies for Caregivers - Happy To Help (https://happytohelpcaregiving.com/understanding-dementia-and-eating-strategies-for-caregivers)
- Address Caregiver Well-Being: Managing Stress and Burnout
- Caregiver Statistics: Health, Technology, and Caregiving Resources (https://caregiver.org/resource/caregiver-statistics-health-technology-and-caregiving-resources)
- New Report Reveals Crisis Point for America’s 63 million Family Caregivers (https://press.aarp.org/2025-07-24-New-Report-Reveals-Crisis-Point-for-Americas-63-million-Family-Caregivers)
- As Family Caregiving Grows, So Does the Need for Reform - Medicare Rights Center (https://medicarerights.org/medicare-watch/2025/08/14/as-family-caregiving-grows-so-does-the-need-for-reform)
- The Silent Struggle: Caregiver Stress and the Need for Support | Tahoe Forest Health System (https://tfhd.com/news/the-silent-struggle-caregiver-stress-and-the-need-for-support)
- Managing Caregiver Stress - Zumbro Valley Health Center (https://zvhc.org/news/2025/04/managing-caregiver-stress)